The role of the optometrist has expanded in recent years as community eye care services have changed. With the limited scope of general ophthalmic services (GOS) regulations in most parts of the UK, the funding to support additional care has been negotiated on a local basis, and schemes to support GPs and to reduce urgent ophthalmic referrals to Accident and Emergency departments (AEDs) have been developed. Concerns over challenges with access to care have been one of the drivers for commissioners; as medical services become stretched, solutions need to be found.
Challenges in primary care
Red sticky eyes have traditionally been safely managed by self-medicating, or by seeing a GP for a prescription. Difficulties arise when the patient presents with a condition that is seemingly more complex, where the vision is blurred, when there is pain, or indeed when prescribed medication or OTC treatments have been unsuccessful. A lack of a slit-lamp to conduct a detailed examination and limited ophthalmology training makes a differential diagnosis difficult. For many GPs this results in a referral to the local ophthalmology AED.
General practice services in the UK are very stretched [1]. Despite an increase in GP numbers over recent years, patients are still finding it difficult to access GP services; shifting care into the community and a more complex mix of conditions has added to this situation. Two percent of GP consultations relate to eye conditions [2] and GPs have welcomed schemes that allow them to refer patients to optometrists for urgent, same day appointments rather than only having the opportunity to refer to the hospital eye service [3]. Such schemes also encourage patients to attend their optometrist as the “first port of call”, avoiding general practice entirely.
“UK community optometrists would seem ideally placed to support and manage patients with non-sight threatening eye conditions.”
Changes in community optometry
UK community optometrists would seem ideally placed to support and manage patients with non-sight threatening eye conditions. The optometric consulting room is equipped with the assessment and examination equipment required, including a slit-lamp and diagnostic drugs. Already responsible for case-finding ocular disease as part of the GOS eye test [4], their role and training extend to the use of therapeutic agents; the law supports the supply by an optometrist from a defined formulary with a written order to the pharmacy for drug supply to treat minor eye conditions.
In 1999 there were changes made by the General Optical Council to rules under the Opticians Act 1989 [4] that relate to injury and disease of the eye [5]. The optometrist was able to use his own discretion when deciding how to manage a patient with a disease or an abnormality of the eye. Previously there was an obligation to refer any such patient to a medical practitioner. This change opened the possibility that patients could be monitored and / or treated within community practices.
What has been lacking is the funding to support any additional service from the NHS. Optometrists are able to provide private services and many have, but with the treatment of red eyes falling within what the general population consider to be an NHS service, charging many patients is difficult. Negotiating local payments for services through local optical committees has more recently allowed areas to contract to provide services beyond the constraints of the GOS eye test. The national body, local optical committee support unit (LOCSU), has provided support to allow this to be developed with pro-forma contracts, but fees for similar services vary depending on where in the country you are providing that service.
Most local schemes are accredited to some extent, and optometrists are required to undertake what amounts to a ‘revalidation’ of GOC core competencies [6] to provide care. Audit and on-going monitoring is often in place to ensure that the quality of the service is maintained.
National evaluation of enhanced projects
The College of Optometrists launched the Enhanced Eyecare Evaluation Project in 2012 with the aim of evaluating the changes to community optometry in England [7]. With a multidisciplinary project team, the evaluation is looking at all aspects of care from the point of view of the patient, optometrist, GP, ophthalmologist and also commissioners. The Minor Eye Conditions Scheme in Lambeth and Lewisham has been reviewed as part of this project [8]. Using the neighbouring London borough of Southwark as a control, the service has been shown to be clinically effective and has extremely high patient satisfaction scores. The evaluation concluded that the service was an effective replacement to the local AED, and referrals into the hospital were reduced.
Differences across the nations
Other areas of the UK are using different models. The Southern Health and Social Care Trust in Northern Ireland has extended its acute community eye care scheme following a successful pilot in Armagh and Dungannon [9]. The project study showed that there was safe and appropriate management of minor non-sight threatening eye conditions. The ‘first port of call’ service with an accredited community optometrist, was shown to support local GPs and has allowed patients to be seen closer to home. Emergency hospital services were utilised for the most serious eye conditions. The scheme identified that “in most cases, the outcome is advice, reassurance and minor treatment”.
Wales and Scotland have developed national schemes. Eye Health Examinations Wales supports patients who attend their optometrist with an urgent eye condition [10]. The emergency service is provided by accredited optometrists, who are required to re-accredit every three years. The service is very carefully audited and evaluated to ensure high quality and a consistency of care. The service is provided by over 90% optometrists in Wales.
The Scottish model is very different and rather than being provided as an ‘add-on’ to the GOS regulations, first port of call is part of the whole package of care [11]. Funding has been provided to increase fees, develop practices, support on-going continuous professional development (CPD) and develop guidance. Access to medication has been developed on a regional and local basis with support from pharmacists through the minor ailments scheme, patient group directions (PGDs) or arrangements for signed orders. Some areas of Scotland have gone further, and extended the service to provide more advanced care within the community, e.g. NHS Grampian and NHS Lanarkshire.
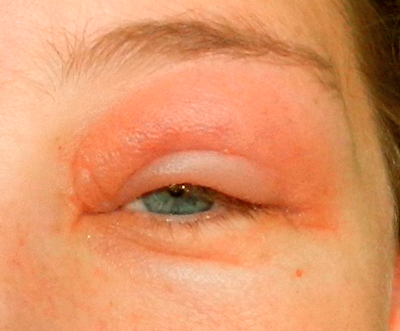
Figure 1: Insect bite on lid – a typical presentation that is concerning to
a patient but that can easily be managed by community optometry.
Issues arising with shifting the care
One of the criticisms of providing local schemes is that they generate demand; patients who would previously have attended their pharmacist and self-medicated, may now be accessing a local optometrist for advice and / or treatment. This may be the case, but it is clear that demand is already high and rising across healthcare as a whole. An issue often cited is that patient concerns are generated from an internet search of symptoms. Previously a visit to the pharmacist would have sorted out a red eye with an over the counter preparation in complete ignorance of any potentially sight-threatening conditions. In the vast majority of cases of course, ignorance is bliss!
Consistent evidence points to the traditional AED full of patients who do not require such a service [12]. That it provides invaluable training for ophthalmic nurses and medical trainees is invariably true, but should that training dictate the service provision, or should the needs of the patient dictate the service? Surely essential training could be developed to support a patient centred service model.
First port of call
It is important that an easily accessible, safe, cost-effective and high quality service is available to patients who are having problems with their eyes. General practices are struggling to manage their patient load and are not best equipped to manage more complex ophthalmic presentations. Evidence suggests that community optometry could support patients as a first port of call for eye problems, removing the gatekeeper role from the GP. This also has the advantage of an extended service being made available within the community, further reducing the burden on the secondary sector. Whether this is cost-effective for the NHS and for the optometry contractor needs careful consideration and detailed evaluation; more work clearly needs to be undertaken.
References
1. The King’s Fund. Understanding pressures in general practice (2016)
https://www.kingsfund.org.uk/
publications/pressures-in-general-practice
2. Sheldrick JH, Wilson AD, Vernon SA, Sheldrick CM. Management of ophthalmic disease in general practice. Br J Gen Pract 1993;43(376):459-62.
3. Royal College of Ophthalmologists and the College of Optometrists (2014) Urgent Eyecare
https://www.rcophth.ac.uk/wp-content/
uploads/2014/12/urgent-eye-care
-template-25-11-13-2013-_PROF_264.pdf
4. The Opticians Act (1989)
http://www.legislation.gov.uk/
ukpga/1989/44/contents
5. General Optical Council, Rules relating to injury or disease of the eye (1999)
https://www.optical.org/en/
about_us/legislation/rules
_and_regulations.cfm
6. General Optical Council. Core Competencies (2016)
https://www.optical.org/en/
Education/core-competencies
--core-curricula/index.cfm
7. College of Optometrists. Enhanced Scheme Evaluation Project (2017)
https://www.college-optometrists.org/
the-college/research/research-projects/
enhanced-scheme-evaluation-project2.html
8. Konstantakopoulou E, Edgar DF, Harper RA, et al. Evaluation of a minor eye conditions scheme delivered by community optometrists. BMJ Open 2016;6:e011832.
9. Health and Social Care Board, Northern Ireland. Southern Primary Eyecare Assessment and Referral Service Pilot “Spears”: Pilot Evaluation Report (2016)
http://www.hscbusiness.hscni.net/
pdf/SPEARS_Evaluation_Report_March_2016.pdf
10. NHS Wales. Wales Eyecare Services (2018)
http://www.eyecare.wales.nhs.uk/home
11. The Scottish Government. Community Eyecare Services Review (2017)
http://www.gov.scot/
Publications/2017/04/7983
12. The Royal College of Ophthalmologists. The Way Forward: Emergency Eye Care
https://www.rcophth.ac.uk/wp-content/
uploads/2015/10/RCOphth-The
-Way-Forward-Emergency-Eye-Care-300117.pdf
(All links last accessed April 2018).
COMMENTS ARE WELCOME