
World Sight Day (WSD) was celebrated globally on 8 October 2020 [1]. From Australia and the Pacific to the Americas, via Asia, Africa and the Caribbean, awareness-raising and advocacy activities took place throughout the day, to focus attention on unnecessary blindness and visual impairment.
The VISION 2020 LINKS Programme [2] and DR-NET [3], its collaborative network of 28 diabetic retinopathy (DR) centres in 20 low- and middle-income countries (LMICs), came together virtually with a celebration of the progress made in screening and treating people living with diabetes (PLWD).
The workshop was opened by Professor Hannah Faal, well-known to all participants as a founder of the VISION 2020 initiative, and former President of the International Agency for the Prevention of Blindness (IAPB) [4]. The message for WSD 2020 was ‘Hope in Sight’, which matched the aim of DR-NET – to preserve the sight and improve the lives of the 463 million adults who are living with diabetes and are at risk of DR.
The international collaboration of DR-NET was highlighted by the varied and fascinating presentations and videos of experiences from Botswana, Zambia, Kenya, Malawi, Burundi, Nigeria and the UK.
Cova Bascaran and Nyawira Mwangi and colleagues at the International Centre for Eye Health, London School of Hygiene & Tropical Medicine, anchored the workshop with their research into the available evidence, addressing some of the key questions about screening and treatment of PLWD for DR in LMICs, using rapid reviews (research as yet unpublished; funded by The Fred Hollows Foundation). The need for more research and evidence to drive forward the development of effective, sight-saving DR services in LMICs had been highlighted previously by the DR-NET participants. Equally, the need for DR services to be more patient-centred was key to driving down the number of people unnecessarily blind from DR.
Dr Bascaran used a ‘leaky pipe’ analogy to describe four key points at which patients were failing to access the detection or treatment that they needed and which had been highlighted by a panel of invited experts to be in need of research to review the available evidence.

‘Leaky pipe’ diagram of a patient’s journey through DR services.
Several of the subsequent presentations looked at the role of task-shifting in development of DR services and the challenges of providing high-quality screening services in resource-poor settings. Participants heard how in the main government hospital in Lagos, Nigeria, there is no fundus camera, so screeners use their mobile phone with a 20D lens for screening and grading PLWD for DR. In Zambia people previously employed as patient assistants and porters had been trained to take pictures using a fundus camera and to grade the images. This way, the skills of the ophthalmologists fromand nurses could be focused on patient treatment and care. Counselling of patients so that they understand the seriousness of their condition and what to expect when they have treatment for DR was crucial to ensure that people returned for regular screening and for treatment, if necessary.
Leaky pipe 1 – DR screening
The first ‘leak’ investigated was at the stage of screening for DR. The number of PLWD in Africa is increasing rapidly and there is a need to examine them annually for DR. The aim of the review was to synthesise the evidence on the effect of task-shifting screening to non-clinical staff on uptake, quality and cost-effectiveness outcomes. The review of the literature from the last 10 years showed that there had been 12 articles reporting uptake and detection rates of screening after task-shifting, none of which provided a baseline or comparator, limiting the conclusions on the effectiveness of the interventions. The research also looked at diagnostic accuracy of the task shifting cadre compared to ophthalmologists; there was moderate evidence that other cadres could achieve comparable accuracy to that of ophthalmologists, with a similar detection rate.
Describing the development of DR services in the UK, Professor Tunde Peto of Queen’s University Belfast outlined the approach taken to task-shifting to address the huge burden of diabetes in the population. She highlighted the value of a multidisciplinary approach, where people with different roles in the care of PLWD work together, the need for every step of the patient journey to have a quality and a failsafe component, and the need for clinicians to empower and show trust in the professional skills of their team.
The next part of the workshop addressed this issue through a patient-centred approach to DR services. Interviews with patients from Kenya and Botswana enabled their personal perspectives on screening and treatment to be heard. Both patients had had diabetes for over 10 years and had been referred to the eye clinic. “The only challenge is now when it is affecting my eyesight,” said one patient. Both were appreciative of the DR services that they had received. However, the cost of treatment was raised as an issue and one stated that there was a lack of awareness of information about DR and the existence of support groups. In addition, COVID-19 meant that patients were afraid to go to hospital and risk becoming infected.

