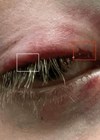
We report a case of unilateral mydriasis in a female patient referred by her general practitioner (GP) with a dilated and sluggish left pupil, likely caused by the accidental use of her husband’s prescription eyedrops. This case highlights the importance of educating patients on the safe use of ophthalmic medications and the dangers of using medications prescribed for others.
Case presentation
A female patient of approximately 65–68 years old was referred to the ophthalmology emergency department by her GP after presenting with a dilated and sluggish left pupil. She reported that the previous Saturday, while gardening, some dirty leaves brushed into her eyes. She instinctively wiped her eyes but did not rinse them. The next day, she noticed a subconjunctival haemorrhage in her left eye and experienced slightly faded vision in that eye. She did not report any dryness or foreign body sensation.

An anonymised close-up image of the patient’s eyes demonstrating marked unilateral mydriasis of the left pupil compared with a normal right pupil.
Her ocular history included mild myopia, for which she occasionally used reading glasses. She had self-administered Optrex (an over-the-counter eyedrop) prior to presentation. On examination by her GP:
- Visual acuity: right eye 4/6, left eye 5/6
- Pupils: left pupil mydriatic with sluggish response to both light and accommodation
- Ocular motility: full, no ophthalmoplegia
- Anterior segment: subconjunctival haemorrhage, fluorescein staining normal
- Lymph nodes: no palpable lymphadenopathy
- Neurological exam: normal deep tendon reflexes, no focal neurological signs.
Further history obtained from her son revealed that the patient had used her husband’s prescription eyedrops – specifically atropine, and possibly dexamethasone – in an attempt to relieve discomfort. She was unaware of the contents or the potential effects of these medications. The final diagnosis was pharmacologic mydriasis secondary to inappropriate topical atropine use.
Discussion
Atropine is a long-acting antimuscarinic agent that induces mydriasis and cycloplegia by inhibiting parasympathetic input to the iris sphincter and ciliary muscles. This case illustrates the diagnostic challenge posed by incomplete medication histories, particularly when patients use eyedrops prescribed for others or are unaware of what they have used. Self-medication, especially with mydriatics or corticosteroids, can lead to both diagnostic confusion and potential harm.
As the triage nurse, I also recalled a relevant community anecdote: a neighbour once told me that she routinely used the same bottle of artificial tears for herself, her children and her husband. After I explained the associated risks – such as cross-contamination, inappropriate dosing and unintended exposure to medications – she discontinued the practice. This reflects a widespread lack of awareness about the safe use of eyedrops in the general population.
Conclusion
This case emphasises the importance of:
- Taking a thorough and specific medication history, including over-the-counter products, and
- Educating the public on the dangers of using someone else’s prescription eyedrops.
Healthcare professionals must proactively inform patients that eyedrops should not be shared. Greater public awareness is essential to prevent medication errors and avoidable harm.
Patient education messages
Patients and caregivers should be advised:
- Never use eyedrops prescribed for someone else
- Avoid sharing any eye medications, including artificial tears
- Consult a healthcare provider before using any eyedrops, especially following trauma or irritation
- Clearly label and store medications separately, especially in households with multiple users.
Acknowledgement: The author would like to acknowledge the support and guidance offered by Tendai Gwenhure during the creation of this article, and her inspirational leadership.
Declaration of competing interests: None declared.