Incomitant vertical and / or horizontal strabismus is a challenging presentation. Patients are usually symptomatic as the onset is either sudden so they haven’t developed any coping mechanisms or very complex so that any coping mechanisms will not cover all the field of binocular single vision.
In this article we will have an overview of common conditions that present with incomitant strabismus and discuss various surgical management strategies.
Duane’s syndrome
For the purpose of surgical management, Duane’s syndrome could be classified into typical and atypical types. The typical Duane presents with limitation of abduction and esotropia in primary position and the atypical type presents with limitation of adduction or abduction and exotropia (or orthophoria) in primary position. In the typical type, surgical treatment will depend on the degree of esotropia in the primary position as well as the presence of any compensatory head posture and upshoots or downshoots. It is suggested that options will include recession of the ipsilateral medial rectus (MR) muscle or asymmetric bilateral MR recessions (+/- contralateral MR Faden).
Newer techniques or superior rectus (SR) (+/- lateral rectus) temporal transpositions could be considered, but with attention to the possibility of creating vertical or torsional imbalance.
In cases of up shoots and down shoots it is possible to recess the ipsilateral LR muscle combined with ipsilateral MR recession (+/- contralateral MR recession depending on the angle of esotropia). This could be combined with Y splitting procedure to the ipsilateral lateral rectus (LR) muscle.
Management of atypical Duane will usually need supramaximal recession of the ipsilateral LR (+/- ipsilateral MR resection).
Dissociated vertical deviation (DVD)
It usually presents as part of the infantile esotropia triad so can be present in combination with inferior oblique muscle (IO) overaction but it is important to differentiate the two conditions. Surgical management options include IO anteriorisation or large SR recession. The first option helps with both IO overaction and DVD hence can be used in cases where the two are present, while SR recession could be used in cases with absent IO overaction or if the anteriorisation procedure fails to control the DVD. If the DVD persists after the SR recession, IO recession could be performed if not operated on before.
Thyroid eye disease (TED)
Despite the slow onset and progress of this condition, patients will suffer from diplopia due to the asymmetric nature of muscle contracture and limitations of movements. Most common findings are limitation of elevation and abduction. This is due to tightness of inferior rectus (IR) and MR muscles. This usually creates esotropia and vertical imbalance in the primary position. Surgical options are usually limited to muscle recessions as performing resections on such muscles is advised against. Esotropia is usually managed by unilateral or bilateral MR recessions. The amount of recessions is judged by performing intraoperative forced duction tests (FDT) and finding the so-called muscle resting position. Vertical imbalance is usually more challenging to correct and the strategy will depend on the angle of deviation in the primary position and in down gaze. Options include recession of IR of the lower eye (+/- recession of the SR of the higher eye) or bilateral IR recessions (usually asymmetrically) with or without recession of the SR in the higher eye aiming for a small under correction. The choice of suture material (non-absorbable or absorbable) and the use of adjustable sutures depends on the surgeon’s choice as well as the tightness of the muscles and suitability of the patient. There is some tendency to avoid putting the IR muscle on adjustable sutures, especially while using absorbable material. It is possible to put the SR muscle on adjustable sutures more safely.
Brown’s syndrome
In this condition patients are usually binocular in the primary position, but they could be aware of diplopia on elevation. They are also concerned about the appearance of their eyes (downshoot on adduction) or an abnormal head posture or hypotropia in primary position. This syndrome could be unilateral or bilateral and could be congenital or acquired. The surgical strategy usually necessitates weakening of the ipsilateral superior oblique (SO) muscle. The usual option is SO tendon expander using either a silicon band (usually 6mm) and using chicken wire non-absorbable suture. It is usually advised to avoid doing total SO tenectomy or tenotomy as this can lead to significant torsional imbalance.
Orbital floor fracture
There are several concerns following orbital fractures from the ocular motility point of view. These include incarceration of the IR muscle or its peri-muscular tissue and paresis of the muscle due to damage to its innervation. Most of these cases will be seen by maxillofacial or orbital colleagues before being referred for squint management. The ocular motility intervention will depend on the patient’s symptoms, such as diplopia or abnormal head posture, the time passed since the trauma and any chances of spontaneous recovery and the angle of deviation in primary position and in down gaze. If there is a limitation to elevation in the affected eye then possible strategies include: ipsilateral IR recession if it is tight (+/- contralateral IO or SR recession with or without Faden).
If there is limitation of depression in the affected eye then transposition of ipsilateral MR and LR muscles inferiorly, ipsilateral IR resection and SR recession or contralateral SO or IR weakening procedures could be considered. If there is a limitation of elevation and depression of the affected eye then contralateral SR and IR recessions with or without Faden could be offered.
III cranial nerve palsy
Various techniques have been considered in the surgical management of the III cranial nerve palsy. In cases of complete III nerve palsy, it is rarely possible to achieve any ocular motility and the usual aim is to have good centralisation of the globe. There are several techniques that could be considered. These include supramaximal recession of the LR muscle (+/- anchoring to the lateral orbital wall) and large MR resection. It might be necessary to perform a weakening or transposition of the SO muscle to aid centralising the globe. It might also be necessary to use traction sutures through the insertions of the SR and IR muscles to pull the globe into an adduction position in the immediate postoperative period. Another strategy that gained some popularity recently is splitting and transposing the LR muscle nasally around the globe and suturing it above and below the MR insertion.
In cases of partial III nerve palsy, the surgical strategy will depend on the affected muscle(s), the angle of deviation in the primary position and the area of maximal deviation. Common combinations would be resection of the affected muscle (such as MR muscle) and recession of its antagonist (LR muscle), or transposing neighbouring muscles (such as the SR / IR) nasally. Other strategies include surgery on the contralateral yoke muscles to balance the weakness (recession +/- Faden).
IV cranial nerve palsy
This could be congenital or acquired and patients could be symptomatic with diplopia or compensatory head posture or aware of their hypertropia. Various classifications have been used to discuss the spread of comitance in the vertical imbalance with the passage of time and to suggest surgical strategies. There are several principles that have been adopted in managing patients with IV nerve palsy. These include: Surgical treatment for torsion usually takes priority if it was a barrier to fusion. This would need a Harada Ito procedure which could be unilateral or bilateral depending on the angle of torsion measured. Incomitant vertical imbalance usually needs surgery on oblique muscles. If the angle of deviation is larger in elevation positions, ipsilateral IO recession is usually the procedure of choice, while if the deviation is larger in depression positions SO tuck could be performed. Comitant vertical deviation will necessitate surgery of rectus muscles. This could be SR or IR recessions (depending on the position of maximal deviation) or transposition of MR and LR either superiorly or inferiorly (depending on the area of maximal deviation). Angles of deviation that are larger than 15 prism dioptre usually require surgery on two muscles. This could be done as a staged procedure to avoid over corrections. Common combinations are ipsilateral IO recession and ipsilateral SO tuck or contralateral IR recession. In cases of bilateral IV nerve palsy and V pattern, surgery on MR muscles to address the pattern might be needed.
VI cranial nerve palsy
The surgical strategy will depend on the angle of deviation in primary position as well as the amount of limitation of abduction and the ipsilateral MR contracture. In cases of paresis with limitation of abduction of -1/-2, it is possible to perform a large recess / resect procedure (+/- contralateral MR recession) with good outcome. It is also possible to put both muscles on adjustable sutures to avoid large postoperative over corrections and diplopia. In cases of complete palsy (limitation of abduction of -3/-4) it is usually necessary to perform a temporal transposition of the SR (+/- IR) muscle(s) with or without Foster sutures combined with botulinum toxin to the ipsilateral MR which might need to be recessed at a later stage. Attention should be paid to avoid creating any vertical or torsional imbalance.
