In this report, both authors present their personal experiences of an observership at the Comprehensive Community Based Rehabilitation in Tanzania (CCBRT) Hospital, a large regional teaching hospital located in Dar es Salaam, with a particular focus on resource management, attitudes of patients and healthcare staff, and the clinical cases we encountered.
Background
In June 2023, we embarked on a transformative journey as we undertook a month-long surgical observership at CCBRT Hospital. Guided by the expertise of British Consultant Surgeon Rita Ohri, a seasoned trainer and long-standing visiting clinician at the destination, we delved into the realm of international ophthalmology.
This unique opportunity marked our inaugural step in translating our medical training to a global context. Our primary objective was to glean insights not only from clinical perspectives but also the intricate interplay between distinct cultures, demographics and environments. This exploration aimed to shed light on how these factors collectively shape and impact healthcare delivery challenges within a developing nation.

Theatre staff.
Tanzania is a lower- to middle-income country with a population of 62 million, located on the East African coast. Benefitting from a tropical climate and a dry period from June to September, it offers favorable conditions for travel. Swahili is the national language, but English is widely spoken and there is significant ethnic and linguistic diversity in the country. Tanzania has maintained relative political stability since gaining independence in 1961 and has not experienced large-scale armed conflict since the Uganda-Tanzania War in 1979.
In the most populous city, Dar es Salaam, the CCBRT hospital serves as one of the country’s major tertiary eye facilities. It consists of both private and public wings, collectively seeing up to 300 patients per day. The public wing receives funding from donors and charitable organisations, which in contrast to the many private ophthalmic facilities in the city, makes it the only affordable option for underprivileged Tanzanians.
Over the past decade, the ophthalmology department has witnessed significant growth and is currently under the leadership of senior ophthalmologists specialising in retina, glaucoma, paediatrics and oculoplastics. Furthermore, CCBRT has a well-established history of hosting UK-based consultants for extended periods of work and training within the centre. These include Danny Mitry (vitreo-retinal), Nick Koutroumanos (oculoplastics) and Rita Ohri.
"The team takes great efforts to see all patients arriving at their door, as the opportunity to provide sight-saving care may present itself only once"
Rita Ohri has been providing valuable support to this eye unit across various subspecialties through extended visits for the past 13 years, and many of the current clinical staff have been fortunate to receive training from her. Her impact was illustrated by Dr Sonia Vaitha, a local doctor who received the entirety of her subspecialty training under Miss Ohri’s guidance, and is anticipated to gain recognition in becoming a fully qualified paediatric ophthalmologist.
In addition to ophthalmologists, the team consists of six trainees at different stages in their career, along with specialised nurses, orthoptists, optometrists and the country’s sole ocular prosthetist, who meticulously crafts hundreds of high-quality prostheses each year.
Observership and living arrangements
Upon arrive, we were welcomed by Dr Nicholaus Chaula, the head of department, and received an induction which helped develop rapport with the staff and made for an easy assimilation. We felt very welcome there and were even invited to dinner with the head of human resources (HR). There were multiple clinics and theatre lists running simultaneously throughout the working day. We were entrusted with a flexible schedule whereby we could switch between clinics and theatre to see cases of special interest. We found ourselves very welcome to participate in clinical activities, including reviewing patients in clinic, discussing interesting cases, supervising juniors and observing, assisting and performing surgeries in theatre, following discussion with the relevant supervisor.
