In this second article (see first article here), Samuel Aryee and Rhys Dumont Jones review the challenges involved in managing this condition.
Examination and diagnosis
Cataracts in children can appear in a variety of forms, each presenting in a different way depending on the timing of cataract development. Referral of infants may occur after abnormalities found at the new-born baby check, a new onset squint, but most often due to an absent red reflex.
Older children may present after failing the school vision screening test, or after parents become concerned about the child bumping into things when walking. Children with systemic disease may be referred to ophthalmology from the paediatrician.
There are many identifiable causes of the paediatric cataract, and the clinical examination should always begin with a comprehensive history which elicits any delayed developmental milestones, failure to thrive, and family history of congenital cataracts. It is also important to consider early input from paediatrics in order to assist the general assessment of the child for potential systemic disease [1]. The main causes of bilateral congenital cataracts are hereditary autosomal dominant genetic mutations, metabolic disorders such as galactosaemia, and congenital rubella [2,3]. It is therefore vital to ask about the mother’s pre-natal and gestational health to rule out drug use and intrauterine TORCH infections [1].
“Examination, diagnosis and treatment of paediatric cataract are only the first steps of a multi-faceted visual rehabilitation journey. Close collaboration between the patient, parents and the wider ophthalmic team is vital in achieving the best visual prognosis”
Unilateral congenital cataracts are typically sporadic and often present later in childhood without any family history or systemic disorder [3]. Secondary cataract can also form as a result of trauma, uveitis, use of topical steroids, chronic retinal detachment or radiation. The age of presentation and the examination of such cases presents unique challenges to the ophthalmological team. If the age of onset is uncertain, reviewing old photographs of the child for abnormal red reflex can reveal whether the cataract was present during the critical period of visual development, thereby influencing its management. Before examining the eyes, a general inspection of the child’s face should be performed, looking for any dysmorphic facial features. Characteristic facial features of syndromes associated with congenital cataracts are summarised in Table 1.

An assessment of visual acuity should be performed using a visual acuity test appropriate for the child’s age, summarised in Table 2. Objection to occlusion should also be assessed by covering one eye at a time and observing the child’s reaction. When the occlusion of one eye provokes more objection than the other, this could indicate a disparity in visual acuity.
Assess pupils, including checking for relative afferent pupillary defect and compare the red reflexes. The eye-lid margins, conjunctiva, cornea and sclera should also be examined with direct ophthalmoscopy. Look closely for strabismus or nystagmus. Using the slit-lamp biomicroscope, the anterior segment of the eye should be examined for any developmental anomalies, synaechiae or signs of relative microphthalmos [4]. Inspect the lens for opacity, which may be located peripherally or centrally, or located at the anterior or posterior aspect of the lens.
The size and density of the opacity along with other distinguishing features such as colour and shape may aid classification and influence management. Assess the posterior capsule for any co-existing defects such as posterior lentiglobus or persistent foetal vasculature (PFV), which is frequently associated with congenital cataracts [1]. Intraocular pressure and corneal diameter could help the diagnosis of congenital glaucoma, which can present alongside the cataract [1,3], although it is often difficult to measure in clinic. Measurement of refractive error can help guide the choice of post-surgical refractive correction. Indirect ophthalmoscopy is useful in assessing the health of the optic disc, retina and macula.
Alternatively, ultrasound bio-microscopy can be used if these are not easily visualised, such as in total cataract, anterior segment anomalies or PFV [6]. The examination should conclude with an examination of the child’s parents and siblings, as any previously undetected cataract may aid in a diagnosis of an inherited systemic cause or hereditary cataract [1].
Morphology
Congenital cataracts are generally categorised based on location, with a variety of shapes, sizes and densities associated with different causes. Other conditions associate with specific cataract morphology can be seen in Table 3.

Management and challenges
There are a number of important factors to consider in the management of paediatric cataracts. These include the age at presentation, type and laterality of cataract(s), developmental changes of the eye during the critical period, and the likelihood of further complications or interventions which may be invasive in nature. Early diagnosis is therefore crucial in helping the ophthalmology team develop an individualised treatment plan, limit further visual loss, amblyopia or nystagmus. It is particularly important to engage the parents or guardian in the process of decision making, as further management and visual rehabilitation postoperatively relies heavily on the family’s cooperation [8]. The risks and implications of the timing of surgery, conservative or surgical approach, and methods of visual rehabilitation must be clearly explained. They should also be given the opportunity to consider and ask questions about the pros and cons of different treatment options.
