Aadil Hussain discusses an ophthalmologist’s risk of musculoskeletal injury and highlights the importance of ergonomics education, to ensure a pain-free career.
Chronic and disabling musculoskeletal injury has been identified in the field of ophthalmology with increasing prevalence. The ophthalmologist is vulnerable due to awkward and prolonged posturing, task repetition, equipment design, examination techniques, and the heightened cognitive load associated with fine motor tasks.
Ergonomics is the discipline focused on the relationship between human anatomy, biomechanics, and the physical components of a working environment. With increasing reports of chronic pain, the need for surgery, and potential reduction of career longevity, a spike in interest in ergonomics has been observed.
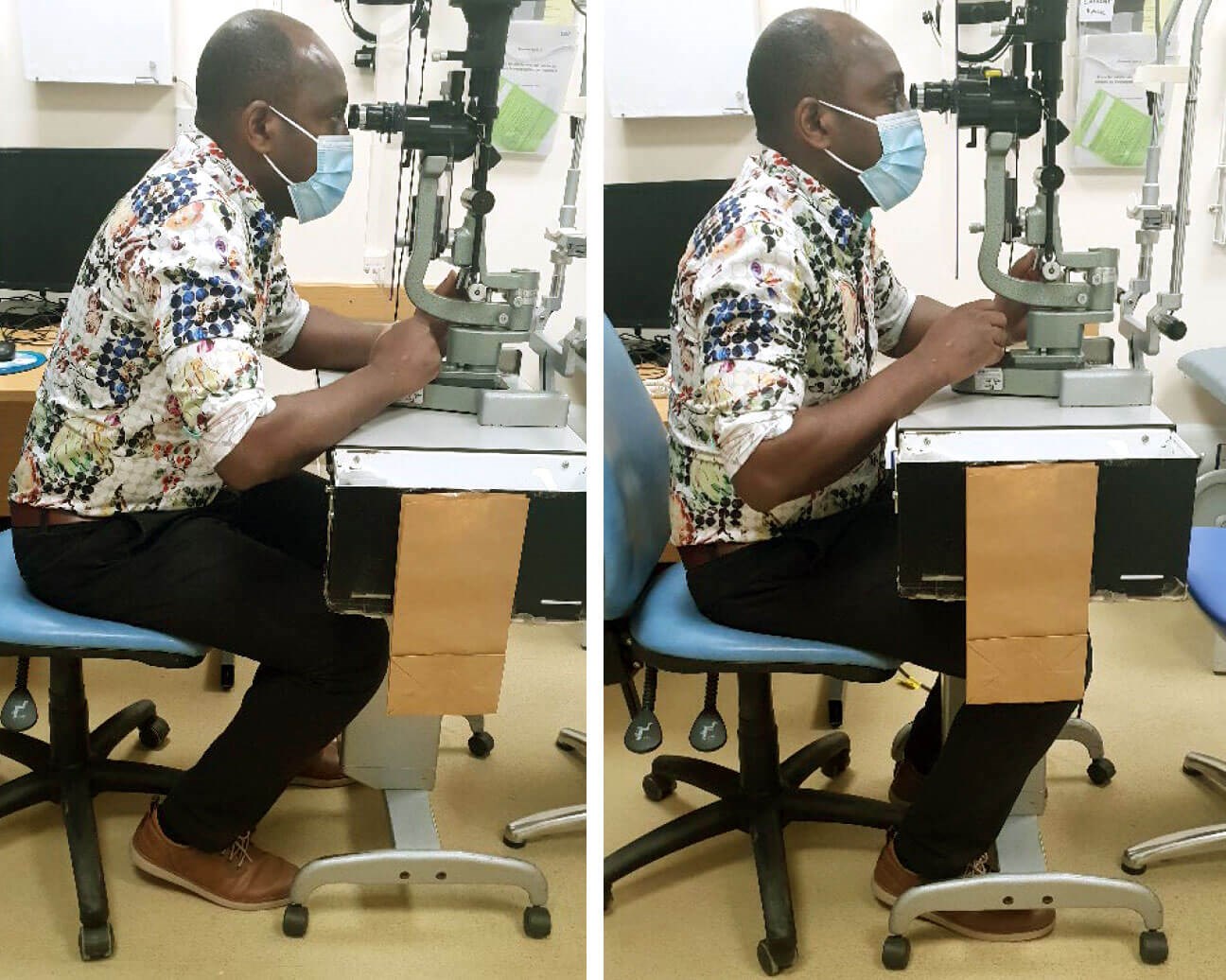
Figure 1: Awkward versus optimal slit-lamp posture.
