This is the first in a series of three articles (see Part 2 here) about strengthening eye health services in Nigeria through collaboration with the LINKS and Networks run at the International Centre for Eye Health, London School of Hygiene & Tropical Medicine (LSHTM).
Introduction
Increasing the quality and quantity of all essential eye health services and the population covered by these services is a policy priority for Nigeria. A key strategy is to make eyecare an integral part of Nigeria’s journey towards universal health coverage (UHC) by implementing inclusive, integrated care that meets the growing eyecare needs and expectations of the population.
The National Eye Health Programme (NEHP) of the Federal Ministry of Health (FMOH) is tasked with leading in the strengthening of eye health infrastructure, increasing workforce capacity and creating an enabling environment such that the eye health system can leverage on existing partnerships while establishing new local and international links to respond to priority eye health issues.
Over the years, coordination and service delivery has focused on cataract being the major cause of blindness. However, as interventions in that direction continue, the eye health system needs to develop the dexterity to tackle other eye conditions that have the potential to increase the burden of blindness and visual impairment. Major demographic shifts, economic and lifestyle changes have led to an increase in life expectancy and the number of people who develop blindness from glaucoma (associated with age) and diabetic retinopathy (DR). While retinoblastoma is a rare childhood ocular cancer, it can have devastating effects on vision, education, productivity, and quality of life, and can be fatal.

Dupe and team members welcome the team from Israel at the airport in Lagos.
A concerted, country-led integrated approach through the development of national guidelines, strengthening of services, infrastructure and workforce training will ensure comprehensive, standardised, evidence-based, cost-effective care and improved outcomes to individuals, families, and the nation. Furthermore, a comprehensive monitoring and evaluation system to generate high quality evidence to improve care models, guide policy and track Nigeria’s progress to UHC through eye care is essential.
In line with the National Eye Health Policy, the NEHP is presently working in collaboration with the DR-NET and Glaucoma-NET run by the VISION 2020 LINKS Programme to develop frameworks for glaucoma and DR and hopes to expand the ongoing effort with Rb-NET in the care of patients with retinoblastoma.
Beyond that, we hope for further collaboration to broaden the research horizon and open the door to much-needed technological innovations that will help to overcome local challenges and take eyecare in Nigeria to the next level.
Background
Retinoblastoma (Rb) is a rare but deadly cancer, which affects approximately 9000 children globally every year. It is the most common ocular cancer of childhood. In high-income countries, with specialised Rb treatment centres, almost all children survive, and most eyes do not need to be removed. However, in low- and middle-income countries (LMICs), particularly in Africa, mortality is typically around 60%.
The Retinoblastoma Network, Rb-NET, was established in 2017 by the VISION2020 LINKS Programme to support and coordinate action against Rb in response to requests from LMICs [1].
Alongside the capacity-strengthening activities of Rb-NET, global research is underway. The Global Retinoblastoma Study Group, led by Didi Fabian and Richard Bowman, was developed to bring together units treating children with Rb, to share findings and combine their data to provide a greater understanding of the disease globally [2]. A recent publication from the Group shows that children with Rb in low-income countries are 16 times more likely to die within three years of diagnosis than children in high-income countries [3].
Didi Fabian is one of the technical advisors to the Rb-NET and has been involved since 2017. This article describes a training visit to Nigeria by Didi Fabian’s team from Israel in January 2023 at the request of Dupe Ademola-Popoola, a leading Specialist Paediatric Ophthalmologist working with children with Rb. The specific request was to establish intra-arterial chemotherapy (IAC) for children with Rb for the first time in Nigeria [4].

Planning the IAC treatment of children with Rb.
