As he retires from clinical practice, the author looks back on his long career in uveitis and how care of these patients has changed dramatically since his days as an undergraduate.
My trainees and fellows are often bored by my anecdotes of change in ophthalmology during my lifetime, and one of my oft-repeated claims is that I have been privileged to witness more developments during my career than has any generation of practising clinician before.
A more insightful raconteur would of course realise that each preceding generation of teachers has said exactly the same, and the expectation is that those young ophthalmologists will, in their own dotage, repeat the story. Nevertheless, such acceleration in change, both recent and anticipated, can be bewildering even to the careful observer, and occasionally, a review of what once was, can put into better context the limitless expectations of young ophthalmologists and patients alike. We need to know how we got where we are.
Summers in theatre
I was fortunate, as an undergraduate in the 1970s, to blag my way into summer employment for several years at the Wolverhampton Eye Infirmary, in my home town. Employed officially as a theatre porter on £17.50 per week, my enthusiasm rapidly led me to work in practice as an operating theatre assistant, learning the practical ropes of operating theatre work. Servicing and replenishing the Boyle’s machines (no mains gases then), cleaning the used, Cidex-soaked endotracheal tubes for re-sterilisation (not the favourite job), rolling the laundered gowns for boxing and sterilising in the ‘Big Sister’, and of course the interminable mopping and cleaning, all was grist to the mill. Income was supplemented, at the princely rate of £1 for nights on-call and £2.50 for a weekend.
During those nights, before the successes of seatbelt legislation, I witnessed the steady stream of lacerated faces and eyes, pieced back together in the small hours by the registrars, and learning meantime the sardonic humour which kept doctors going during their (pre-UMT) overtime.
The more refined tasks within the theatre were for the nurses. The careful hand-cleaning, in-house honing and sterilisation of surgical instruments was a religion, and those instruments, all re-used perennially, never left the operating theatre (plus ça change). Woe betide the nurse who had not learned the names so that she could pass to the surgeon when needed. Everything was eponymous: Chavasse, Castroviejo, Barraquer, de Wecker, Lindsay-Rea, Ziegler. The nurses hand-threaded the 4/0 silk retraction sutures for intraocular surgery (three black for the eyelids, one white for the superior rectus); but only the senior sister entered the hallowed ground, the leather-stropping of the Graefe knives which were still then used as an ambidextrous art-form by the most skilful surgeons, the section perfectly limbal, slanted upwards at the exit, and then taking a perfect conjunctival flap; or by the less skilful or unlucky, with capsule impalement, broad iridectomy and haemorrhage.
I remember encountering the downside of uveitis twice in the theatres. The first was the admission of an arthritic child with a mature cataract who underwent discission (which for the younger reader, is a bit like intraocular gardening) and then three subsequent visits for ‘lens washout’ using the Fuchs’ syringe. This large, crude glass instrument was the push-me-pull-you of extracapsular soft lens surgery in the 1970s; fill it with saline, put it in the anterior chamber, push to infuse and aspirate simultaneously, take it out, pull to empty, fill again, repeat. Vitrectomy, amblyopia and probable phthisis awaited. The second, also a child, with an old penetrating injury and sympathetic ophthalmia, underwent examination under anaesthetic with Schiøtz tonometry, loupes and Fison indirect ophthalmoscopy. The verdict – irretrievable blindness, and the ward nurse in tears. The surgeons learned of my ophthalmological ambitions and were generous with their teaching. Observation of those contemporaneous practices (and, dare I say, of the obvious variation in skills demonstrated at the operating table) was invaluable, and I felt, years later when I first grasped a globe with Nettleship’s, that I was better-grounded than my contemporaries (though still terrified – no wet-labs then).
Surgical contortions
Working at one of the academic bookshops in St Andrews was an old retainer, who despite his fixed 90-degree bend above the waist and his permanent stick, managed to carry things here and there, looking up sideways to greet people. As a first-year undergraduate I was mystified. Was it a war injury? It was only later that I met patients with ankylosing spondylitis and realised what his (then untreatable) affliction had been. Working in uveitis, such patients are commonplace, and early on in the clinic, the contortions required to allow slit-lamp examination could be undignified if not comical – the foot in the groin was an occupational hazard. But it was the surgery on such patients that was the real challenge.