The team from Frimley Park Hospital with screener / graders during a training session in Zambia.
Pearl Mbulawa, DR screener and grader at Princess Marina Hospital, Gaborone,
discussing DR with a patient during the WSD workshop.
Kenyan ophthalmologists Nyawira Mwangi and Muchai Gachago reflected on the need for more education, not just for patients but also for physicians. Their experience was shared by many other ophthalmologists in LMICs – PLWD were coming forward to the eye services after having diabetes for many years; their DR was already advanced, treatment was expensive and the outcome was not very good. Sometimes the problem was that, although patients were seeing physicians at primary or secondary level, they were not being referred early enough for screening for DR. They identified a need for better education of primary level clinicians.
Leaky pipe 2 – from screening to eye services
The second ‘leak’ identified by the rapid reviews was at the stage of referral of patients with DR from a screening session into the eye service. A patient-centred approach to delivery of DR services is required to address the many issues that determine whether a patient referred from screening in the diabetes clinic or primary care setting will attend for examination in the eye clinic. The review of publications over the last 10 years found eight papers from LMICs that described methods used to ‘plug the leak’, including health education talks, leaflets, posters, use of counselling, and in some places patients carried a ‘diabetic passport’. There were also ways of reaching the wider population, including TV and radio broadcasts. One technique that seemed to be of value was giving and explaining grading results to the patient immediately at the point of care, so that they understood the importance of attending the eye service. None of the eight papers had a comparison of results before and after introducing interventions to address the loss of patients. Despite describing attempts to increase uptake, most of the studies reviewed showed that fewer than half of the patients referred from screening actually arrived in the eye clinic.
Leaky pipe 3 – uptake of treatment
The third ‘leak’ identified by the rapid reviews was at the stage of referral of patients for treatment. The review of publications from LMICs over the last 10 years didn’t find any studies reporting interventions to increase uptake of treatment for DR. Yet this is an area where a significant number of patients are lost and in need of further investigation; as efforts and resources are being put into expanding screening services there is a need for evidence that this leads to uptake of potentially sight-saving treatment.
Adel Pinnock, DR Screener / Grader and Health Promotion Specialist, used Beattie’s model [5] to explain how different approaches to health promotion can be used – and that they are most effective when a number of different approaches are used together. Beattie’s model uses four quadrants; the vertical axis is the mode of the interventions and the horizontal axis is the focus of the interventions. It encompasses top-down, expert-led interventions and bottom-up, participant-led interventions.

Beattie’s model.
Beattie’s model explains that a combination of different approaches from within each quadrant is needed to get the maximum impact. Most of the interventions described in the presentations fell into the health persuasion quadrant; research had found this to be ineffective in promoting positive health behaviours when used in isolation. There was a need to address the wider social determinants of health that cause health inequalities.
Leaky pipe 4 – the safety of vial sharing for multiple patients treated with anti-VEGF
The final area chosen for review was the safety of vial sharing for multiple patients treated with anti-VEGF. As patients often require multiple treatments, the high cost of anti-VEGF treatment can lead to ‘fall off’ of patients receiving treatment. Anti-VEGF vials often exceed the dose needed, so many centres share vials between patients, taking care to reduce cross-contamination. From the very small number of relevant papers it was concluded that vial sharing was cost-effective, but rates of endophthalmitis varied hugely and no studies included rates of completed treatment. ‘Leaky pipe’ diagram of a patient’s journey through DR services.
Presentations from Malawi and Burundi followed. Participants were given insights into the effect of the COVID-19 pandemic on the provision of eye care services at Lions Sight First Eye Hospital in Lilongwe, Malawi. Consultant Ophthalmologist Joseph Msosa talked to LINK partner Ophthalmologist Caroline Styles from NHS Fife, Scotland. For six months, only emergency services had been offered and the staff of the eye hospital had worked on a rota system to enable emergency services to be maintained while reducing the risk of contracting or passing on the disease. Thankfully, eye services had recently returned to nearer normal.
Celebrating World Sight Day 2020 in Dominica
Hazel Shillingford-Ricketts, Consultant Ophthalmologist at the Dominica-China Friendship Hospital
“World Sight Day on the second Thursday of October each year gives us a platform for raising awareness and promoting the need for the general public to be vigilant with their sight. The theme this year was ‘Hope in Sight’ which enabled us to highlight the many advances in screening and treatment of eye diseases, particularly DR, that are enabling us to offer better eye services to the public.
“This year we focused on diabetic retinopathy, the leading cause of preventable blindness in the working age population. The day began with our staff joining the online session with the DR-NET and LINKS partners to review development of DR services together across the globe.

