
Introduction
Herpes zoster, commonly known as shingles, is caused by the reactivation of varicella zoster virus (VZV). The term herpes is derived from a Greek work, herpein, which means ‘creeping’ and the word zoster means a belt or a girdle which is worn like an armour, which covers one half of the body [1]. VZV belongs to the alpha herpes family.
It is an enveloped, double stranded DNA virus which stays dormant in the sensory root ganglion after the primary infection and reactivates later in agEing patients due to the decrease in cell mediated immunity [2]. The reactivation can happen in any sensory ganglia and when it occurs in the trigeminal ganglion associated with ocular involvement, the term herpes zoster ophthalmicus (HZO) is used. Any branch of the trigeminal nerve (ophthalmic, maxillary, mandibular) can be involved, but ophthalmic division of the trigeminal nerve is most commonly affected [1].
Pathogenesis
VZV causes two important diseases, namely chickenpox and shingles [3]. Varicella Zoster virus is predominantly transmitted through the respiratory route or through direct contact from another person. The incubation period is 10 to 21 days. The primary infection involves the virus being transported from the pharyngeal lymphoid organs to the skin, which then presents as vesicular eruption on the skin. Due to active viral replication, the skin lesions show inflammatory cells and necrosis on histopathological analysis [1]. The VZV in the epidermis spreads to the surrounding sensory nerves, travels in a retrograde fashion to the sensory ganglion, where it lies dormant [3]. Though the primary infection resolves, the virus remains dormant in the ganglion and reactivates later in life or in immunocompromised states.
Risk Factors
- Advancing age
- Decreased cellular immunity such as cancer, radiation, acquired immunodeficiency syndrome, organ transplantation.
Clinical features:
What not to miss in history taking:
- Any previous history of immunosuppression (immunosuppressive medications for solid organ transplantation or other indications, radiation, HIV, malignancy)
- Recurrent episodes.
Examination of the rash
Approximately 60% of the patients have pain along the distribution of the trigeminal nerve [4]. The skin manifestation begins as a painful rash with an erythematous base, which later progresses to a papule, and, finally to a cluster of vesicles containing serous or purulent fluid. Virus transmission from person to person can occur through the fluid from the vesicles. The rash typically lies along the distribution of the ophthalmic branch of trigeminal nerve (V1) and does not cross the vertical midline. If the lesions involve the side or tip of the nose, ocular involvement is more likely (Hutchinson’s sign).
What to look out for in the eye
Any patient demonstrating involvement of the ophthalmic division of the trigeminal nerve should be suspected of eye involvement. Examination of the eye involves checking pupillary response for relative afferent pupillary defect (RAPD), slit-lamp examination and dilated fundus examination.
Ocular manifestations:
1. Blepharoconjuctivitis
Cutaneous rash with or without vesicular lesions over the eyelid along with papillary or follicular conjunctivitis is very common. The vesicles usually heal within two to three weeks. Vesicles can also affect the conjunctiva and cornea. Secondary bacterial infection of the vesicular lesions can lead to scarring in lids and resultant entropion, ectropion or trichiasis.
2. Corneal involvement
About two third of the patients have corneal involvement [1]. Corneal involvement can be superficial punctate keratitis, pseudo-dendrites, stromal keratitis, disciform keratitis or endothelitis [7].
A) Superficial punctate epithelial keratitis (SPEK)
Punctate epithelial keratitis is due to the oedema of the superficial epithelial cells of the cornea. They appear as multiple, small punctate lesions which stain with fluorescein.
B) Pseudo-dendrites
These are superficial oedematous epithelial lesions, which have a branching pattern with no terminal bulbs (Figure 1). These lesions stain minimally with fluorescein. It is important to differentiate these pseudo-dendrites from the dendritic lesions associated with herpes simplex virus infection.
