Jim Innes.
Dear Editors,
I write to congratulate Aadil Hussain on his excellent Trainees article “Watch your back: Ergonomics and Ophthalmology”.
Please can I reassure him that, at least in the Yorkshire School of Ophthalmology, the importance of good posture is part of our curriculum and has been taught during ST1 induction for the last nine years. We have a one-day course entitled “Introduction to the wet lab”, where sitting correctly is discussed and demonstrated as the first item of the day, then practised all day and beyond.
More than ten years ago I invented a simulated surgical table with a built-in drainage area and more importantly a height adjustable support mechanism. Coupled with a multi-adjustable “operators chair” (for operators of industrial machinery) we can simulate the operating theatre position very closely. More recently I developed an award-winning mobile version of the workstation incorporating the same drainage table on a mobile and height-adjustable base, coupled with a “bench top” microscope. Because such microscopes have fixed 45-degree eyepieces good posture is even more important. Of course, we couple each workstation with the same style of operator chair.
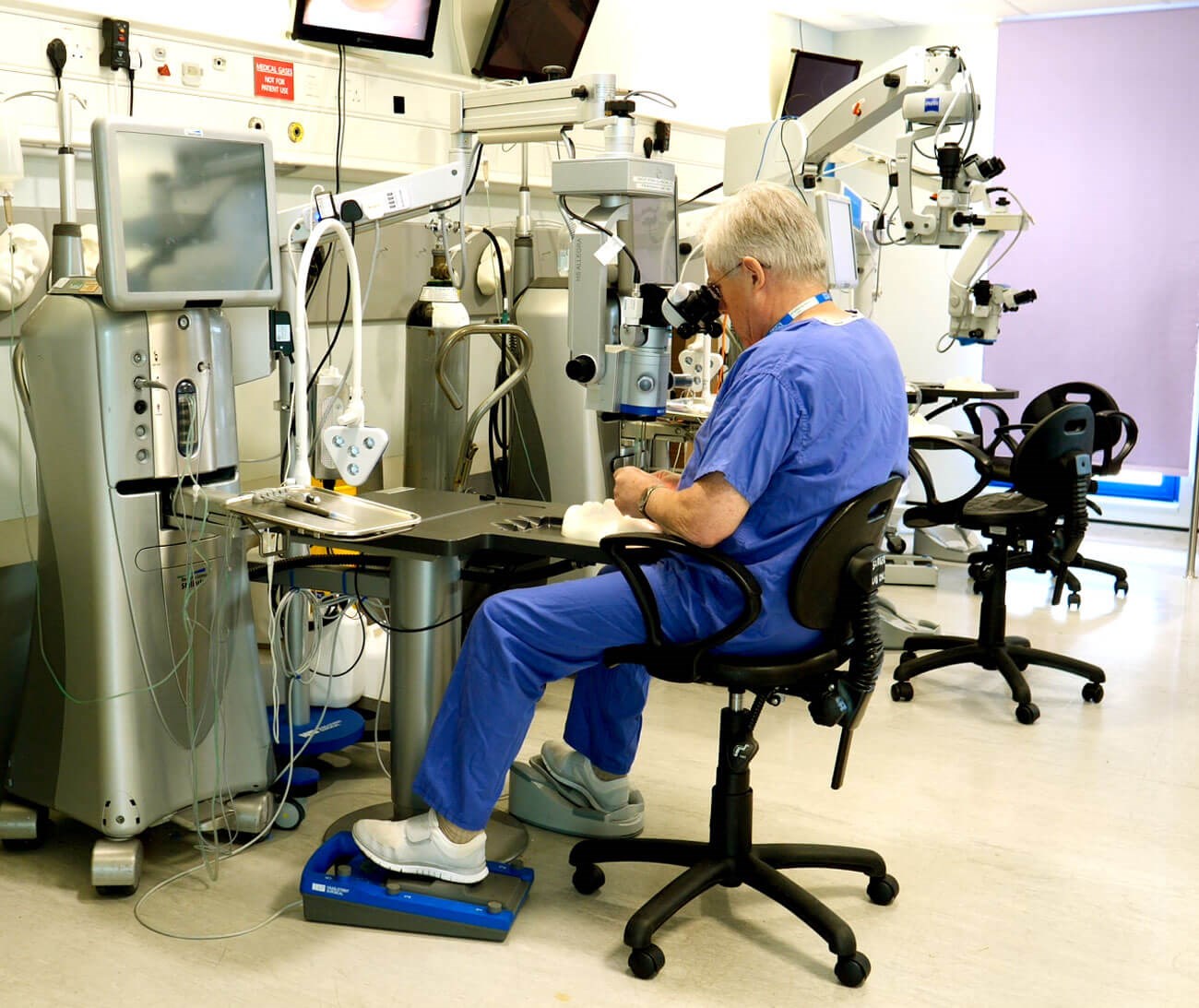
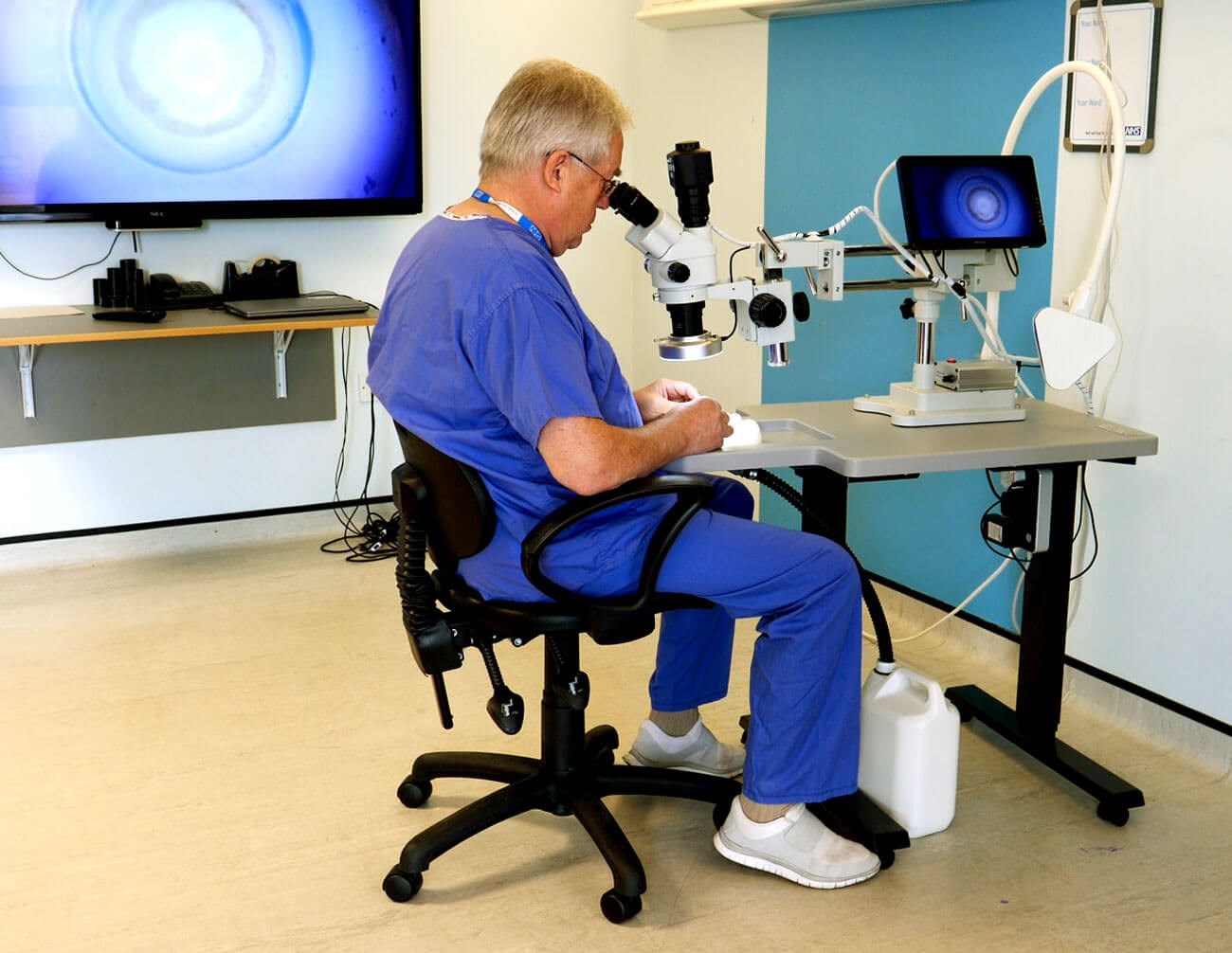
I do take some issue with the demonstration of the optimal seating position. In my opinion the surgeon should be more relaxed, with the whole body leaning back from the hips at an angle greater than 90 degrees and nearer to 120 degrees (hence the need for a proper supportive chair) with the elbows supported, forearms horizontal and with the patient’s head as low as possible. The surgeon’s pelvis should be close to the top of the table.
The reason for this is not primarily to protect the surgeon’s back (although that is obviously a good thing) but instead is for patient safety. Sitting this way allows the surgeon to gently lift the eye during the various manoeuvres. When entering the anterior chamber (AC) with a keratome that the limbus should be gently held and lifted to fix the eye, and as the blade enters and leaves the eye there should be an additional small vector upwards so that no aqueous leaves the eye during wound formation. Subsequent instruments should also be gently lifted against the anterior lip of the wound to maintain the anterior chamber depth, unless deliberately allowing aqueous out (by gently pressing on the posterior lip of the wound as in for example viscoelastic / aqueous exchange). This gentle lifting can only be done consistently by sitting properly as described.
Poor posture can result in the hands being held too high (“like a chipmunk”) and, having no support, they will tend to drop. This is the main reason for capsulorrhexis “running out” as the surgeon concentrates on the tip of the forceps, not realising that the shaft of the forceps is pressing on the posterior wound lip, allowing viscoelastic to leak and shallowing the AC with the inevitable consequences. This is a form of perceptual blindness most exemplified by the “gorilla in the lift lobby” experiments of Daniel J Simons.
The answer to this problem is to develop the habit of sitting properly, learned from the beginning, with repeated intentional practise. It is really important, and I strongly agree that such training should be part of the curriculum for all.
Our mobile simulation workstations are being distributed to the other units in Yorkshire, and now with orders from some hospitals in the London School, so I hope that such teaching and practice can become more regular.
Those with EyeSi products would also do well to invest in a proper chair to match the machine. Often the opportunity to teach and learn proper seating at these simulators is missed and I have often wondered why a proper adjustable seat is not included in the very expensive package.
The “operator’s chair” mentioned above is from Industrial Seating - a T2 with lock-loaded castors and reversed arms. It is inexpensive, robust and ideal for use with EyeSi and slit-lamps, as well as in surgical simulation. I have no affiliation or financial interest in the company, but I think they produce an excellent product, some still going strong in our wet lab 10 years on.
Sincerely,
Jim Innes,
Consultant Ophthalmologist (Retd.),
HILS Eye Consultant (Education),
Simulation Lead Yorkshire School of Ophthalmology, Hull, UK.
The article referred to in this letter can be found here.
COMMENTS ARE WELCOME