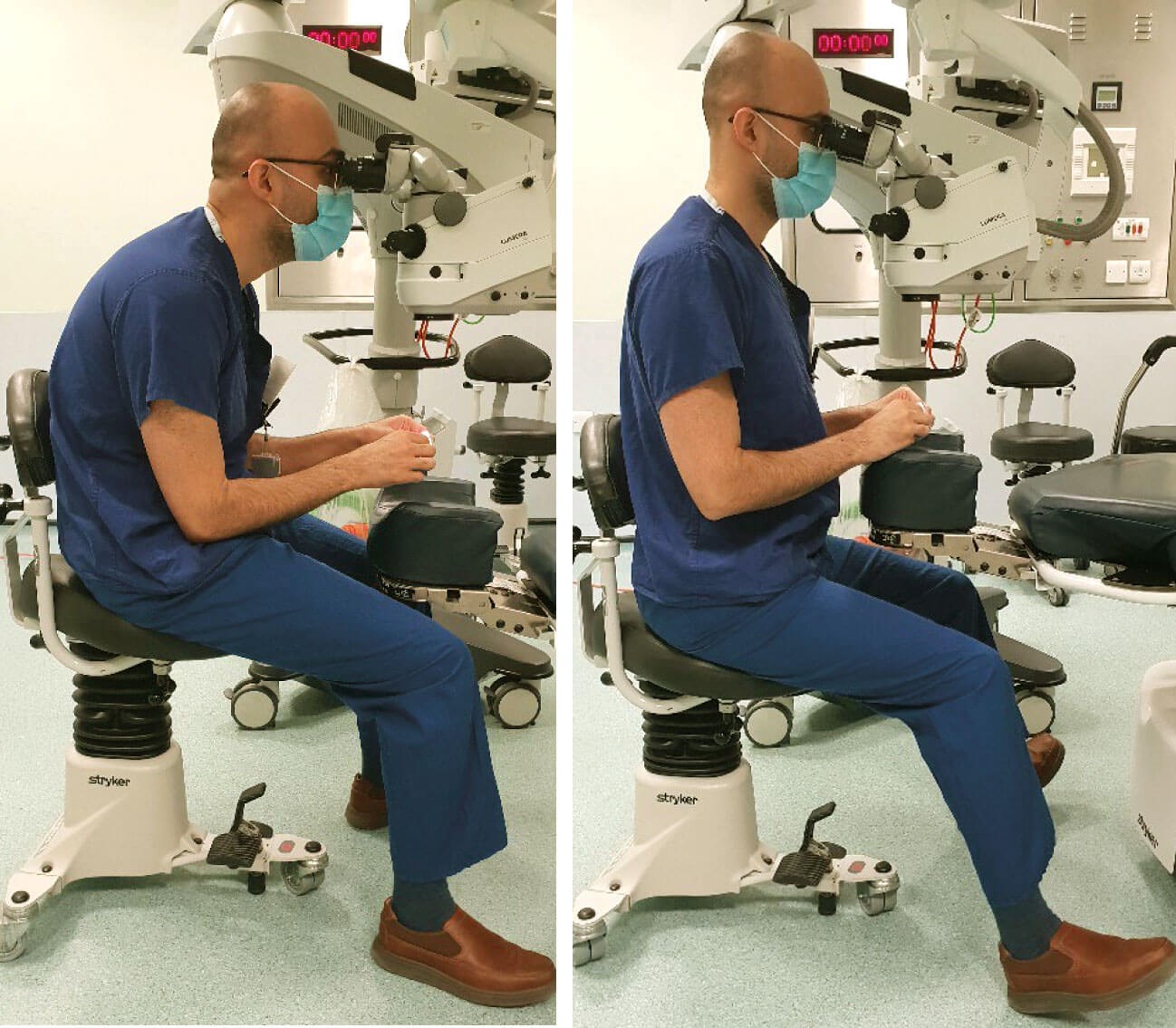
Figure 2: Awkward versus optimal slit-lamp posture.
The problem
In a 2015 UK study, 62.4% of consultant ophthalmologists reported back and / or neck pain, an increase compared to a survey two decades prior [1,2]. Of those surveyed, 57.1 % reported using nonsteroidal anti-inflammatory drugs (NSAID’s) for pain relief, 40% required physiotherapy, and, most significantly, 4.9% required surgery. Over 30% reported pain while operating or using a slit-lamp [1].
These findings correspond to data internationally. A survey of American ophthalmologists demonstrated that 52% of 697 respondents reported neck, upper body, or lower back pain, with 15% consequently having to limit their work [3]. Eighty percent of respondents reported back pain in a survey of Iranian ophthalmologists, and 71% in a survey of Indian ophthalmologists [4,5].
Ophthalmology is a branch of medicine which evokes a greater physical burden compared to other subspecialities. Musculoskeletal injuries develop insidiously due to years of practice and associated wear and tear rather than acute high-risk activities. Years of practice can render the body susceptible to injury and damage. This can manifest as chronic back and neck pain secondary to spinal degenerative diseases, as well as sciatica, and carpal tunnel syndrome. Such injuries could be devastating to the health and career of an ophthalmologist.
Risk factors in ophthalmology
A multitude of factors exist in day-to-day ophthalmic practice which may contribute to the development of musculoskeletal injury. Overarching themes are highlighted below.
Posture:
Suboptimal postures lead to strain on the back, neck, hips, and abdomen, precipitating chronic stiffness and pain. Postures utilised by an ophthalmologist are dependent on the clinical task at hand, may differ depending on subspeciality, and pose their own relative risks. For example, loose lens retinoscopy in a paediatric clinic, indirect ophthalmoscopy in vitreoretinal clinics, and a complicated general ophthalmology examination of an elderly / immobile patient. The prolonged nature of these tasks which require sustained non-neutral positioning serve to facilitate chronic injury.
Repetition of tasks:
Repetitive movements in the era of high-volume clinics and theatre lists predispose the ophthalmologist to wear and tear of the back, neck, and shoulder joints. Damage is expedited when coupled with postural factors.
Lifestyle:
Poor postural awareness and habitual postures can be developed from a young age, increasing the risk of injury if not addressed. Different levels of physical endurance and mobility are observed among ophthalmologists. General health promotion with light resistance training and mobility work, supplemented with stretches throughout the day during clinic or theatre are recommended in managing internal physical factors.
Day to day considerations
Implementing simple measures into daily practice can go a long way in avoiding the development of injury. These will be tailored to the task at hand, but some of the fundamentals for common activities in clinic and theatre are described below.
In clinic:
The slit-lamp is the most common examination tool used in a clinic setting. When using a slit-lamp, the head, neck, and spine should be vertically aligned to maintain a relaxed and neutral position. When examining a patient, it is common to lean forward bringing the neck out of alignment, exacerbating cervical lordosis and thoracic kyphosis (Figure 1). Leaning into the slit-lamp brings the hips into flexion, thus increasing load and shearing forces into the lumbar spine.
The examiner should position themselves with the slit-lamp closer to themselves to maximise vertical alignment and minimise head tilting and neck stretch. The examiner’s chair should be modified to form a hip angle slightly greater than 90 degrees (greater than the perpendicular) (Figure 1).
An elbow rest aids in controlling excessive shoulder flexion and elbow extension, as well as preventing the neck and back from becoming non-neutral. A cushioned surface also serves to protect the bony protuberances of the elbow.
In theatre:
Long durations of static positioning while operating lead to persistent time under tension in the posterior chain, contributing to fatigue and muscle exhaustion. There is a greater physical strain for surgical tasks which require fine manual dexterity and high precision as in ophthalmology. The required level of mental concentration during surgery also promotes a tense posture.
Primary focus on task completion can cause surgeons to persevere through discomfort and not identify modifiable risk factors. This is especially true for the junior ophthalmology trainee, possessing general anxieties of beginning to operate, and yet to develop the level of spatial and positional awareness subconsciously required for microsurgery. Cue the taller overarched and overextended shorter trainees almost slipping out of their chairs.
Surgery should not be started until chair, operating microscope, and table are positioned to facilitate a neutral neck and spine. Ideally the hips should be flexed at 90 degrees, with thighs parallel and feet flat on the floor, enabling relaxed and controlled access to the foot pedal (Figure 2).
Addressing the issue
An increase in musculoskeletal injury has been associated with length of practice. This rationalises early proactive intervention with preventative measures as the most suitable approach in managing risk of injury. Regular self-assessment of one’s own ergonomic practice could include identifying high-risk behaviours and optimising the surrounding physical environment.
Implementing ergonomics education into the training programme curriculum as a formal requirement would have the greatest impact on a young ophthalmologist’s movement strategy for daily clinical activities.
As seen internationally with the American Academy of Ophthalmology Task Force, a designated group consisting of ophthalmologists and ergonomics experts could aid in the design of educational ergonomic modules and guidelines for trainee ophthalmologists. Such guidelines could highlight a prevalence of musculoskeletal injuries, address risk factors, and describe ergonomic techniques for a large variety of activities in greater depth.
Efficacy for educational ergonomic modules has been reported. In a Canadian study determining risk of injury in ophthalmology residents completing indirect ophthalmoscopy, injury risk scores decreased following the completion of learning modules outlining proper ergonomic technique and risk factors. Results from the study also identified ergonomic markers requiring further work which could then be addressed and incorporated into future modules [6].