I first observed an inferior cataract section for intracapsular surgery on such a patient at Southampton, performed with loupes, and undertook my first of a few later in Manchester, using many pillows, unapproved operating table manoeuvres and supporting assistants, with myself either standing one-legged like a flamingo, or, with the operating microscope wrenched to its most horizontal, sitting temporally in what I called my “easy rider” position. Of course, it was in just these eyes that the cataracts were mature, the posterior synechiae were most widespread, the iris most fragile, and the need for smooth, ‘atraumatic’ surgery most acute.
I look back on these cases with a mixture of nostalgia and horror, and think now that the huge strides made in rheumatology firstly with the widespread use of better immunosuppression, and then with biologics, has revolutionised this population; it is now rare to see anybody with spinal immobilisation; we still see wheelchairs, but they are rarely arthritic patients, and surgical contortions are very uncommon.
Cataracts – to implant or not?
All the Wolverhampton cataract patients were left aphakic. During my training in the early 1980s, it was the time for experimentation; every conceivable design of intraocular lens (IOL) was being attempted after intracapsular surgery: Choyce IX was de rigeur in Southampton (the lens, unlike 6-up the fizzy drink, never quite made it to the acceptable level) with a few Binkhorsts; in Manchester, Boberg-Ans, the awful Severin, and the short-lived cornea-bouncer, Novoflex. It was a time of glorious, unfettered development, with “a hatful of eyes” going on to corneal decompensation, Uveitis-Glaucoma-Hyphema Syndrome (UGH) and beyond.
At this time, the more sensible surgeons realised that eyes with uveitis were no-go areas for IOL implantation; after all, look at the way they behaved after ‘standard’ surgery: broad iridectomy, chymotrypsin injection, 8/0 virgin silk sturing; even then they often filled up with fibrin, formed vascularised pupillary membranes and became phthisical. However, a few were unable to resist (usually selecting patients with Fuchs’ uveitis because they were ‘straightforward’); iris-sutured IOLs bounced around in uveitic eyes and were sometimes declared in print to be successful after short follow-up. Later after UGH, the IOLs, or sometimes the eyes, were removed. In my first years as a uveitis consultant I removed many IOLs from pre-phthisical eyes, the patients much better aphakic.
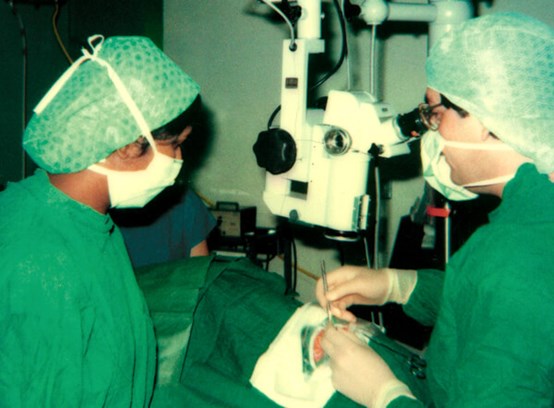
Figure 1: NPJ operating, 1985-style. Re-used gowns and drapes, wheeled microscope.
In time the general developments in cataract surgery assisted uveitis patients greatly. The move ‘back’ to extracapsular surgery in the mid-1980s (Figure 1 – this time with microscope, red reflex, heparin-coated IOLs in the sulcus, safer and complete aspiration, and 10/0 nylon) allowed for the first time a much safer technique, even when pupillary membrane division and iridectomy were still needed. Marinading in steroid before, during and after became the norm and the uveitis world evolved from aphakia to pseudophakia. This phase passed quickly and by 1993 I had converted to scleral-tunnel phako for 90% of uveitis patients. The move to smaller incisions, corneal incisions, second generation machines (a breath of fresh air, this), iris hooks and foldable acrylic IOLs were together the developments that now allow one to say to patients awaiting surgery that the outcome, with adequate inflammation control, is likely to be as good as that of any cataract operation. Again, some go too far – no multifocals yet, please!
