Learning how to refract requires theoretical knowledge, practice and determination. Refraction is a notoriously challenging skill to acquire and the competing demands on junior ophthalmologists can often be restrictive of the development of this core skill. To consolidate theory learnt from textbooks, refraction courses have become popular amongst those preparing for professional exams.
Each individual has a preferred learning style which influences the way they engage in such courses. A number of tools have been developed to identify these learning ‘preferences’ or ‘styles’; one of the most widely known being Honey and Mumford’s, which is based on a questionnaire and an associated matrix of characteristics. Their work suggested that learners will tend to exhibit a preferred learning style (Figure 1) [1,2].

Figure 1: Honey and Mumford’s learning theories.
Applying theory to practice in a short time period is a challenge. Designing an optics and refraction course requires a strategy on how to structure / organise the sessions and clear learning outcomes must be arrived at. Choosing the appropriate learning environment and strategies to promote preparation or consolidation of learning are essential, as well as course-based activity. The pre-course material is invaluable here as is an awareness of the learning methods of the target delegates.
A proposed course needs to be constructively aligned to the professional refraction examinations and designed according to the RCOphth curriculum. In 2015 the first South West Peninsula Refraction course (SWPRC) was delivered to teach basic refraction skills to trainee ophthalmologists. The course aimed to solve practical problems to which answers are not easily accessible in the textbooks.
The programme entailed a full day of lectures and practical sessions, followed by mock assessments. The course was held at the School of Health Professions at Plymouth University, in a purpose built Peninsula Allied Health Centre near Derriford Hospital. Delegates were given logbooks to work through during the practical sessions with one-to-one tuition and video modules on focimetry and hand neutralisation of spectacle lenses. Pre-course reading was sent to each of the delegates outlining basic refraction techniques with useful tips and advice on objective and subjective refraction. Delegates enjoyed the practical and interactive sessions and each left with structured plans on how to put their new learnt skills to practice / towards their upcoming assessments.
“The success of any such teaching and learning activity is dependent upon the experience of the tutors and the quality of the resources provided.”
The success of any such teaching and learning activity is dependent upon the experience of the tutors and the quality of the resources provided. As such the tutors involved in the SWPRC are all experienced optometry lecturers and practitioners or previous examiners. The feedback from the course and the success in the latest round of examinations highlighted the importance of high quality tailored one-to-one tutorials.
To balance the budget effectively it was essential to confirm delegate numbers early, confirm sponsor / deanery contributions – the main contribution, and confirm catering costs. Once the delegate numbers were confirmed the task of making up conference packs must be completed, including certificates, timetables, feedback forms, name badges and stationery.
Given the success of the 2015 course we are pleased to confirm that the SWPRC will be returning in 2016 and hope to welcome more delegates on board. Should you be interested in attending the November 2016 course please feel free to contact our team.
References
1. Mumford A: Putting learning styles to work. In Action learning at work. Brookfield, VT: Gower; 1997:121-35.
2. Honey P, Mumford A. Learning styles questionnaire: 80-item version. London; 2006.
Acknowledgments:
Professor N Habib, Mr A Booth, Mr Kieran Loft, Mr Adam Jones, Mr K Vadhani, Dr J Huelle, Dr Hetal Buckhurst, Mrs Susan Sian. Ms Hirut Von Lany and Peninsula Ophthalmology Meetings and The Plymouth School of Optometry.

Mr Kieran Loft discusses the ‘art’ of refraction.
Why organise a skills course?
-
To fill gaps in your own clinical knowledge
-
To help fellow trainees
-
To promote local awareness
-
To network
-
To encourage discussion
-
To add to your CV / portfolio
-
To give yourself a challenge.
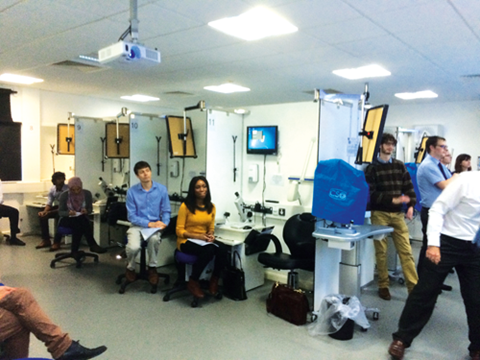
Delegates being introduced to the optometry teaching facilities at the Peninsula Allied Health Centre.
Balancing the budget: important features
-
Confirm sponsorship fees
-
Collect delegate fees
-
Deanery funds may be available
-
Venue/ catering costs
-
Speakers accommodation / travel fees / gifts
-
Cost of delegate packs.

Group sessions – Examination ‘pearls’ by Professor Nabil Habib.
Important evaluation and learning points
-
Was there a structured team? Yes, all tasks were delegated prior to the meeting
and we successfully shared the workload.
-
Were the presentations relevant to the topic of the course? Yes, with positive feedback.
-
Were goals for the course and its activities met? Yes, as per the learning curriculum devised.
-
Was the venue suitable? Yes, a purpose built centre –
https://www.plymouth.ac.uk/schools/
school-of-health-professions/
peninsula-allied-health-centre -
Were delegates engaged in the topics? Yes, we ensured logbook exercises could be discussed at the end of each practical session in groups.
-
Was the time allotted appropriate? Yes, there was ample time to discuss all aspects of the learning curriculum with an emphasis of the importance of regular practise of the skills learnt.

Video modules and one to one refraction tuition.
Practical tips to remember
-
During retinoscopy, a target should be used that will promote accurate and steady fixation with no stimulus to accommodation. The fixating eye controls accommodation, it must therefore be fogged to ensure that accommodation is relaxed.
-
Plus cylinders tend to give a clearer, more easily neutralised streak and are favoured by some practitioners who rely on retinoscopy to provide a final prescription (e.g. working with children).
-
Using minus cylinders does ensure that accommodation is better controlled. Minus cylinders are more commonly used in routine refraction.
-
Modify the spherical element when changing the power of the cylinder, in order to keep the circle of least confusion on the retina. As a general rule, every cylinder change should be matched with a change of sphere by half the amount and with the opposite sign.
-
Binocular refraction should not be used where acuities are markedly unequal, or one eye is strongly ‘dominant’.
-
In such cases, occlude the better eye, refract the worst eye. Then refract the better eye with the worst eye fogged.
-
If the spherical power was correctly calculated prior to cylinder refinement, the patient should be slightly under-plussed. If the patient requires more minus at this stage, it most likely is due to under minusing on the cylindrical power.
COMMENTS ARE WELCOME