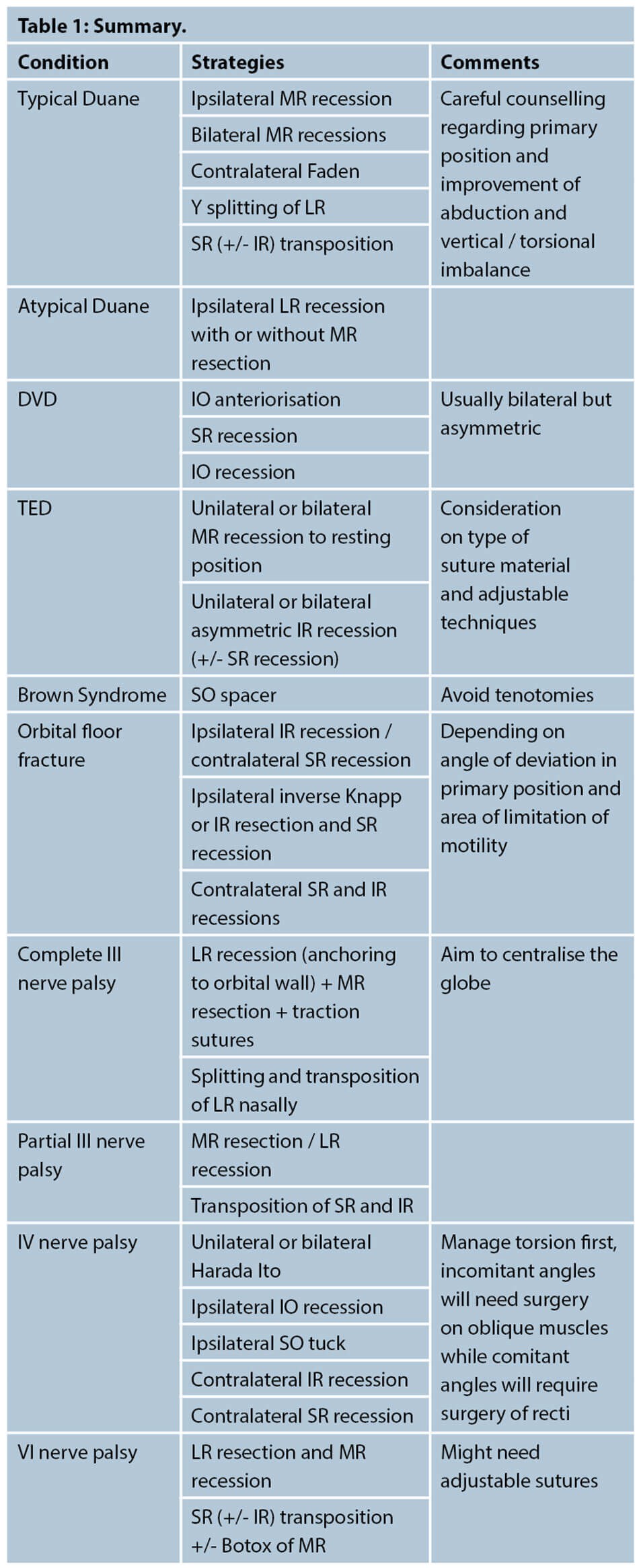
Summary
Incomitant ocular motility imbalance is a challenging presentation and should be managed carefully with meticulous planning, detailed orthoptic assessments, multidisciplinary team (MDT) discussions and careful counselling of patients and managing their expectations (most patients will have some residual diplopia but aim for a useful field of binocular single vision in primary position and in down gaze) in order to avoid any potential complaints or unexpected outcomes.
Further reading
- Ferris JD, Davies PEJ. Surgical Techniques in Ophthalmology: Strabismus surgery. Elsevier Inc: Amsterdam, Netherlands; 2007:131-64.
- Ansons A, Davis H. Diagnosis and Management of Ocular Motility Disorders. Wiley Blackwell: New Jersey, USA; 2013: 462-528, 543-611.
COMMENTS ARE WELCOME