The debate now rages about those uveitis patients most likely to do badly after IOL implantation – the children with juvenile idiopathic arthritis (JIA)-associated uveitis. Cautious surgeons are still leaving these children aphakic and considering secondary implantation after the disease is quiescent; the ‘brave’ are claiming that adalimumab is the ultimate protection, and are implanting many. And now sometimes we are having to explant these IOLs from children under 10. Plus ça change, plus c’est la même chose.
Uveitis and glaucoma
The story in uveitic glaucoma is a virtual mirror of that in cataract surgery. In the 1970s there was pilocarpine, guanethidine / adrenaline and acetazolamide, followed by scleral trephining or iridencleisis, with high complication rates, early failure and occasional sympathetic ophthalmia. The evolution of topical medication benefits all glaucoma patients, but surgical technique improvement, with trabeculectomy enhancement (in Manchester, using Strontium90, too rapidly abandoned, elsewhere 5FU) increased bleb survival rates in the high-risk, and uveitis was and is the highest risk. Young uveitis patients are the paradigm for those most needing drainage tubes and very intensive perioperative management, and centres such as ours with high experience and two consultants with particular expertise in uveitic glaucoma surgery, have pushed bleb survival from the adequate to the impressive. Recently, the microinvasive glaucoma surgery (MIGS) implants have appeared like a Cambrian explosion, and although many will disappear into a similar evolutionary cul-de-sac, others offer major steps forward.
In Manchester the Xen45 gel stent has had such dramatic (and surprisingly enduring) success in emergency uveitic glaucoma that cyclodestruction is bordering on extinction, and newer MIGS implants show great promise in this difficult group of patients. My old friend Peng Khaw, in naming his 10-10-10 challenge for world glaucoma (a post-op intraocular pressure of 10mmHg, lasting for 10 years, achieved in a 10-minute operation) surely did not have uveitis patients in mind, yet we may have this target in sight even for this most at-risk group.
Infective uveitis
In the mid-1980s we were dealing with the AIDS epidemic in the cities, and the early antiretrovirals, inadequate and toxic, were merely prolonging the dreadful decline, so that in addition to cytomegalovirus (CMV) retinitis (which came with a mean eight-month life-expectancy) we were also seeing pneumocystis, cryptococcus, other strange fungi and aggressive toxoplasmosis in the eye. The introductions firstly of protease inhibitors, and then by degrees, the drug combinations that evolved into highly active antiretroviral therapy (HAART), were transformative. In 2020 we share the care of many HIV+ patients with our infectious disease colleagues, and still deal sometimes with sight-threatening disease (mainly in the self-neglected), but do so entirely in the context of long-term disease management, and nowadays, the blinding CMV disease is almost always in the iatrogenically immunosuppressed: the organ (particularly lung and marrow) transplant and severe lupus patients.
But every silver lining has a cloud. The MSM community in particular, emerging from two decades of terror of an early death from AIDS, became less careful. From 1999 onwards, an enormous surge of other sexually-transmitted diseases arose in new epidemics in all the major cities of Europe and America. Manchester was in the vanguard, being christened by the BMJ in 2004 as “The Syphilis Capital of Europe”. In the uveitis clinic, we rapidly learned the techniques of diagnosis and treatment that our elders had forgotten, and the management of ocular syphilis (immensely satisfying, as if diagnosed early, it is curable with minimal legacy) is now a regular feature.
Other infectious diseases too have evolved in the uveitis clinic. Read Duke-Elder and find tuberculosis (TB) every few pages, but the gradual decline in incidence during the twentieth century began to reverse at the turn of this one. Immigration from TB-endemic countries, mycobacterial resistance, better diagnosis and the appearance of newly-recognised ocular manifestations (including atypical serpiginous / placoid chorioretinopathy) led to a substantial increase in diagnosis and treatment and now once again, ocular TB is regularly diagnosed and treated in the uveitis clinic. Globalisation has also introduced even the temperate Western world to the ocular manifestations of tropical and bizarre diseases; we need nowadays to be aware of diffuse unilateral subacute neuroretinitis, Dengue, West Nile and rickettsial uveitis amongst returning travellers.
