Children aren’t the best historians. As a result, clinicians sometimes rely on the accounts of parents regarding problems. Missed foreign bodies due to poor histories or incomplete examinations may result in irreversible loss of vision. This case report shines light on a case of a missed foreign body due to it not being deemed necessary to evert the lids to compete the examination, despite reported sightings of a foreign body.
Background
Children have varying capabilities to give histories that are diagnostic. Many present with nonspecific symptoms with a reliance on parental histories to guide examination and management [1]. As a result, clinicians may misdiagnose or not be able to identify foreign bodies. Missed foreign bodies run the risk of causing long-term visual impairment, and even irreversible loss of vision [2]. Literature states the importance of everting the eyelids when examining patients and gives clear advice regarding the procedural steps to be taken but doesn’t specify the indications where this should be applied [3].
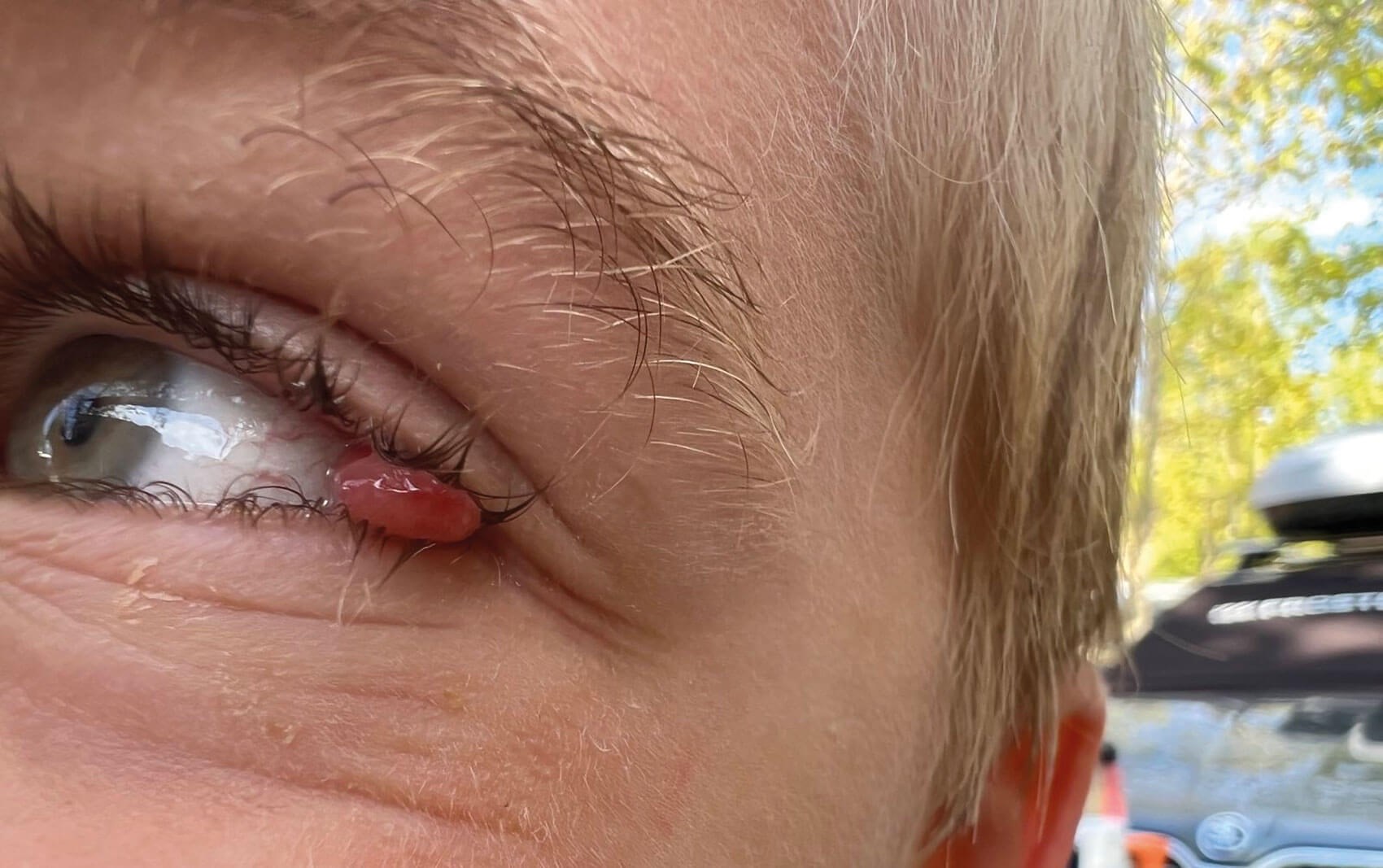
Figure 1: Initial picture taken by parents.