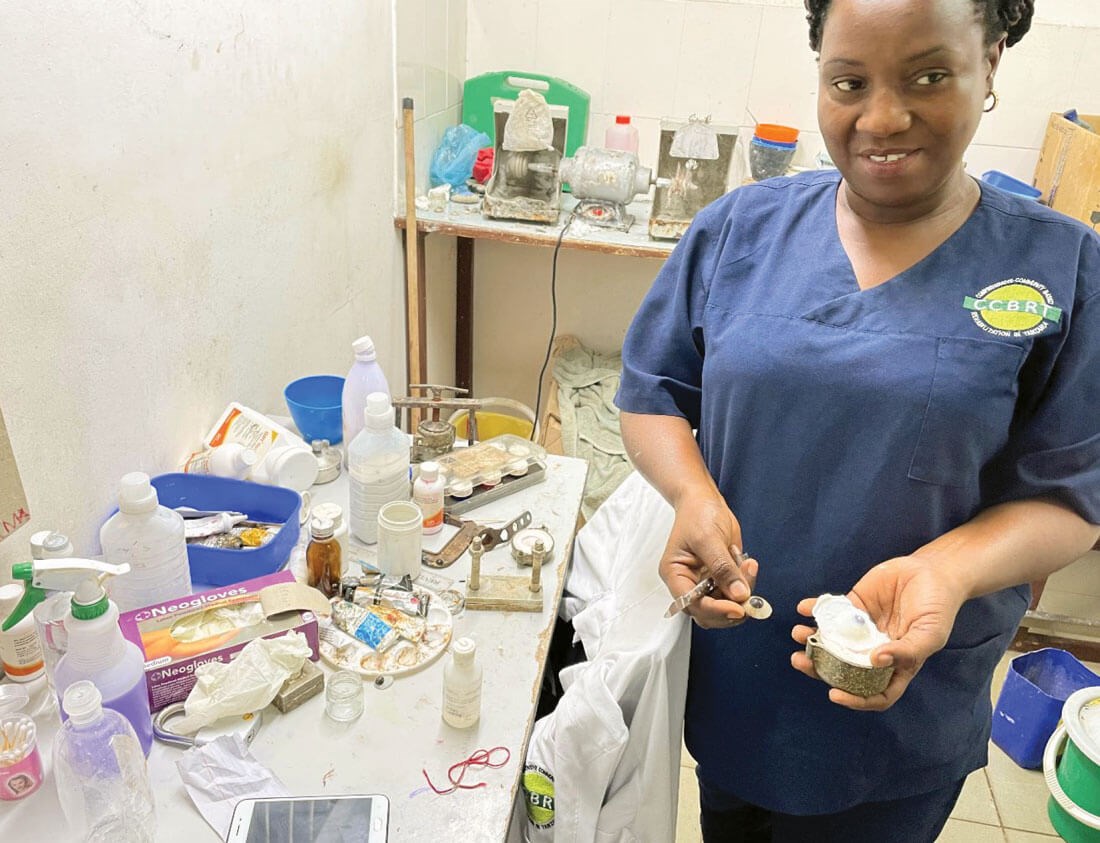
Rahima, Ocular Prosthesis Technician.
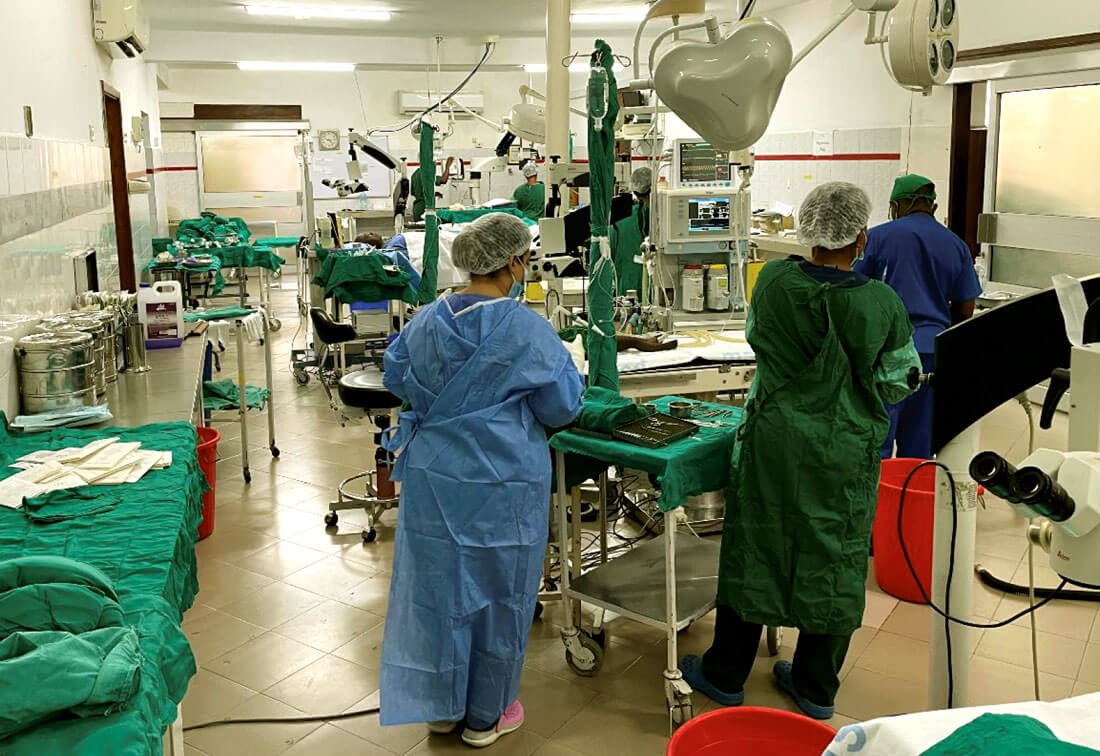
Main theatre.