Conservative
There are indeed a proportion of paediatric cataracts that do not need urgent surgical intervention, and can be effectively observed regularly in order to discern if there is any compromise to the visual axis. This requires an objective assessment with particular note taken to the morphology present.
The main types of cataracts that can be initially observed without surgery are less than 3mm in diameter, peripheral and anterior opacities. Small anterior cataracts and opacities that contain punctate zones can also be observed initially. In contrast, central, posterior cataracts and confluent cataracts greater than 4mm are usually best treated surgically due to higher likelihood of progressive visual disruption and the child presenting with one or more visual complications at diagnosis. Lamellar cataracts, although a more central type of cataract, tend to be partially formed at birth and develop slowly, which allows for appropriate early visual development.
Therefore, they can initially be managed by observation [3]. Pupillary dilatation can be used to delay surgery in borderline cases by using 2.5% phenylephrine hydrochloride to the eye with cataract and part-time occlusion of the better eye. Daily use of a cycloplegic agent such as atropine should, however, be avoided due to the risk of causing amblyopia. These patients should be monitored closely and if amblyopia develops, surgical treatment will be required [9].
Children with amblyopia but visually insignificant cataracts can be treated successfully with patching and glasses [1]. Amblyopia treatment is also important post-surgically and the results of patching depend on the age, compliance and level of visual acuity prior to patching. This will be covered in more depth in the visual rehabilitation section.
Surgical
Surgical management is used in patients with significant cataracts affecting the visual axis, and timing is crucial in order to preserve visual acuity during the critical period of eye development. This period ranges from eight weeks to six months of age. As a general rule, unilateral congenital cataracts should be operated on as early as possible, before six weeks of age, and bilateral cataracts before eight weeks of age [1,4]. Surgery delayed beyond two to three months has been shown to potentially increase the risk of strabismus and nystagmus. The neonatal eye is complex in that it is constantly growing, with axial eye growth being difficult to predict. Some reports have observed a variability in axial eye growth post intraocular lens (IOL) implantation, which adds further uncertainty in predicting the optimal type and strength of IOL [4]. The neonatal eye is naturally hyperopic as the globe length is much shorter than an adult, as well as having a more plastic cornea and sclera. This means that ocular surgery in this age group is more likely to result in an inflammatory response, also due to the fact that there is an immature blood-to-aqueous barrier.
The benefits and drawbacks of aphakia versus IOL implantation should also be discussed in detail with the family. Leaving the child aphakic means removal of the lens without IOL implantation. The use of contact lenses or glasses is essential to achieve the desired visual acuity, as well as accounting for accommodative loss. Non-compliance or ‘down-time’ may result in significant amblyopia. In infants aged less than seven months, primary IOL insertion appears to have no significant benefit over contact lenses with aphakia. Long-term outcomes have shown that in unilateral cataract, visual acuity at one, four and 10 years is approximately the same regardless of treatment with primary IOL or aphakia with contact lenses [10].
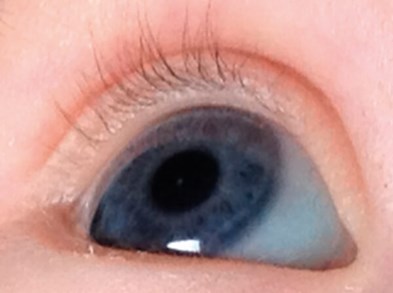
Figure 1: Anterior polar cataract diagnosed around eight weeks of age.
Observed six-monthly for five years and discharged with no further treatment.

Figure 2: Dense bilateral cataracts in a two-year-old.
Treatment at this age is still indicated although there will likely be poorer visual outcomes.
Primary IOL insertion may be associated with higher risk of adverse events such as glaucoma, and further intraocular surgery after one year. This is usually to treat visual axis opacification (VAO) [11], which is caused by lens epithelial cell proliferation on the IOL or on the posterior capsule if left intact during surgery [12]. Oculomotor and refractive complications can also develop as a result of paediatric cataract surgery. Both primary and secondary IOL insertion are also associated with high rates of strabismus [13].