Celebrating World Sight Day in Kenya with a feature in the national daily newspaper, The Standard.
“Then we held a DR screening session at our own hospital for the staff of the hospital. Other screening sessions were held in other parts of the island.
“Ophthalmologist Nancy Lawrence and Optometrist Kitwanie Dumas held a district eye clinic in the St Joseph Health District. A talk on DR was also given to the patients.
“I was invited to address the students and staff of Convent High School on DR. It was highlighted that the working age group is 15-64 years-old and many of them are in that group. Obesity is a risk factor for diabetes mellitus and it is increasing, especially among our women. Controlling this risk by diet, exercise and weight loss can reduce the risk for diabetes mellitus. Increased emphasis is placed on prevention of diabetes mellitus to reduce the prevalence of blindness from diabetic retinopathy.
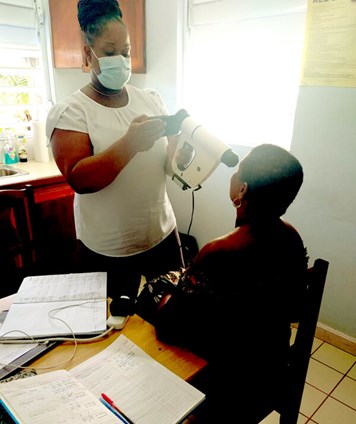
Screener Grader Nanda Matthew examining a patient during a mobile
DR fundus photography screening clinic in the north of the island.
“Next I was hosted on radio talk shows at Dominica Broadcasting Station and Q95 radio station. The listening public was informed about DR and eye services. The opportunity was used to let them know that there is ‘Hope in Sight’ because of increased human resources and eye services. There are now three ophthalmologists in public service on the island, up from one. There are two internationally-certified screener graders providing island-wide DR fundus photography screening. This provides for early detection and early treatment to prevent blindness from DR.

Patient education talk at the special WSD screening session in the St Joseph Health District.

WSD presentation to staff and students at Convent High School, Dominica.
“In Dominica eye services are integrated into Primary Health Care island-wide. PLWD with other eye problems are also detected and referred for further management. Laser treatment is the gold standard treatment for DR. In the last three months treatment with Avastin intravitreal injection has started. A new eye clinic is almost completed at the Dominica China Friendship Hospital. It has an eye operating theatre which will increase eye surgical time from one day a week to five days a week. This will significantly reduce waiting times for eye surgery.
“During WSD, acknowledgment was made of the contribution by the Queen Elizabeth Diamond Jubilee Trust [6] to DR-NET and the development of DR services for the people of Dominica, and the support of the VISION 2020 LINKS Programme at the London School of Hygiene & Tropical Medicine in enhancing the management of DR through training and capacity-building.

Hazel Shillingford-Ricketts on Dominica
Broadcasting Station radio, October 2020.
“With our newly-expanded eye services, and greater public awareness of DR and other causes of blindness, we will be able to achieve our goal of preventing unnecessary blindness throughout the island of Dominica. ‘Hope in Sight’ is a reality in Dominica.”
Closing remarks and feedback survey results
Hannah Faal closed the workshop with a reminder of the need for evidence for the efficacy of interventions: there were opportunities for multidisciplinary and multi-centre working using standardised approaches in order to build the evidence base. There was a clear need to include the patient’s perspective when planning such research.
A feedback survey showed that: 94% of respondents found the workshop ‘very useful’ or ‘useful’ to their practice and everyone felt that it was the right length; 94% would like online refresher training in grading of DR images, either for themselves or for others in their DR team. Respondents suggested that future workshops would be valuable, subjects including DR screening pathways, eye health awareness and promotion, and management of glaucoma.
Comments included:
“I am honoured to have been present at the workshop. I look forward to future workshops to broaden my scope in DR management.”
“Great presentations, I would love to be part of more of these meetings.”
“It was a wonderful workshop where we can see that our problems in handling DR in Indonesia also happen in other countries and it is interesting to see how they deal with it.”
In summary, despite the competing demands on people’s time during WSD, the workshop was attended by over 70 people from 18 countries. The benefits of sharing learning between countries as they develop their DR services was recognised and the collaboration and support offered by the DR-NET and the LINKS Programme was greatly appreciated.
References
1. World Health Organization. World Sight Day 2020:
https://www.who.int/news-room/events/
detail/2020/10/08/default-calendar/
world-sight-day-2020
2. Vision 2020 LINKS Programme:
https://iceh.lshtm.ac.uk/
vision-2020-links-programme/
3. Astbury N, Burgess P, Foster A, et al. Tackling diabetic retinopathy globally through the VISION 2020 LINKS Diabetic Retinopathy Network. Eye News 2017;23(5):30-2.
4. The International Agency for the Prevention of Blindness:
https://www.iapb.org/
5. Beattie A. Knowledge and control in health promotion: a test case for social policy and social theory. In: Gabe J, Calnan M, Bury M (eds). The Sociology of the Health Service. Routledge: London; 1991.
6. The Queen Elizabeth Diamond Jubilee Trust:
https://www.jubileetribute.org/

COMMENTS ARE WELCOME









