The date 6.6.2020 was selected as a significant milestone for celebrating the achievements of the VISION LINKS Programme as part of the global ‘VISION 2020: The Right to Sight’ initiative [1]. This virtual full-day seminar included LINK partners in the UK and those overseas (mainly Africa, but also the Caribbean and South Pacific regions).
Over 400 participants from 26 countries participated in the virtual seminar. Throughout the day, delegates contributed through small and large group discussions, polls and feedback to give their input. New approaches, technologies and ways of working were explored to develop existing programmes and consider new opportunities. The full recording of the Celebration Day is available [2]. This article is an overview of the day’s events.
Achievements and challenges of the VISION 2020 global initiative
The day’s sessions opened with a presentation by Professor Allen Foster, charting the progress made through the VISION 2020 global initiative. In the last 25 years there has been an overall reduction of 25% in the age-standardised prevalence of blindness and visual impairment, with significant reductions in the number of people blind through onchocerciasis, trachoma and vitamin A deficiency. However, the ageing and growing population presents an ongoing challenge, with an increase in people with visual impairment from non-communicable conditions such as cataract, refractive error, glaucoma and diabetic retinopathy. Over the coming years it is essential to prepare for the increasing needs of the ageing population.
In low- and middle-income countries (LMICs) there is a need to move from vertical disease programmes (e.g. trachoma control) to comprehensive, sustainable eye care services, especially in the light of the increasing number of people affected by long-term, non-communicable conditions. The regular monitoring and complex management needed to address these diseases will become a further challenge for an already overstretched workforce.
Meeting this challenge will only be possible through increasing the number and the distribution of trained eye personnel, who are all too often concentrated in the cities in LMICs. In 2000, recommendations were provided on the minimum number of eye healthcare staff required to provide eye care per million population; by 2017, the numbers were still well below these recommendations for most cadres in most countries of Africa. Enhancing the training and skills of eye personnel is the key area in which the VISION 2020 LINKS Programme has been making a difference since 2004.

Figure 1: Some of the participants in the 6.6.2020 Celebration.
Besides increasing the number and distribution of eye personnel, Prof Foster’s message was that services need to be better targeted at needy populations and made accessible to marginalised communities. Improvements were needed at every level of healthcare delivery, particularly primary eye care. Technology could help to address some of these issues if it was used well, e.g. mobile eye health, online training, surgical simulation training and monitoring eye health information.
International Agency for the Prevention of Blindness (IAPB)
On behalf of the IAPB, Simon Day, Regional Programme Coordinator for the Africa region, explained to delegates IAPB’s role in advocating for policies and resources to be directed to increasing access to universal eye health. In 2019 the World Health Organization (WHO) had published the World Report on Vision, which had set out clear proposals to address the challenges [3]. There was a call to action to all partnerships represented at the 6.6.2020 day to ask their heads of state to scale up comprehensive eye care.
VISION 2020 LINKS Programme
Marcia Zondervan and Nick Astbury described the development of the LINKS Programme over the last 16 years. It has resulted in 30 lasting LINK partnerships to help improve the skills of eye care professionals in 13 countries. Out of the LINK partnerships have arisen the opportunity to build Networks – in particular the Diabetic Retinopathy Network, DR-NET [4], and the retinoblastoma network, Rb-NET [5], both established thanks to funding from the Queen Elizabeth Diamond Jubilee Trust [6]. These allow sharing of learning within regions. The ethos of LINKS and Networks is to identify and address the priority needs and then work together as a partnership team, using the skills of a wide range of eye health professionals, to improve eye care.

A slide from the presentation by Barnabas Mshangila and Rosie Brennan about their LINK.
COECSA-RCOphth
LINK John Nkurikiye, the President of the College of Ophthalmology of Eastern, Central and Southern Africa (COECSA), and Mike Burdon, the immediate past President of the Royal College of Ophthalmologists (RCOphth) in the UK, chaired the first session. The COECSA team of John Nkurikiye and Josiah Onyango described the achievements of their 12-year-long LINK partnership with the RCOphth in building expertise in training, Fellowship examinations and institutional development.
The LINK has played a key role in raising the standard of ophthalmology training in the region through the ‘Training the Trainers’ (TTT) programme, delivered over many years thanks to the drive and commitment of the Head of Education at the RCOphth, Melanie Corbett. There are now 120 ophthalmologists in the COECSA region who have undertaken TTT training and are applying their learning in the way they teach their trainees (MMeds). Cascading the training has meant that over 30 COECSA ophthalmologists are now at the higher level of National Lead, Faculty or Facilitator, and are able to lead or assist in locally-run TTT training courses.