Preoperative biometry is used to obtain ocular measurements to evaluate IOL strength and potential myopic shift. This is usually done under general anaesthesia prior to surgery. It is generally accepted to under-correct the eye(s) involved, leaving the child moderately hypermetropic with the use of glasses or contact lenses in the interim in order to avoid undesired myopia in adulthood. However, some may aim for an emmetropia target as they feel that it will enhance visual development in childhood while accepting a need for myopic correction in the future [1,4,14].
Primary IOL implantation is usually reserved for visually significant paediatric cataract in older children [10], while in infants and younger children it is often not recommended due to its associated complications. There are various techniques to achieve lensectomy, with or without IOL implantation. After making an initial incision at the limbus or via scleral tunnel, some surgeons may proceed by performing a curvilinear continuous capsulorhexis (CCC) to access the lens substance with subsequent lens aspiration as in an adult cataract surgery. In other cases, a CCC may not be possible with forceps and needs to be created with a vitrector (vitreorhexis).
Alternatively, lensectomy could be done using a pars plana approach. As children are generally too young to tolerate YAG laser capsulotomy, a primary posterior capsulorhexis is usually recommended due to the risk of posterior capsular opacity formation. This can be performed anteriorly via the cornea before or after IOL implantation, or posteriorly via the pars plana.
The prognosis for developmental cataracts is better than that of congenital cataracts, as they are likely to have less visual disruption during the early critical period [15]. A small study undertaken by Elston et al. showed clinical evidence for a latent period of roughly six weeks in neonates, in which effective treatment of visual abnormalities was likely to result in normal visual development [14].
Visual rehabilitation
Amblyopia is less common in bilateral cataracts as children are usually referred at younger ages and generally have less anisometropia postoperatively [15,16]. However, bilateral stimulus deprivation amblyopia can develop, which may be heightened by nystagmus, or an ametropic component in high refractive error [17]. Amblyopia in unilateral cataracts is treated with occlusion therapy beginning the second week post-surgery [10]. Adherence with occlusion is essential, and has a significant association with visual acuity outcomes at one-year-old [18]. Table 4 shows two different occlusion regimes.

Intensive occlusion therapy is usually required to prevent and treat amblyopia, but disruption of binocular input during early visual development may decrease potential for binocular single vision (BSV), and predispose to strabismus. A reduced occlusion regime is associated with a higher prevalence of BSV, reduced incidence of strabismus, and has been shown to produce equally good visual outcomes [20].
However, there is no conclusive evidence on which regime produces the best visual outcome, or until what age children should be occluded. Children are typically patched until they are no longer at risk of developing amblyopia, but this can pose a challenge as the child grows older. Compliance with patching often decreases with age, and can be influenced by parental socioeconomic status and education [21]. Compliance may also be affected by other visual complications of cataract, such as latent nystagmus, which is worsened by total occlusion such as patching [16]. Atropine occlusion therapy can be used in unilateral pseudophakic / aphakic patients, but is only indicated if the patient is older and using spectacles with a near add [18]. It is not an option for bilaterally pseudo-phakic or aphakic patients.
“The prognosis for developmental cataracts is better than that of congenital cataracts”
Optical penalisation is possible in unilateral or bilateral cases, by prescribing the amblyopic eye full correction and near add, while intentionally mis-correcting the non-amblyopic eye on a part-time basis. If emmetropic, optimal blur can be achieved with plus lenses, while a plano lens can be used if refractive error is present. In bilaterally aphakic children using contact lenses, optical penalisation is possible by depriving the non-amblyopic eye of its contact lens for the required number of hours each day [16].
In summary
There are a vast number of factors to consider when deciding on the method of treatment of a paediatric cataract. Is it bilateral or unilateral? Is it developmental or congenital? Is visual development limited by the opacity? Surgical treatment can be very effective if initiated early, but is associated with risks of secondary complications.
The decision of leaving the child aphakic or implanting an artificial lens requires planning and compliance with the family. Proper visual rehabilitation of the neuro-ophthalmic axis is crucial in order for better long-term visual outcomes.
References
1. Medsinge A, Nischal K. Pediatric cataract: challenges and future directions. Clin Ophth 2015;9:77-90.
2. Santana A, Waiswo M. The genetic and molecular basis of congenital cataract. Arquivos brasileiros de oftalmologia 2011;74(2):136-42.
3. Salmon JF: Kanski’s Clinical Ophthalmology: A Systematic Approach, 9th ed. Elsevier: Amsterdam, The Netherlands; 2019.
