Madagascar is a fascinating and culturally rich island which has an ‘exotic’ status in most people’s eyes. Yet it is among the poorest countries in the world. According to the World Bank, 92% of the population live on less than $2 per day [1]. Moreover, until recently, the country was fraught by years of political instability, which served to compound the economic crisis and worsen the health of the nation.
Madagascar identified that it needed support to implement its national VISION 2020 Plan. It is estimated that 160,000 (~0.75%) of the population in Madagascar are blind (best corrected visual acuity of < 3/60 in the better seeing eye). Many more suffer from preventable visual impairment.
Madagascar-Leeds VISION 2020 LINK
The Madagascar-Leeds VISION 2020 LINK was inaugurated in 2008 under the auspices of the VISION 2020 LINKS Programme, run by the International Centre for Eye Health (ICEH) [2] and supported in Leeds by the Overseas Partnering and Training Initiative (OPTIN) [3]. Over the last seven years, our exchange training visits have helped to establish a strong and trusting rapport between our department in Leeds, the Malagasy Ministry of Health, the main government teaching hospital in the capital city – the Hospital Joseph Ravoahangy Andrianavalona (HJRA) – and a faith-based hospital eye unit, SALFA Hospital, Ambohibao.
As with all health partnerships, the priority objectives for the LINK as a tool in developing eye care were identified and defined in a Memorandum of Understanding. Key activities over each three-year period were agreed by the partners and formulated into a timetable of activity (Activity Plan).

Audit meeting in HJRA.
Earlier exchange visits in both directions had achieved a number of goals, including implementation of the World Health Organization (WHO) safe surgery guidelines, development of the paediatric and oculoplastic service, and audit of clinical and surgical outcomes.
In April 2014, as part of the seventh Madagascar-Leeds VISION 2020 LINK visit, two eye care teams from St James’s University Hospital, Leeds, visited the ophthalmology department of Antananarivo, Madagascar. The first team comprised Vernon Long, Consultant Paediatric Ophthalmologist and Lorna Pankethman, Senior Orthoptist. Their aim was to strengthen the existing paediatric ophthalmology service in Antananarivo, specifically with reference to standardisation of paediatric vision testing and use of Bjerrum visual fields.
A month later, John Buchan, Consultant Ophthalmologist and Aditi Das, ST3 Ophthalmology Registrar, visited. We carried out a number of training courses including an intensive two-day programme on sutureless small incision cataract surgery (SICS), and facilitated the first round of a departmental cataract surgical audit, along with preparing for repeated audit cycles.
Arrival
We arrived in Antananarivo in the early hours of the morning. After what could only be described as a ‘power nap’ we were greeted by the Ministry of Health lead, Dr Hery, who escorted us to the HJRA, where we met the entire ophthalmology team. We were warmly welcomed and as we outlined our mutual aims, we were pleased to hear that the trainees were keen to develop their surgical skills and take the lead in the proposed audit projects.
Case Study
This 65-year-old lady was found in a village in the North West of Sierra Leone by an outreach team from the capital, Freetown. With bilateral perception of light vision she was unable to contribute to the family by caring for children, as would be her traditional role; she herself required looking after instead.

Sutereless extra-capsular cataract extraction allows us to bring her into the regional surgical centre, operate on one eye the next day, and the other the following day, then send her home after another 48 hours observation. National settings which rely on “hub and spoke” type arrangements of surgical service provision, such as also seen in Madagascar, have greatly benefitted from the transition to sutureless surgery with the faster visual recovery, more reliable refractive outcomes and lack of need of future follow-up or suture related problems.
Cataract surgery
Quantity
Addressing cataract-related blindness has been one of the priorities of the global initiative ‘VISION 2020: The Right to Sight’. Prior to our arrival, the Ministry of Health and the ophthalmologists in HJRA had expressed a desire to increase their cataract surgical rate or CSR (the number of cataract operations per million population per year). Whilst it is recognised that sub-Saharan African countries need to have CSR rates of about 2,000 to address their levels of cataract blindness, actual figures are much lower. Figures from the Ministry of Health suggest that the CSR for Madagascar is around 350. No doubt a reason for the low CSR is the cost of cataract surgery, which despite subsidy, costs patients $25 (equivalent to two-week’s salary for an average person), a large part of which is due to the cost of sutures.
The ophthalmology team at the HJRA are a motivated group of professionals who are dedicated to improving their outcomes. In particular, they were keen to build their confidence in performing SICS in order to improve the quality and quantity of cataract surgery. We facilitated a two-day intensive SICS training course. This was led by John Buchan, who was able to share his skills gained while working as an ophthalmic surgeon in Sierra Leone for CBM. In the SICS course, Mr Buchan supervised the ophthalmic surgeons on a one-to-one basis, providing constructive feedback and practical advice.
Most of the surgeons had had some prior experience with SICS, and a two-day refresher training was successful and well-received. We were also able to provide additional written and video training materials including copies of the Community Eye Health Journal and a SICS video [4,5].
As a result of this pilot course, we have secured a grant to facilitate a five-day SICS course (consisting of one-to-one surgical training, complemented by interactive lectures) to be carried out in Madagascar in April 2015.
Quality
Whilst our aim was to promote an increase in the CSR, it was clear that a focus was also needed on the quality of existing surgery. One of the prime objectives of our visit was to facilitate an audit of refractive and visual outcomes following cataract surgery, using the WHO benchmarks. While the concept of audit is not widely practised in many low-resource settings, we were impressed that the ophthalmologists in HJRA engaged enthusiastically with the process. They presented their findings at the departmental meeting and have arranged re-audit of their surgical complication rates this year.
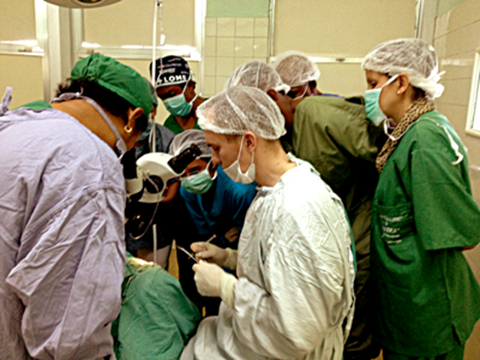
Training in small incision sutreless cataract surgery (SICS).