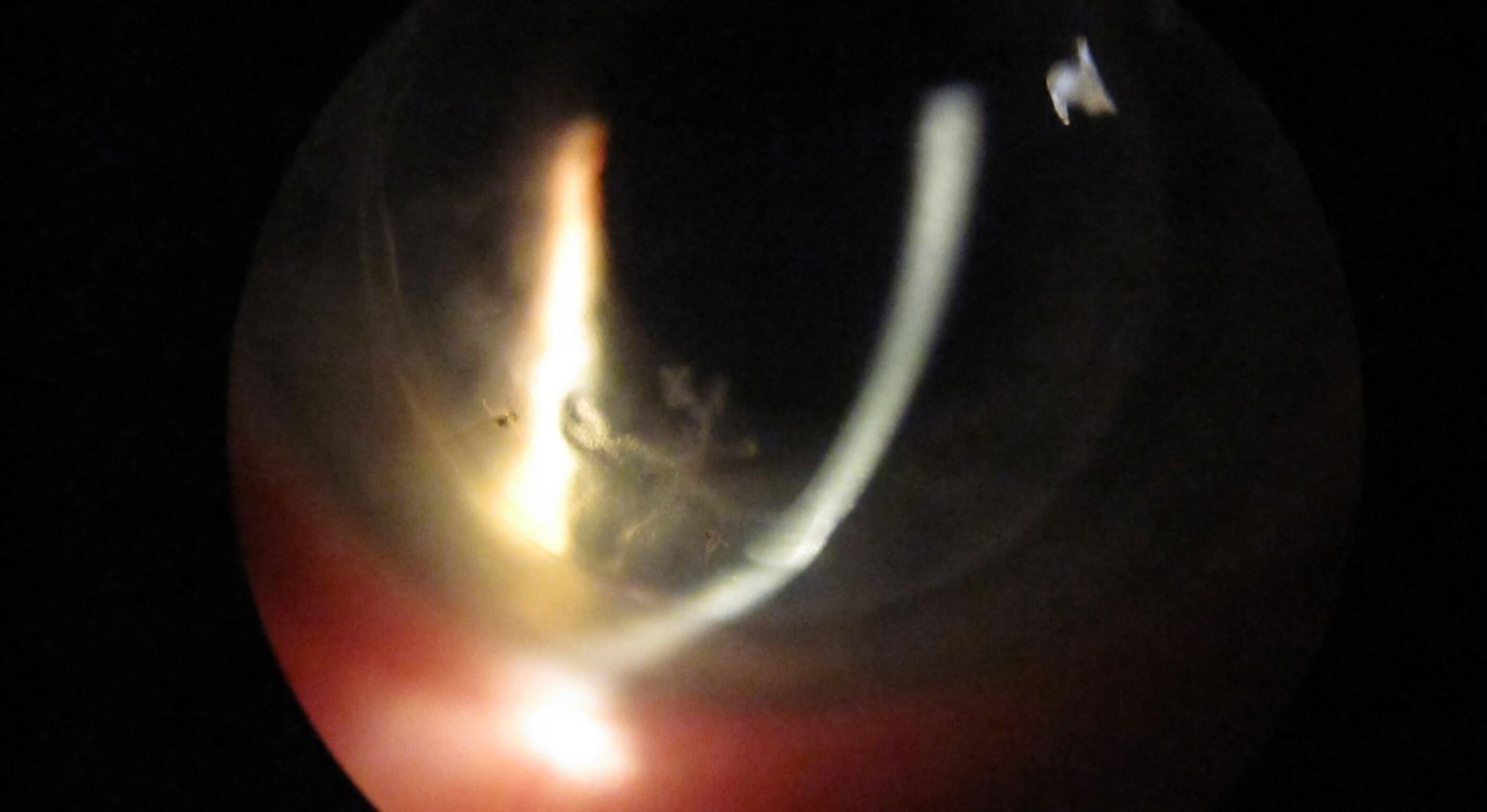
Figure 1: Pseudo-dendrite in a patient with Herpes zoster ophthalmicus.