4. Khokhar SK, Pillay G, Dhull C, et al. Pediatric cataract. Ind J Ophth 2017;65(12):1340-9.
5. Ansons AM, Davis H: Diagnosis and Management of Ocular Motility Disorders, 4th ed. Wiley-Blackwell: Hoboken, USA; 2013.
6. El Shakankiri NM, Bayoumi NH, Abdallah AH, El Sahn MMF. Role of ultrasound and biomicroscopy in evaluation of anterior segment anatomy in congenital and developmental cataract cases. J Cataract Refr Surg 2009;35(11):1893-905.
7. Amaya L, Taylor D, Russell-Eggitt I, et al. The Morphology and Natural History of Childhood Cataracts. Surv Ophth 2003;48(2):125-44.
8. Vasavada AR, Shah SK, Vasavada V. Management Options in Pediatric Cataract. US Ophth Rev 2012;5(1):44-7.
9. Wright KW, Strube YNJ: Paediatric Ophthalmology and Strabismus, 3rd ed. Oxford University Press; 2012:782.
10. Infant Aphakia Treatment Study Group, Lambert SR, Buckley EG, Drews-Botsch C, et al. A randomized clinical trial comparing contact lens with intraocular lens correction of monocular aphakia during infancy: grating acuity and adverse events at age 1 year. Arch Ophth 2010;128(7):810-8.
11. Plager DA, Lynn MJ, Buckley EG, et al. Complications, adverse events and additional intraocular surgery one year after cataract surgery in the Infant Aphakia Treatment Study. Ophthal 2011;118(12):2330-4.
12. Chen J, Chen Y, Zhong Y, Li J. Comparison of visual acuity and complications between primary IOL implantation and aphakia in patients with congenital cataract younger than 2 years: a meta-analysis. J Cataract Refr Surg 2020;46(3):465-73.
13. Infant Aphakia Treatment Study Group, Lambert SR, Lynn MJ, Hartmann EE, et al. Comparison of contact lens and intraocular lens correction of monocular aphakia during infancy: a randomized clinical trial of HOTV optotype acuity at age 4.5 years and clinical findings at age 5 years. JAMA Ophth 2014;132(6):676-82.
14. Elston JS, Timms C. Clinical evidence for the onset of the sensitive period in infancy. BJO 1992;76:327-8.
15. Birch EE, Cheng C, Stager DR Jr, et al. The critical period for surgical treatment of dense congenital bilateral cataracts. JAAPOS 2009;13:67-71.
16. Lambert SR. Treating amblyopia in aphakic and pseudophakic children. Am Orthopt J 2007;57(1):35-40.
17. Wilson ME. Pediatric cataracts: overview [Internet]. San Francisco: AAO 2015. [cited 2020 Apr 23]:
https://www.aao.org/disease-review/
pediatric-cataracts-overview
Last accessed June 2020.
18. Drews-Botsch C, Celano M, Kruger S, Hartmann EE. Adherence to occlusion therapy in the first six months of follow-up and visual acuity among participants in the Infant Aphakia Treatment Study (IATS). IOVS 2012;53(7):3368-75.
19. Lambert SR, DuBois L, Cotsonis G, et al. Factors associated with stereopsis and a good visual acuity outcome among children in the Infant Aphakia Treatment Study. Eye 2016;30:1221-8.
20. Jeffrey BG, Birch EE, Stager DR Jr, et al. Early binocular visual experience may improve binocular sensory outcomes in children after surgery for congenital unilateral cataract. JAAPOS 2001;5(4):209-16.
21. Loudon SE, Fronius M, Looman CW, et al. Predictors and a remedy for noncompliance with amblyopia therapy in children measured with the occlusion dose monitor. IJOVS 2006;47(10):4393-400.
TAKE HOME MESSAGE
The paediatric cataract is multi-faceted in terms of age of onset, morphology, associated disease and risk factors. Early diagnosis and treatment can help to avoid long-term adverse sequalae such as amblyopia and strabismus, but have different associated risks depending on treatment initiated. Visual rehabilitation with adequate compliance can have a great deal of benefit in improving visual acuity and binocularity, but must be tailored to the individual and family for optimal results.
Acknowledgements
The authors would like to thank Latif Miah, FY1 Doctor for photographic editing; and Mr Hugh Jewsbury and Mr Patrick Watts, Consultant Ophthalmic Surgeons in strabismus and paediatrics at UHW for reviewing the article.







