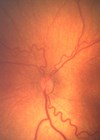
Retinopathy of prematurity (ROP) is a disorder of the immature preterm retina and a leading cause of preventable, irreversible blindness in children. There are 15 million preterm births annually, and over 32,000 neonates became blind from ROP in 2010 [1].
Blindness in children impacts psychomotor and cognitive development, educational attainment, has negative social and financial consequences and increases the likelihood of death in childhood, particularly in low-income countries (LICs) [2].
ROP in low-income countries
Countries with high rates of vision loss from ROP are those where neonatal intensive care units (NICUs) have recently expanded, but where the quality of care is variable, with inadequate or no coverage of ROP screening and treatment. Modifiable risk factors for ROP include hyperoxia from uncontrolled unmonitored oxygen use, sepsis, poor weight gain and blood transfusions [3]. Many NICUs in LICs lack the resources necessary to address these risk factors. This means that both the incidence and severity of ROP are greater in LICs compared with middle- or high-income countries.
Screening and treatment of ROP
Control of visual loss from ROP entails high-quality neonatal care from immediately after birth, timely screening of infants at risk, followed by treatment of those identified with severe disease. Standard screening requires weekly visits to NICUs by trained ophthalmologists who examine the eyes to decide whether to screen again, treat or stop screening. They use indirect ophthalmoscopy, which allows a detailed view of each baby’s retina. Treatment is usually needed in 5-15% of those screened. The time window to intervene is tight as ROP starts a few weeks after birth, and regresses, or progresses, over a few weeks.
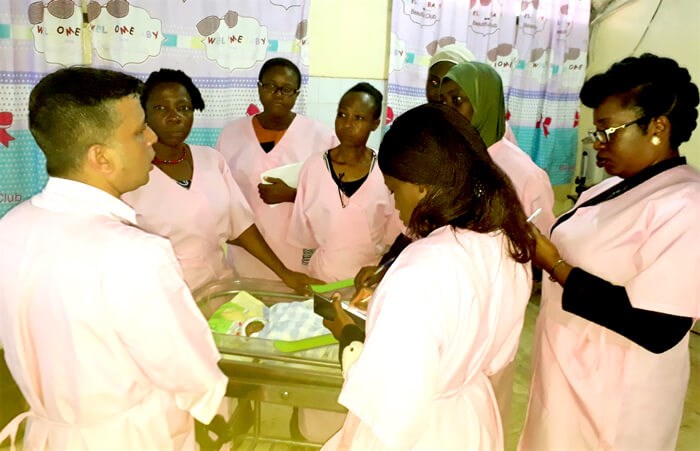
Figure 1: ROP screening training session.
In high-income countries, control strategies are effective, and few infants become ROP blind. Middle-income countries in South America and India have shown that it is possible to implement ROP programmes [4,5]. However, research by Professor Clare Gilbert and others into ROP blindness shows that it is now rapidly emerging in many LICs, including Africa, as NICUs for sick and preterm newborns expand [6,7]. Key challenges in controlling ROP blindness in LICs include under-resourced neonatal care, the low number of ophthalmologists, the extensive training required to become competent in screening and treatment, the time-consuming nature of examinations, high medico-legal risks involved and follow-up of babies who have been discharged from the hospital [8]. Services for ROP are being developed in some countries in Africa e.g., Nigeria and Kenya, but coverage remains low, due mainly to the lack of trained ophthalmologists to conduct the screening [5].
Telemedicine for screening
Telemedicine with wide-field retinal imaging taken by a trained technician or nurse, with remote image grading by an ophthalmologist, is a potential solution as an alternative to standard screening. This approach, which addresses the challenge of the low number of ophthalmologists, is effective in India and Chile, but has not yet been widely implemented elsewhere [9-11]. In telemedicine screening, trained, non-medical technicians take retinal images, which allows scale-up to multiple NICUs. ROP telemedicine screening is superior to standard ROP screening in terms of cost-effectiveness, documentation and earlier detection of potentially treatment-requiring ROP. It is also used to educate parents and neonatal teams, to seek second opinions and for medico-legal reasons [12,13].
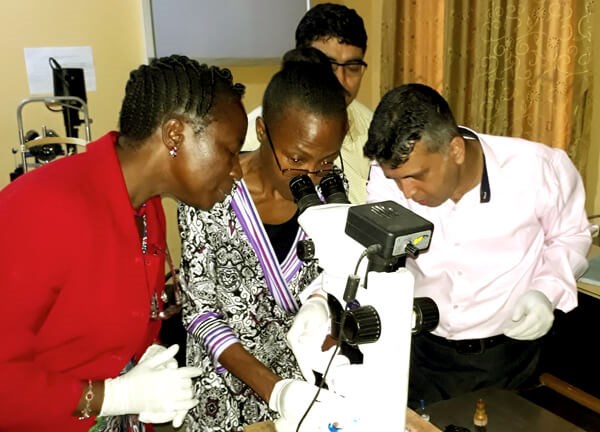
Figure 2: Training on intravitreal anti-VEGF.