C) Stromal keratitis
Stromal keratitis usually involves the anterior stroma. It presents as granular stromal infiltrates under the surface of epithelial lesion. The stromal keratitis can represent active viral infection or an immune reaction to the viral antigens (Figure 2).
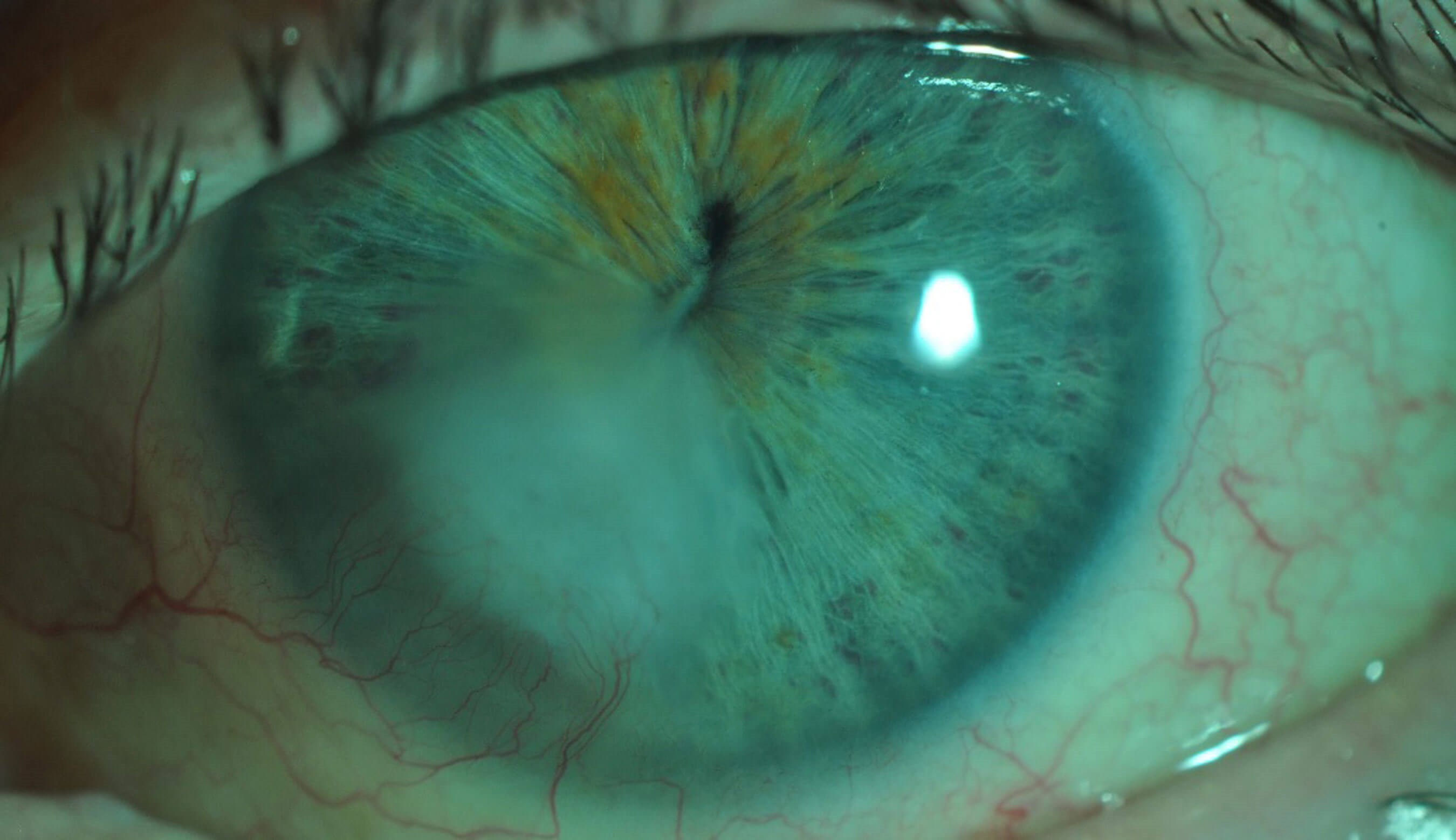
Figure 2: Stromal keratitis with anterior stromal involvement and superficial vascularisation.
D) Endothelitis
Endothelitis present as a Descemet’s membrane folds and keratic precipitates over the corneal endothelium. This can be associated with overlying corneal oedema.
E) Disciform keratitis
Disciform keratitis is a disc shaped stromal oedema in the central or paracentral cornea due to immune reaction to the viral antigens. The epithelium overlying the oedema is usually intact. This may be associated with keratic precipitates in that area (Figure 3).
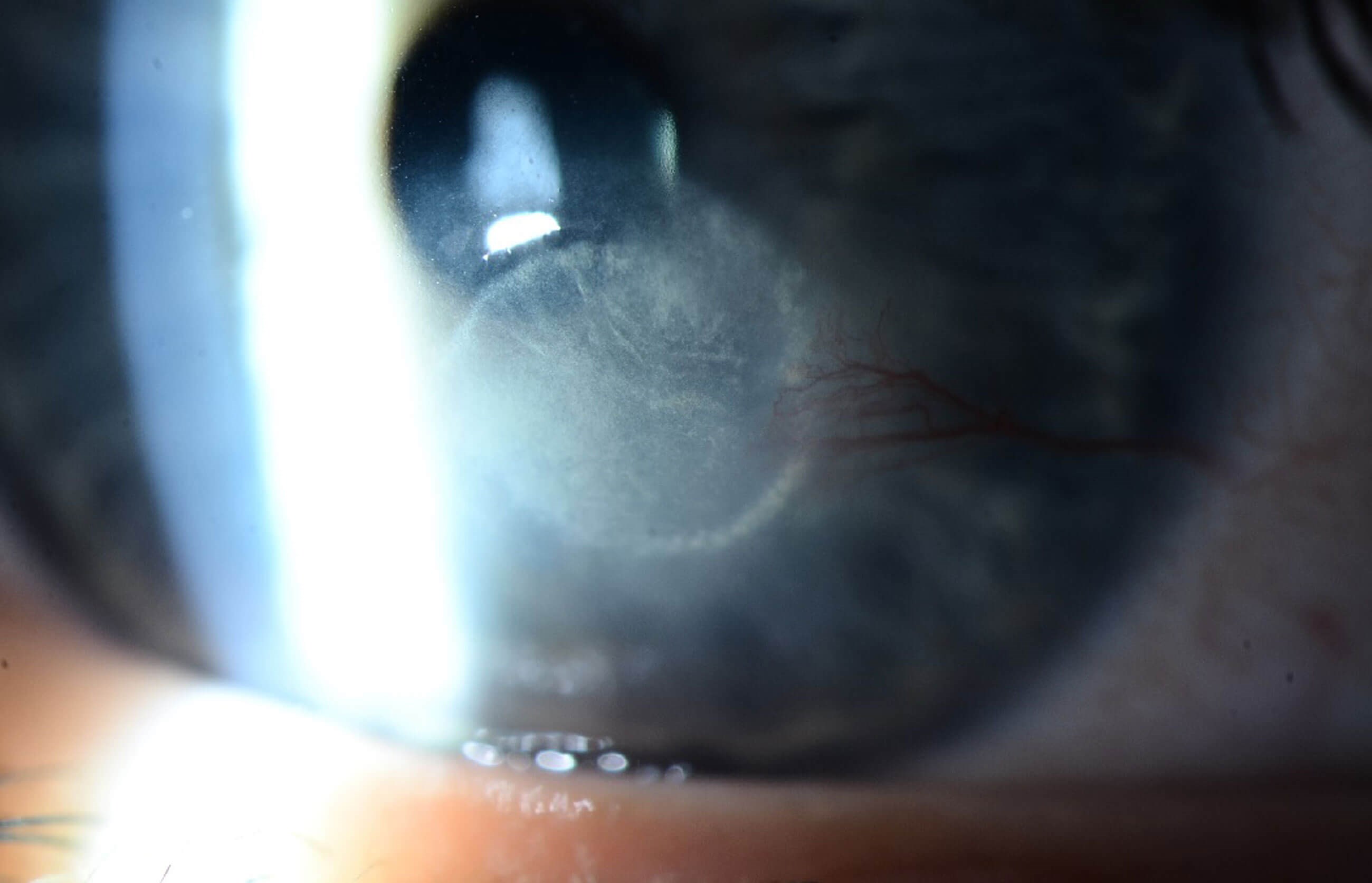
Figure 3: Disciform keratitis.
