A 58-year-old Caucasian male presented to the emergency eye clinic with a two-day history of a painful, red left eye and blurred vision. His past ocular history included uncomplicated left phacoemulsification cataract surgery in 2010 and left retinal detachment repair (vitrectomy and gas tamponade) due to superonasal retinal detachment two days post cataract surgery. Recently, the right eye is phakic and had suffered a vitreous haemorrhage with retinal tears requiring cryoretinopexy in April 2020. There was no past history of uveitis.
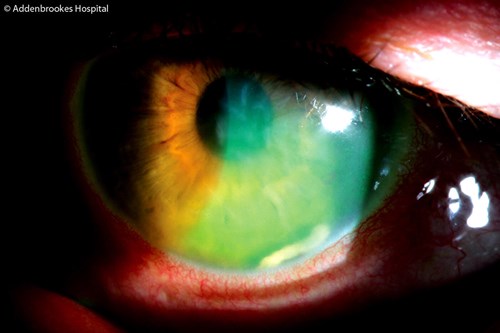
Figure 1: Focal corneal oedema and acute uveitis with a clump of retained lens matter.
Slit-lamp examination showed left focal corneal oedema with an adjacent clump of greyish white lens material in the inferonasal anterior chamber (Figure 1). Vision in the affected left eye had reduced to 6/24 Snellens acuity. There was no wound leak, grade 2 flare with intraocular pressure of 10mmHg in the affected eye. Both retinae were flat and there was no new evidence of retinal tears.
A diagnosis of left acute anterior uveitis due to the migration of retained lens matter was made with a decision to proceed with left anterior chamber (AC) washout that same evening. The soft lens fragment was removed with Simcoe cortex extractor and completed with corneal sutures. Postoperative topical medications included dexamethsone 0.1% eye drops two-hourly tapering course and chloramphenicol for the left eye that resulted in complete resolution of uveitis and full visual recovery to 6/9 Snellens in four weeks.
Discussion
This case highlights some key learning points. Firstly, the importance of a clear, accurate history and thorough, systematic examination. This patient’s past ocular history helped the ophthalmologist to consider causes for the acute anterior segment inflammation several years following cataract surgery. These included recurrent uveitis, endogenous endophthalmitis, intraocular infections and retained lens matter [1].
A retained lens fragment in the anterior segment after phacoemulsification is not uncommon in the early postoperative period [2] but the late migration of such retained material is an uncommon event, particularly when associated with acute onset of iritis, corneal oedema and vision loss. It is thought that this can be due to direct mechanical contact and corneal endothelial cell toxicity [3] with possible role of lens epithelial cells playing a role in intraocular inflammation [4].
The reasons for late migration of retained lens matter into the anterior chamber are speculative and possibly resulting from capsule deformation or minor trauma such as eyelid rubbing or indeed retinal indentation during vitreoretinal assessment, as could be the case for this patient.
The patient had bilateral 360 degree scleral indentation by a vitreoretinal surgeon to both eyes prior to cryoretinopexy two months prior to presentation with acute vision loss in the left eye. It may be reasonable to postulate that performing scleral indentation may have dislodged the retained soft lens matter and caused it to migrate anteriorly. Interestingly, the lens matter whilst in the capsular bag does not normally induce such a reaction but migration to the anterior chamber seems to initiate an acute response, even as late as 10 years following cataract surgery.
Ophthalmologists must be cognisant of this late complication with recommendation for an early AC washout as an effective treatment strategy. It also highlights the importance of removing all soft lens matter from the capsular bag at the time of cataract surgery.
References
1. Hui JI, Fishler J, Karp CL, et al. Retained nuclear fragments in the anterior chamber after phacoemulsification with an intact posterior capsule. Ophthalmol 2006;113:1949-53.
2. Bagga A, Soukiasian SH, Cotran PR, Speert PK. Delayed appearance and consequences of retained nuclear fragments after uneventful phacoemulsification. Invest Ophthalmol Vis Sci 2004;45:290.
3. Bohigian GM, Wexler SA. Complications of retained nuclear fragments in the anterior chamber after phacoemulsification with posterior chamber lens implant. Am J Ophthalmol 1997;123:546-7.
4. Majima K. Lens epithelial cells in postoperative aqueous humor. Jpn J Ophthalmol 1997;41(1):55-8.
COMMENTS ARE WELCOME