The ROP Network (ROP-NET)
The ROP-NET was established in 2017 with funding from the Queen Elizabeth Diamond Jubilee Trust and included six countries aiming to either establish or expand ROP services: Ghana, Nigeria, Kenya, Tanzania, Pakistan and Sri Lanka. A network model with south-south partnerships was established. Important principles included joint local neonatology-ophthalmology teams leading the programmes, whole team training and team building and development of needs-based country-specific plans.
After an initial planning meeting and workshop, where mentee institutions established their needs and formulated an initial country-specific ROP plan, they were partnered with mentor institutions in India (Aravind, LVPEI, HV Desai), South Africa (Durban) and the UK (London). The partners worked together to develop and establish their ROP programme goals including multi-disciplinary training in the Indian institutions, team visits between institutions, raising awareness of ROP within country and working with national Ministries of Health. A final ROP-NET meeting in 2019 established progress made and specific goals achieved. All participating countries had established ROP programmes. ROP services have continued after the Queen Elizabeth Diamond Jubilee Trust funding ended, which demonstrates the sustainability of the approach.
ROP-NET Nigeria-India experience – Professor Dupe Ademola-Popoola, Ilorin, Nigeria
In Nigeria, between 2017 and 2019, ROP-NET supported expansion and scale-up of ROP services primarily by the development of a partnership between University of Ilorin Teaching Hospital, Nigeria and specialist ophthalmologists and neonatologists at LVPEI, India. The programme goals were to amplify ROP services in Nigeria using three main approaches:
- Human resource development
- Advocacy within the institution and nationally
- National partnerships between NICU staff and ophthalmology units
The aims were to reduce the incidence of ROP by improving the quality of neonatal care, screening and providing prompt care for babies who develop ROP.
The first step was a visit by the team from LVPEI for training, raising awareness of ROP and advocacy. This included joint planning and organisation of two face-to-face workshops and a joint meeting of stakeholders in Nigeria in 2018, held at the University of Ilorin Teaching Hospital, Gwarinpa General Hospital and in Abuja, Federal Capital Territory. The events were attended by all stakeholders including nurses, obstetricians, neonatologists and ophthalmologists. This was followed by a reciprocal visit to India by the Nigerian ophthalmologist for training on ROP screening and treatment, so that she was later able to provide advocacy and training visits for ROP services at two further tertiary hospitals in Nigeria, University of Abuja Teaching Hospital and Federal Medical Centre, Lokoja.
The advocacy activities involved presentation and distribution of key messages on ROP to paediatricians and other stakeholders including clinical meetings and conferences of ophthalmologists, paediatricians and neonatologists. There was emphasis on blinding ROP and prematurity-related ocular morbidities beyond ROP, and the consequences. Strategies for effective prematurity-related programmes at hospital, state, regional and national levels were discussed including the need for information, education and provision of communication materials for all stakeholders including caregivers, neonatologists / paediatricians, NICU nurses, ophthalmologists, midwives and obstetricians, the community and hospital administrators.
Professional communication platforms were set up to support continuous engagement among the stakeholders. Institutional research and audit and national research were also encouraged.
The impact of ROP-NET implementation was the sustainable platform for ongoing development of ROP services and improved awareness and engagement among critical stakeholders, as well as improved research output on ROP in Nigeria [14].
ROP-NET Tanzania-India experience – Dr Sucheta Kulkarni, HV Desai Eye Hospital, Pune, India
Five ROP specialist teams from five eye institutions in India (HV Desai Eye Hospital, Pune; LV Prasad Eye Institute, Hyderabad; LV Prasad Eye Institute, Bhubaneshwar; Aravind Eye Hospital, Madurai and Aravind Eye Hospital, Coimbatore) were invited as mentors to work with training institutions in Africa. The first step was to formulate the goal and objectives of each mentor-mentee partnership. The discussion and the process of identifying SMART objectives was immensely helpful in understanding the situation of each mentee. Clear timelines were agreed upon for each of the objectives.
The mentee teams were invited to the mentor institutes for ROP training. The teams comprised an ophthalmologist, neonatal nurse and paediatrician. The neonatal team were able to experience an ROP screening programme, observe best neonatal care practices and learn about ROP screening guidelines. The ophthalmologist stayed on longer to practise the skills used in ROP screening – first on dummy eyes and later in preterm infants. Observing and assisting in ROP laser as well as intravitreal anti-VEGF injections was an important part of their training.
During the visit to India, the ophthalmologist from Tanzania also travelled with the ROP team to various districts to understand the challenges and solutions in an outreach setting. This helped her to understand the role of each stakeholder (paediatrician, neonatal nurse, screening technician, programme manager, etc). This is crucial to achieve a successful, sustainable ROP screening programme.
Another advantage of an outreach setting is high-volume screening (25-30 babies in a day). This helped the ROP trainee understand how to achieve efficiency in screening in addition to getting to practice her skills in a high-volume setting. By the end of the training period, the Tanzanian ophthalmologist was very confident in screening.
