History
A 45-year-old female patient presented with left upper eyelid swelling present for six months. There was mild pain and a sense of fullness over the left eye. Examination revealed a palpable firm mass over the lacrimal gland area without proptosis or associated visual impairment. An excisional lacrimal gland biopsy was performed and the specimen sent for ophthalmic histopathological assessment.
Questions
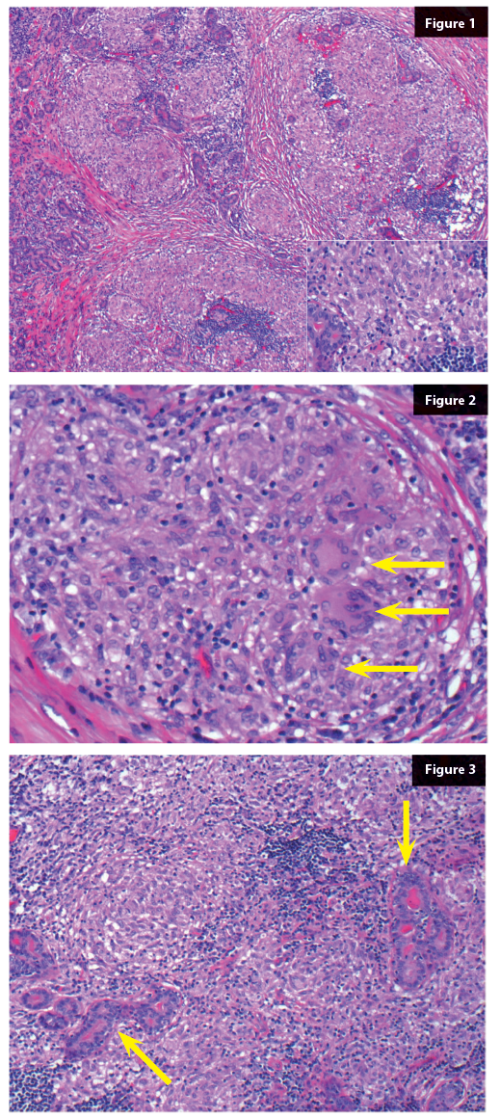
1. What are the key features on the H&E (Figure 1)?
2. What do the arrows show (Figure 2)?
3. What are the arrows pointing at (Figure 3)?
4. What is the most likely diagnosis?
5. What is the clinico-pathological differential diagnosis?
6. Which further investigations should be carried out?
Answers
1. Non-caseating epithelioid granulomas and patchy lymphocytic infiltrate.
2. Multinucleate giant cells.
3. Remainder lacrimal gland acini.
4. Sarcoidosis.
5. Other conditions with epithelioid granulomas such as tuberculosis / atypical mycobacteriosis and fungal infection.
6. Special stains for micro-organisms (Ziehl-Nielsen for AAFB and PAS / grocott for fungi). Clinical correlation is required including laboratory tests (ACE, ANCA and other inflammatory markers), radiological assessment of the chest and tuberculosis skin test.
COMMENTS ARE WELCOME