Europe: from the Greek eurus: broad, wide, and ops: eye, face, sight. Thus Europe = the far-sighted (lady).
For my first contribution to this column – as the successor of Jonathan Park, whose witty observations and entertaining style many of us will miss – I have decided to take the opportunity to write on a topic that comes as a given to me, having previously trained in Germany, and help answer the question “How is ophthalmology training done elsewhere and should I set out for some overseas experience?”
When I presented a paper to a German Refractive Surgeons Congress earlier this year I met one of my first and truly admirable teachers in ophthalmology, Professor Maya Mueller, now running a department at a Zurich hospital in Switzerland. She introduced me to a former colleague from Lübeck, Gerd Geerling, who in the meantime had become the director of Düsseldorf University Eye Hospital in Germany.
When I shared my latest experiences as a specialist trainee at Musgrove Park Hospital, Taunton with them Professor Geerling became interested and wanted to learn about all details of my training at the hospital. He became attracted to the British way of training some years ago whilst working at Moorfields Eye Hospital with John Dart and now wanted to give some of his staff involved in teaching the opportunity to experience teaching in the UK, supporting his plan to reform training at his own department back home. We soon realised that the best way to gain a full insight would be a visit to our deanery and two of its teaching hospitals, the Royal Devon & Exeter and Musgrove Park at Taunton.
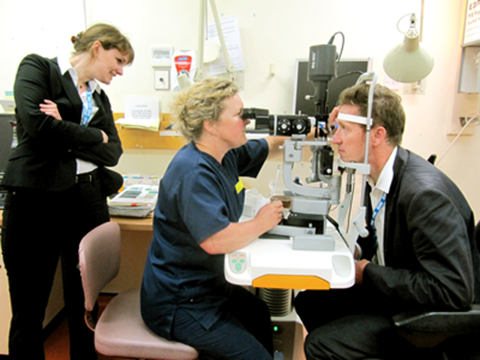
Figure 1: Eva observes the art of how her Professor’s eye pressure is taken by
the lead nurse specialist Jane Kingett (photograph by Prof Rainer Guthoff).
The visit took place recently and Prof Geerling also brought one of his consultants, Professor Rainer Guthoff and a junior, Eva Bramann. We had many opportunities for comparing the ophthalmic trainee programs of the UK and Germany whilst shadowing clinics, engaging in interesting talks and staging assignments (Figure 1). Germany has produced many famous ophthalmologists, such as von Graefe, Axenfeld and Mooren. Still, training in the specialty is less structured than one might expect [1] – see Table 1.

One key factor for the success of UK training that became obvious during the talks is the strong British teaching culture. I remember one patient with a third nerve palsy that I managed poorly during an early on-call session at Taunton, not writing down a clear management plan. The consultant spotted this and discussed it with me (I was indeed ashamed that those notes bore my name). Then, to my great surprise, later that day, she came down from theatres to the eye casualty that I was covering at that time saying “You do the next case in theatre and I will cover for you here in the meantime.” I was puzzled that I should be rewarded for a mistake I made but she explained: “No, it is because you took responsibility for the poor management and showed me that you learned from it by managing future patients better.”
I think that the teaching culture in British eye departments is ultimately made possible by the College overseeing and auditing our training with a vigilant eye. This is what may be lacking elsewhere in Europe where there is no such independent regulating power in place.
If you are interested in gaining overseas experience in ophthalmology I think it is worth considering Germany. This applies especially if you do not have a training number yet and are working hard to improve your CV for that purpose. If you are a research minded person, you could get involved in some research at a German eye clinic (most are university hospitals) and acquire some basic ophthalmology skills at the same time. The time is favourable now as there are many more job opportunities than have been seen for many years, and with Germany coming out top on a BBC poll of the world’s most popular countries (which nearly made us fall off our chairs) it is also a nice place to live.
If your primary goal is to become an eye surgeon, the UK seems to remain one of the most attractive countries to train, as you will be likely to get higher surgical numbers than elsewhere including Germany. However, there are also significant regional variations in surgical training experience across the UK deaneries [1,2].
Let us hope then that ophthalmology training in Europe will live up to the origin of her name and will become far-sighted, perhaps with some inspiration from the UK model.
References
1. Chan WH, Saedon H, Falcon MG. Postgraduate ophthalmic training: how do we compare? Eye 2011;25(8):965-7.
2. Rodrigues IA, Symes RJ, Turner S, et al. Ophthalmic surgical training following modernising medical careers: regional variation in experience across the UK. BMJ Open 2013;3(5).
Acknowledgements:
I am very grateful to all patients, consultants, fellow trainees and nurses who contributed to our Düsseldorf friends’ visit to Exeter and Taunton.
COMMENTS ARE WELCOME








