The advent of simulation technology has enhanced modern medical training. The first utilisation of simulation was in 1929 where Edward Link used this concept to develop a mechanical flight simulator [1]. Industries such as aviation, nuclear power and the military all use simulation as a core part of their training. As a result simulators have increasingly become available, with special emphasis on invasive surgical procedures which are associated with a substantial learning curve such as modern cataract surgery [2].
The Royal College of Ophthalmologists curriculum requires 50 cataract cases to be conducted by a trainee over the first two years of training, and 350 after seven years. To meet these requirements in the current NHS environment trainers must look to other forms of teaching rather than the traditional approach many have encountered of ‘see one, attempt one, teach one’.
For simulation to be successful as a teaching tool an awareness of how students learn and the impact of the nature of the teaching and learning environment is essential. This has been shown to promote the learning approach adopted by the students (Kember et al. 2008, Ramsden 1988). A drive towards adopting teaching approaches that promote ‘deep’ rather than ‘surface learning’ (Fry et al. 2008) is important for skills to be learnt and maintained. Newly acquired knowledge needs to be facilitated through active experiential, problem-based or research-based learning and encouraging continual development of their knowledge base by revisiting and expanding on key concepts. An example of this in a real training setting is regular practice with the simulation facilities [3].
Biggs and Tang (2011) suggested that good teaching is to facilitate most students to use the higher cognitive level processes that the more academic students use spontaneously. Such teaching methods will enable the maximum number of trainees to meet the learning objectives of the simulation modules and, additionally, in the case of ophthalmology, the competencies set out in the Royal College’s core curriculum [4]. The constructivism theory of learning (Fry et al. 2008, Fosnot and Perry 1996), illustrates that teaching in a way that enables students to take things back to ‘first principles’ and then construct their own knowledge and understanding of a subject is key in effective learning. This is very relevant in the context of eye surgery simulation training as all skills learnt must be constantly worked on and improved, however, the basic skills will always be key [5].
The educational literature suggests that simulation schemes that have been successful had carefully constructed education and training programs that objectively evaluated technical skills and the learning experience. Introducing trainees to surgery as an assistant in theatres followed by a wet-lab experience has shown to increase success with the virtual-reality modules. The simulation programs have then given insight into the variations surgery can pose with different clinical scenarios and complications. A similar approach was implemented in a general surgery training program using a GI endoscopy simulator with great success [6].
Simulation training in microsurgery has three defining steps; 1) skills generalisation, 2) skills transfer and 3) simulation applied cognition. Most surgical researchers appear to interpret cognition as knowledge or decision-making. Undoubtedly, knowledge is crucial for the practice of surgery, however, behavioural or cognitive scientists would have some difficulties with the very restricted interpretation of knowledge or decision-making as cognition. Knowledge and decision-making are really only the end product of a process of perception, attention, information processing, information storage and then retrieval from long-term memory at the appropriate time as ‘knowledge’ which helps the individual make their decision [6].
(1) Skills generalisation refers to a training situation where the trainee learns fundamental skills that are crucial to completion of the actual operative task or procedure.
(2) Skills transfer refers to a training modality that directly emulates the task to be performed in vivo or in the testing condition.
(3) Simulation applied cognition refers to aspects of human behaviour that are crucial for safe minimum incision surgery performance, and none seems to be less understood by surgeons than cognition. From reading the surgical literature, most surgical researchers appear to interpret cognition as knowledge or decision-making.
Simulation vs. traditional methods
On the question whether simulation is non-inferior to traditional methods we can evaluate current surgical training which follows the Halsted model, where trainees achieve surgical competence by gaining knowledge from literature, observing procedures and then performing surgery on real patients under the supervision of an experienced surgeon ‘see one, do one, teach one’. Trainees are appraised on the number of procedures they have conducted but not necessarily the quality [5].
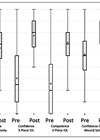
Saleh et al. compared simulation to traditional surgical teaching [7]. This is the first study of its kind looking at the effect of supervision during ophthalmic simulation training. It concluded that structured simulation teaches a significant degree of skill to early trainees. It is apparent that this was only the case when a structured course was in place, requiring trainees to pass through set tasks in the same order. Sixteen individuals were involved in the study and underwent simulation training for cataract surgery. The outcomes assessed were the total score from the simulator obtained at the beginning of the training compared to the score after supervised training, analysed using the Wilcoxon signed-rank test set at a significance level of 0.05. Improvement after the course was evident in all parameters and found to be statistically significant, representing a marked improvement in capsulorhexis procedures (circular incisions) and anti-tremor. Such skills are the hardest to master during training and most likely to cause complications in live patients.
Ultimately the goal is to establish programmes which aim to accelerate trainee learning, benefit trainers and improve patient safety in surgical training. Simulation technology provides a means for learners to engage in acquisition and practice of clinical skills without using live patients. Simulation users should weigh the benefits and costs of the technology. The key element in the successful use of simulators is that they become integrated throughout the entire curriculum so that deliberate practise to acquire expertise over time is possible. Simulation allows learners to receive professional feedback with opportunities for repetition and feedback.
The use of simulation must not become a barrier for training; simulation may be undertaken in low tech / fidelity settings and is not simply reliant on high tech equipment. This should be encouraged as essential in training and provision made locally, however, there may be situations where trainee and trainer can decide that the trainee can undertake a task without specific simulation.
How may this be implemented?
Training programme directors and college tutors should be canvassed to make sure that the opportunities in simulation are created and trainees are aware of their options. The trainee should start by revising the anatomy and familiarising themselves with the required instrumentation. Simulation should be approached in a modular form where possible, and follow initial training on the correct techniques from observation of live surgery. It is also helpful for senior input and review of technique during the practise period, particularly in cataract surgery, and senior trainees can be encouraged to supervise more junior trainees as this enhances their own learning experience too. Documentation of this assessment should be uploaded to the trainee’s portfolio. What role simulation will play in the evolution of surgical training is uncertain. Each individual has a preferred learning style which influences the way they engage in simulated teaching environments. Are simulators ‘Education or Training’? The two terms are often used interchangeably, however, they are not the same. Education usually refers to the communication or acquisition of knowledge or information, while training refers to the acquisition of skills (cognitive or psychomotor).
Fundamentally, the trainer is key to how the trainee progresses and influences where they are on their learning curve, not just psychomotor learning but cognitive. Simulators are the future for surgical training programs. Their power can only truly be realised if they are integrated into a well-constructed curriculum.
References
1. Clark, M, Eichelberger J. Edwin A. Link 1904-1981. Binghamton University Libraries. Retrieved 06.06.2012.
2. Cook DA, Hatala R, Brydges R, et al. Technology-enhanced simulation for health professions education: a systematic review and meta-analysis. JAMA 2011;306(9):978.
3. Jonassen DH, Peck KL, Wilson BG: Learning with Technology: A Constructivist Perspective. UpperSaddle River, NJ: Pearson/Merrill/Prentice Hall; 1999.
4. Rogers GM, Oetting TA, Lee AG, et al. Impact of a structured surgical curriculum on ophthalmic resident cataract surgery complication rates. J Cataract Refract Surg 2009;35(11):1956-60.
5. Biggs J, Tang, C. Teaching for Quality Learning At University. Open University Press; 2011.
6. Belyea DA, Brown SE, Rajjoub LZ. Influence of surgery simulator training on ophthalmology resident phacoemulsification performance. J Cat Refract Surg 2011;37(10):1756-61.
7. Saleh GM, Lamparter J, Sullivan PM, et al. The international forum of ophthalmic simulation: developing a virtual reality training curriculum for ophthalmology. Br J Ophthalmol 2013;97:789-92.
COMMENTS ARE WELCOME