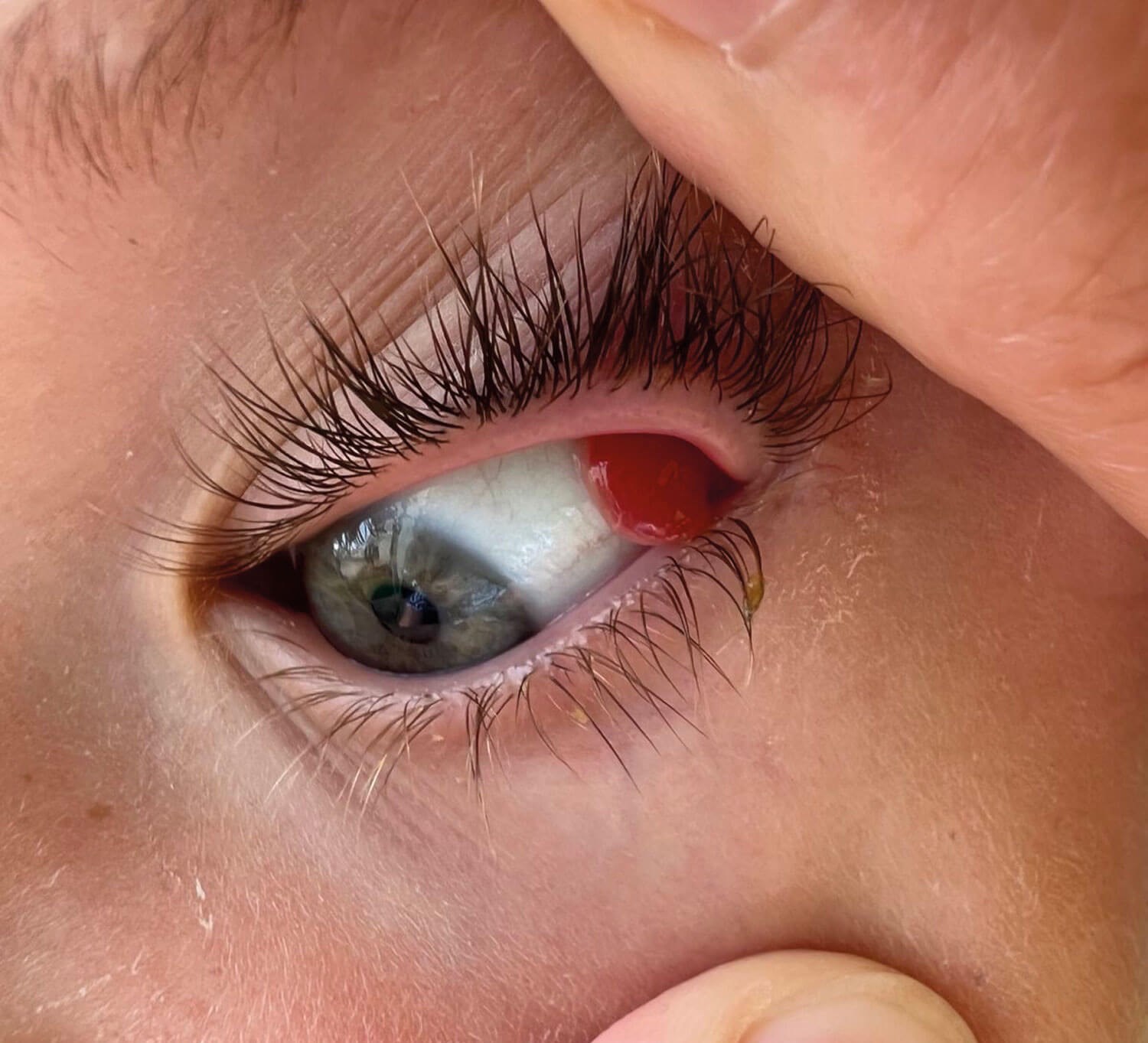
Figure 2: Initial picture taken by parents; upper lid retracted.
Case presentation
A seven-year-old boy presented to eye casualty with a one-week history of a small lump in the corner of his left eye (Figures 1 and 2).
Presenting complaint
The patient woke up with pain one night and the parents reported seeing a foreign object. They attempted to remove it at home, unsuccessfully. They then attended The Bristol Eye Hospital (BEH) and were seen, and, given the symptoms and parent’s concerns, the patient was examined. Documentation reported streaks of what mum thought to be a foreign body, however, the clinic deemed this not the case and felt the symptoms didn’t warrant further examination under the eyelids. After this visit, the family were discharged and the child had no more symptoms.
One month later the family went on holiday to Italy and the patient was noted to have an irritable left eye one evening, causing him to constantly rub it. Earlier that day he had been running through grass / shrubbery. He did not report any worsening pain or blurriness of vision. The eye did not appear excessively red or watery.
The local doctor in Italy prescribed topical Tobradex (dexamethasone with tobramycin) bd and advised the parents to take their son to eye casualty in the UK upon returning from holiday. Differentials included papilloma, conjunctival swelling with granuloma and foreign body.
Past medical and social history: Nil
Medications: Nil
Allergies: Nil
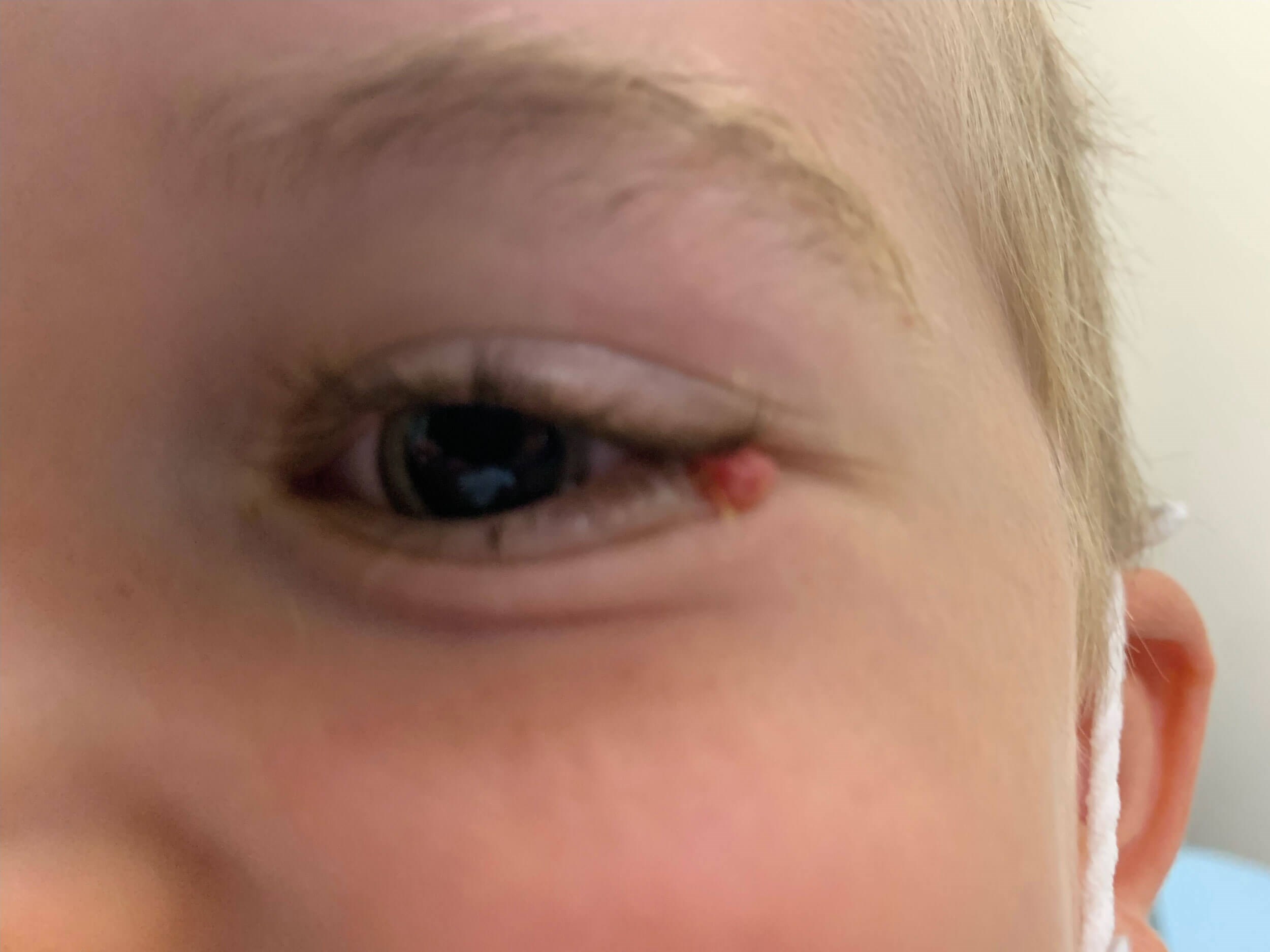
Figure 3: Presentation in ED.
Examination
The boy attended BEH four days later. There was a small red pedunculated solid round lump arising from the temporal conjunctiva in the left eye. The parents reported that this was smaller than the original lump but was still causing some mild irritation (Figure 3).
Right visual acuity: 6/6 (unaided)
Left visual acuity: 6/6 (unaided)
Examination of the cornea, anterior chamber, pupil, lens, vitreous and retina were all unremarkable.
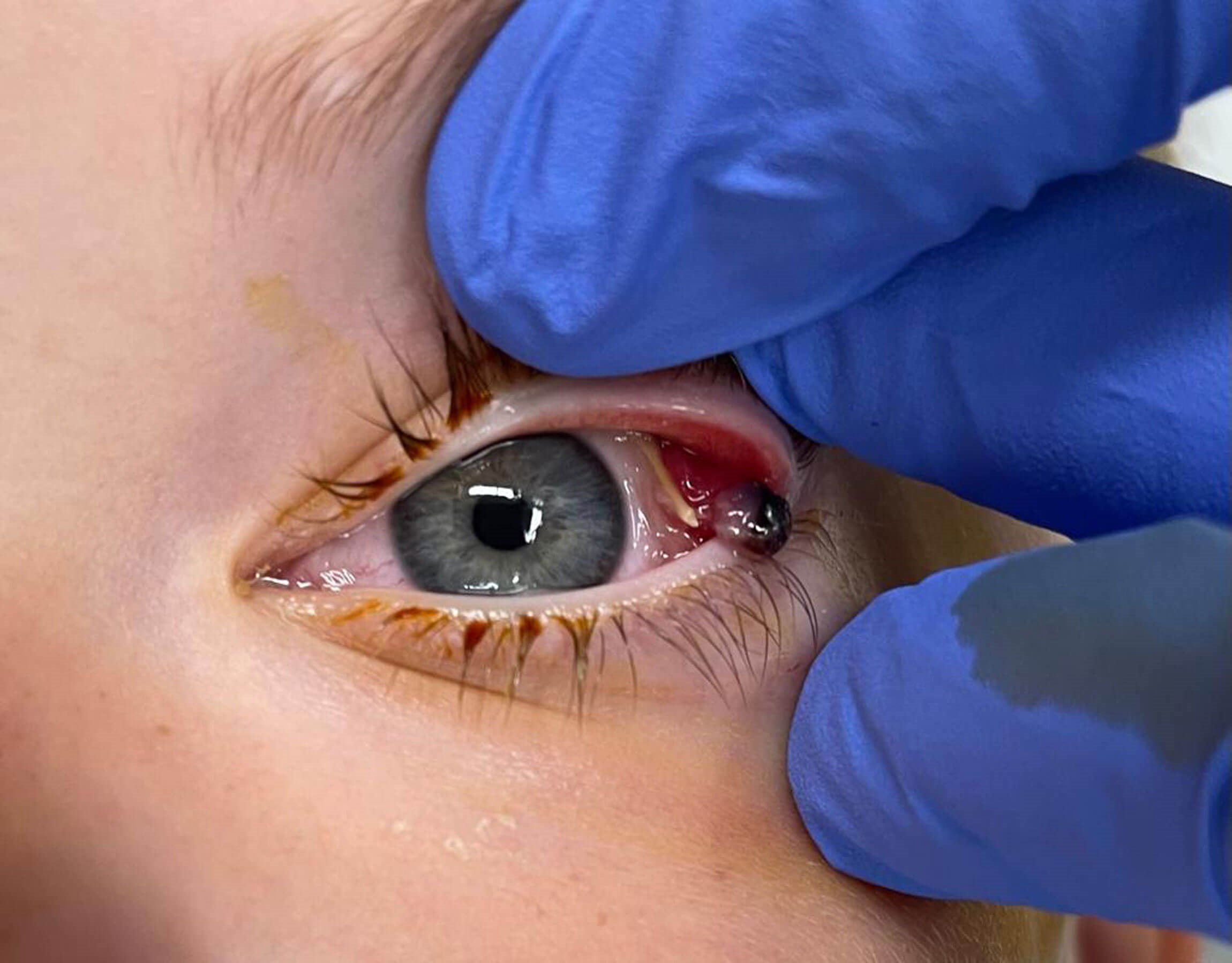
Figure 4: Examination under anaesthetic showing foreign body in upper eyelid and granuloma.
Management and outcome
The following morning the patient was taken to theatre for exploration under general anaesthetic and the removal of the lesion. In theatre, a foreign body (resembling a piece of yellow straw) was found under the upper lid, lodged in the conjunctiva. This was removed (Figure 4). The stalk of the pedunculated lesion had twisted since the previous day and the lump appeared shrunken and partially necrotic. It was easily removed and sent for histology. The upper eyelid was everted to check for any further foreign bodies or abnormalities (Figure 5). Topical chloramphenicol was prescribed for a week, with a follow-up by video consultation planned for two weeks.
