The aim of management for all patients with strabismus should centre around four goals: to prevent amblyopia, to alleviate symptoms, to restore binocular single vision (BSV) and to improve ocular alignment.
The conservative management options available for strabismus include observation, occlusion, optical, orthoptic exercises and the use of prisms. A summary of the options and the indications for use are available in Figure 1. Some of these options can be used diagnostically and therapeutically, however, only the therapeutic options will be discussed in this article.
Figure 1: A summary of conservative management options for concomitant strabismus.
Management option: Observation
Indications:
-
Well-controlled intermittent deviation in young patients with potential risk of amblyopia
-
Parent / patient refuses treatment
-
Uncertainty of how best to treat, e.g. variable test results
What to do:
-
Regular orthoptic assessments to assess the patient’s VA, control of deviation (e.g. cover test, controlled binocular acuity and Newcastle control score), angle of deviation and BSV.
Management option: Occlusion
Indications:
-
To treat amblyopia
-
To relieve diplopia
What to do:
-
Options include conventional patching or Atropine 1% twice weekly
-
Follow PEDIG guidelines
-
Allow refractive adaptation
Management option: Optical
Indications:
-
To improve VA
-
To improve BSV
What to do:
-
Prescribe the full hypermetropic correction if patient esotropic
-
Trial extra plus lenses (up to +3.00DS) if convergence excess suspected
-
Trial minus lenses (up to -3.00DS) in intermittent distance exotropia
Management option: Orthoptic Exercises
Indications:
-
To improve BSV and alleviate symptoms
-
Wean out of extra lenses and prisms
What to do:
-
For eso deviations, focus on improving negative fusional amplitudes and negative relative vergence
-
For exo deviations, focus on improving convergence, positive fusional amplitudes and positive relative vergence
Management option: Prisms
Indications:
-
To alleviate symptoms and restore BSV
What to do:
-
For eso deviations, base-out (BO) prism
-
For exo deviations, base-in (BI) prism
Observation
The indications for observation versus active management are stated in Figure 1. This option is often not thought of as a management plan but may be essential in some cases. For example, if a patient’s strabismus is unstable, observation is essential before deciding on further treatment. However, they should still be regularly followed up and it should be ensured that there is no benefit to active treatment. For instance, if a young patient’s intermittent deviation begins to decompensate, treatment must be initiated. Therefore, regular orthoptic investigations should be maintained to monitor the areas stated in Figure 1. Specific tests such as the Newcastle Control Score have been encouraged when observing intermittent distance exotropia (IDEX) to help decide whether surgery is indicated [1].
Occlusion
Occlusion can be used to improve VA, relieve diplopia or to disrupt suppression. To improve VA, conventional patching of the non-amblyopic eye can be prescribed, the number of hours required is dictated by the level of vision and evidence-based practice regime suggested by Paediatric Eye Disease Investigator Group (PEDIG). For moderate amblyopia (6/12-6/30) up to two hours is suggested, whereas, up to six hours is suggested for severe amblyopia (6/30-6/120) [2,3]. In cases of eccentric fixation, prior to conventional occlusion, a short period of inverse occlusion of the affected eye may be beneficial to help break the fixation pattern.
There is little evidence to suggest that inverse occlusion is effective, therefore this is not common practice. An alternative to ‘patching’ is the use of one drop of atropine 1% twice weekly. PEDIG have found that atropine is equally effective for those with moderate amblyopia [4]. It is also an effective treatment for those with severe amblyopia, especially those aged three to six [5]. It is important to note that prior to any occlusion a patient should be refracted, and a sufficient period of refractive adaptation should be allowed (up to 18 weeks). Stewart et al. reported a mean improvement of 0.24 LogMAR from refractive correction alone [6].
Optical
Besides the use of lenses to correct refractive error and hence improve VA, lenses may be used to manipulate accommodation and convergence, and improve control manifest and latent deviations. The principle of this is that convex lenses encourage relaxation of accommodation hence reducing the amount of convergence exerted, whereas concave lenses stimulate accommodation and therefore encourage extra convergence.
Convex lenses are used to treat accommodative esotropia. The full hypermetropic correction should be prescribed, where tolerated, to determine if BSV can be restored (fully accommodative esotropia). If the angle is reduced, but BSV is not achieved, the use of extra plus lenses (up to +3.00DS) should be explored. In cases of convergence excess esotropia (CXS) the patient will become binocular. This is due to patients with CXS having a high accommodative convergence / accommodation ratio (AC/ A). For CXS patients, bifocals can be prescribed and have been shown to be an effective short- to medium-term management option for establishing good BSV. In the long-term some patients can be weaned out by orthoptic exercises whilst others may progress to surgery. In cases of consecutive exotropia, reducing the strength of the hypermetropic/convex spectacles may possibly result in a satisfactory outcome, as more accommodation and convergence can be exerted.
Concave lenses (of up to -3.00DS) can be used in IDEX’s to achieve control of a manifest deviation and hence restore / maintain normal BSV. Over time the strength of the concave spectacles can be reduced if the patient can control their deviation, and if they cannot the patient may go on to have surgery. To help patients achieve better control orthoptic exercises might be prescribed in conjunction with concave lenses to help improve convergence and negative fusional amplitudes. Authors have suggested trailling minus lenses in all IDEX types with poor control, however, Kushner suggested that they work best in those with a high AC/A [7].
Orthoptic exercises
Orthoptic exercises can be used to improve control, alleviate symptoms, or to wean patients out of lenses or prisms. They can only be used in patients who are able to appreciate physiological diplopia. Options include convergence exercises (e.g. pen convergence and dot card), improving fusional amplitudes (e.g. homemade prism bars) and improving relative vergence (e.g. bar reading or stereograms). Suppression is a contraindication for exercises, anti-suppression can be undertaken but the safety of this is questionable. There is little evidence base to support the use of exercises, especially in the management of esotropic deviations but good outcomes can be achieved [8]. Success will be affected by the level of patient compliance and appropriate patient selection.
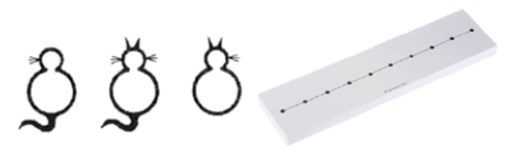
Figure 2: A cat stereogram (used to improve relative vergence) and dot card (used to improve convergence).
The focus in esotropic deviations is on improving negative fusional amplitude (using base in prisms) and negative relative convergence (using distance stereograms or bar reading). Such exercises can be used to wean patients with fully accommodative and convergence excess esotropias’ of out extra lenses that are not necessary to improve vision. The patient needs to be cooperative and able to attend the clinic regularly, have a deviation <20PD and a refractive error <+3.00DS/1.00DC [9].
The aim of orthoptic exercises in exotropic deviations is to improve convergence, positive fusional amplitudes (using base out prisms) and positive relative convergence (using near stereograms). For esophoric and exophoric patients’ exercises may be used to improve control and relieve asthenopic symptoms (e.g. frontal headaches, ache behind eyes and diplopia), and the same pre-requisites apply. It is important to tell patients to relax their eyes after completing the exercises as spasm of the near reflex can be caused by overzealous use.
Alternate occlusion is an emerging therapy used in IDEX without a fixation preference. This is an anti-suppression exercise with an aim to remove suppression present under binocular conditions and improve binocularity. However, there is a lack of evidence to prove that alternate occlusion is an effective treatment. The use of alternate occlusion is therefore uncommon in the UK.
“The success of therapy is largely based upon suitable patient choice and the level of compliance”
Prisms
Fresnel prisms may be used to help restore and maintain BSV in children with late-onset strabismus, or decompensating latent deviations who experience diplopia. They are cut out and stuck onto a pair of spectacles (plain lenses if patient does not wear spectacles) with the apex of the prism orientated in the direction of the deviation. Fresnel prisms are often used in the short-term with progression to surgery, however, they can be incorporated into spectacles for a more long-term option if surgery is contraindicated. Alternatively, orthoptic exercises can be used to improve control whilst prism strength is reduced gradually. It is important to remember if the deviation is particularly large, prisms may not be suitable as they may blur the patients VA and thus prevent BSV.
Conclusion
Conservative management options include: observation, occlusion, optics, orthoptic exercises and prisms. They are a feasible alternative or adjunct to strabismus surgery, but may not be suitable for all patients. Patients/parents should be carefully selected and consulted about their management choice. Their ocular condition should be monitored once treatment is commenced and therapy should be altered if necessary. The success of therapy is largely based upon suitable patient choice and the level of compliance. Further research is required in specific areas, such as the use of alternate occlusion in intermittent distance exotropia.
References
1. Buck D, Hatt SR, Haggerty H, et al. The use of the Newcastle Control Score in the management of intermittent exotropia. Br J Ophthalmol 2007;91(2):215‑8.
2. Repka MX, Beck RW, Holmes JM, et al. Pediatric Eye Disease Investigator Group. A randomized trial of patching regimens for treatment of moderate amblyopia in children. Arch Ophthalmol 2003;121(5):603-11.
3. Holmes JM, Kraker RT, Beck RW, et al. Pediatric Eye Disease Investigator Group. A randomized trial of prescribed patching regimens for treatment of severe amblyopia in children. Ophthalmology 2003;110(11):2075-87.
4. Pediatric Eye Disease Investigator Group. A randomized trial of atropine vs patching for treatment of moderate amblyopia in children. Arch Ophthalmol 2002;120:268‑78.
5. Repka MX, Kraker RT, Beck RW, et al. Treatment of severe amblyopia with weekend atropine: results from 2 randomized clinical trials. J AAPOS 2009;13:258-63.
6. Stewart CE, Moseley MJ, Fielder AR, et al. Refractive adaptation in amblyopia: quantification of effect and implications for practice. Br J Ophthalmol 2004;88:1552‑6.
7. Kushner BJ. Diagnosis and treatment of exotropia with a high accommodation convergence-accommodation ratio. Arch Ophthalmol 1999;117(2):221-4.
8. Aziz S, Cleary M, Stewart HK, Weir CR. Are orthoptic exercises an effective treatment for convergence and fusion deficiencies? Strabismus 2006;14(4):183-9.
9. Ansons A, Davis H: Diagnosis and Management of Ocular Motility Disorders. 4th edition. Wiley & Sons Ltd: Oxford, UK; 2014.
COMMENTS ARE WELCOME





