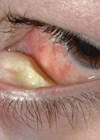
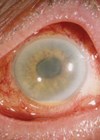
Detection
If you screen for an intraocular tumour, dilate the pupil. If the patient is driving, use phenylephrine only. If the patient declines, document this in the casenotes. Don’t forget to look for sentinel vessels, which would indicate a ciliary body tumour.
Document even typical naevi in the notes. It is not unusual to see a very anxious patient referred urgently to an oncology centre with a tiny naevus, ‘which was not there previously’.
Diagnosis
Never biopsy a conjunctival tumour. If this tumour is malignant, you can cause seeding of malignant cells to other parts of the conjunctiva and the nasolacrimal system, with disastrous consequences.
Remember the features suggestive of small choroidal melanoma:
- Confluent lipofuscin (‘orange pigment’), which shines brightly on autofluorescence imaging.
- Serous retinal detachment, more easily seen with optical coherence tomography (OCT), if subtle.
- Tumour thickness exceeding 2mm (excluding sclera and retina in the ultrasound measurements).
- Lack of drusen on the surface of an elevated tumour.
- Lack of de-pigmented halo around the tumour margins.
Some melanomas are less than 2mm thick and not all autofluorescence indicates lipofuscin. Although melanomas usually have a low internal acoustic reflectivity on ultrasonography, so do some amelanotic naevi, whereas some deeply pigmented melanomas have a very high reflectivity.
If you decide to monitor the lesion yourself, you will never regret having good baseline colour photographs, OCT and autofluorescence images even if it is not possible to perform such imaging at every visit. Follow-up assessments are usually undertaken after four months, then every six months for four to five years, then annually – indefinitely. Patients have been discharged by their ophthalmologist after being followed up for several years only to present months or years later with a large melanoma.
It is surprising how many choroidal metastases are misdiagnosed, even with patients who have had previous mastectomy, lung cancer or other malignancy. Although central serous retinopathy and other conditions do obviously develop in patients with a history of cancer, serious mishaps might be avoided by taking a history in every patient.
It is not uncommon for patients with retinal lymphoma to be treated for uveitis for several months. Similar delays occur with patients having diffuse basal cell carcinoma of the eyelid or pagetoid, conjunctival sebaceous gland carcinoma, who are misdiagnosed as having blepharitis or conjunctivitis.
You may find it useful to refer to www.oculonco.com, an online atlas created to help ophthalmologists diagnose ocular tumours, including lesions they may never have heard of. Unlike other atlases, it orders tumours according to their location and colour.
Counselling
If you find a naevus (or indeed any abnormality), do inform the patient. Say whether it is typical or atypical. If there is any possibility of malignancy, mention this, even if you consider the risk to be very small. Patients get very upset when they find out they were not told about abnormal findings, especially when the ‘naevus’ subsequently turns out to be a melanoma. Just as it is essential to obtain informed consent for treatment, it is equally important to obtain consent for non-treatment.
Always share with the patient your presumed diagnosis. If you’re not sure what the tumour is, don’t be reticent about expressing your uncertainty. Patients will appreciate your candour. Patients complain bitterly when they are referred to an oncology centre without being informed of the possible diagnosis only to discover that their ophthalmologist suspected a malignancy all along.
The importance of breaking bad news sympathetically cannot be overestimated. Give yourself time to do this properly. Watch your body posture. Show compassion and express it vocally. Mute your phone. Invite questions. If the patient is alone, ask whether there is a close friend or relative in the waiting area who could be invited to be present during the conversation. Don’t worry about allowing patients to record the discussion if they wish to do so using their tablet or smartphone. I have been giving patients audio-recordings of my conversations with them for many years, with great feedback. If possible, arrange for a nurse to provide emotional support once you’ve left the room. At least, allow the patient to regain composure in privacy for a few minutes before having to walk through a busy waiting room.
Be sure to advise the patient what to do if an appointment is not received from the oncology centre by a specified time. Some patients are surprisingly patient, possibly waiting many months for an appointment letter they never receive.
Referral
If you refer a patient to an ocular oncology centre after months or years of surveillance, any astute ocular oncologist will want to review old photographs, so you might as well arrange for copies of any useful images to be sent with the referral letter. The images must be of good quality, so don’t bother faxing colour photographs.
Similarly, if you have biopsied or excised a conjunctival tumour, the ocular oncologist will need to arrange for the histology sections to be reviewed by an experienced ophthalmic pathologist. It’s surprising how often the pathology report shows the wrong diagnosis, with conjunctival naevus being mistaken for melanoma and vice versa.
Do not delay the referral because of imaging or other investigations. It is not unusual for patients with uveal melanoma to wait several weeks for liver scans before they are referred to an oncology centre for treatment. Such scans only rarely reveal metastases even when these are present, unless the uveal melanoma is massive.
Treatment
Think twice about attempting to treat a conjunctival melanoma. If you must do anything, follow the no-touch technique and remember to use fresh instruments for closure. The recurrence rate after excision alone is unacceptably high without adjuvant therapy. Never excise a lesion without first photographing it. The ocular oncologist may wish to administer adjunctive radiotherapy, which is more difficult without pre-excision imaging.
Treatment of the tumour is only one aspect of the patient’s overall management, especially if the malignancy is highly lethal. These patients need holistic care, plenty of information and, in many cases, professional psychological support. Increasingly, patients expect to be informed of patient advocacy groups, to benefit from a ‘buddy’ system, to be advised on how to speak to children about their disease, and to be informed of the impact of their tumour on their lifestyle, occupation, finances and relationships. All these needs require resources that are not available in most ophthalmic departments.
“Always share with the patient your presumed diagnosis. If you’re not sure what the tumour is, don’t be reticent about expressing your uncertainty. Patients will appreciate your candour.”
If you are obliged to enucleate an eye with melanoma, before you do so, discuss with the patient the possibility of genetic tumour analysis, which greatly enhances prognostication. Many ophthalmologists feel that there is no point in predicting untreatable disease; however, most patients with uveal melanoma have a tumour that is not life-threatening. Furthermore, with few exceptions, even those with a bad prognosis are glad they were informed of their survival prospects, because they feel empowered to prepare for any eventuality. Patients can be upset when they discover, through online networks, that they were not offered genetic prognostication. Therefore, be prepared to make arrangements for genetic tumour analysis at a specialist centre.
Your patient may want to discuss with you the results of genetic typing of their melanoma, even if these were already explained to them at the oncology centre where the testing was performed. Or else they may have read about genetic prognostication. It is worth remembering that chromosome 3 loss and a class 2 gene expression profile merely indicate that the tumour has metastatic potential. To estimate the survival probability it is is also necessary to consider tumour size and extent, and, if known, melanoma cytomorphology and mitotic count, also taking age and gender into account.
Follow-up
If you are involved in the after-care of patients who have been treated at an ocular oncology centre, expect to spend some time answering questions and providing emotional support every time the patient returns to your clinic.
Be prepared to treat macular oedema, neovascular glaucoma, cataract, dry eye and other side-effects of radiotherapy, or to refer the patient back to the ocular oncology service for specialist care.
If you perform ultrasonography to measure tumour dimensions after radiotherapy of a choroidal melanoma, you can easily obtain spurious readings, mistakenly diagnosing tumour recurrence, if you scan the lesion obliquely. If the tumour is eccentrically located, ask the patient to look in the direction of the tumour when you perform your scan. Be sure to place your caliper on the inner scleral surface, which can be difficult to identify unless the ultrasound beam is perpendicular to the inner scleral surface. Remember that ultrasonography shows measurement variation of +/- 0.5mm, so ignore minor increases in apparent tumour thickness unless sequential scans show a definite trend. Some tumours ‘swell’ for a few weeks after radiotherapy, before regressing.
Screening for metastases from uveal melanoma
Remember, it is rare for metastases to develop in the lung or anywhere else in the absence of hepatic secondaries; therefore, focus on the liver.
Avoid exposing patients to ionising radiation, which can reach dangerous levels over many years. In other words, liver ultrasonography and MRI are preferable to CT scans and PET/CTs.
There is no consensus on what screening test is best, which patients with uveal melanoma should be screened, how often, and for how long. Therefore, you can do no wrong, but you could cause harm.
Informed patients will demand MRI scans, which are expensive but more sensitive than ultrasonography, especially if the patient is obese or if the ultrasonographer is inexperienced.
Take account of the prognosis. If the survival probability is 90% at ten years, then each year the chances of six monthly scans revealing metastases are approximately 1 in 200. False alarms are not uncommon. For these reasons, there is an argument for targeting screening at high-risk patients.
Chest x-rays are unhelpful, and so are liver function tests.
Even with early detection, the treatment of metastases only rarely prolongs life unless the tumour is treated by surgical resection, which is possible in only a minority of patients. However, early detection enhances opportunities for clinical trials, and recent advances are exciting.
Patients with a poor prognosis (i.e. with a monosomy 3 melanoma) derive great benefit from normal screening results, which reassure them that even though metastatic disease is probable it is not likely to develop in the next few months. This helps them to worry less, at least until the next screening test is performed.
A common complaint from patients with uveal melanoma is that they are not given satisfactory advice and information on any lifestyle changes and clinical trials that might improve their chances of survival. Even if there is nothing much to offer it is helpful to discuss this with them or refer them to someone who can do so.
Never assume that a medical oncologist knows much about uveal melanoma, as this is such a rare condition.
Finally
A guiding principle is to treat your patients as you would like to be treated yourself should you ever be in their unfortunate position.
Remember that, even in the privacy of your clinic room, you might be under an international spotlight without knowing it.Patients are increasingly joining societies such as OcumelUK, and, in the US, the CureOM and the Ocular Melanoma Foundation, where they are comparing notes, sharing anecdotes, mentioning names, and highlighting shortcomings as well as excellence in care.
COMMENTS ARE WELCOME