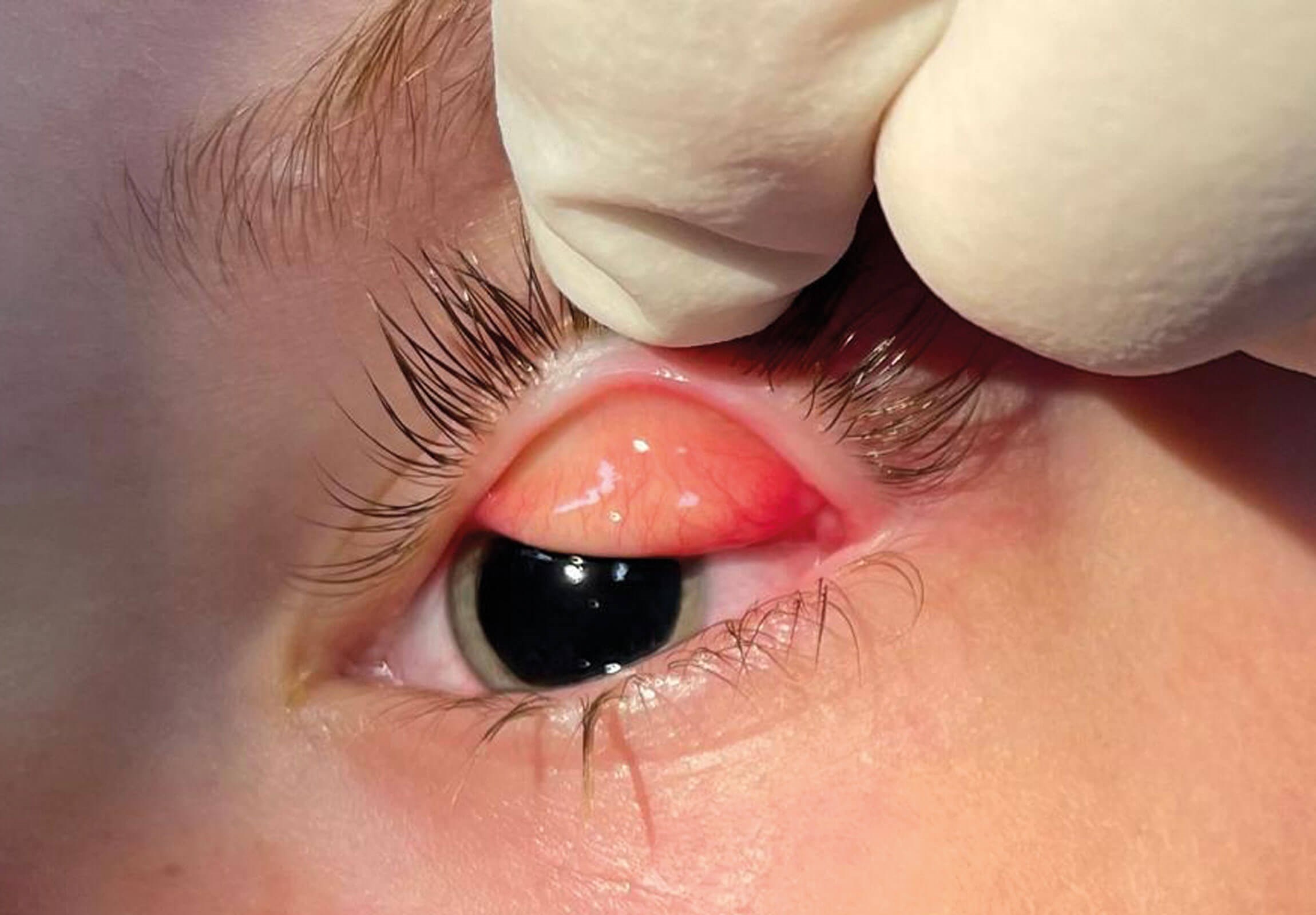
Figure 5: Examination under anaesthetic with upper eyelid eversion.
Histology of the excised lesion showed it to be a pyogenic granuloma. A follow-up video consultation after two weeks found the conjunctiva to be white in appearance, with no residual pathology and the child was completely symptom-free. The parents reported their son had been “fully back to normal” within a few days of the surgery. The child has since been discharged from the hospital service.
Patient experience
The following passage was obtained from the patient’s father (all names have been changed to preserve patient confidentiality):
“In early July, our son woke us in the middle of the night complaining of eye pain. We saw a foreign object and spent a few days trying to remove it at home. Although he would let us inspect his eye, he wouldn’t let us put anything in to remove it. So we attended the BEH to get assistance removing it.
“My wife took our son to the hospital where the doctor dismissed us as fussy parents having caused irritation by looking for something which wasn’t there. A disappointing diagnosis which was later proven incorrect.
“Our son stopped complaining of eye irritation. A month later while on holiday a herniated cyst appeared. We consulted an Italian hospital who recommended treatment at home and suggested palomino virus as the cause, providing treatment. Key to this for us was that it wasn’t in need of emergency treatment, and we had time to head home.
“We returned to the BEH and saw another ophthalmologist who suggested the foreign object was indeed present, and inspection and removal to be sure under general anaesthetic was recommended. We discussed and agreed with the cause of action. Everyone we engaged with this second visit were exemplar in their openness, understanding and supportive behaviours. This was reflected with our son’s absolute composure and self-control during the preparation for the procedure and being placed under general anaesthetic. The procedure was a success and the foreign object we’d described in July was removed.
“I would like to stress that as parents we are absolutely pleased with, and thankful for, our son’s treatment on the second visit to the BEH where the trauma induced herniated cyst was removed.
“Conversely, we are extremely disappointed and displeased that our initial concerns were inappropriately dismissed, and a simpler and less risky cause of action prohibited by judgement of parents and not of appropriate assessment of the patient and their presenting symptoms.”
Discussion and conclusions
It is impossible to know when the foreign body became lodged in this young man’s eye. It may have been whilst on holiday in Italy or prior to his initial visit to the BEH, after which the foreign body may have become lodged and ceased to cause irritation. From this case, clinicians should be reminded of the importance of everting the upper lid in any examination when suspecting a foreign body. Additional measures such as arranging an examination under anaesthesia, should be considered if there is any uncertainty, especially regarding patients who may not be able to provide a focussed history. Had the patient’s upper eyelid been everted upon initial presentation to the BEH and to the hospital in Italy, this lodged foreign body could have been identified and removed, thus preventing the granuloma formation and subsequent conjunctival irritation.
There are reports in the literature of missed foreign bodies, later found through examination of the eyelids under anaesthesia, which have also resulted in new lesions in the eyelids [4]. Additionally, organic matter such as thorns, insect or animal hairs have the potential to cause fulminant endophthalmitis, leading to irreversible reduction in visual acuity and potentially loss of sight [5,6].
Additionally, the use of antibiotic eye drops in this case is likely to have prevented a more severe infection. Clinicians should have a high index of suspicion for foreign bodies in paediatric cases, where children may not be able to identify or communicate the presence of a foreign body [7].
LEARNING POINTS
-
Thorough assessment under the eyelids for patients with suspected foreign body.
-
High threshold for suspecting the presence of foreign bodies in patients who are unable to give you a thorough history or have non-specific symptoms.
-
Early administration of antibiotic eye drops.
-
Send off any lesions for histology to rule out any other causes for their occurrence.
References
1. Jandial S, Foster H. Principles of clinical examination in children. In: Watts RA, Conaghan PG, Denton C, et al (Eds.). Oxford Textbook of Rheumatology. UK; Oxford University Press; 2013:36-48.
2. Ding J, Fernando-Sieminski S, Yoganathan P. Intraocular Foreign Bodies—A Review from Entry to Exit and Beyond. US Ophthalmic Rev 2015;08(02):135.
3. Oke I, McGovern C, Mantagos IS. Eversion of the Upper Eyelid to Evaluate for Foreign Bodies. J Pediatr 2022;249:114.
4. Zhou L, Li SY, Cui JP, et al. Analysis of missed diagnosis of orbital foreign bodies. Exp Ther Med 2017;13(4):1275-8.
5. Gupta A. Intraocular Foreign Body. In: Tripathy K (Ed.). StatPearls. Treasure Island (FL); StatPearls Publishing; 2023. PMID: 35015440.
6.Lee YW, Koh KM, Hwang KY, et al. A case report of fulminant endophthalmitis caused by Streptococcus dysgalactiae in a patient with traumatic corneal laceration. BMC Ophthalmol 2020;20(01):238.
7. Natung T, Shullai W, Lynser D, Tripathy T. A challenging case of a large intraorbital foreign body perforating the nasal septum in a child. Indian J Ophthalmol 2018;66(10):1511-3.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME