Expanding intraocular lens (IOL) capabilities provide broadening options, ranging from next-generation monofocal IOLs for basic cataract surgery, to specialised premium IOLs for lens-based presbyopia correction and astigmatism correction at the time of cataract surgery. Rod McNeil considers several newer alternative IOL product innovations and evidence of high-quality visual performance after cataract surgery.
Monofocal IOLs
The Tecnis Eyhance IOL (Johnson & Johnson Vision), model ICB00, is a next-generation monofocal IOL that extends the depth of focus, improving vision for intermediate tasks while providing similar distance vision to that of a standard aspheric monofocal IOL (Figure 1) [1]. Data show a low incidence of halo, glare or starburst comparable to that reported with the Tecnis 1-piece IOL.
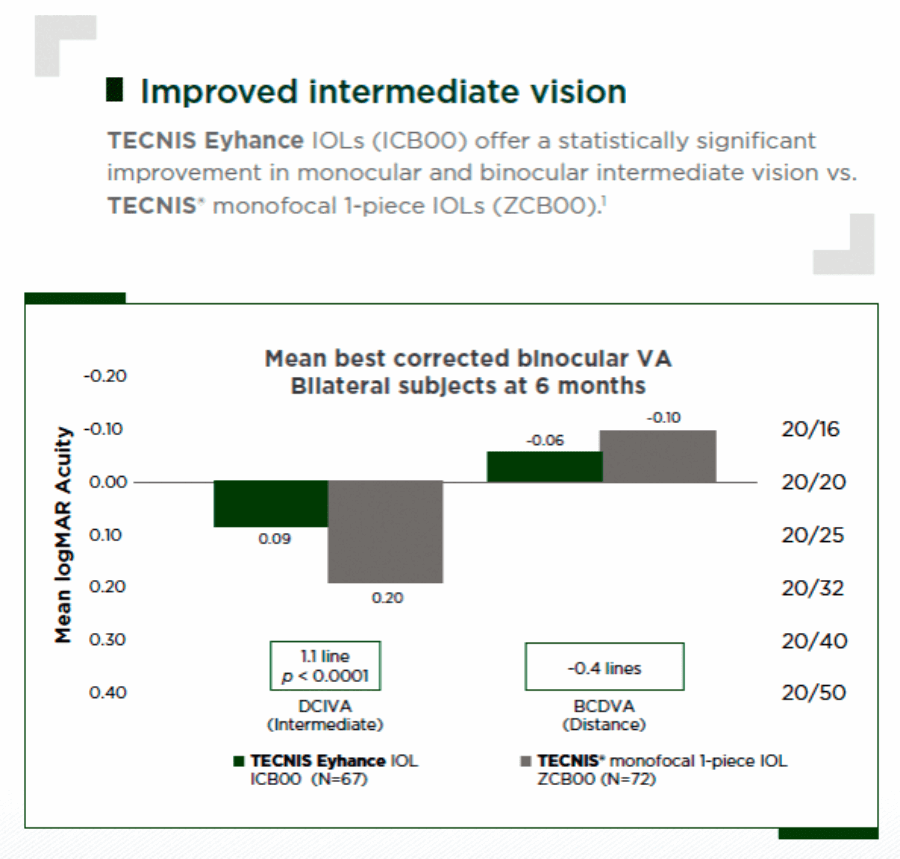
Figure 1: Tecnis Eyhance IOL (ICB00) vs. Tecnis monofocal 1-piece IOL (ZCB00):
intermediate and distance vision at six months post-surgery [1].
“Tecnis Eyhance IOL offers high quality intermediate as well as distance vision, representing an important advancement in the monofocal IOL category,” said Dr Oliver Findl, MD, MBA, Chief of Department of Ophthalmology, Hanusch Hospital Vienna and ESCRS Board Member and Secretary, speaking in an interview with the author.
“One of the major problems with monofocal IOLs is that we do not always hit the refractive target despite meticulous biometry and power calculation,” explained Dr Findl. “The Tecnis Eyhance IOL provides a two-fold surgical benefit with respect to refractive outcomes. Due to its geometry and optics, this IOL has a larger landing zone and is therefore more forgiving, providing the patient with very good uncorrected visual acuity even if the outcome is a little off from emmetropia. Secondly, if you do achieve emmetropia, then the patient will have good intermediate vision, an additional benefit not seen with most current monofocal lenses.
“Preliminary impressions of visual performance from my own case experience implanting the Tecnis Eyhance IOL is that uncorrected visual acuity is better than that typically associated with other monofocal IOLs and that patients experience good intermediate vision when emmetropia is achieved.”
ASPIRA-aXA (HumanOptics) is a monofocal IOL combining a 7.0mm optic with cut-out haptic design for added stabilisation for reliable refractive results. The enlarged XL optic allows for an extended view of the fundus, represents a promising approach to minimise dysphotopsia and is a particularly suitable treatment option for large pupils.
Multifocal IOLs can improve vision at all distances, with a high percentage of spectacle independence
Compared with standard monofocal IOLs, multifocal IOLs offer the benefit of improved vision at all distances and correct the symptoms of presbyopia after cataract surgery, increasing the likelihood of spectacle independence. Trifocal IOLs produce good visual acuity at all distances and consistently better intermediate vision than bifocal IOLs. Trade-offs with multifocality include night vision problems and an increase in glare, halos and / or starbursts in comparison with standard IOLs.
A recently published systematic review and meta-analysis by Khandelwal et al. concluded that multifocal IOLs compared to standard monofocal IOLs or monovision for cataract surgery and lens replacement result in better uncorrected near vision and a higher proportion of patients achieving spectacle independence, but greater risk of unwanted visual phenomena [2]. Better vision outcomes with less risk of halos was noted for newer diffractive multifocal lenses than older diffractive lenses and refractive lenses, when compared to monofocal IOLs.
A Cochrane systematic review concluded that multifocal IOLs are effective at improving near vision relative to monofocal IOLs, adding that there was uncertainty as to the size of the effect [3]. Distance acuity achieved with multifocal lenses was similar to that achieved with monofocal lenses. The authors observed that ‘motivation to achieve spectacle independence is likely to be the deciding factor’ in considering whether the improvement in near vision outweighs the adverse effects of multifocal IOLs.
Alcon’s latest diffractive AcrySof IQ PanOptix trifocal IOL has an intermediate focal point at 60cm, the distance for common intermediate vision activities, combined with a single piece design providing excellent rotational and axial stability.
A 12-month multicentre study demonstrated that patients (n=145) implanted with AcrySof IQ PanOptix trifocal IOL showed visual acuity of 20/25 or better in both corrected and uncorrected conditions across near, intermediate and distance visions [4]. A prospective, multicentre, randomised post-market clinical study evaluated the visual performance of AcrySof IQ PanOptix and the AT LISA tri 839MP presbyopia correcting IOL following bilateral implantations in 180 patients. Results showed that both IOLs improved visual acuity while the AcrySof IQ PanOptix group had better uncorrected near (40cm) and intermediate (60cm) vision at six months compared with the AT LISA tri IOL group (Figure 2 and Figure 3) [5].