The ROP mentee then went back to Tanzania and had a detailed discussion with her ophthalmology and paediatrics team to sensitise them before starting actual screening activity in the country’s biggest national health facility. Subsequently, the mentor visited Tanzania to support and advise on any challenges encountered in establishing a smooth ROP screening programme. The team had meetings with the institute head to advocate for the urgent need to establish a screening programme. There were three sensitisation meetings held with medical students, nurses and the ophthalmology team as well as paediatrics resident doctors. During the visit, two babies who needed urgent treatment were identified and treated with laser and anti-VEGF injection respectively. This provided an opportunity for the mentee to practice her treatment skills under supervision, which proved to be helpful for her confidence.
The wider group discussions that happened with global experts and ROP-NET partners during the period of the project were enriching in terms of sharing best practices, challenges and possible solutions. Several institutes in India emerged as international ROP training centres. The advocacy efforts taken by the entire group in respective mentee countries to establish ROP screening programmes ultimately resulted in great impact on the ground in terms of higher numbers of screenings and identification of infants who needed treatment.

Figure 3: ROP stakeholders in Ilorin, Nigeria, who came together to promote ‘No-ROP-Blindness’ in our city.
Conclusion and the future of ROP-NET
ROP-NET emerged as a collaborative international effort to improve ROP care in six countries. All countries involved in the ROP Network have plans to expand their ROP services and are keen to participate in a second phase. There have also been requests from other countries, such as Nepal, Indonesia and Malawi, to join. The planned next phase of the ROP-NET would keep the successful south-south partnerships and network model with country-led programme goals from strong local multidisciplinary teams.
However, the development of telemedicine ROP programmes is ideally placed for expansion of ROP services and plans to focus on:
- Strengthening data collection and monitoring
- Integrating with neonatal data systems wherever possible
- Collaboration with Ministry of Health, WHO and UNICEF in country for integration into national policies and to establish sustainable programmes
- Regular webinars and meetings to discuss clinical cases and service challenges between all network members for continuing education and ongoing support.
This next phase would allow the ROP teams to expand services in a sustainable and scalable way, demonstrate clearly the impact of the programmes and learn from each other’s experiences – taking the impact of the ROP Network beyond even the countries which are included.
References
1. Blencowe H, Lawn JE, Vasquez T, et al. Preterm-associated visual impairment and estimates of retinopathy of prematurity at regional and global levels for 2010. Pediatr Res 2013;74(S1):35-49.
2. Keil S, Fielder A, Sargent J. Management of children and young people with vision impairment: diagnosis, developmental challenges and outcomes. Arch Dis Child 2017;102(6):566-71.
3. Hellström A, Smith LE, Dammann O. Retinopathy of prematurity. Lancet 2013;382(9902):1445-57.
4. Arnesen L, Durán P, Silva J, Brumana L. A multi-country, cross-sectional observational study of retinopathy of prematurity in Latin America and the Caribbean. Rev Panam Salud Publica 2016;39(6):322-9.
5. Bowe T, Nyamai L, Ademola-Popoola D, et al. The current state of retinopathy of prematurity in India, Kenya, Mexico, Nigeria, Philippines, Romania, Thailand, and Venezuela. Digit J Ophthalmol 2019;25(4):49-58.
6. Gilbert C, Malik ANJ, Nahar N, et al. Epidemiology of ROP update: Africa is the new Frontier. Semin Perinatol 2019;43:317-22.
7. Melesse MA. Retinopathy of prematurity - an emerging cause of childhood blindness in Ethiopia. Eth Med J 2020;58(2):167-72.
8. Barrero-Castillero A, Corwin BK, VanderVeen DK, Wang JC. Workforce shortage for retinopathy of prematurity care and emerging role of telehealth and artificial intelligence. Pediatr Clin N Am 2020;67(4):725-33.
9. Vinekar A, Gilbert C, Dogra M, et al. The KIDROP model of combining strategies for providing retinopathy of prematurity screening in underserved areas in India using wide-field imaging, tele-medicine, non-physician graders and smart phone reporting. Indian J Ophthalmol 2014;62(1):41-9.
10. Shah PK, et al. Evolution of ROP screening at Aravind Eye Hospital, Coimbatore - Lessons learnt and the way ahead. Comm Eye Health 2018;31(101):S23–4.
11. Ossandón D, Zanolli M, Stevenson R, et al. A national telemedicine network for retinopathy of prematurity screening. JAAPOS 2018;22(2):124-7.
12. Castillo-Riquelme MC, Lord J, Moseley MJ, et al. Cost-effectiveness of digital photographic screening for retinopathy of prematurity in the United Kingdom. Int J Technol Assess Health Care 2004;20(2):201-13.
13. Ells AL, Holmes JM, Astle WF, et al. Telemedicine approach to screening for severe retinopathy of prematurity: a pilot study. Ophthalmology 2003;110(11):2113-7.
14. Ademola-Popoola DS, Fajolu IB, Gilbert C, et al. Strengthening retinopathy of prematurity screening and treatment services in Nigeria: a case study of activities, challenges and outcomes 2017-2020. BMJ Open Ophthalmol 2021;6(1):e000645.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME