History
-
A 57-year-old lady presents with a right subconjunctival lesion which has been increasing in size for three months (Figure 1).
-
She has never had vision problems other than presbyopia.
-
Past medical history: hypertension and asthma.
-
On examination, she had a subconjunctival salmon patch 9-11 o’clock. Left eye was unremarkable.
-
Given concerning differential diagnoses, a conjunctival biopsy was performed and sent for ophthalmic histopathological assessment.
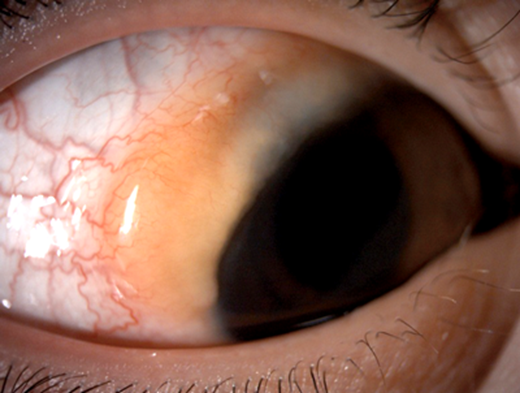
Figure 1.
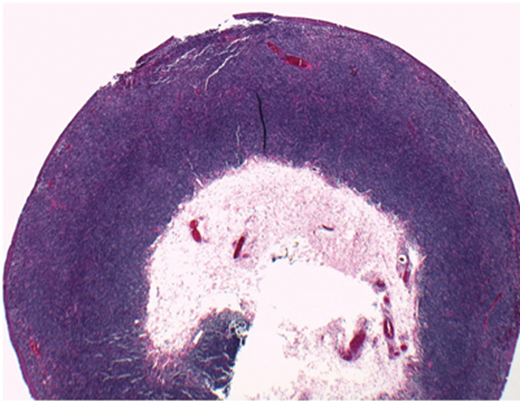
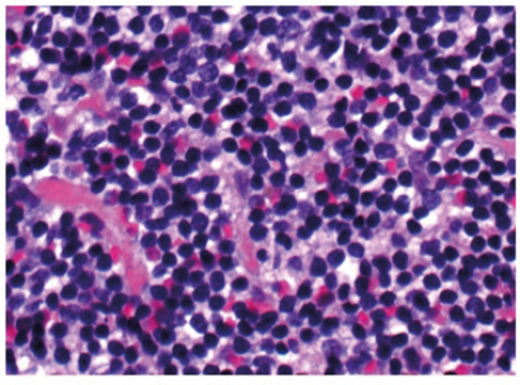 Figure 2 (top and above).
Figure 2 (top and above).
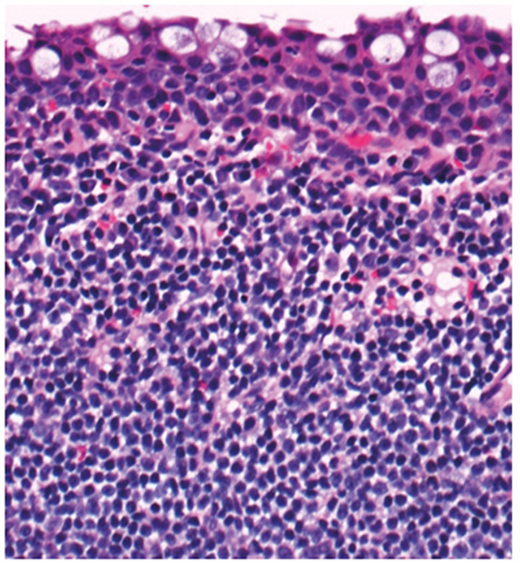
Figure 3 (top and above).
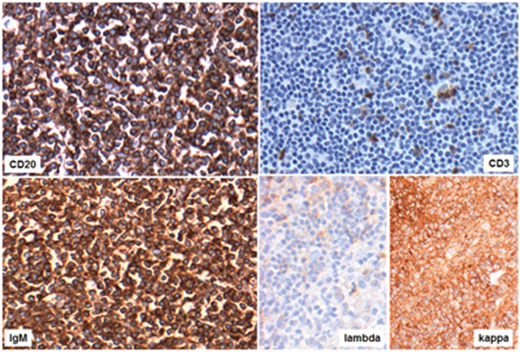
Figure 4.
Questions
-
Figure 2 contains representative histological sections of the biopsy taken. What does it show?
-
Considering clinical information and features on Figures 1 and 2 what is the differential diagnosis?
-
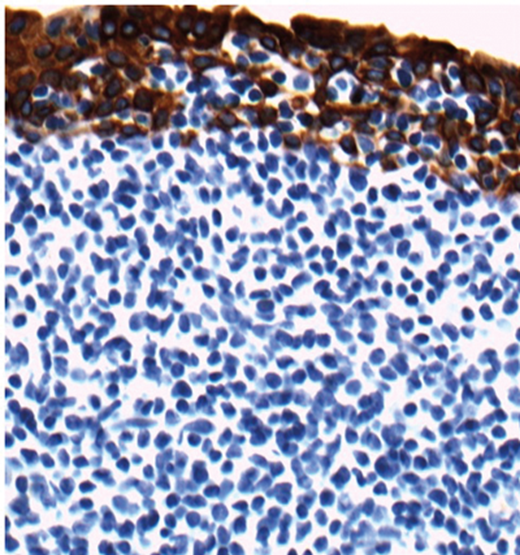
Figure 3 shows H&E stained section and immunohistochemistry with epithelial marker AE1/AE3. Both sections include conjunctival surface. How can this figure be described?
-
Figure 4 shows a number of positive and negative markers. How these can be interpreted?
-
Considering features in Figures 2-4 what is the likely diagnosis?
-
Are there any further diagnostic / staging steps?
Answers
1. Diffuse lymphoid proliferation consisting predominantly of small cells.
2. Lymphoma and reactive lymphoid proliferation. Immunohistochemistry is required to help establish the diagnosis.
3. Both images show conjunctival epithelial surface and underlying monotonous infiltrate. Immunohistochemistry for AE1/AE3 highlights the conjunctival epithelium in brown while the lymphoid infiltrate is negative (blue). Note lymphoid cells infiltrating into the epithelium represented by negative patches.
4. The top images show predominance expression of B-cell marker (CD20) over T-cell marker (CD3) by lymphoid cells. Lymphoid cells also express IgM. Finally, kappa light chain restriction is confirmed by positive kappa and negative lambda.
5. Non-Hodgkin B-cell lymphoma, likely extranodal marginal zone lymphoma.
6. Immunoglobulin gene rearrangement studies are required to confirm monoclonal B cell expansion. Full haematological assessment is essential for staging.
COMMENTS ARE WELCOME