New investigations, new treatments
The introduction of any new effective diagnostic technique is so immediately accepted into clinical practice that it is easy to forget what it was like before. Anybody using azathioprine in many patients deals with the occasional frisson caused by a neutrophil count of zero, but pre-treatment thiopurine methyltransferase testing has now removed a substantial part of that life-threatening risk. Polymerase chain reaction testing for microbes is now such a routine part of uveitis practice that it is forgotten how, based upon sometimes unreliable clinical acumen, empirical treatment was often used either with clinical response as the only diagnostic method, or while awaiting chicken egg-sac viral culture. Cytology of intraocular specimens, previously entirely a morphological and stain-based interpretation, is now performed with a myriad of cell markers.
The nightmare of late-diagnosed vitreoretinal lymphoma is ameliorated by the ability to find Myd-88 and IgH gene mutations and IL-10. Beta-2 microglobulin assists in tubulointerstitial nephritis and uveitis syndrome diagnosis, and finding anti-retinal antibody identification is becoming more widely available for suspected autoimmune retinopathy. One sometimes wonders where clinical acumen will be needed in future uveitis practitioners.
The two changes that have most improved the lot of the uveitis patient during my career have been firstly, the expansion of uveitis expertise, and secondly, the substantial improvements in treatment quality for non-infective uveitis. In 1991 the specialty was a rare indulgence within understaffed eye units. A mere handful of enthusiasts, mostly in the university departments, were the forerunners in the UK. Now, some 30 years later after expansion, increasing subspecialisation, mandatory curricular uveitis training, the increasing availability of high-quality educational courses and a change in referral patterns to specialist units, there are about 70 ophthalmologists in the UK practising in the field. These changes have been mirrored internationally: the expansion of the International Uveitis Study Group (IUSG), the leadership of IUSG and others in collaborative multicentre studies and the worldwide improvement of teaching in the subject have made access to expertise easier than ever before.
The second change, not unassociated, is the improvement in medical management. High-dose systemic steroid may remain the mainstay of treatment initiation for sight-threatening non-infective uveitis, but rapid replacement with well-supervised immunosuppression, and the greater availability of biologics (state funding in England provoked by the superb VISUAL I, VISUAL II and SYCAMORE studies led by Andrew Dick), has not only improved the visual lot of patients, but has spared them the burden of long-term steroid and immunosuppression complications. Anti-TNF biologics have now been on the scene for 20 years, and rheumatology has been transformed by them. This effect transfers to juvenile uveitis, where with earlier immunosuppression and biologic treatment, blindness is now extremely rare compared to only 30 years ago. In adults, those with awful emergency panuveitis can often be ‘switched off’ by infliximab, far fewer being exposed to the toxicity of cyclophosphamide. Knowledge accumulates on the next generation of monoclonal antibodies – we now seek funding for tocilizumab (already used in JIA uveitis) for recalcitrant inflammatory macular oedema; anakinra may rescue the cryopyrin-associated autoinflammatory diseases; rituximab is occasionally transformative in both uveitis and scleritis. In the meantime, new biologics emerge almost weekly, and the future for tailored, rather than off-the-peg management, is exciting.
Intraocular steroid usage in uveitis patients has become absolutely routine, but the search for the Goldilocks molecule and method (not too short-lasting, not too much glaucoma please) continues. We have moved away from repeated periocular methylprednisolone lasting four weeks, via intraocular triamcinolone and dexamethasone implants lasting three months and more, to the fluocinolone implant which promises less intrusive management for the patient with chronic disease. Yet the perfect injection – just the right effect, for as long as you like – is yet to come.

Figure 2: The International Council of Ophthalmology / International Uveitis Study Group
Uveitis Course participants, Venice 2019 (NPJ at back left with Justine Smith and Manfred Zierhut).
As I leave the world of clinical uveitis, I look back with satisfaction on three things: firstly, that the Manchester Uveitis Clinic, inaugurated by myself nearly 30 years ago, is now internationally recognised and amongst the busiest in the world, with four consultants ably led by Laura Steeples; secondly, that my contributions to uveitis teaching and training have been useful to many both here and abroad (Figure 2); and lastly and most importantly, that our ex-fellows are now contributing substantially to uveitis in the UK, in Europe and beyond. I leave clinical practice with envy that I shall only be observing the inevitable future improvements in uveitis care from the outside.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME