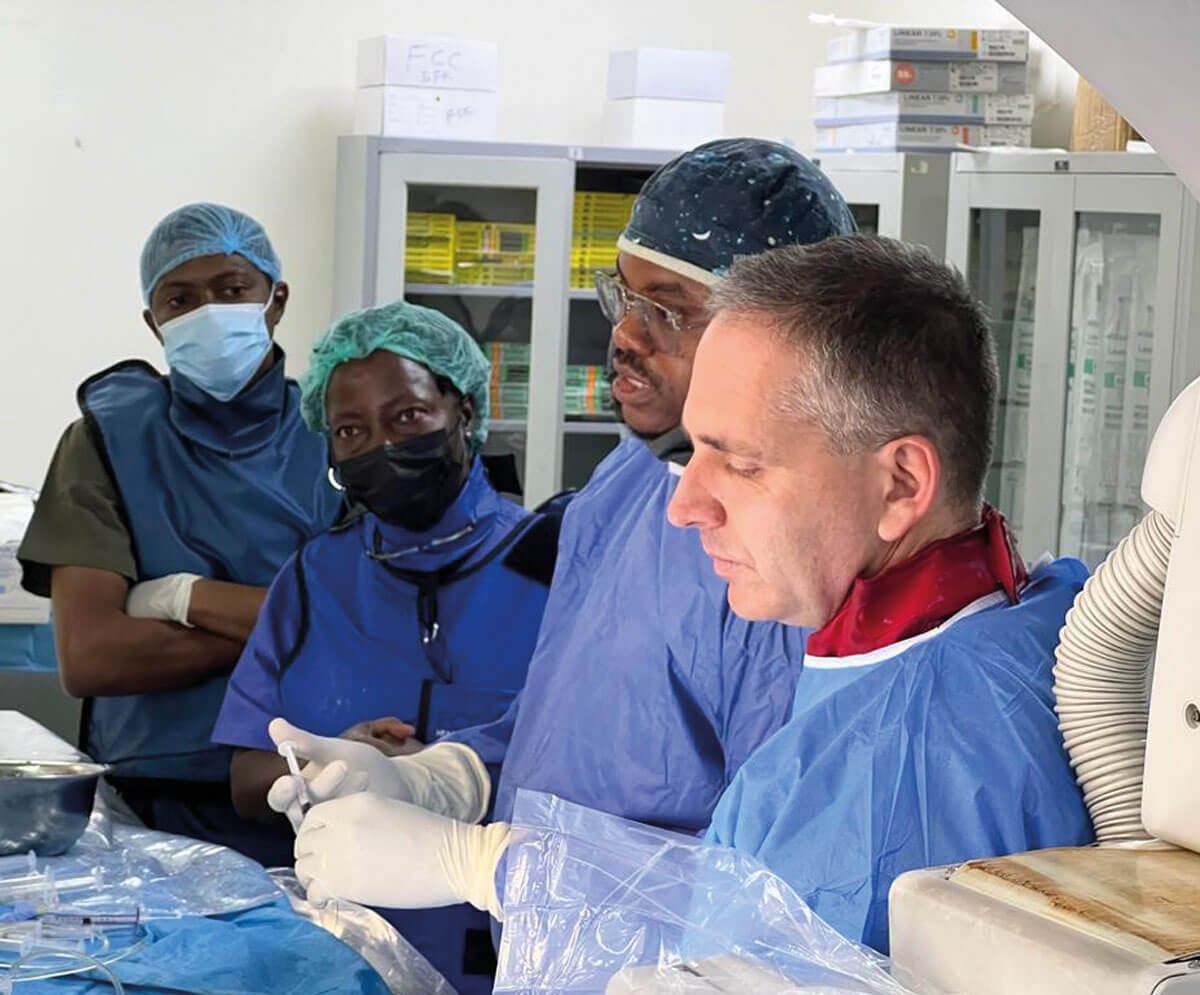
The team working together in the cathlab.