Currently, assessable training requirements, modules, or guidelines are yet to be incorporated into the formal curriculum of ophthalmic specialty trainees in the UK. Scope could be further extended with workshops introduced into practical courses organised and run by the Royal College of Ophthalmologists such as the ‘Microsurgical skills’ and ‘Introduction to phacoemulsification’ courses. This would be tailored for new and aspiring trainees - the demographic which would receive greatest benefit. Lectures and stations at national conferences and meetings provide further options.
Looking ahead
Quantitative studies have confirmed the increasing prevalence of musculoskeletal injury and have culminated in qualitative ergonomic advice being produced. Beyond this, the objective scientific analysis into what makes ergonomic postures and equipment designs effective currently remains limited.
With the advent and application of newer technologies, the potential for objective analysis is becoming increasingly available. Such measurement systems will be able to assess joint and postural control and confirm efficacy of purported ergonomic techniques and designs. However, these remain a fresh avenue to venture into, with data specific to the movement needs of an ophthalmologist limited.
Kinematic data can now be obtained with three-dimensional video capture and motion analysis of live, simulated, or recorded surgery. Biomechanical motion analysis has been previously used to evaluate surgical skill in intraocular surgery and oculoplastics [7,8]. Systems comprise of multiple fixed synchronised cameras in a test setting and can collect and compare postural data from the head, neck, and wrists. Collected data can assist with determining postural angles and movement velocity over joints with at-risk movements identified and modified accordingly.
Electromyography (EMG) data has been used to determine muscular efforts and fatigue, as well as repetition and degree of movements. The duration of static postures and associated amplitudes of muscular tension may provide important data due to high levels of static loading and repetition exhibited in ophthalmology. Data has been collated from experimental and real-time clinical / surgical settings, highlighting preferential muscular efforts, with evidence dictating ergonomic recommendations [9].
Refinement in the application of such methods is needed, but there remains a wide scope in utilising these to determine key biomechanical markers of ergonomic techniques in the field of ophthalmology.
Conclusion
The worldwide effects of musculoskeletal disorders on ophthalmologists are significant. These predominantly stem from the insidious effects of routine clinical activities. Minimal interventions within day-to-day practice can make a positive difference. Methods to objectively analyse ergonomic techniques are continuously updated, with findings implemented into producing new recommendations. There is an opportunity for effective ergonomic practices to be incorporated formally into ophthalmic specialty training.
TAKE HOME MESSAGE
-
Ophthalmologists are disproportionately predisposed to musculoskeletal injury and chronic pain.
-
A proactive versus reactive approach of incorporating good ergonomic habits and preventative measures best facilitates for career longevity.
-
Wide scope exists for ergonomic education to be included in the specialty training curriculum.
-
Advancing technology will objectively determine optimal ergonomic markers and dictate best postural practice.
-
Always seek help if you begin to experience back / neck pain.
Acknowledgements: A special thank you to Yomi Imasogie and Abhijeet Yadav for their assistance in producing the images used in this article.
References
1. Hyer JN, Lee RM, Chowdhury HR, et al. National survey of back & neck pain amongst consultant ophthalmologists in the United Kingdom. Int Ophthalmol 2015;35(6):769-75.
2. Chatterjee A, Ryan WG, Rosen ES. Back pain in ophthalmologists. Eye (Lond) 1994;8(4):473-4.
3. Dhimitri KC, McGwin G, McNeal SF, et al. Symptoms of musculoskeletal disorders in ophthalmologists. Am J Ophthalmol 2005;139(1):179-81.
4. Chams H, Mohammadi SF, Moayyeri A. Frequency and assortment of self-report occupational complaints among Iranian ophthalmologists: a preliminary survey. MedGenMed 2004;6(4):1.
5. Venkatesh R, Kumar S. Back pain in ophthalmology: national survey of Indian ophthalmologists. Indian J Ophthalmol 2017;65(8):678-82.
6. Ratzlaff TD, Diesbourg TL, McAllister MJ, et al. Evaluating the efficacy of an educational ergonomics module for improving slit lamp positioning in ophthalmology residents. Can J Ophthalmol 2019;54(2):159-63.
7. Saleh GM, Lindfield D, Sim D, et al. Kinematic analysis of surgical dexterity in intraocular surgery. Arch Ophthalmol 2009;127(6):758-62.
8. Saleh GM, Litwin A, Collin JR, et al. Kinematic analysis in oculoplastic reconstructive surgery: measuring manual control and fluidity of movement. Arch Ophthalmol 2012;130(12):1570-4.
9. Stucky CH, Cromwell KD, Voss RK, et al. Surgeon symptoms, strain, and selections: Systematic review and meta-analysis of surgical ergonomics. Ann Med Surg (Lond) 2018;27:1-8.
COMMENTS ARE WELCOME






