
Importance of work experience
Medical schools expect applicants to understand what a career in medicine involves, which can be gained through work experience and volunteering. It is strongly recommended by the Medical Schools Council that work experience involves working in a people-focused environment in a caring role, or direct observation of a healthcare environment.

Opportunities to gain work experience in NHS settings, particularly in a hospital, are very competitive and challenging to secure. They require persistence and determination in order to succeed in getting a placement. From the hospital’s perspective, placements require lots of pre-checks and pathways drawn up in advance so that students have the required permission and authority to observe. From the student’s perspective, work experience is invaluable and an inexpensive way of knowing for sure whether a certain career path is the right one.
How to arrange work experience
As an A-level student aspiring to study medicine at university, I sent emails to various doctors working in NHS hospitals in my area, addressing my desire to gain work experience. I also contacted local hospices and care homes to request a volunteering role with them.
As COVID restrictions came into place, students were restricted from gaining work experience in NHS hospitals in a bid to minimise footfall. In response to this, I thought I would try to gain the vital experience I needed in the independent health sector. I was apprehensive initially as my peers had not heard of this route so I made initial contact with Newmedica.
I was fortunate enough to get a positive response from their human resources team, who had a specific pathway created for students and trainees looking to gain work experience, and after the initial contact, I was offered a one-week placement at Teesside Newmedica Eye Health Clinic and Surgical Centre.
Other Resources
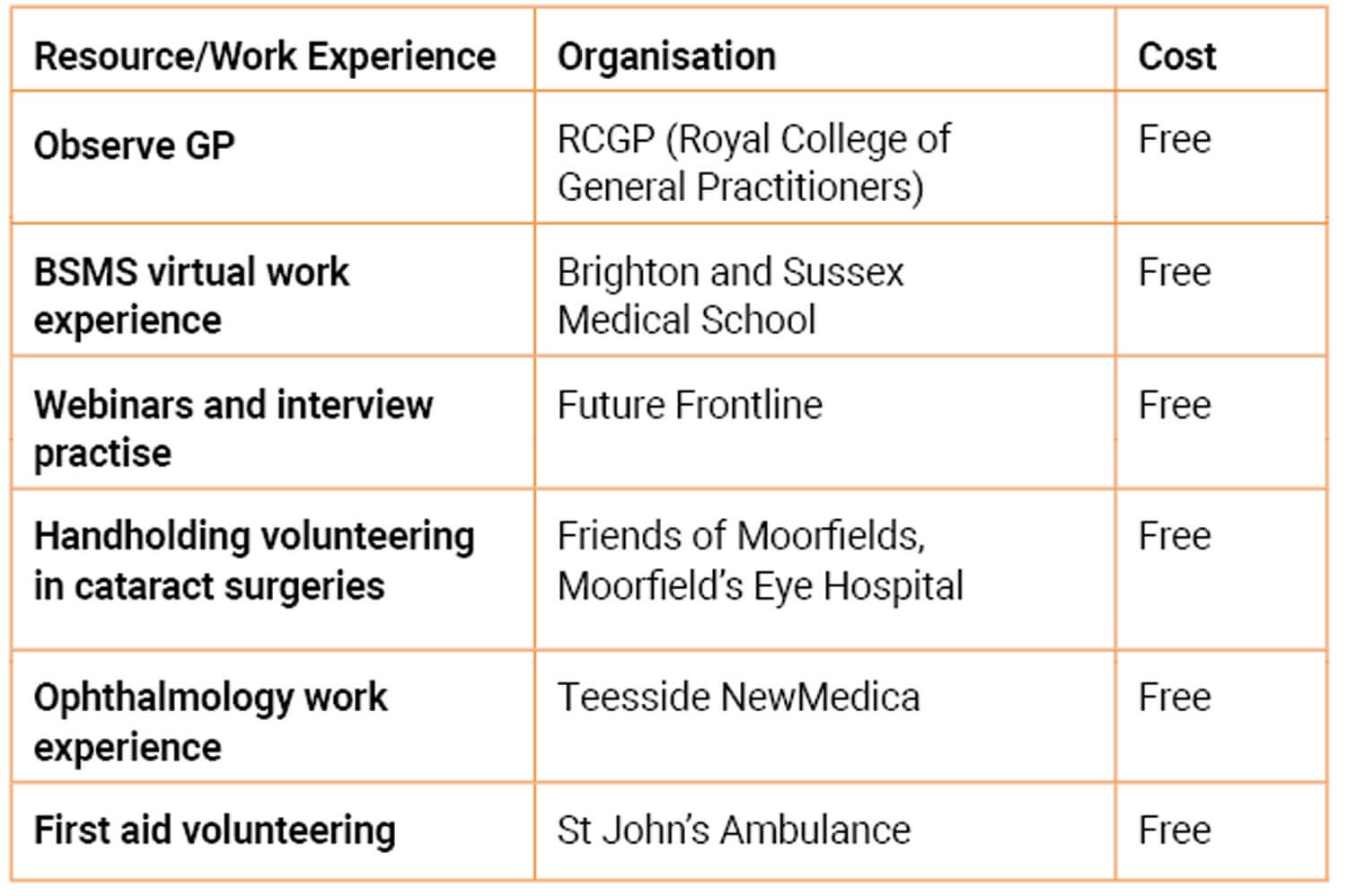
Table 1: A list of opportunities for virtual and in-person work experiences and volunteering.
Reflections on my work experience
During my time at Newmedica, I observed patient journeys from the minute they entered the door, following as they travelled along the integrated patient pathways. The seamless manner in which this pathway prepared patients for their cataract surgeries was only possible through the commendable teamwork of the healthcare staff. The ophthalmic technician saw the patient first to do a biometry (lens power measurements) and take OCT (optical coherence tomography) scans. Following this, the nurse would check the patient’s medications and explain the procedure, as well as check for mental competence and capacity to consent.
Lastly, the patient is seen by a consultant ophthalmologist who examines their eyes using a slit-lamp, analyses their scans and explains the surgical procedure in detail. The consultant also discusses the risks and benefits of the procedure and takes informed consent from the patient for surgery. I was keen to know more about the consent process, so I read some resources online written by the General Medical Council on decision making and consent.
This experience reinforced the importance of empathy and collaborative working with all healthcare staff. The process of assessing capacity and gaining voluntary consent was done by asking patients open-ended questions and providing information in a clear and honest manner. This highlighted to me how clinicians and healthcare staff were geared towards patient safety, ensuring the patients’ right to beneficence without compromising their autonomy. I was able to witness the pillars of medical ethics in practise and their application in different patient scenarios, which helped me in preparing for ethics and scenario-based questions for my university application to medicine.
In the ophthalmic theatre environment, I observed high volume cataract surgeries and shadowed patients throughout their integrated cataract pathway. Despite the repetitive nature of their tasks, each member of the team would ensure that they do their very best to reduce the risk of any human error.
Speaking to one of the consultants, Mr Qasim Mansoor at Newmedica, I learned about human factors in the theatre environment and their importance in determining patient safety. These included effective teamwork and communication, which proved to be essential towards delivering exceptional care – for example, the runner performing the simple task of writing the patient’s name, which eye, lens type and whether the patient has any allergies onto a whiteboard in the theatre. This made information easily visible at a glance for the surgeon to reconfirm. While these small tasks may seem minor at first, once transformed into standardised procedures through repetition, they collectively form the fundamental foundation for patient safety.
TAKE HOME MESSAGES
-
Ensure you adhere to the ethics of Good Medical Practice.
-
Apply your understanding of Human Factors in Medicine.
-
Prioritise patient safety.
-
Work collaboratively to provide patient-centred care.
Further reading
1. The Royal College of General Practitioners. Observe GP.
https://www.rcgp.org.uk/your-career/
work-experience/observe-gp\
2. Brighton and Sussex Medical School. BSMS Virtual Work Experience.
https://bsmsoutreach.thinkific.com/
courses/VWE
3. Future Frontline.
https://futurefrontline.co.uk/
4. Friends of Moorfields. Volunteering.
https://friendsofmoorfields.org.uk/
what-we-do/volunteering/
COMMENTS ARE WELCOME







