Malawi is a small land-locked country in eastern Africa with a growing population of over 17 million people. About 45% of the population is aged 14 or under; only 5% are aged 60 or over. The gross national income per capita is 750 USD and total expenditure on health is 90 USD per capita. The main export is tobacco and the main imports are fuel oil and fertilisers. More than half of the population lives below the poverty line, and over 85% depend on subsistence agriculture. Malawi faces annual inflation rates in excess of 20%. It is ranked 146th in the world [1].
In January this year, a VISION 2020 LINK between Blantyre and Liverpool was formalised. The preparation and signing of a Memorandum of Understanding (MoU) was facilitated by the VISION 2020 LINKS Programme. The participating institutions are the Lions Sight First Eye Hospital, Queen Elizabeth Central Hospital (QECH), Blantyre and the College of Medicine, University of Malawi, with St Paul’s Eye Unit, Royal Liverpool University Hospital.
This LINK runs alongside, and communicates closely with, existing LINK partnerships between the Lions Sight First Eye Hospital in Blantyre and the Royal Hospital for Children, Glasgow for paediatric ophthalmology training, and between the Lions Sight First Eye Hospital in Lilongwe and the Queen Margaret Hospital in Dunfermline for diabetic retinopathy (DR) training and capacity building.
The VISION 2020 LINKS between Malawi and Scotland have been running for almost a decade and have benefited from a number of grants from the Scottish Government. The LINKS are also part of DR-NET [2-4] and benefit from funding from the Queen Elizabeth Diamond Jubilee Trust to build DR services in Malawi [5].

The team from Blantyre and Liverpool at the signing of the MoU.
Front row from left: Michael Briggs; Feggie Bondole, Chief Nursing Officer, QECH; Simon Harding,
Consultant Ophthalmologist and Head of the Department of Eye and Vision Science,
Institute of Ageing and Chronic Disease, University of Liverpool; Andrew Gonani, Hospital Director, QECH.
Back row from left: Petros Kayange, Nick Beare, Gerald Msukwa.
The Malawi perspective: Petros Kayange, Consultant Ophthalmologist, Lions Sight First Eye Hospital, Blantyre
The signing of the MoU for a VISION 2020 LINK between Blantyre and Liverpool in January 2016 was a milestone and cemented an informal relationship that had existed for many years.
Since 2009, there have been tremendous local efforts in developing services for detection, referral and treatment of DR. This was led in Blantyre by Professor Theresa Allain, head of the Department of Medicine and me, as head of the ophthalmology unit at the College of Medicine, University of Malawi. It was done in close but informal collaboration with Liverpool.
With a grant from the World Diabetes Foundation (WDF), Prof Allain initiated and coordinated a project to develop diabetes services in the southern region of Malawi. The project was done in collaboration with the Ministry of Health, Lions Sight First Eye Hospital and the Diabetic Association of Malawi. The objectives of the project were to establish diabetes clinics at district hospitals and to develop DR management.
Fifteen diabetes clinics were established at district hospitals within our catchment area, in addition to the busy diabetic clinic at QECH in Blantyre, where the Lions Sight First Eye Hospital is also based. The district clinics are run by clinical officers and nurses. Clinical officers are mid-level health workers who are trained to provide medical care to patients. Ophthalmic clinical officers in the district have been trained to identify and refer patients with diabetic retinopathy. Ophthalmic clinical officers are health workers with less training and scope of practice than ophthalmologists. Due to the shortage of medical doctors, the clinical officers form the backbone of the health workforce in many developing countries. The implementation of the WDF-funded project provided the initial foundation towards development of DR services in the southern region of Malawi. It has been further built on by involvement in DR-NET [2-4] and the DR training visits to Malawi by the LINK team from Dunfermline.
About 50 people with diabetes per month come from the general diabetic clinics to have DR screening at the Lions Sight First Eye Hospital. Most of these patients are from the diabetic clinic at QECH and a few (three to five per month) are referrals from the district hospitals. We plan to further strengthen DR services at district level so that more patients can be screened, subject to funding being available.
With the VISION 2020 LINK with Liverpool now formally in place, the LINK has joined the DR-NET, as described below. The Lions Sight First Eye Hospital is striving to greatly reduce blindness from DR by building accessible, affordable and effective services in Blantyre and surrounding districts.
Patient report by Petros Kayange
The supply of drugs for patients with chronic diseases such as diabetes is erratic in public hospitals in Malawi. This makes control of diabetes very difficult. A patient at the diabetes clinic, Melinasi Undani, was not aware that diabetes could affect her sight. She had been attending the diabetic clinic at Queen Elizabeth Central Hospital for many years. She started losing sight in both eyes and came to the Lions Sight First Eye Hospital. We diagnosed clinically significant macular oedema. She received macula laser treatment. Fortunately, her vision improved and she was very happy.
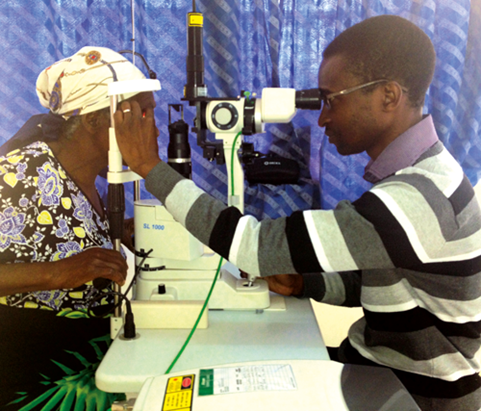
Patient Melinasi Undani being examined by Petros Kayange at
the Lions Sight First Eye Hospital, Blantyre, Malawi.
The UK team perspective: Nick Beare, Consultant Ophthalmologist, St Paul’s Eye Unit, Royal Liverpool University Hospital
The Blantyre-Liverpool LINK is unusual in that there has been an informal partnership between the two eye units for some time. This has developed out of joint research and personal connections between the two departments. However, in 2016 we decided to formalise this connection under the VISION 2020 LINKS Programme and to involve a wider group of eye health professionals in the LINK partnership and DR-NET.
I first arrived in Blantyre, Malawi in 1999, hauling a heavy rucksack, for a four-month research fellowship investigating malarial retinopathy. This was based in the Paediatric Department of QECH under the direction of Professor Simon Harding, researching children with cerebral malaria. The project was part of a larger programme on malaria involving a number of researchers from the US, Europe and Malawi, with funding from NIH and the Wellcome Trust. When I tracked down the Ophthalmology Department at the QECH, Henry Nkume was the sole ophthalmologist in a single ward and an attached operating theatre.
Subsequently I was able to extend my fellowship to 18 months, including working in the ophthalmology department. I felt that as an SHO I could offer limited assistance, but luckily I had learned extracapsular cataract extraction in the tail end of its use in Europe. So I was able to contribute to lists and quickly found myself immersed in the work of the ward after the malaria season. That was the beginning of my connection with ophthalmology in Blantyre.
The research into malarial retinopathy developed, and I returned in 2005 for a second research fellowship armed with a fluorescein angiogram camera and a portable ultrasound. In the intervening years the eye department had moved to a large separate building through the efforts of Dr Nkume, funded by the Lions organisation – the Lions Sight First Eye Hospital. The personnel had also increased, with another ophthalmologist, Gerald Msukwe, and optometrists and additional ophthalmic clinical officers.
Research has been a mechanism by which we have been able to develop a long-term relationship between Blantyre and Liverpool. This developed further in 2010 when we started a research project in DR based in the Lions Sight First Eye Hospital. This collaboration has been very productive, enabling the first cohort study of DR in sub-Saharan Africa [6].
Petros Kayange was appointed as a consultant with a special interest in retinal disease and has been closely involved in this work. We have had several research fellows, including a three-year PhD student researching DR, and also helping to develop the DR service and teaching DR to all cadres. More generally, research can help develop subspecialties in eye departments in sub-Saharan Africa, enhance professional development and ophthalmologist retention.