Leading the TTT courses for COECSA is Professor Ciku Mathenge, who said that she had recognised the need for training in how to teach others and how to assess her students’ progress. She had attended one of the earliest TTT courses and found it very valuable; her skills grew, as did her involvement in delivering TTT courses, and she had eventually become the head of TTT in the region. Miss Corbett considered that a great deal of learning from Africa had been fed back into the UK TTT programme and it was much stronger as a result. Mr Burdon thanked COECSA for their excellent facilitation of the LINK partnership and expressed the joy he experienced at being part of it.
Learning from LINK partnerships and networks
Demonstrating the vital role of international collaboration, 14 LINK partnerships from across the world and five clinical training networks and projects described their achievements and shared their learning.
Presentations from LINK partnerships in East and West Africa and Indonesia highlighted the varied ways in which having a LINK makes a difference to development of clinical skills and services; the underlying importance of personal friendships between participants; examples of the ways that training through LINKS has been cascaded and shared; and the development of networks for shared learning, south-south, as well as with high-income countries.
Mbeya-N Ireland LINK
From Tanzania, ophthalmologist Barnabas Mshangila presented the LINK between Mbeya Referral Hospital and Altnagelvin Hospital in N Ireland. He described how the LINK had strengthened the eye care services that he and his team provide. Before the LINK began there used to be about 20 patients per week; now they were seeing more than 60 per day. Rosie Brennan, LINK lead for Altnagelvin, said that her eye department had benefited from team-building during their training visits to Mbeya; it was much easier to make changes in working practices at Altnagelvin as the team was more cohesive and understood each other’s strengths and expertise.
DR-NET
Presentations from Nigeria, Malawi, Zambia and St Lucia highlighted how participation in the DR-NET had transformed screening and treatment of DR. In Nigeria, the development of national guidelines for DR services was underway. The team from St Lucia felt that the early involvement of the Ministry of Health had been key to the success of the project. There was now a strong DR programme across the whole island, which was preventing a lot of people from going blind.
Dr Cova Bascaran from the International Centre for Eye Health (ICEH) reported that, overall, across all the participating centres, DR-NET had resulted in an 88% increase in the number of patients screened, and a 40% increase in the number treated over a five year period (2013-18).
Rb-NET A case study of a child patient in Kenya with retinoblastoma was presented by the Rb-NET team (see below).
Concluding remarks and way forward
Peter Holland of IAPB said that VISION 2020 had put eye health on the global agenda and kept it there. Tangible outcomes such as the LINKS Programme and the national eye health committees established in a large number of LMICs were evidence of the enduring achievements of the VISION 2020 initiative. He felt that integrating eye care into mainstream health services was the main challenge for the next 10 years.
Bringing the day to a close, Dr Hannah Faal highlighted the importance of embracing tele-learning and the developments offered by new technology to build sustainable, integrated, comprehensive eye care services globally. While COVID-19 presented problems it also offered opportunities to develop tele-learning, which in turn would have a positive impact on climate change.
Finally, Mike Burdon of the RCOphth reminded delegates of the United Nations 2030 Agenda in which the member states pledged that ‘no-one will be left behind’.
Feedback
A detailed feedback survey was sent out after the Celebration Day, and 298 responses were received. These were overwhelmingly positive. Some examples are:
- How well did the webinar keep your interest? 92% answered well or very well
- How valuable was the webinar to your practice or areas of interest? 84% answered valuable or very valuable
- Are you interested in this international partnerships day being an annual event? 88% answered interested or very interested
This case study is about a child in Kenya who would have lost both eyes, but working together with Rb-NET partners enabled one eye to be saved, with useful vision. The case was featured in the Celebration Day as an example of an multidisciplinary team (MDT) taking place remotely, with input from Rb-NET participants in India, Israel and the UK.
The child was managed at Kenyatta National Hospital (KNH) by Dr Kahaki Kimani and Dr Lucy Njambi, with input from Dr Swathi Kaliki at LV Prasad Eye Institute (LVPEI), India.
March 2018: The child presented at one month old with right eye leukocoria. The right eye had a Group E tumour so it had to be enucleated. The left eye had a Group B tumour. The child was given cryotherapy to the left eye then chemotherapy with vincristine, etoposide and carboplatin.
