The Lead Forward project was an initiative of the VISION 2020 LINKS Programme, funded by the Department for International Development (DFID) via the Tropical Health Education Trust (THET). It aimed to improve the quality of medical leadership within VISION 2020 LINK hospitals, and to strengthen LINK partnerships. The project began with a bespoke three-day workshop in Manchester in 2015, designed by Amy Brockbank and Clare Inkster, which trained eye health workers from 12 LINK partnerships in seven different countries [1]. The impact of the training is measured through participants’ implementation of their skills through cascade training workshops and quality improvement projects [1].
This article describes how Lead Forward training was implemented in the UK, Kenya and Uganda, and includes case studies arising from the workshops.
1. UK experiences: LSHTM PhD students’ workshop
In October 2015, Denise Mabey and Nyawira Mwangi cascaded the Lead Forward workshop to PhD students at the International Centre for Eye Health, London School of Hygiene & Tropical Medicine (LSHTM). The eight students who participated were from Sub-Saharan Africa and Southeast Asia. The group was heterogeneous in terms of prior experience with facilitation, leadership and quality in healthcare. The theme was leadership in research, the rationale being that leadership is crucial to ensuring that research is carried out effectively. Feedback from this workshop showed that the participants’ confidence in facilitation had increased.
“I am empowered…I realise one person in an organisation can make a big difference.”

Participants practising coaching skills at the COECSA workshop, Nairobi.
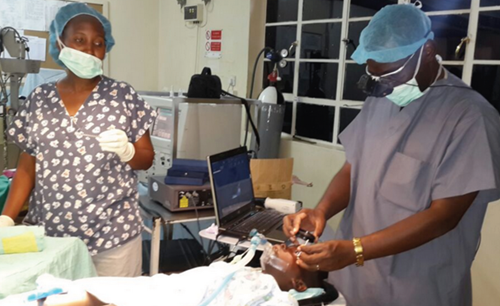
Lucy Njambi and Dr Charles at Kikuyu.
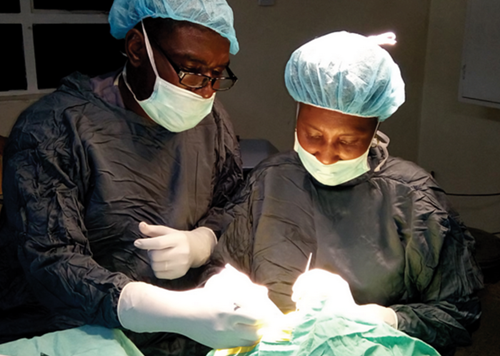
Retinoblastoma fellow Dr Charles in a theatre session at Kikuyu with Dr Kimani.
Participants from the infection control team with Dr Doreen Birabwa-Male and the facilitators, Kampala.
Graduands of the leadership training march to the ceremony.
Values of Bushenyi HC: Quality, Teamwork, Transparency and Customer Care.
2. Kenyan experiences: COECSA workshop
In January 2017, 14 ophthalmologists from eight countries of the College of Ophthalmology of Eastern, Central and Southern Africa (COECSA) attended a Lead Forward workshop in Nairobi facilitated by Simon Arunga, Clare Inkster and Marcia Zondervan. The workshop focused on leadership skills and mentorship training. Participants were asked to think of a word associated with leadership at the start of the course and then again at the end. The answers showed a marked difference in the themes used to describe leadership. ‘Responsibility’ and ‘being in charge’ were the strongest themes at the start, changing to ‘emotion’ and ‘tools learnt’ after the course.
All participants were encouraged to deliver a quality improvement project after attending the course. Participants were enthusiastic with regard to impacting leadership and quality in their institutions.
“I’ve learnt that…leadership is done best when working as a team.”
3. Ugandan experiences: Infection control team workshop
In Kampala, Nyawira Mwangi and Clare Davey delivered a Lead Forward workshop to the infection control team at Mulago Hospital. The workshop had been requested by the hospital Deputy Executive Director, Dr Doreen Birabwa-Male, having observed the positive impact of the first cascade run by Grace Ssali and Clare Davey. Feedback was positive from the participants who attended.
“I was taught how to respond to challenging behaviour and troubleshoot.”
Case study 1: Quality Improvement Project – retinoblastoma management in Kenya
Lucy Njambi, Consultant Paediatric Ophthalmologist and Lecturer, University of Nairobi.
The problem
The national retinoblastoma care centre at Kenyatta National Hospital (KNH), the largest teaching and referral centre in Kenya, was grounded due to the doctors’ strikes that started in December 2016 and continued until March 2017. This led to interruption of care of patients with retinoblastoma. Lacking the doctors to continue providing retinoblastoma care was a huge barrier to overcome. The protracted strike caused despair to patients, their parents and doctors. Temporarily transferring the retinoblastoma services to Kikuyu, a mission hospital approximately 30km away, would allow access to theatre space and staff.