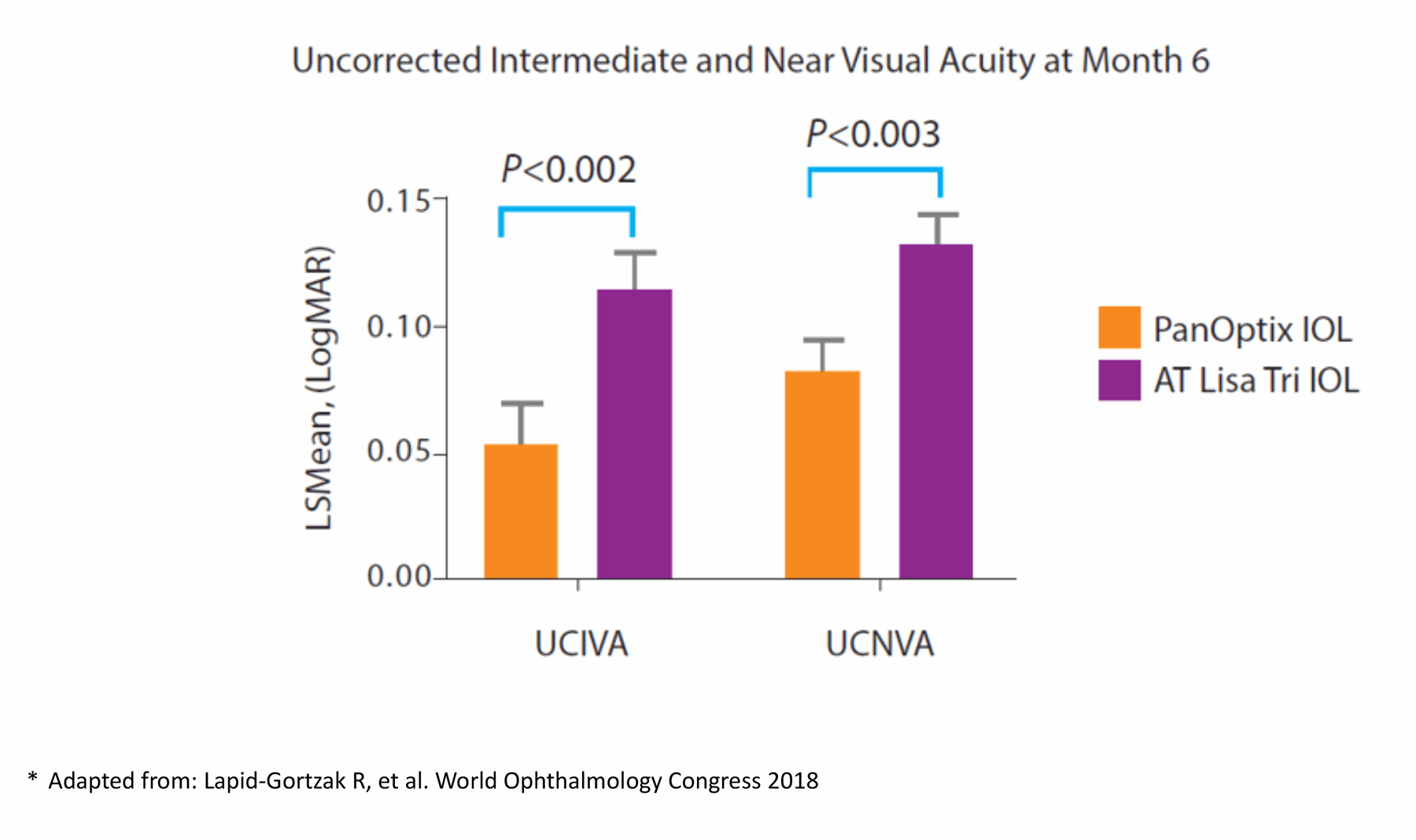
Figure 2: Comparison of two trifocal presbyopia correcting IOLs – six months’ postoperative results [5].
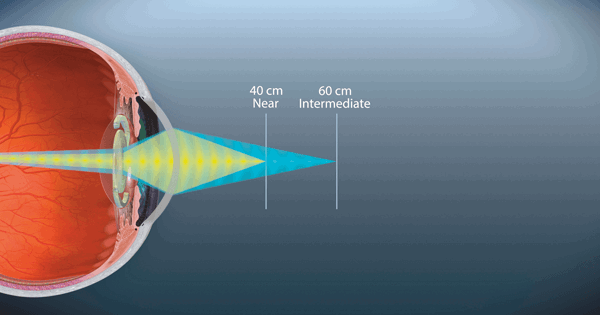
Figure 3: Illustrative outline showing AcrySof PanOptix Trifocal IOL.
Mencucci et al. undertook a comparative outcomes analysis with two models of trifocal diffractive IOLs (PanOptix IQ and AT LISA tri 839MP) and an extended depth of focus (EDOF) IOL (Tecnis Symfony) [6]. All IOLs tested provided good visual outcomes, reading performance and spectacle independence after cataract surgery, with no statistically significant difference between groups for uncorrected and corrected distance visual acuity. Better near visual acuity results were observed with the trifocal IOLs compared with the extended range of vision IOL, while the latter lens provided better contrast sensitivity outcomes than the trifocal models.
A six-month, single-centre, prospective comparative evaluation of AcrySof IQ PanOptix, FineVision Micro F and Tecnis Symfony IOLs in patients undergoing routine cataract surgery found, overall, that all three IOLs provided good visual acuity at all distances, high spectacle independence (90%), and little or no impact of visual symptoms on the patients’ daily functioning [7]. Monocular and binocular uncorrected near vision was significantly better for both trifocal IOLs compared with the EDOF IOL (P=0.002).
Extended depth of focus IOLs: description of several presbyopia-correcting lens technologies.
Product: Tecnis Symfony (Johnson and Johnson Vision)
Brief description of lens design and features: Biconvex, wavefront-designed anterior aspheric surface, posterior achromatic diffractive surface designed to reduce chromatic aberration for enhanced image contrast and echelette feature to extend the range of vision. UV-blocking hydrophobic acrylic. The lens mitigates the effects of presbyopia by providing an extended depth of focus. Compared to an aspheric monofocal IOL, the lens provides improved intermediate and near visual acuity while maintaining comparable distance visual acuity.
Product: AT LARA 829 (Zeiss)
Brief description of lens design and features: Diffractive, aberration-neutral aspheric optic design. Hydrophilic acrylate (25% water content) with hydrophobic surface properties. AT LARA EDOF IOLs are designed to provide a high degree of spectacle independence and to induce less visual side -effects compared to multifocal IOLs, enabling excellent vision over a wide range of distances. Because the lens induces fewer visual side-effects compared to multifocal IOLs, patients will enjoy greater visual comfort, especially at night.
Product: Precizon Aspheric Presbyopic IOL (Ophtec)
Brief description of lens design and features: Aberration neutral, acrylic IOL with a Continuous Transitional Focus (CTF) optic designed for the correction of presbyopia. Hybrid hydrophobic and hydrophilic monomers. The transitional zones of the CTF optic offer a full range of vision from near to infinity with a smooth continuous transition.
Product: Lentis Comfort (Oculentis)
Brief description of lens design and features: Foldable acrylic lens for optimised depth of focus and high contrast sensitivity with aspherical surface. HydroSmart, a copolymer, consisting of acrylates and hydrophobic surface, UV absorbing. Compared with monofocal IOLs, provides excellent visual acuity for intermediate and distance vision, improved contrast and depth of focus for optimal vision in low light conditions. Aberration neutral.
Product: IC-8 (AcuFocus)
Brief description of lens design and features: Biconvex, anterior aspheric surface optic design. Single-piece hydrophobic acrylic. Small aperture IOL implanted in the non-dominant eye.
Product: WIOL-CF (Medicem)
Brief description of lens design and features: Bioanalogic IOL, incorporating a design and material developed to resemble the properties of the natural crystalline lens. Designed to deliver premium visual acuity at all distances, with 9mm optics minimising dysphotopsias.
WIOL-CF is suitable for any patient with cataract or presbyopia who expects excellent far to intermediate visual acuity and keep or restore near vision for reading newspapers, books or electronic media and can eventually accept correction by spectacles for very fine near vision.
Product: Mini WELL Ready (Sifi MedTech)
Brief description of lens design and features: A progressive extended depth of focus aspheric IOL, with three optical concentric zones and a continuum of foci.
Additional opportunities for lens-based presbyopia correction with extended depth of focus IOLs
A range of EDOF IOLs utilising various approaches for correction of presbyopia are available, several detailed in Table 1. The underlying technology is based on utilising an optical design that provides for reduced near addition of the IOL while maintaining a continuous range of functional vision across intermediate and near distances [8].
Studies show that EDOF lenses may provide satisfactory near and intermediate vision with reduced incidence of optical phenomena often experienced by patients implanted with multifocal lenses [9].
A study involving 57 patients found that EDOF IOL Mini Well (SIFI) performed similarly to a distance-dominant diffractive multifocal IOL (ReSTOR SV25T, Alcon) at distance and near but was associated with better visual acuity at intermediate distances [10].
A retrospective cohort study comparing Tecnis Symfony EDOF IOL targeted at micro-monovision to a monofocal IOL targeted at binocular emmetropia (176 eyes of 88 participants) found that the EDOF IOL demonstrated superior range of visual acuity and spectacle independence compared with the monofocal IOL [11]. At postoperative review (5+ months), 93% of the EDOF IOL group reported spectacle independence at near distance compared with 33% of the monofocal group. Extended depth of focus IOL ZEISS AT LARA is based on a diffractive optical platform (Figure 4).
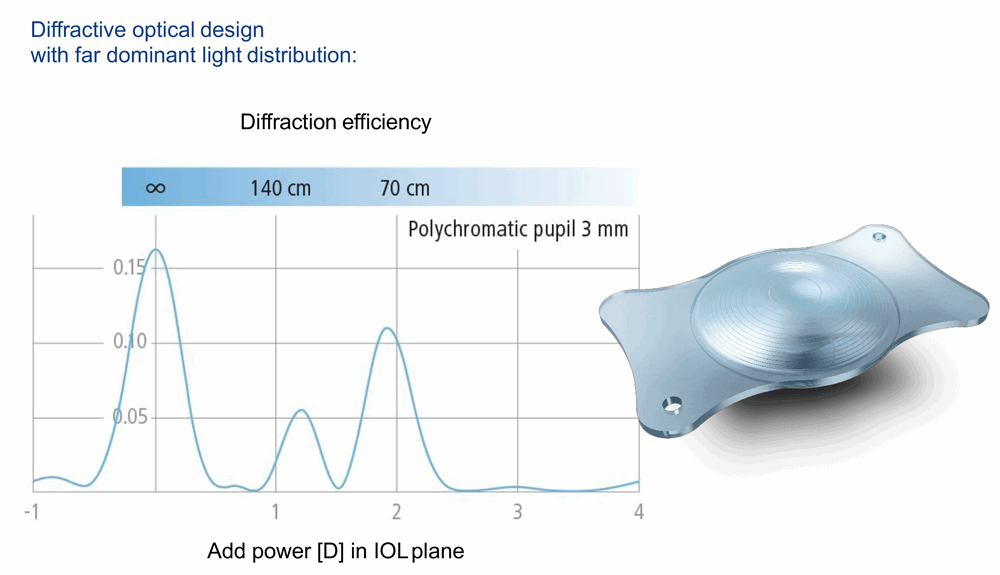
Figure 4: ZEISS AT LARA: Light Bridge Optical Design to create a continuous range of focus.
The lens provides a wider range of focus than previous generation EDOF IOLs, a high level of spectacle independence for intermediate and far distances and minimal incidence of photic phenomena [8]. An aberration-neutral aspheric design and advanced chromatic correction provide optimised contrast sensitivity. A prospective pilot study showed good postoperative refractive predictability after bilateral implantation of AT LARA 829; defocus curve analysis demonstrated stable visual acuity from +0.5 to -1.5 D (Figure 5) [12].
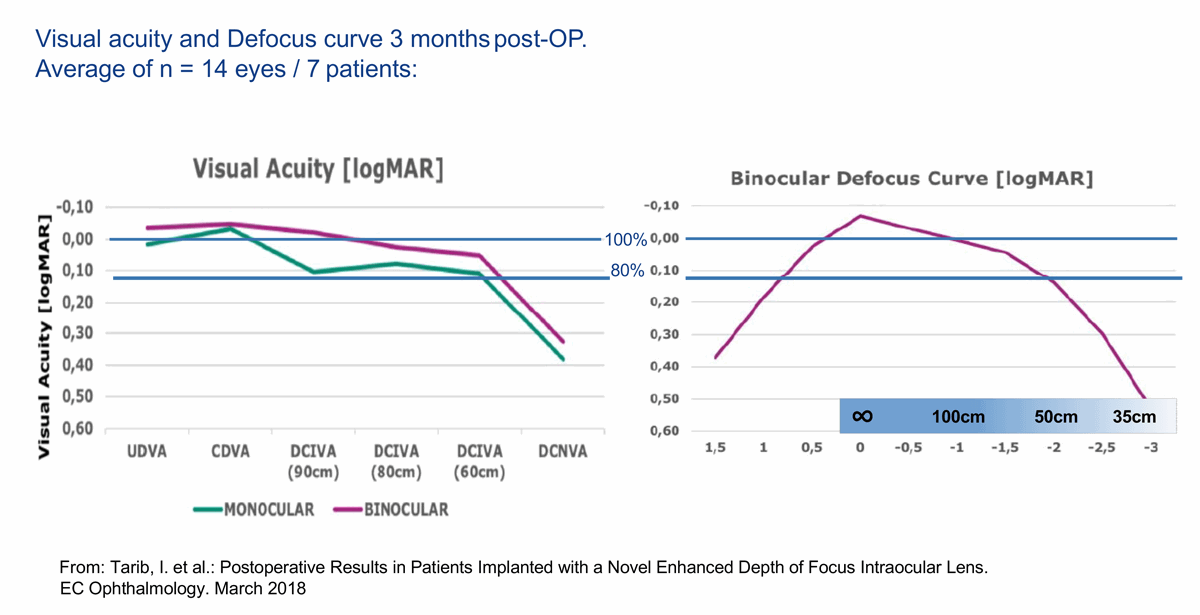
Figure 5: ZEISS AT LARA: Clinical results confirm excellent visual acuity over a wide range of focus.
The IC-8 small aperture IOL (Acufocus) extends depth of focus by combining small aperture optics with an aspheric monofocal lens, and is designed to deliver a natural range of vision with greater spectacle independence for presbyopic and cataract patients [13]. Studies have shown that the IC-8 delivers reliable extended depth of focus with high levels of patient satisfaction [14].

Figure 6: Precizon Presbyopic IOL.
Precizon Presbyopic and Precizon Presbyopic Natural Visual Acuity (NVA) are two new acrylic IOLs from Ophtec for the correction of presbyopia, providing alternatives to regular multifocal IOLs (Figure 6). These IOLs incorporate an aberration-neutral continuous transitional focus (CTF) optical design, with an anterior surface having multiple segments for far and near and designed for ‘natural’ vision at all distances while reducing unwanted glare and halos [15]. Continuous transitional focus lenses can provide focus within the entire depth of field, which means that the image more closely mimics the visual experience of the natural lens [15]. The lens is designed to be pupil independent and to allow patients to enjoy better vision at different distances.
Rayner’s preloaded RayOne Trifocal and the Sulcoflex Trifocal IOLs offer additional options for patients seeking presbyopia correction. The Sulcoflex Trifocal supplementary IOL is an adjustable option that allows practitioners to treat a wide range of patients for presbyopia. It provides predictable refractive outcomes and high visual acuity. The Sulcoflex Trifocal has fewer rings on the optic surface than many trifocal IOLs for reduced potential visual disturbances and improved night vision. RayOne Hydrophobic IOL is a fully-preloaded system that provides surgeons with an easy-to-use injector system for lens delivery, with clinical evaluations showing consistent, excellent refractive outcomes.
Toric IOLs for astigmatism
Newer toric IOLs for cataract surgery are available that effectively reduce levels of postoperative astigmatism and with reducing levels of spectacle dependence compared with non-toric lenses.
Kessel et al. previously demonstrated the superiority of toric IOLs compared with monofocal IOLs with or without corneal relaxing incisions, although patients randomised to toric IOL implantation had to undergo significantly more secondary surgical procedures because of IOL rotation and retinal tears [16]. Evidence from numerous randomised controlled trials (RCTs) demonstrate better uncorrected distance visual acuity, lower levels of postoperative astigmatism and less spectacle dependence for distance viewing in people that received a toric IOL than those implanted with a non-toric IOL, with or without limbal relaxing incisions.
A majority of cataract patients with significant corneal astigmatism undergoing toric IOL implantation can be expected to achieve reduced cylindrical correction and improved unaided visual acuity (UVA), although patients should be counselled about the risk of lens rotation, according to findings from an evaluation of real world refractive outcomes in a UK NHS setting [17].
In this study of 32 eyes of 24 patients who received a toric IOL implant (Tecnis Toric, AcrySof Toric or Rayner T-flex) over a 10-month period at Oxford Eye Hospital, postoperative UVA was superior to preoperative best corrected visual acuity (BCVA) in 81% of eyes, unchanged in 16% and inferior in 3%, with a median improvement of 0.20 logMAR. Previous vitrectomy was identified as a common risk factor in two thirds of cases of significant IOL rotation.
Impact of lens material on postoperative intervention
A retrospective Electronic Medical Record study in the UK evaluated three-year incidence of Nd:YAG capsulotomy and posterior capsule opacification (PCO) and its relationship to monofocal acrylic IOL biomaterial (excluding hybrid combinations), capturing real world data from over 52,000 cataract procedures (restricted to patients aged 65 years or older) performed across multiple UK sites [18].
Approximately one tenth of cases developed PCO at three years’ post-cataract surgery and overall more than half of these required a Nd:YAG capsulotomy procedure to treat PCO. Incidences of Nd:YAG capsulotomy and PCO were lower for hydrophobic compared with hydrophilic acrylic IOLs, reinforcing published evidence suggesting that hydrophobic IOLs are associated with a lower incidence of secondary interventions compared with hydrophilic IOLs [19]. The study found that hydrophobic AcrySof IOLs are associated with a significantly lower risk of requiring Nd:YAG capsulotomy and have the lowest incidence of PCO compared to cohorts of other hydrophilic and hydrophobic acrylic IOLs.
At three years’ post-cataract surgery, the overall incidence proportion of Nd:YAG capsulotomy was 6.4%. For the different cohorts implanted with AcrySof, non-AcrySof hydrophobic and non-AcrySof hydrophilic IOLs, the incidence proportions of Nd:YAG capsulotomy at three years following cataract surgery were 2.4%, 4.4% and 10.9%, respectively [18]. The same trend was observed in single-piece IOLs only.
Principal investigator and lead author Mr Paul Ursell, Epsom & St Helier University Hospitals NHS Trust, Epsom, UK, explained: “There is no doubt from the evidence collated from multicentre clinical practice in the NHS that choice of IOL material for lens implantation during cataract surgery has an overriding effect on the subsequent odds of undergoing an Nd:YAG capsulotomy procedure. The study found that implantation with non-AcrySof hydrophilic acrylic IOLs was associated with an almost fivefold increased odds of undergoing Nd:YAG capsulotomy at three years after cataract surgery compared with hydrophobic AcrySof IOLs.”
Addressing patient expectations of refractive implications, surgeons should ‘underpromise and overdeliver’
Patient expectations of spectacle independence at all distances following cataract surgery have substantially increased in recent years.
Dr Findl said that, as a surgeon, his advice to younger colleagues is always to use the lens that they are most comfortable with, but also the lens that they believe is best suited to the individual patient.
“Particularly in the case of premium IOLs, patients may have high expectations with respect to refractive outcomes after the lens is implanted,” added Dr Findl. “We know also that patients implanted with multifocal IOLs are more likely to undergo IOL exchange than those receiving monofocal implants. It is important therefore to ensure that patients have realistic expectations before surgery and in my opinion, surgeons are encouraged to follow the motto ‘underpromise and overdeliver’.”
Ongoing research and development is focused on further strengthening IOL platforms to further improve surgical and refractive outcomes. Optimisation of IOL design and overall safety will continue to develop alongside enhanced multifocal technology, said Dr Findl. Research evaluating IOL power adjustment using refractive index shaping laser technology may yield future options that allow physicians to adjust the power of an IOL inside the eye after surgery.
References
1. Data on file, Johnson & Johnson Surgical Vision, Inc. 2018. DOF2018CT4015.
2. Khandelwal SS, Jun JJ, Mak S, et al. Effectiveness of multifocal and monofocal intraocular lenses for cataract surgery and lens replacement: a systematic review and meta-analysis. Graefes Arch Clin Exp Ophthalmol 2019 [Epub ahead of print].
3. de Silva SR, Evans JR, Kirthi V, et al. Multifocal versus monofocal intraocular lenses after cataract extraction. Cochrane Database Syst Rev 2016;12:CD003169.
4. Kohnen T, Martinez A. Multicenter visual outcomes evaluation of a novel trifocal presbyopia correcting IOL – 12 months’ post-op results. XXXVI Congress of the ESCRS 2018, Vienna, Austria.
5. Lapid-Gortzak R, Duch F, Elies D, et al. Multicenter visual outcomes comparison of two trifocal presbyopia correcting IOLs – 6 months post-op results. World Ophthalmology Congress 2018, Barcelona, Spain.
6. Mencucci R, Favuzza E, Caporossi O, et al. Comparative analysis of visual outcomes, reading skills, contrast sensitivity, and patient satisfaction with two models of trifocal diffractive intraocular lenses and an extended range of vision intraocular lens. Graefes Arch Clin Exp Ophthalmol 2018;256(10):1913-22.
7. Cochener B, Boutillier G, Lamard M, Auberger-Zagnoli C. A comparative evaluation of a new generation of diffractive trifocal and extended depth of focus intraocular lenses. J Refract Surg 2018;34(8):507-14.
8. Poyales, F, Garzón N, Poyales C, Poyales B. Clinical outcomes with a new model of extended depth of focus intra-ocular lens. Open Journal of Ophthalmology 2018;8:161-70.
9. Akella SS, Juthani VV. Extended depth of focus intraocular lenses for presbyopia. Curr Opin Ophthalmol 2018;29(4):318-22.
10. Savini G, Schiano-Lomoriello D, Balducci N, Barboni P. Visual performance of a new extended depth-of-focus intraocular lens compared to a distance-dominant diffractive multifocal intraocular lens. J Refract Surg 2018;34(4):228-35.
11. Hogarty DT, Russell DJ, Ward BM, et al. Comparing visual acuity, range of vision and spectacle independence in the extended range of vision and monofocal intraocular lens. Clin Exp Ophthalmol 2018;46(8):854-60.
12. Tarib I, Kasier I, Herbers C, et al. Postoperative results in patients implanted with a novel enhanced depth of focus intraocular lens. EC Ophthalmology 2018;9(4):192-202.
13. Grabner G, Ang RE, Vilupuru S. The small-aperture ic-8 intraocular lens: a new concept for added depth of focus in cataract patients. Am J Ophthalmol 2015;160(6):1176-84.
14. Dick HB, Piovella M, Vukich J, et al; Clinical Investigators. Prospective multicenter trial of a small-aperture intraocular lens in cataract surgery. J Cataract Refract Surg 2017;43(7):956‑68.
15. Mesa RR, Monteiro T. Continuous Transitional Focus (CTF): A new concept in ophthalmic surgery. Ophthalmol Ther 2018;7(2):223-31.
16. Kessel L, Andresen J, Tendal B, et al. Toric intraocular lenses in the correction of astigmatism during cataract surgery: a systematic review and meta-analysis. Ophthalmology 2016;123(2):275-86.
17. Xue K, Jolly JK, Mall SP, et al. Real-world refractive outcomes of toric intraocular lens implantation in a United Kingdom National Health Service setting. BMC Ophthalmol 2018;18(1):30.
18. Ursell PG, Dhariwal M, Majirska K, et al. Three-year incidence of Nd:YAG capsulotomy and posterior capsule opacification and its relationship to monofocal acrylic IOL biomaterial: a UK Real World Evidence study. Eye (Lond) 2018;32(10):1579-89.
19. Zhao Y, Yang K, Li J, et al. Comparison of hydrophobic and hydrophilic intraocular lens in preventing posterior capsule opacification after cataract surgery: An updated meta-analysis. Medicine (Baltimore) 2017;96(44):e8301.
TAKE HOME MESSAGE
-
Monofocal IOLs, the current standard IOL design used for cataract surgery in the NHS, have a single focal point and, where the intended refractive outcome is good unaided distance visual acuity, patients usually require spectacles for reading.
-
Multifocal IOLs can improve vision at all distances and correct the symptoms of presbyopia, increasing the likelihood of spectacle independence; however, they are associated with adverse symptoms, have a significant cost premium and are not recommended by the National Institute for Health and Care Excellence.
-
Extended depth of focus lenses may provide satisfactory near and intermediate vision with a reduced incidence of optical phenomena often experienced by patients implanted with multifocal lenses.
-
Toric IOLs effectively reduce levels of postoperative astigmatism and can result in increased unaided distance visual acuity, with reducing levels of spectacle dependence compared with non-toric lenses.
-
A study of over 52,000 cataract procedures in the UK show that incidences of Nd:YAG capsulotomy and posterior capsule opacification were lower for hydrophobic acrylic IOLs compared with hydrophilic acrylic IOLs.
The author has no proprietary or financial interests in the products discussed.
COMMENTS ARE WELCOME