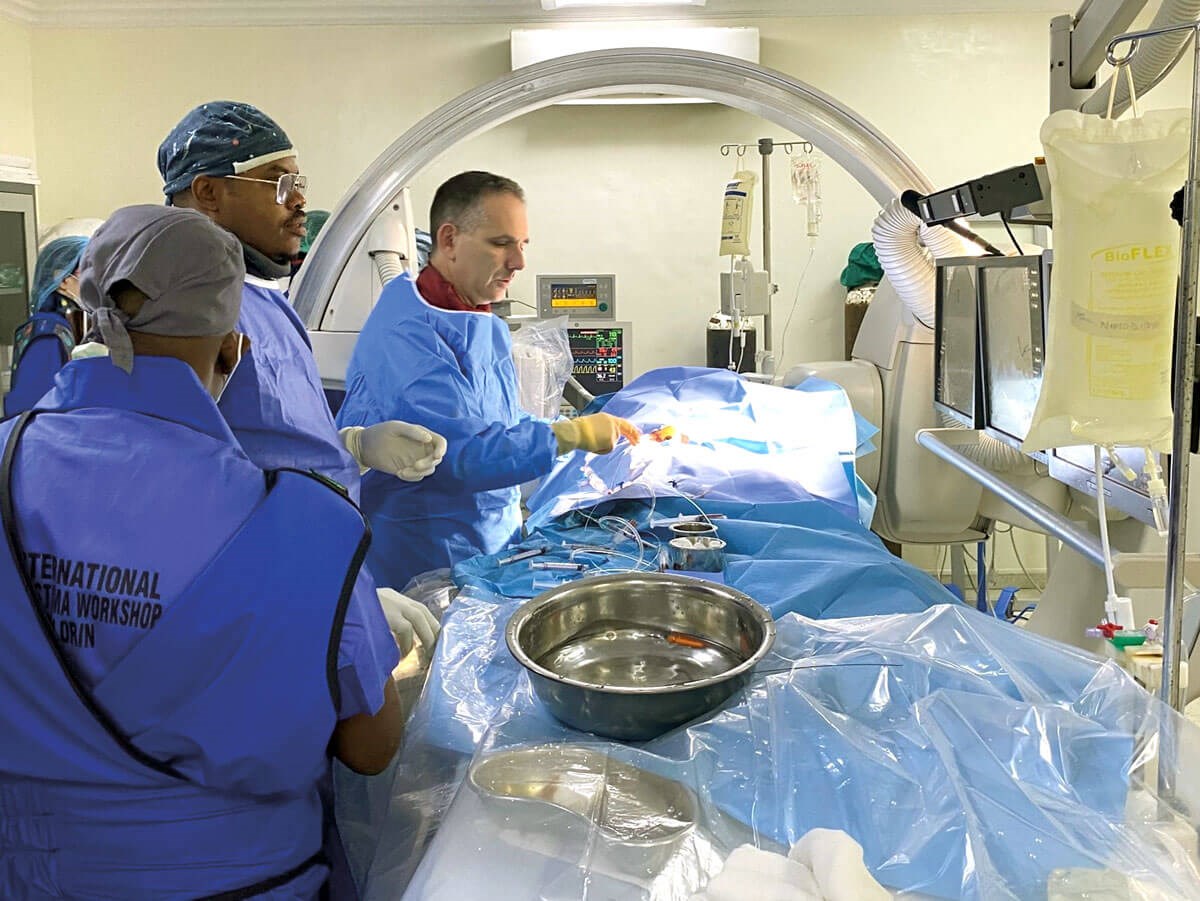
Gal Yaniv, Sheba Interventional Radiologist, doing the first IAC while other team members look on.
