The authors describe their elective experience and delve further into high myopia, an emerging ophthalmic disease that is increasingly recognised in and outside Asia.
The medical school elective programme presents an opportunity for students to conduct learning in their chosen specialties and healthcare settings. We were fortunate to attend National Taiwan University (NTU) in Taipei, Taiwan for two weeks in the ophthalmology department.
The elective experience
The two-week ophthalmology clinical elective in National Taiwan University Hospital (NTUH) was highly organised and structured. The schedule consisted of a mixture of small-group tutorials, lectures, practical workshops, clinics and surgeries.
There was a strong teaching culture in the department. This was exemplified by daily morning meetings for case-based discussions and departmental subspecialty teachings. These meetings were attended by medical students, junior doctors and consultants. The topics discussed were varied, ranging from foreign body assessment to toxoplasma retinitis.
There were ample teachings on different ophthalmic examination techniques such as slit-lamp examination, direct and indirect ophthalmoscope, application of fluorescein dye to check for corneal ulcers or to check the tear break-up time, exophthalmometer, use of prisms to examine squint and others. We were also introduced and taught how to operate different investigation instruments such as the pneumotonometer. I was extremely impressed that these were all components of ophthalmology curriculum for medical students in NTU.

Figure 1: Entrance to National Taiwan University Hospital.

Figure 2: View of Taipei 101.

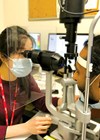
Figure 3: Practising slit-lamp examination.
The elective programme is also an opportunity to understand health systems different from the NHS in the UK. Taiwan boasts a wide-reaching National Health Insurance (NHI) covering at least 99% of the population [1]. This hopes to provide equitable and affordable healthcare to all. Whilst not free at the point of delivery, medical fees are kept to the minimum, with payments ranging from 80 to 400 NTD (£2‑10). NHI premiums are means-tested based on income, and the central government provides more support for low-income households. Akin to the NHS, the system is put under pressure with an increasing proportion of older population and chronic diseases. One stark difference from NHS was the freedom to choose their healthcare providers, including opting for specialist services and thus bypassing primary care physicians.
“During this elective, we began to appreciate myopia as more than just a mere refractive error”
The high demand for secondary care was palpable even during our short elective placement in the NTU hospital ophthalmology clinic; I have been told that a single ophthalmologist would see 80-100 patients in a single clinic session! Luckily for students, there were dedicated teaching clinics whereby clinicians were not under pressure to rush through a certain number of patients. This allowed more time for discussions of the different clinical signs. Where appropriate, we were allowed to take clinical histories and carry out eye examinations prior to patients being seen by the consultants. This was a valuable time to practise operating the slit-lamp to examine the lids, external eye, cornea, anterior chamber and lens. Examining the vitreous and retina required additional use of a condensing lens; admittedly, this was extremely difficult to learn and perform within the short period of two weeks!
We were particularly impressed by the set-up of the dedicated teaching clinics, in which the slit-lamp view could be projected live onto a screen. This allowed consultants to provide feedback on our examination technique. In addition, the screen capture function enabled consultants to explain the findings in greater detail. This tremendously helped our understanding of different pathologies and allowed us to be more comfortable with the use of slit-lamp examination.
We saw patients with various presenting complaints such as blurry vision, visual field loss, eye pain, floaters, lid lesions and others. Eye pathologies commonly seen in a general ophthalmology clinic in NTU were similar to that in UK. For instance, hordeolum, chalazion, corneal lesions, cataract, glaucoma, keratoconjunctivitis sicca (dry eyes) and others. There were also cases of minor ocular trauma and paediatric cases such as amblyopia and strabismus. Management of eye conditions in Taiwan and UK is broadly similar. However, on several occasions, we saw young school-aged children presenting to the ophthalmology clinic for treatment of progressive myopia. It appeared that in Taiwan there was an emphasis on recognising high myopia as a disease (rather than a mere refractive problem) with risks of complications such as cataract, open angle glaucoma, peripheral retinal and macular degeneration. As such, progression of myopia in young children was taken very seriously in NTU, with treatment initiated early.
Myopia
Myopia is traditionally known to disproportionately impact East Asian countries. Up to 80% of teens in Singapore, Taiwan and Japan have myopia, with the prevalence of high myopia reaching 10% [2]. This contrasted with the relatively low prevalence of high myopia of 2% amongst the adult Western European or American population. However, myopia is increasingly more prevalent. It was estimated that by 2050, half of the world’s population would have myopia, and 10% would suffer from high myopia [3]. Uncorrected myopia is currently the leading cause of moderate to severe visual impairment and the second leading cause of blindness globally.
Risk factors for myopia or pathophysiology of myopia
For clear vision, light rays from an object need to be appropriately refracted onto the retina for stimulation of photoreceptors, eventually leading to stimulation of the visual cortices. In myopia, the visual image forms in front of the retina, either due to excess refraction or axial length.
Myopia develops as a result of both genetic and environmental influence. Parental myopia is a risk factor for myopia development [4]. Environmental factors include less time spent outdoors and near work [5]. Interestingly, the Sydney Myopia Study showed that higher levels of time spent outdoors were associated with less myopia, even after adjusting for parental myopia, ethnicity and near work [6]. Other risk factors for high myopia include Stickler syndrome, Down syndrome, Ehlers-Danlos syndrome, Marfan syndrome and prematurity. Undercorrection of myopia is also associated with progression of myopia [7].
Several mechanisms of myopia development have been suggested. Near work is associated with insufficient accommodative response (accommodative lag). This places the plane of best focus behind the retina (hyperopic defocus). It is thought that peripheral optical blur is a signal for axial elongation [8]. It has also been suggested that intensive near work increases axial length by means of extraocular muscle forces and ciliary muscle contraction [9].
In pathological myopia, the elongated globe is thinned and stretched, leading to various fundal abnormalities characteristic of pathological or degenerative myopia, such as lacquer cracks, staphyloma, retinal detachment, macular degeneration and choroidal neovascularisation. Risks of retinal detachment and macular choroidal neovascularisation are increased at any levels of myopia, but become markedly higher at myopia greater than 5 dioptres (D) [10]. The risks of these complications are not reversed by refractive procedures such as LASIK [11].
Myopia prevention and control
Control of myopia is an area of active research. Strategies to prevent myopia development or control myopia progression include lifestyle changes, pharmacological treatment and optical control (spectacles or contact lenses).
Increasing outdoor time
Increasing outdoor time has been shown to prevent myopia development. In a school-based cluster randomised trial, an additional 40-minutes outdoor time in each school day reduced myopia incidence by 23% at three-year follow-up, although difference in axial length elongation was not significantly reduced [12]. Another school-based interventional study in Taiwan showed that outdoor activities during class recess significantly reduced the incidence of myopia from 17.65% in the control group to 8.41% the interventional group [13]. Increasing outdoor time as a method to prevent myopia development is further supported by a large meta-analysis of 25 studies [14]. Interestingly, despite showing that increasing time outdoors could reduce myopic shift, this intervention did not slow progression in already myopic eyes.
Positive results from various studies led to a policy change in Taiwan; the Tian-Tian 120 outdoor programme encouraged schools to take students outdoors for 120 minutes every day. This was shown to reverse the previous long-term trend of rising myopia prevalence, leading to a reduction in myopia prevalence within three years of implementation [15].
Spectacles
Spectacle lenses used for optical control of myopia are designed to reduce defocus. The Correction of Myopia Evaluation Trial (COMET) showed that progressive addition lenses (PAL) reduced myopia progression by 0.2D especially in the first year of use [16]. PAL are one-piece lenses designed to have a gradient of lens power with distance prescription at the top, and near prescription at the bottom without any line of demarcation. This is designed to reduce defocus, which is thought to be stimulus for axial elongation.
A meta-analysis of nine trials showed that multifocal lenses slowed myopic progression by 0.25D/year, compared to single vision lenses [17]. More recently, a trial investigated the use of prismatic bifocals, showing greater efficacy in myopia control [18]. Although statistically significant, the use of lenses in myopia control has been criticised for its small clinical effect.
Orthokeratology
Orthokeratology involves the use of rigid gas-permeable contact lenses with a reverse geometry design to reshape the cornea at night-time. In myopia, it mechanically flattens the central cornea. Its use has been shown to reduce axial length elongation [19,20]. Orthokeratology has the advantage of not requiring daytime use of lenses or spectacles, making this suitable for active individuals. However, its effect is temporary, with reported rebound effect, in which axial elongation is more pronounced after discontinuation [21]. In addition, there is a concern about the risk of microbial keratitis associated with lens use [22].
Pharmacological method
Atropine eye drops have been widely investigated in myopia control. The exact mechanism is not fully understood. Due to its cyclopegic effect, side-effects include photosensitivity and blurry vision. The efficacy in myopia control was demonstrated in the Atropine in the Treatment of Myopia (ATOM) study. The ATOM study showed that 1% atropine showed a 77% reduction in myopia progression [23]. The subsequent ATOM2 trial comparing 0.01%, 0.5% and 1.0% doses of atropine found that even a 0.01% dose could slow myopia progression, with less rebound effect and less side- effects [24,25]. However, only 1% atropine was shown to slow axial elongation. In the UK, low-dose atropine is being investigated in the Childhood Atropine for Myopia Progression (CHAMP) trial.
Conclusion
The elective programme in the NTU ophthalmology department is a fantastic chance to experience and appreciate ophthalmic practice in another healthcare setting. This is an exciting opportunity to fully immerse in the world of ophthalmology, and to enjoy the amazing Taiwanese food! We have provided high myopia as an example of ocular disease that we began to appreciate more during our electives. For those aspiring to enter ophthalmology specialty training in the UK, an ophthalmic elective scores a point for the portfolio section of the application.