Ophthalmologists engaging in leadership training.
Leadership training
Many of the challenges that hinder the delivery of eye care in Madagascar could be minimised through effective leadership. Leadership training has been identified by the VISION 2020 LINKS Programme as a way of helping to build capacity in overseas eye departments to develop eye health systems. The LINKS Programme has established a leadership course to provide training and support to develop the expertise of eye specialists overseas. Aditi Das attended the one-day workshop at ICEH before the visit to Madagascar. As leadership ‘facilitators’ we were provided with a toolkit to engage people with the concept of leadership.
During the visit the team provided leadership training to the ophthalmology and rehabilitation doctors at HJRA. What had seemed fairly straightforward in London became less so in Madagascar. Translating leadership theories in English let alone French can be surprisingly tricky. Nevertheless, we were amazed by how enthusiastically the department came together in order to develop their leadership skills and strengthen their respective roles in the department.
Outreach programme
Perhaps the most memorable experience during the visit was the paediatric outreach clinic with SALFA. Aditi Das joined the team during one of their community clinics outside the capital.
Starting in the early hours of the morning, the eye care team comprised a doctor, two refractionists and an orthoptist from SALFA, and Aditi Das. We were driven to a school hall where the local elders greeted us eagerly. The outreach programme had been advertised for months and there were over 100 children waiting obediently in the courtyard as our van pulled in.
The team quickly organised themselves within the space that was allocated. We set up four examination areas; two refraction stations and two clinical areas. In another room, a makeshift pharmacy was opened to provide patients with drops or arrange follow-up if required.

Key informant training to recruit patients for cataract surgery.
The challenges of working in a resource-poor setting soon became apparent. The team relied only on their clinical judgement and limited tools (a direct ophthalmoscope, a retinoscope and a small supply of dilating drops). It was a steep learning curve, without the diagnostic tools we are accustomed to in the UK. As well as frustration at the lack of equipment, it was sad to see the futility of some of the cases. Many of the children were farm workers who had sustained ocular traumas which had already rendered them amblyopic. Others with active disease such as corneal ulcers were referred to the government hospital, but their fate was likely to be equally bleak, due to the well-known barriers in accessing healthcare.
Overall, the experience was entirely humbling. The SALFA ophthalmology team were a wonderfully dedicated unit who worked hard to provide eye care among marginalised communities. The following day, the manager of the team took us to a village 40 miles outside Tana in order to carry out key informant training [6]. This is an awareness-building method in low-income countries, whereby respected community members are educated about ocular health and subsequently play a fundamental role in bringing patients with visual impairment and blindness to health services. The scheme is playing a vital role in reducing the burden of visual impairment in low-income settings.
VISION 2020 LINKS
The Madagascar-Leeds VISION 2020 LINK has acted as an important vector for change and eye care development, both in Leeds and Madagascar. Over the years, our LINK has led to positive change in the partner hospitals; notably implementation of the WHO checklist, patient consent and safe surgical practices at HJRA. Visits of the Malagasy ophthalmologists to Leeds have strengthened our relationship and allowed the mutual exchange of knowledge and expertise. In Leeds, our LINK with Madagascar has prompted us to work towards sustainable practice in healthcare and still provide excellent patient care. The next training visit will take place in spring 2015.
References
1. Madagascar: Measuring the Impact of the Political Crisis. World Bank.
http://www.worldbank.org/en/news/
feature/2013/06/05/madagascar-
measuring-the-impact-of-the-political-crisis
Last accessed October 2014.
2. International Centre for Eye Health.
http://iceh.lshtm.ac.uk
Last accessed October 2014.
3. OPT IN (Overseas Partnering and Training Initiative).
www.optin.uk.net
Last accessed October 2014.
4. Community Eye Health Journal.
www.cehjournal.org
Last accessed October 2014.
5. Sutureless Extra-capsular Cataract Extraction (SECCE). ICOpedia: Video and Lecture Center. http://icopedia.ophthalmologyblogs.org
/2012/02/29/sutureless-extra-
capsular-cataract-extraction-secce/
Last accessed October 2014.
6. Key informant method Africa. International Centre for Eye Health.
https://iceh.lshtm.ac.uk/
research-activities/key-informant-method-africa/
Last accessed October 2014.
Acknowledgement
We acknowledge the support of the Four Acre Trust and OPTIN for funding training visits, and the support and advice of the VISION 2020 LINKS Programme and THET.
COMMENTS ARE WELCOME