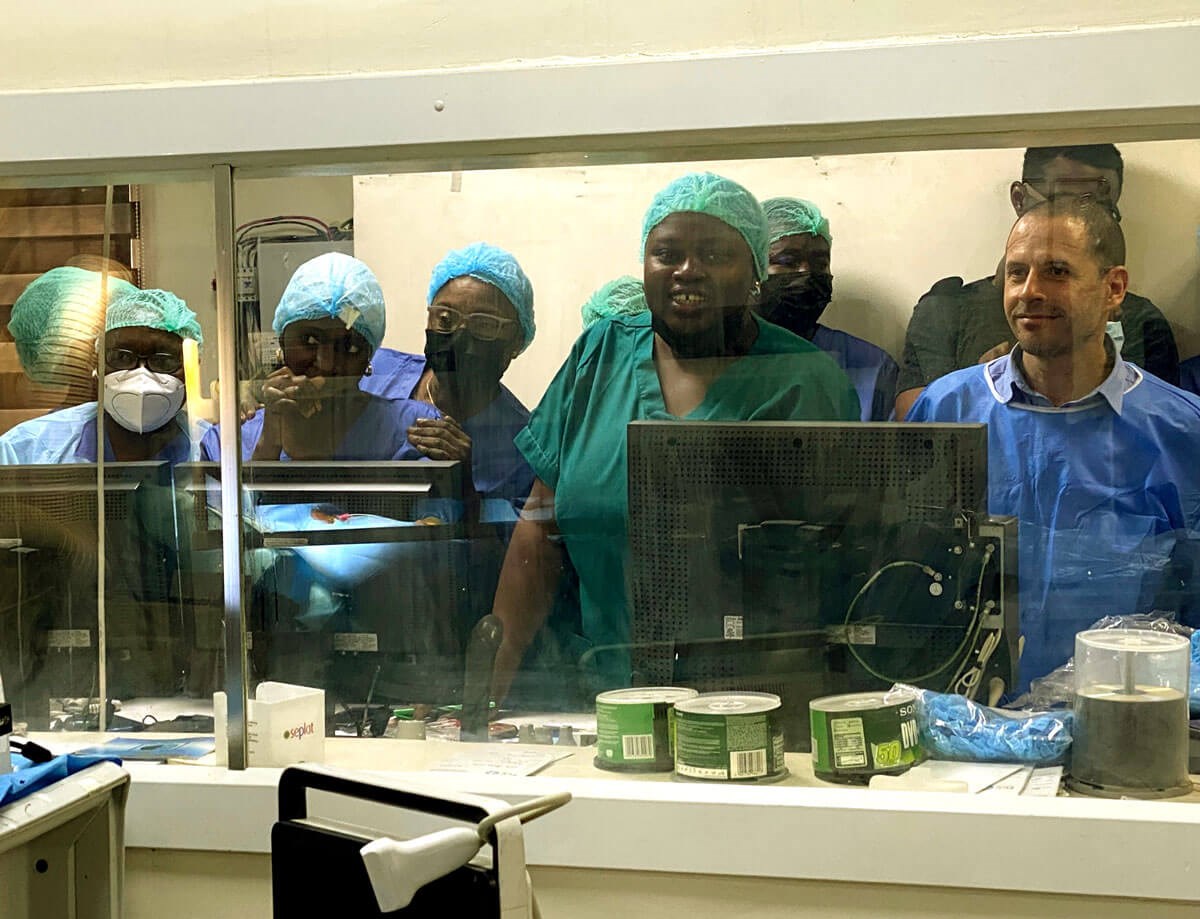
Others from the team watching from behind the screen.
The training visit – the Nigerian team perspective
Rb-focused clinical care was started by Dupe Ademola-Popoola and her team in 2007. Since then, her team has provided expert, compassionate care to patients from all six geopolitical zones in Nigeria. Training has also been provided to ophthalmology colleagues – residents, nurses, community health workers and medical students at the University of Ilorin Teaching Hospital (UITH) and University of Ilorin, Nigeria.
Treatment for Rb has advanced from just removing eyes (enucleation) to using chemotherapy through the veins and laser treatment to salvage the eyeball and, in some cases, save vision. The need to provide advanced care and services including IAC and genetic testing have become imperative in Nigeria. IAC would enable more eyes affected by Rb to be salvaged, as the eyes are reached directly with chemotherapy delivered through the ophthalmic artery accessed through the groin (femoral artery).
Since 2017, Dupe has been part of Rb-NET and participates in regular online Rb-NET multidisciplinary team meetings, through which she met Didi Fabian and other experts who give their time to advise on challenging cases in LMICs [5,6]. Dupe asked Rb-NET if any of the members would be able to provide technical support and capacity-strengthening for IAC in Nigeria. Didi Fabian jumped in with a great offer from Sheba Medical Centre in Israel.
In order to undertake IAC, an interventional radiologist and a catheterisation lab (cathlab) would be required. This is not available yet at our hospital in Ilorin, but we did not allow that to deter us. We are very grateful that First Cardiology Consultants in Ikoyi, Lagos provided their cathlab for this initiative.
The 12 Nigerian team members included:
- Dupe Ademola-Popoola – Paediatric Ophthalmologist and Ocular Oncologist.
- Hammed Ninalowo – Interventional Radiologist.