Declaration of competing interests: None declared.
*equally contributing co-first authors.
References
1. Wu TY, Majeed A, Kuo KN. An overview of the healthcare system in Taiwan. London J Prim Care (Abingdon) 2010;3:115-9.
2. Lin LLK, Shih YF, Hsiao CK, et al. Prevalence of Myopia in Taiwanese Schoolchildren: 1983 to 2000. Ann Acad Med Singapore 2004;33(1):27-33.
3. Holden BA, Fricke TR, Wilson DA, et al. Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology 2016;123:1036-42.
4. Pan CW, Ramamurthy D, Saw SM. Worldwide prevalence and risk factors for myopia. Ophthalmic Physiol Opt 2012;32(1):3-16.
5. Lin Z, Vasudevan B, Jhanji V, et al. Near work, outdoor activity, and their association with refractive error. Optom Vis Sci 2014;91(4):376-82.
6. Rose KA, Morgan IG, Ip J, et al. Outdoor Activity Reduces the Prevalence of Myopia in Children. Ophthalmology 2008;115(8):1279-85.
7. Chung K, Mohidin N, O’Leary DJ. Undercorrection of myopia enhances rather than inhibits myopia progression. Vision Res 2002;42(22):2555-9.
8. Smith EL, Hung LF, Arumugam B. Visual regulation of refractive development: Insights from animal studies. Eye 2014;28(2):180-8.
9. Ghosh A, Collins MJ, Read SA, et al. Axial elongation associated with biomechanical factors during near work. Optom Vis Sci 2014;91(3):322-9.
10. Flitcroft DI. The complex interactions of retinal, optical and environmental factors in myopia aetiology. Prog Retin Eye Res 2012;31(6):622-60.
11. Jorge J, Junior N, Cândido R, et al. Alterações da retina periférica após LASIK. Rev bras oftalmol 2008;67(3):124‑31.
12. He M, Xiang F, Zeng Y, et al. Effect of time spent outdoors at school on the development of myopia among children in China a randomized clinical trial. JAMA - J Am Med Assoc 2015;314:1142-8.
13. Wu PC, Tsai CL, Wu HL, et al. Outdoor activity during class recess reduces myopia onset and progression in school children. Ophthalmology 2013;120(5):1080-5.
14. Xiong S, Sankaridurg P, Naduvilath T, et al. Time spent in outdoor activities in relation to myopia prevention and control: a meta-analysis and systematic review. Acta Ophthalmol 2017;95:551-66.
15. Wu PC, Chen CT, Chang LC, et al. Increased time outdoors Is followed by reversal of the long-term trend to reduced visual acuity in Taiwan Primary school students. Ophthalmology 2020;127(11):1462-9.
16. Gwiazda J, Hyman L, Hussein M, et al. A randomized clinical trial of progressive addition lenses versus single vision lenses on the progression of myopia in children. Investig Ophthalmol Vis Sci 2003;44(4):1492-500.
17. Li SM, Ji YZ, Wu SS, et al. Multifocal Versus Single Vision Lenses Intervention to Slow Progression of Myopia in School-age Children: A Meta-analysis. Surv Ophthalmol 2011;56(5):451-60.
18. Cheng D, Woo GC, Drobe B, et al. Effect of bifocal and prismatic bifocal spectacles on myopia progression in children: Three-year results of a randomized clinical trial. JAMA Ophthalmol 2014;132(3):258-64.
19. Swarbrick HA, Alharbi A, Watt K, et al. Myopia control during orthokeratology lens wear in children using a novel study design. Ophthalmology 2015;122(3):620-30.
20. Si J-K, Tang K, Bi H-S, et al. Orthokeratology for Myopia Control. Optom Vis Sci 2015;92:252-7.
21. Cho P, Cheung SW. Discontinuation of orthokeratology on eyeball elongation (DOEE). Contact Lens Anterior Eye 2017;40(2):82-7.
22. Bullimore MA, Sinnott LT, Jones-Jordan LA. The risk of microbial keratitis with overnight corneal reshaping lenses. Optom Vis Sci 2013;90(9):937-44.
23. Chua WH, Balakrishnan V, Chan YH, et al. Atropine for the Treatment of Childhood Myopia. Ophthalmology 2006;113(12):2285-91.
24. Chia A, Chua WH, Cheung YB, et al. Atropine for the treatment of childhood Myopia: Safety and efficacy of 0.5%, 0.1%, and 0.01% doses (Atropine for the Treatment of Myopia 2). Ophthalmology 2012;119(2):347-54.
25. Chia A, Chua WH, Wen L, et al. Atropine for the treatment of childhood myopia: Changes after stopping atropine 0.01%, 0.1% and 0.5%. Am J Ophthalmol 2014;157(2):451-7.e1.
COMMENTS ARE WELCOME