Ophthalmology
Pathological myopia: a trainer’s perceptive
High myopia is defined as myopic refraction of greater than -6 dioptres with an axial length greater than 26.5mm, while pathological myopia is myopic refraction with posterior pole degeneration [1]. These degenerative changes can affect a young population and in...
My top five: Emerging alternatives to manage and treat nAMD
Wet (exudative or neovascular) age-related macular degeneration (AMD) is characterised by choroidal neovascularisation, in which new blood vessels from the choroid invade through Bruch’s membrane. These blood vessels proliferate beneath or through the retinal pigment epithelium (RPE), causing patients to...
The Escape Room and gamification of ophthalmology teaching
Recently, there has been an interesting development in medical education and its ‘gamification’. Educators are constantly looking for new ways to engage their students by adding a friendly element of competition, as evidenced by the great success of online education...
Part 1: The Arclight Project – Frugal tech for sight
The Arclight Project is a mix of frugal design, manufacturing, distribution, teaching, research, and advocacy, all wrapped up in a social enterprise based at the University of St Andrews. The project is driven by the high burden of needless blindness...
Virtual ophthalmic conferences: learnings from the Covid-19 pandemic
The Covid-19 pandemic was the catalyst for a number of paradigm shifts in numerous industries. The demand for proxies that follow social distancing measures created a hotbed for digital solutions and transitioned these to social convention. In the aftermath, the...
The All Eyes Foundation
At its core, All Eyes Foundation (AEF) wishes to help bring vision back to Iraq, and it intends to do this through ophthalmic subspecialty training, mentoring and infrastructure development. Based in Najaf, just over 100 miles south of Baghdad, the...
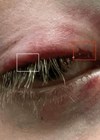
Hidden eyelid laceration following blunt trauma
A paediatric case report of a hidden eyelid laceration following blunt trauma. Blunt injury to the eyelid can result in a multitude of issues, such as damage to the eyelid margin, lacrimal system and surrounding orbit [1]. These can often...
Acute macular neuroretinopathy
Acute macular neuroretinopathy (AMN) is a rare condition that typically affects young women and presents with photopsia and paracentral scotomata [1]. We describe a case of severe acute macular neuroretinopathy, following Covid-19 infection. A 30-year-old woman presented to the urgent...
Strabismus and ocular motility, demystified
I am a former orthoptist, now trained in medicine and working as a foundation doctor. In my previous work, I was frequently approached by ophthalmology trainees eager for guidance with strabismus and ocular motility. Drawing on my clinical experience, I...
Minimally Invasive Glaucoma Surgery: What options are there and when might they be considered?
In recent years there has been a rapid expansion in a group of operations termed ‘minimally invasive’ or ‘micro invasive’ glaucoma surgery (MIGS). These options generally offer less significant IOP reduction, but with a more favourable safety profile when compared...
My top five: Innovative approaches to dry AMD
Age-related macular degeneration (AMD) is one of the leading causes of irreversible blindness in the developing world with its prevalence rising alongside age. In societies characterised by ageing populations, it is imperative we explore more effective treatment to alleviate the...
Evolving towards an interventional glaucoma mindset
Traditionally, a newly diagnosed glaucoma patient would be treated first with medical therapy. As the disease progressed or the initial intervention failed to adequately control intraocular pressure (IOP), clinicians would add more drops, selective laser trabeculoplasty (SLT), repeated SLT and...