However, purely focusing on research neglects service development and training of other personnel that can be achieved through a VISION 2020 LINK. That is why the time was right to formalise the partnership. We also wanted to be part of the DR-NET, a network of VISION 2020 LINKS with a shared goal of developing DR services [2]. DR is an increasing problem, with Africa set to catch up with middle-income countries that already have high rates of diabetes [7]. This is an area where most UK eye units have expertise that they can offer to LINK partners, however, that knowledge has to be tailored for the African situation. Our latest research has shown that laser treatment is a very cost-effective and sustainable treatment for DR in Malawi (N Beare, unpublished data). We see great synergy between what can be achieved through collaborative research, capacity building and VISION 2020 LINKS Programme and DR-NET input into service development.

Michael Briggs and Petros Kayange shaking hands at the signing
of the MoU between Blantyre and Liverpool in January 2016.
The UK team perspective: Michael Briggs, Clinical Director, St Paul’s Eye Unit, Royal Liverpool University Hospital
My consultant colleague Nick Beare is the inspiration behind our involvement with the VISION 2020 LINKS Programme and he invited me to accompany him to Blantyre in January 2016 to formalise the LINK partnership with Blantyre. All parties – the two eye units and the College of Medicine, Malawi – signed a MoU setting out our commitment to the VISION 2020 LINK.
Having grown up in the West of Scotland I was familiar with the story of David Livingstone and had visited his childhood home in Blantyre, Lanarkshire. I knew little else about Blantyre, Malawi, other than that Nick appeared to have a compulsion to go there on a regular basis.
I quickly learnt that Malawi is a fascinating country. The statistics make depressing reading – DP, average income and life expectancy are all amongst the lowest in the world. However, all the people that I encountered – hospital staff, patients or members of the public – were universally charming and welcoming.
The staff of the eye hospital, led by Gerald Msukwa and Petros Kayange, is resourceful and dedicated despite the challenges of limited facilities, resources and equipment. I was particularly impressed by the enthusiasm of the ophthalmology trainees for the teaching that we were able to offer during our short visit.
The challenge for us is to make our contribution relevant and useful in an environment in which many of the techniques and devices with which we are familiar are not readily available. As Nick has outlined, diabetic eye disease and malarial retinopathy are two research areas in which the collaboration has already been productive. We hope that over the coming years we will be able to inspire our consultant colleagues and other eye professionals in Liverpool to participate in the LINK and contribute their expertise.
We are at the beginning of what I hope will be an enduring relationship which will primarily benefit the practice of ophthalmology in Blantyre and elsewhere in Malawi but which will also give members of St Paul’s staff a chance to make a fulfilling contribution and to gain personally from their involvement. We also intend to engage staff at St Paul’s in fundraising to facilitate reciprocal visits to Blantyre and in provision of teaching and support to their Malawian counterparts.
Having visited Blantyre, I now understand Nick’s passion for the country and I am looking forward to a long and fruitful LINK partnership between St Paul’s and the Lions Sight First Eye Hospital.
References
1. Malawi. 2016 Index of Economic Freedom.
http://www.heritage.org/index/country/malawi
Last accessed June 2016.
2. Diabetic retinopathy LINKS network. Commonwealth Eye Health Consortium.
http://cehc.lshtm.ac.uk/dr-links/
Last accessed June 2016.
3. Poore S, Foster A, Zondervan M, et al. Commonwealth nations join forces to prevent blindness from diabetes. Eye News 2015;21(5):33-6.
4. Blows P, Peto T, Philippin H, Zondervan M. Situation analysis of diabetic retinopathy services in eleven countries. Eye News 2016;22(4):42-4.
5. The Queen Elizabeth Diamond Jubilee Trust.
http://jubileetribute.org/
Last accessed June 2016.
6. Burgess P, Allain T, Garcia-Finana M, et al. High prevalence in Malawi of sight-threatening retinopathy and visual impairment caused by diabetes: identification of population-specific targets for intervention. Diabet Med 2014;31(12):1643-50.
7. Burgess P, Msukwa G, Beare N. Diabetic retinopathy in sub-Saharan Africa: meeting the challenges of an emerging epidemic. BMC Medicine 2013;11:157.
COMMENTS ARE WELCOME