F) Neurotrophic keratopathy
Reduced corneal sensation because of damage to the ophthalmic branch of trigeminal nerve leads to neurotrophic keratopathy. The clinical features of neurotrophic keratopathy include corneal haze, corneal epithelial irregularity, frequent epithelial breakdown, ulceration (Figure 4) or in severe cases corneal melt and perforation. This can affect vision to various degrees.
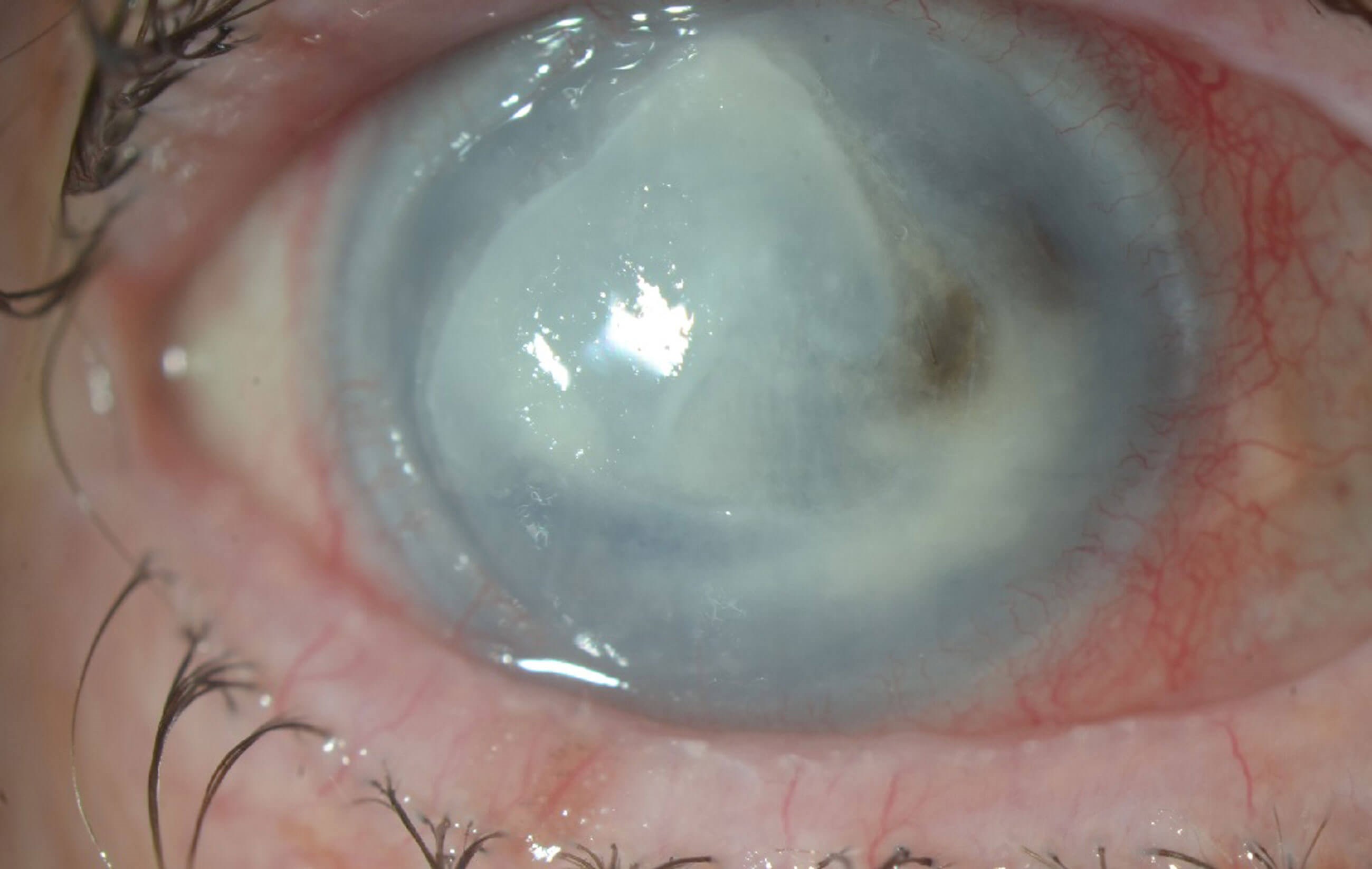
Figure 4: Non healing neurotrophic ulcer with irregular raised edges.
3. Uveitis
Approximately 40% of patients with herpes zoster ophthalmicus develop uveitis [1]. The inflammation presents as corneal oedema, keratic precipitates, anterior chamber cells, hypopyon and posterior synechiae. Uveitis is often associated with a raised intraocular pressure. Due to ischemia of the iris vessels, sectoral iris atrophy and irregular pupil shape are not uncommon
4. Post-herpetic neuralgia
Post Herpetic neuralgia occurs in around 9.3-17% of the patients [1]. The patients present with pain along the affected dermatome, which is described as burning, stabbing, or shooting.
5. Herpes zoster optic neuropathy
Herpes Zoster Optic Neuropathy is a rare, but vision threatening complication of herpes zoster which occurs in 1.9% of the patients affected by HZO [6]. Profound loss of vision with a relative afferent pupillary defect and swelling of the optic disc can often be associated with inflammation in the central nervous system.
Diagnosis
In the majority of the cases, the diagnosis is based on the typical signs and symptoms. In the situation of a diagnostic uncertainty, investigations are needed to confirm clinical suspicion. Viral swabs can be obtained from the skin lesions or from the eye. The virus can be identified by polymerase chain reaction (PCR), Tzank smear, enzyme linked immunosorbent assay (ELISA) or by viral culture.
Differential diagnosis for the clinical presentation
Acute phase of VZV infection with lid swelling can share clinical features with the following:
- Pre-septal cellulitis/orbital cellulitis because of bacterial/fungal infection: restricted ocular movements and proptosis are often seen in orbital cellulitis.
- Acute angle closure attack: this is usually unilateral and presents as rapid onset unilateral headache associated with nausea, vomiting, and halos. Patients complain of decrease in vision due to corneal oedema secondary to rapid rise in intraocular pressure. Skin rash is absent.
- Contact dermatitis: allergic reaction due to exposure to a substance can lead to erythematous changes on the skin. In contrast to the herpes zoster ophthalmicus, the erythematous region does not respect the midline and can cross over to the other side.
Corneal lesions can be confused for:
- Herpes simplex keratitis: Herpes simplex virus, just like herpes zoster can reactivate in immunosuppressed individuals. It is very important to ask about history of cold sores. The dendrites on the cornea are small, branching and have terminal bulbs in contrast to herpes zoster keratitis which has a pseudo dendrite without a terminal bulb (Figure 3).
- Healing corneal abrasion: Pseudo-dendrite can also be observed in healing corneal abrasion. There is usually a history of injury / surgery.
- Acanthamoeba keratitis: Corneal pseudo-dendrites are usually seen in contact lens wearers and are extremely painful at presentation.
Management
- In the acute stage presenting with skin rash (HZO): The standard recommended treatment for Herpes zoster ophthalmicus is oral acyclovir 800mg, five times per day for seven to 10 days. If the treatment is started within 72 hours of onset of symptoms, there is decrease in viral shedding [4]. More severe acute presentations such as optic nerve involvement will need intravenous acyclovir therapy. There is a reduced risk of ocular complications by 20%-30% in patients treated with Acyclovir [6]. There is also a reduced risk of post-herpetic neuralgia if the oral antiviral therapy is instituted within 72 hours of the onset of rash [5]. Valacyclovir and famciclovir are alternatives to acyclovir with increased bioavailability. Antivirals should be administered with extra caution in patients with deranged renal function and intravenous route of acyclovir is avoided in patients with renal failure.
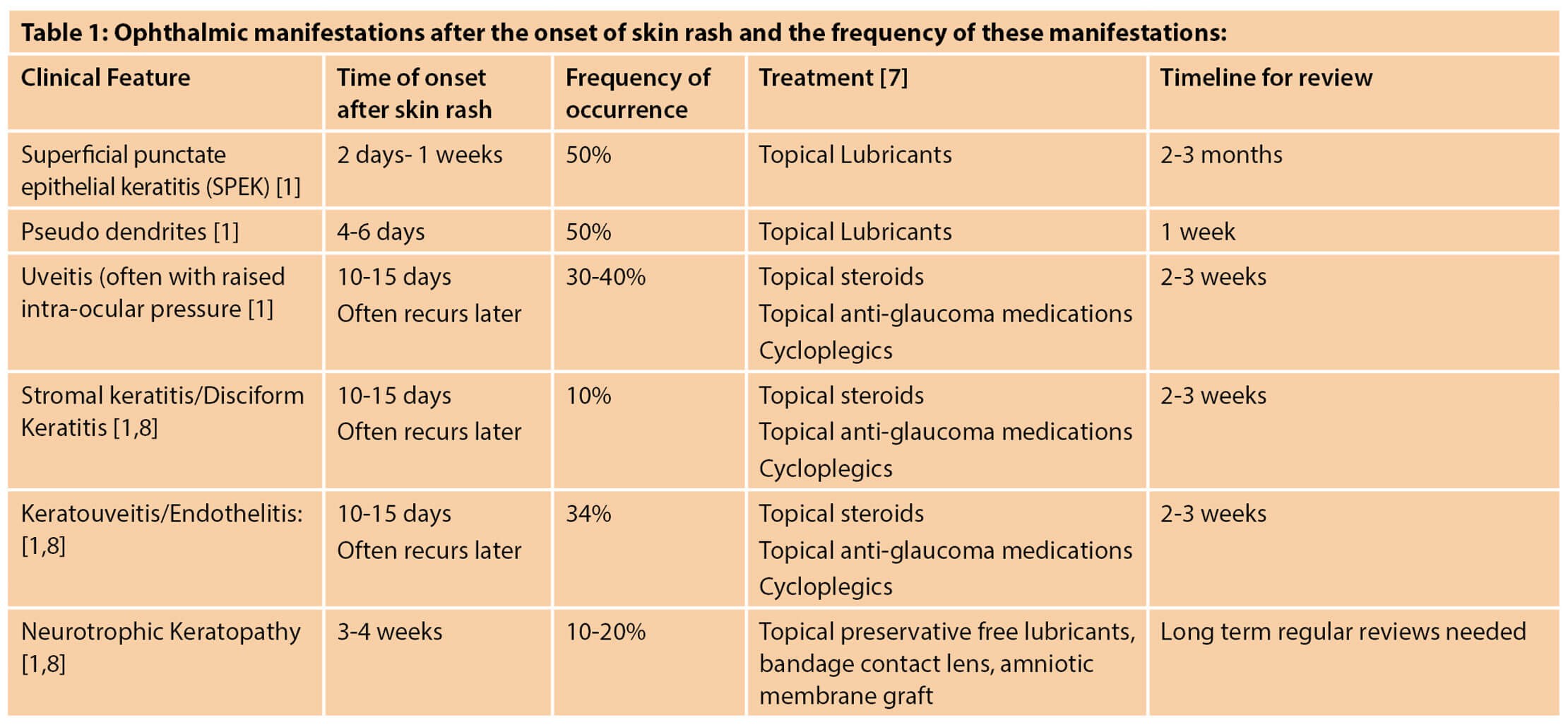
- Managing ophthalmic manifestations of HZO: The usual timeline of other ophthalmic manifestations after the onset of skin rash and the frequency of these manifestations along with their management plan is described in the table below (Table 1).
- Post-herpetic neuralgia: Persistent pain more than three months after the initial skin rash following the dermatomal distribution of the initial HZO episode can occur in 10-20% of cases. Oral antiviral therapy started within 72 hours of onset of skin rash reduces incidence and severity. VZV vaccine also reduces incidence and severity. A wide variety of systemic and local therapies exist [1]. The pain can be chronic and debilitating.
Conclusion
Hepes zoster ophthalmicus caused by reactivation of varicella zoster virus is common with advancing age and in immunocompromised patients. In patients presenting with rash on one half of the face, it is important to rule out ocular involvement. This article summarises the ocular manifestation of herpes zoster and how they are encountered in a clinical setting. Early recognition and treatment would prevent irreversible vision loss and complications.
TAKE HOME MESSAGE
-
Herpes zoster ophthalmicus caused by varicella zoster virus can occur because of reactivation of the virus which remained dormant in the trigeminal ganglia.
-
It is important to examine the rash and to rule out ocular manifestation of herpes zoster.
-
Patients with active viral infection should be started on tablet acyclovir 800mg five times per day for seven to 10 days.
References
1. Krachmer J H, Mannis M, Hollabd E. Cornea. 3rd edition. Amsterdam, Netherlands; Elsevier; 2010:985-1000.
2. Weinberg JM. Herpes zoster: epidemiology, natural history, and common complications. J Am Acad Dermatol 2007;57(Suppl 6):S130-5.
3. Gershona AA, Gershon MD, Breuer J, et al. Advances in the understanding of the pathogenesis and epidemiology of herpes zoster. J Clin Virol 2010;48(Suppl 1):S2–S7.
4. Shaikh S, Ta CN. Evaluation and management of herpes zoster ophthalmicus. Am Fam Physician 2002;66(9):1723-30.
5. Jackson JL, Gibbons R, Meyer G, Inouye L. The effect of treating Herpes zoster with oral acyclovir in preventing post herpetic neuralgia. A meta-analysis. Arch Intern Med 1997;157(8):909-12.
6. Hunt CM, Gregory HM, Gannon W. Oral valacyclovir treatment of herpes zoster ophthalmicus-induced optic neuritis. Cureus 2021;13(8):e17033.
7. Liesegang TJ. Diagnosis and therapy of herpes zoster ophthalmicus. Ophthalmology 1991;98(8):1216-29.
8. Cobo M, Foulks GN, Liesegang T, et al. Observations on the natural history of herpes zoster ophthalmicus. Curr Eye Res 1987;6(1):195-9.
9. Liesegang TJ. Corneal complications from Herpes zoster ophthalmicus. Ophthalmology 1985;92(3):316-24.
10. Schott GD. Whence 'zoster'? The convoluted classical origins of a sometimes illogical term. Med Humanit 2017;43(1):15-18.
11. Ting DSJ, Ghosh N, Ghosh S. Herpes zoster ophthalmicus BMJ 2019;364:k5234.
12. Aggarwal A, Suresh V, Gupta B, Sonthalia S. Post-herpetic neuralgia: a systematic review of current interventional pain management strategies. J Cutan Aesthet Surg 2020;13(4):265-74.
13. Leung J, Harrington T, Dooling K. Zoster. In: Hall E, Wodi AP, Hamborsky J, Morelli V, Schillie S, (Eds.). Epidemiology and Prevention of Vaccine-Preventable Diseases. 14th Edition. Atlanta, USA; CDC; 2021:349-58.
COMMENTS ARE WELCOME