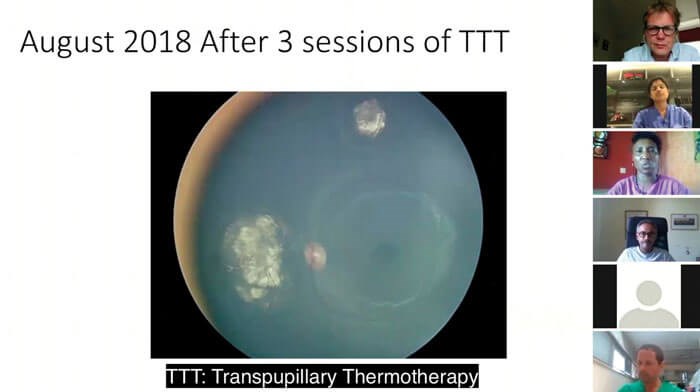
June 2018: After four courses of chemo, the tumour was flat enough for transpupillary thermotherapy (TTT) and the child was given three sessions at three-weekly intervals. A further three sessions were given in August.
October 2018: The tumour recurred and a new tumour was visible. Six courses of chemo were given.
December 2018: Dr Swathi Kaliki was at KNH on an Rb-NET training visit from LVPEI and reviewed the patient with Drs Njambi and Kimani. Swathi recommended completing the six courses.
March 2019: TTT was given to the active area of the tumour.
August 2019: Another recurrence was visible; a further six courses of chemo were given. There was no regression and it was clear that, after 17 cycles of chemo, the tumour had become resistant. It was felt that the only way to save the eye was to refer the child to LVPEI.
March 2020: The child was treated with Ruthenium-106 plaque brachytherapy, giving a 40 Gy dose to the apex. The child was discharged and Swathi plans to review the child during her next training visit to KNH later in the year.
The general feeling of the Rb-NET international multidisciplinary team was the hope that there would be no more recurrences and that this would be end of treatment for this child.
A discussion about the case and the variations in treatment around the world ensued. Ashwin Reddy commented that generally he would only use TTT if there was a relapse after six cycles of chemo, but in this case he might have been more aggressive as it was the only eye. In Toronto they do TTT after every cycle of chemotherapy, so there is variation around the world. In London, if there is a big relapse that TTT can’t control they have the opportunity to use intra-arterial chemotherapy (IAC), but there is increased risk of vitreous haemorrhage if TTT has been done before. They would do more than six cycles of chemo before using IAC, but as this is the only eye there is the risk of visual loss after IAC.
Swathi Kaliki said that at LVPEI they would start focal treatment after the second cycle of chemotherapy. Dr Kimani commented that she was treating three more children at KNH who were in a similar situation; she had treated one of them with intravitreal melphalan and topotecan the previous week and waiting to see the response. One child has a tumour that has been recurring for six years.
Examples of comments from the participants:
“It brought in many exciting perspectives about eye care from top eye care planners and providers across the globe.” – Tanzania, ophthalmologist
“Each project faces its unique challenges, not just us.” – Zimbabwe, ophthalmologist
“It has shown me the importance of working together to fight blindness. We do much more together.” – Kenya, ophthalmologist
“Bringing expertise from different continents to work for the betterment of the community.” – Malaysia, admin / manager
“It was great and enlightening. It also demonstrated how much we can learn without physical meetings.” – Malawi, ophthalmologist
“It was a great celebration of the achievements made in the past years and I appreciated the investments in improving eye care in developing countries and collaboration with partners from various parts of the world. It was nice seeing those behind the successes of the programs.” – Kenya, ophthalmologist
References
1. VISION 2020 LINKS Programme:
http://iceh.lshtm.ac.uk/
vision-2020-links-programme/
2. Link to full recording of the day on RCOphth website:
https://iceh.lshtm.ac.uk/662020-2/
3. WHO launches first world report on vision. World Health Organization 2019:
https://www.who.int/news-room/
detail/08-10-2019-who-launches
-first-world-report-on-vision
4. Astbury N, Burgess P, Foster A, et al. Tackling diabetic retinopathy globally through the VISION 2020 LINKS Diabetic Retinopathy Network. Eye News 2017;23(5):30-2.
5. Williams P, Bowman R, Foster A, et al. Rb-NET: a network to save life and preserve vision in children in Africa. Eye News 2018;24(6):32-4.
6. The Queen Elizabeth Diamond Jubilee Trust:
https://www.jubileetribute.org/
(All links last accessed August 2020)

ACKNOWLEDGEMENTS
We offer our grateful thanks to the key funders of the VISION 2020 LINKS Programme for their support, including the David and Molly Pyott Foundation, CBM, EyeBag Company, Beatrice Laing Trust and Steel Charitable Trust. Without them, none of the achievements of the LINKS Programme would be possible.
COMMENTS ARE WELCOME