- Olanrewaju Oyedepo – Paediatric Anaesthetist.
- Modupe Olarewaju – Oncology Pharmacist.
Because healthcare is offered as ‘fee for service’ in Nigeria, funding is the greatest challenge to IAC treatment. Financial support was provided by the Nigeria team members, our friends and Irdocnigeria, to augment funds from the patient care givers and some consumables provided in kind by team members from Israel.
The training visit – the Israeli team perspective
Nigeria, with its population of over 200 million people, has some of the highest numbers of cases of Rb in the world (about 400 new cases per year). Dupe Ademola-Popoola and her team are part of the Rb-NET MDT programme, through which they review cases and discuss outcomes with experts from across the world [6,7]. The team in Israel heard the request from Dupe for help in establishing IAC in her country and responded by planning a training visit and putting together the multidisciplinary team needed:
- Didi Fabian – Team Leader and Ocular Oncologist.
- Shani Caspi – Paediatric Oncologist.
- Michal Ivri – Paediatric Anaesthesiologist.
- Gal Yaniv – Neuro-interventionalist.
- Mattan Arazi – Ophthalmology Resident.
A photographer from Ynet, the Israeli national news agency, also joined the group. The team spent time in advance of the visit reviewing with Dupe the patients with Rb who would be treated and organising the logistics, such as: Who will transport the chemotherapy drugs from the pharmacy to the hospital? How will we ensure safety of the kids while they are anaesthetised?
After two long flights we arrived in Lagos, Nigeria. We were immediately greeted by Dupe and her team, who graciously welcomed us. The excitement in her eyes was unforgettable! We had an introduction of team members and an overview of the plan for the next day before we headed to our hotel for the night.

Dupe Popoola (far left) and the team from Israel meeting senior
representatives of the University of Ilorin Teaching Hospital.
Early the next morning we met Dupe and her team of medical specialists. We reviewed the case histories of the children we would be treating. The first child is a 46-month-old female being managed for bilateral Rb (ICRB RE group E and LE group C). The child had already received two courses of neoadjuvant intravenous chemotherapy as well as focal consolidation therapy in her left eye. We discussed the case and decided to proceed with bilateral IAC.
We would be catheterising and injecting chemotherapy drugs into both eyes, one after the other.
We reviewed the other cases, and headed into the cathlab to begin the procedure. Michal joined Olanrewaju Oyedepo, the Nigerian Anaesthesiologist, in sedating the child. Gal joined the Interventional Radiologist, Hammed Ninalowo, and started preparing the equipment. After a few minutes, the child was successfully intubated and mechanically ventilated.
Throughout the procedure, Gal showed Dr Ninalowo the technique and described possible complications. Gal accessed the ophthalmic artery and injected contrast, outlining the vessels of the right eye. Dr Ninalowo and Dupe started preparing the chemotherapy to inject into the eye. They injected three agents – melphalan, topotecan and carboplatin. After successfully injecting the chemotherapy, Gal retracted the catheter and proceeded to the contralateral eye. However, this time, the anatomy of the ophthalmic artery was different. Cannulation may have been more difficult; however, Gal and Dr Ninalowo successfully accessed the ophthalmic artery. A dose of chemotherapy agents entered the left eye, and bilateral IAC was completed.
The combined team of 12 Nigerian and six Israeli medical professionals started applauding. The collaborative effort of all the doctors, nurses, pharmacists and hospital staff in the room, from different parts of the world, made this possible, and the relief and happiness was palpable.
The next child is prepped, and this time Dr Ninalowo takes the lead. Gal stands at his side, guiding him as he advances the catheter through the femoral artery up to the carotids. Accessing the ophthalmic artery this time proved difficult. At the third attempt, Dr Ninalowo successfully advanced into the artery and injected contrast. IAC was given, and the catheter was removed. The dream of establishing a formal IAC service in Nigeria had come true.
The following day, we travelled to Ilorin to go to UITH, where we were warmly greeted by Dupe, as well as the head of the hospital and other members of the hospital board. We established a formal connection between our two major hospitals – UITH and Sheba Medical Center.
One of the aims of our visit to Nigeria was to participate in a symposium that included topics from a variety of disciplines and subspecialties, including ophthalmic and paediatric oncology, anaesthesiology, interventional radiology, and global health.
Dupe spoke movingly about the struggle of treating Rb in Nigeria. During her residency training, every case of Rb was considered extraocular disease. She quoted from Roger Steinert: “Our current challenge is not technological, but social”, and highlighted the difficulties associated with raising awareness and financing treatment as well as access to care.
The visiting team gave lectures relating to our specific fields of work on Rb. We focused on IAC treatment and its indications, complications, surgical techniques, anaesthesia considerations, comparisons to intravenous chemotherapy and contraindications. The symposium was well-attended, with five of the six geopolitical regions in Nigeria represented.
During the Q&A session, we learned about the problems the physicians face in Nigeria. I was surprised to hear that there is no universal healthcare system in the country, and therefore many families are unable to afford first-line chemotherapy treatment. Many Rb children die due to a lack of financial support. In some cases it can simply be lack of transport from their village which means the child’s disease has progressed so far.
The following day we returned to clinical work alongside our Nigerian colleagues. We began with examinations under anaesthesia (EUA). The first patient is a 12-month-old female with bilateral retinoblastoma, left eye already enucleated. Dupe explained that they are struggling to save the other eye. The team examined the eye and Dupe took photos of it, so that we could share what we are seeing and Dupe and Didi could answer questions from the gathered physicians.
We spent the rest of the afternoon performing EUAs on children, deciding whether to continue observation or referral to treatment. Dupe explained that this is tricky, because not every treatment is available, or the parents may not be able to afford it.
At the completion of the project, we received a warm ‘thank you’ from Dupe and her colleagues in Nigeria. We all danced from happiness at the amazing work we were able to accomplish together in the week. What joy!
The scale of the achievement – the Nigerian perspective
Three eyes of two patients successfully had the first IAC in Nigeria. We believe that no less than 50 patients will benefit from this procedure over the next year if funding permits. Nigeria-wide Rb team members look forward to making IAC a regular treatment for all eligible children.
We believe this international collaborative effort – assisted by public-private partnership in Nigeria – will inspire the FMOH in planning for Rb, so that more children who suffer from it will survive, have their eyes salvaged and vision preserved. This will hopefully drive improvement in early presentation and treatment uptake.
The wide publicity received following the IAC testifies to the excitement that the project generated [8]. The goal of establishing a formal IAC centre in Nigeria was achieved – an example of an international collaboration against a fatal paediatric illness, a means to share knowledge across the world, and to make readily available in-country this specialist treatment for advanced Rb.
References
1. Williams P, Bowman R, Foster A, et al. Rb-NET: a network to save life and preserve vision in children in Africa. Eye News 2018;24(6):32-4.
2. Global Retinoblastoma Study Group. Fabian ID, Abdallah E, Abdullahi SU, et al. Global retinoblastoma presentation and analysis by national income level. JAMA Oncol 2020;6(5):685‑95.
3. Global Retinoblastoma Study Group. The Global Retinoblastoma Outcome Study: a prospective, cluster-based analysis of 4064 patients from 149 countries. The Lancet Glob Health 2022;10(8):e1128-e1140.
4. Intra Arterial Chemotherapy for Retinoblastoma. Children’s Hospital of Philadelphia.
https://www.chop.edu/
treatments/intra-arterial-chemotherapy
-iac-retinoblastoma
5. Rb-NET website.
https://iceh.lshtm.ac.uk/iceh-new/the-rb-net/
6. Rb-NET MDT website.
https://www.rb-net-mdt.org/
7. Fabian ID, Astbury N, Nkanga E, et al. The role of virtual Rb-NET Multidisciplinary Team meetings in the management of children with retinoblastoma in low- and middle-income countries. Eye News 2021;27(6):36-40.
8. An example of media coverage in Nigeria. Pulse.ng.
https://www.pulse.ng/news/local/
chemotherapy-nigerian-doctors-partner-israel
-on-eye-cancer-treatment/p2brv82.amp
[All links last accessed February 2023].
COMMENTS ARE WELCOME