The project
I organised a meeting with the head of the eye department and wrote to the CEO of Kikuyu Hospital asking for one theatre slot a week. Having a good working relationship with Kikuyu and the dedication of the retinoblastoma team greatly enabled our cause. Once the proposal was accepted, travel logistics were organised with funding from the National Hospital Insurance Fund (NHIF) to transport patients and their families to Kikuyu. Eight to 10 services a week were provided including examinations under anaesthesia, enucleation, globe salvage therapy (laser, cryotherapy, intravitreal chemotherapy) or referral for systemic chemotherapy.
The outcome
We still encountered difficulties, including being reliant on the host team and anaesthetists to run theatre sessions. These could be cancelled at short notice and we were unable to contact parents in time to re-organise transport. The lack of chemotherapy at Kikuyu was an insurmountable challenge. Furthermore, providing services was seen by some colleagues as going against the spirit of the strike. Despite the issues, 30 children are now on follow-up for salvage therapy carried out at Kikuyu. All new cases of retinoblastoma that have presented during the strike period have been seen and a management plan has been instituted. We have also managed to complete the training of a retinoblastoma fellow from Congo.
Personal learning
Attending the Lead Forward workshop was important for me to gain a better understanding of leadership in order to apply it to improve patient care. I learnt that anybody could be a leader and how my personal values made an impact on leadership. It gave me the skills and confidence to apply these values and I learnt about the greater impact I can make when leading from within a team.
Case study 2: Cascading the training – rural healthcare worker training in Uganda
Viola Ninsiima, Doctor in charge of a health centre in Bushenyi, Western Uganda.
The problem
The enormous workload and stress meant that staff were demotivated and relationships were poor. Viola said: “When you study medicine, you don’t get leadership training, yet you are immediately in a leadership position. You have responsibility for human resources as well as clinical duties. The people around me also lacked leadership training and skills. I felt that if I wasn’t in the facility, people didn’t do their work. Patient care was suffering.”
The project
Viola’s husband, Simon Arunga, is an ophthalmologist in Mbarara and, as part of the VISION 2020 LINK with Bristol, had jointly facilitated a Lead Forward workshop with Miranda Buckle. Simon felt that the Lead Forward workshop would help Viola and her colleagues. Nine people attended – a multidisciplinary group comprising Viola and eight heads of section within the facility. As part of the workshop, each developed a project that would improve healthcare delivery (a quality improvement project). Following the workshop, Simon visited the facility once a month to mentor the staff. All nine section heads completed their projects and in November 2016 a celebration was held, showcasing the improvements and handing out certificates.
The outcome
After the Lead Forward workshop, the staff immediately took on board the facilitation skills they had learnt. Their interactions changed from being aggressive to being positive and supportive. Viola says: “They are all more confident in themselves and their roles and take pride in their work.” The Lead Forward workshop included a video about a fatal medical incident that had occurred in real life [2]. Viola said: “Everyone was touched by the video and it generated a lot of discussion. The nurses now feel empowered to challenge bad practice, something they had never done before. They have embraced the responsibilities of their roles and changed their attitudes to work.”
The facility staff team has recently been invited to seek funding for essential equipment. The team has also set up a screening programme for key diseases, including TB and dysentery, in the population. This outreach activity has never taken place before. The key to this success has been the sharing of responsibilities and clear accountability for specific tasks and roles amongst the team, empowering them to carry out their work confidently.
Personal learning
Viola reports that she is now able to be honest with herself about her own strengths and weaknesses. She is more self-confident and feels empowered and capable of fulfilling the expectations of the senior staff of the municipality. Viola’s leadership skills led to invitations to join three health committees.
Participant reflections
Radhika Patel, Ophthalmology LAT.
As a junior doctor training in the UK where major emphasis is put on audit and quality improvement projects, it was interesting to see how these were applied to the COECSA countries, where some concepts were new.
Attending the leadership training workshop in Nairobi this early in my career when I have very little experience in management was valuable as I feel better prepared for when I assume a more senior role. Understanding my own values and strengths at this stage in my career allows me now to apply my skills to projects where they could be put to best use.
Explaining how attending the workshop had empowered me despite being so junior gave the COECSA delegates the idea of running similar leadership training for junior ophthalmologists. The first such workshop was held at the end of March and included 10 junior ophthalmologists from Uganda who are members of COECSA’s Young Ophthalmologists Forum.
Inspiring training for junior ophthalmologists has not been the only unexpected outcome from the project. It has facilitated training for a group of PhD students at the London School of Hygiene & Tropical Medicine, and enabled training for staff from African hospital departments besides ophthalmology, such as accounts, security, administration and infection control as well as other medical and surgical departments.
References:
1. Bassey Etim, Affiong Ibanga, Linda Okafor, Marcia Zondervan. The VISION 2020 LINKS Programme: Cascading leadership training in Calabar, Nigeria. Eye News 2016;23(3):40-3.
2. NHS Institute for Innovation and Improvement. Just a routine operation: human factors in patient safety. Patient safety resource centre.
http://patientsafety.health.org.uk/
resources/just-routine-operation
-human-factors-patient-safety
Last accessed April 2017.

COMMENTS ARE WELCOME