Living in Dar es Salaam was a multifaceted experience. The city’s rich history, stark contrasts between wealth and poverty and its diverse amenities made it an engaging and eye-opening place to be. The cost of living is relatively low by European standards, with monthly accommodation expenditure for a mid-sized room close to the hospital (including cleaning and air conditioning) in the most exclusive district totalling $800. A typical meal at a restaurant may cost $10 in this area. While taking the standard safety measures in an unfamiliar city, we did not experience any untoward incidents or feel unsafe throughout our visit.
Clinics
Eye clinics in CCBRT can be extremely busy. There are no lists or appointment times as such; rather, all patients registering by 2pm are seen. The clinicians are accustomed to seeing up to 30 patients each per session. Tanzania is a large country and patients have often travelled considerable distances for eyecare. When travelling from distant regions, they often stay with friends or family in the region, or are required to stay in hotels locally, which can prove to be a significant financial burden. Subsequently, the team takes great efforts to see all patients arriving at their door, as the opportunity to provide sight-saving care may present itself only once.
From a trainee’s perspective, the high volume of cases with distinct signs provides excellent educational opportunities, and we were impressed by the clinical acumen and efficiency demonstrated by the junior registrars. Notable pathologies that contribute significantly to the clinical workload, in contrast to UK hospitals, include adnexal trauma, corneal perforation, lid cicatrisation and nasolacrimal obstruction. Additionally, we encountered a higher prevalence of immunosuppression-associated squamous cell carcinoma and nutritional optic neuropathies among adults, as well as congenital cataracts, paediatric glaucoma and refractive amblyopia in children. This is highlight by the fact that Dr Vaitha has performed an estimated 3000 paediatric cataract cases in the past eight years.
The day typically starts at 8am, but the patient flow is remarkably rapid, and usually all patients have been seen by 4pm. Initially, as visiting western clinicians, the pace can be overwhelming. However, we observed several differences in comparison to the NHS environment that facilitate this patient volume. Firstly, a significant proportion of patients here present with advanced pathology, which simplifies the diagnostic process. Consequently, history taking, examination and documentation are concise. Secondly, the limited resources and available competencies further restrict treatment options.
The affordability of treatment and diagnostic procedures significantly influences the treatment algorithm for patients. In this context, diagnostic modalities require individual fees, which can lead to fragmented service delivery. For instance, we encountered a case where a patient declined to pay for histology after the excision of a possible malignant lesion.
We expected the recurrent issue of finance and poor prognosis to make for a difficult environment to navigate for both patients and clinicians. However, the working culture is highly practical in the face of resource limitations. Staff and patients, including children, generally remain stoic and cooperative even in the face of daunting invasive examinations and treatments, or potentially debilitating visual outcomes. It is not unusual to see patients who have travelled and waited up to eight hours for their visit to be told that nothing can be done. However, there is little expression of frustration or dissatisfaction. It is not clear whether this is evidence of resilience or resignation. In our view, it is such ‘pragmatism’ that highlighted the biggest contrast to the UK-based practice and made us conscious of how pure clinical practice is complicated by protocolised management pathways, psychosocial impact and patient expectations, and other governance pressures. It is the focus on early detection and optimising visual outcomes, such as offering low vision services, which clearly presents the major challenge in reducing morbidity in this setting.
Theatre
The theatre setup in CCBRT is oriented towards efficiency while maintaining essential sterility standards. There are two large rooms adjacent to each other, the first containing five anaesthetic beds and the second being utilitised for ‘dirty’ procedures, including eviscerations, which are performed on a greater than weekly basis. Patients are brought in with their consent forms and identifying wristbands. A single anaesthetic practitioner is usually responsible for local anaesthesia, for which they exclusively use retrobulbar blocks. These are fast, require little in the way of equipment and are very effective (but not widely practiced in the UK due to the risk of globe perforation and retrobulbar haemorrhage). Another duo is responsible for general anaesthetic patients. The e sterilisation practices themselves are robust, but lack of equipment can give rise to practices such as using the same theatre gown throughout the list.
The surgical cases we encountered were often complex and challenging from a management point of view. Complication rates appear to be higher than what one might expect in the UK, partly due to the complex and extensive pathology. For example, posterior capsular ruptures can occur more than once on a list. Surgeons regularly need to think ‘outside the box’ and draw on their full clinical acumen to solve unique problems. One particular oculoplastic case involved an only-seeing eye with large lid defect (following tumour resection), for which the dilemma was to preserve sight whilst adequately closing the defect. The surgeon, Dr Attas, determined a Hughes flap was therefore not ideal, and instead a full thickness lid graft was utilised from the blind eye with a successful outcome.

Nigel Griffith, Rita Ohri and (right) Shafak Toufeeq on a hippo trail boat ride.
Setting aside these observations, the remarkable speed and efficiency of case procedures, coupled with a notable level of redundancy, are truly impressive. Consequently, there is a relaxed atmosphere on surgical lists, cancellations are uncommon and theatre staff remain flexible and cohesive. Though many of the practices here cannot be transferred to UK care, it still demonstrates the potential for efficiency gains in the context of delivering high-volume lists in the UK.
In terms of surgical technique, we cannot comment on specifics except that the large quantity of cases surgeons handle here must play a critical role in developing the confidence they show. Most have competencies across multiple disciplines. For example, a ‘routine’ list for Sonia Vaitha involved three bilateral paediatric cataracts, a paediatric trabeculectomy and several strabismus cases. It’s clear that surgical multiskilling acts as a force multiplier when it comes to optimising surgical services available to patients, particularly for urgent cases. Junior ophthalmologists are also encouraged to operate (and even supervise) early in their career.
Postoperative management also seems well organised, but attendance for the follow-up appointments remains an issue due to poor patient compliance. For example, we encountered cases such as a patient with endophthalmitis who did not present until weeks after diagnosis, and a post-dacrocystorhinostomy (DCR) child with nasolacrimal stents still in-situ, two years after surgery.
Final thoughts
Our experience in Tanzania, accompanied by the guidance of an experienced ophthalmologist, has provided us with valuable insights into ophthalmic practice in a developing country. We express our sincere gratitude to CCBRT Hospital for extending this opportunity to us and for the exceptional accommodations made by their dedicated staff despite their busy schedules, and for providing permission to publish photos in this article.
Throughout our observership, we have witnessed the commitment of CCBRT Hospital’s management to establish international links in the realms of clinical practice and research. The mutual educational benefits are evident, and they warmly welcome visits from ophthalmologists interested in clinical or research collaborations, or contributions of medical equipment. If you wish to learn more or get in touch, we would be delighted to provide further information or share contact details via email.
We would also like to extend our heartfelt thanks to Rita Ohri for her invaluable support in organising this endeavour and ensuring that we maximised our learning opportunities.
We highly recommend trainees and consultants alike consider pursuing opportunities of this kind, both to learn and contribute in equal measure, as well as enjoy the sights and sounds of a large coastal city. By sharing our experiences and insights gained from our time at CCBRT, we hope to participate in the global dialogue of providing eyecare in resource-limited settings and foster collaborative efforts in improving eye health worldwide.
TAKE HOME MESSAGES
-
Working in unfamiliar settings bolsters your learning experience by forcing you to re-examine your fundamental approaches to clinic assessment.
-
Networking opens doors to high value opportunities you may not have given prior consideration or thought possible.
-
When confronted by difficult clinical scenarios, accustom yourself to seeking creative solutions rather than persisting with ineffective strategies.
-
Working abroad builds resiliency and helps you develop new skills to manage a busy work-life at home.
-
Building a wide portfolio of clinical and surgical skills acts as a force multiplier when it comes to optimising ophthalmic services available to patients, which consequently will also enhance your employability.
-
A warm and welcoming atmosphere positively impacted our observership experience and we encourage reciprocity to colleagues visiting from abroad.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME