A resident’s view from Makassar
My name is Hendra Kusuma, a final year resident (registrar) in the ophthalmology department at Hasanuddin University in Makassar, Indonesia. We have had a VISION 2020 LINK with Dundee (coordinated at the UK end by Dr John Ellis) since 2008 and this year, thanks to our head of department Dr Habibah Muhiddin, I was chosen to spend one month at Ninewells Hospital, Dundee.
When travelling abroad I find it strange that many people seem unable to place Indonesia on the map, despite it being the world’s largest archipelago, the world’s fourth largest nation in population terms (240 million) and a major economy (16th in UN ranking). Makassar, the capital city of South Sulawesi, is the most developed city in Eastern Indonesia and has a population of 1.3 million. Training is split between Wahidin Sudirohusodo Hospital, a government-owned top referral hospital and the university teaching hospital, Hasanuddin University Hospital.
A national survey in 1993-1996 reported the rate of blindness in Indonesia to be 1.5%, which is the figure used by the World Health Organization. A government survey in 2013 reported blindness to be 0.6% but concerns that the methodology was poor were supported when a Rapid Assessment of Avoidable Blindness (RAAB) of over 50s in our region the same year found a prevalence of 2.6%. Major causes of blindness certainly include cataract at perhaps 0.78% and the cataract surgical rate (CSR) has risen above 500 only in the last five years. Blindness in children is also around 0.6% per 1000. These figures appear to be the highest in South East Asia.
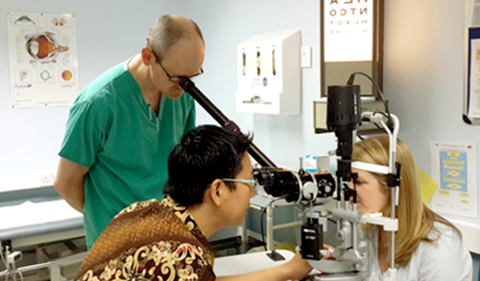
Hendra Kusuma examining a patient in Dundee, watched over by John Ellis.
Through our VISION 2020 LINK, a team from Dundee comes to Makassar for a week once or twice a year, to teach and share skills. Similarly, teams from Makassar visit Dundee for training and observerships. Since the LINK started, 15 people, including three nurses and our Dean and Head of Department, have visited Scotland. It is my observation that things are evolving very fast in our department. A lot of real changes have taken place, including the following:
- When I started, our department had one retinoscope but it was rarely used. The LINK, by bringing out two optometrists, Pamela Robertson and Aileen Buick to Indonesia, taught us how to use one and donated six to the department! Since then, retinoscopy has become a routine part of patient examination. Having optometrists around was a privilege, since there is no equivalent profession in Indonesia.
- The LINK has helped many of our young residents, who have since become permanent members of staff in Makassar, to pursue subspecialties. Now we have consultants in paediatric ophthalmology, vitreoretinal (VR) surgery, neuro-ophthalmology and low vision. Their visits to Dundee have given them exposure and experience in the subspecialities they are passionate about and equipped them to be future leaders. Some have been inspired to take responsibility for districts outside the city of Makassar as the first spearhead in the fight against blindness in Eastern Indonesia. Their time in Dundee has given them a better understanding of systems and the patterns of patient care they will introduce to their districts.
- Retinopathy of prematurity (ROP) screening has been a national priority as part of improvement in neonatal care. National strategies have encouraged ophthalmologists and paediatricians to work together. Although we had already started ROP screening using indirect ophthalmoscopy, the link has helped our department by sending Dr Marliyanti Akib to Dundee to strengthen her skills. Since her return from Dundee, screening ROP in our hospital has become routine and better organised, with residents having a lot more exposure to ROP cases during training. In addition, we have closer relationships with our paediatric department and, with the involvement of the Dundee team, we will improve care together.
- Last year this collaboration resulted in a ‘revolution’ in the structure of referral and care for retinoblastoma (RB) patients in our hospitals. Previously, patients with RB needing chemotherapy were required by our paediatric oncologists to have biopsy evidence of RB prior to treatment. This delayed adjuvant treatment and added the risk of spreading retinoblastoma cells if attempted. The LINK team suggested that we invite Dr Andrew Blaikie, who had experience of treatment of RB in Africa, on one of the LINK visits. We held a symposium involving both the ophthalmology and paediatric departments during the Dundee team visit in December 2013. Dr Blaikie and Dr Andrew Pyott spoke very powerfully about current international standards of RB care in numerous settings. By the end of the meeting there was an agreement between the two departments and the need for biopsy prior to chemo was dropped, provided the diagnosis was agreed by one consultant from each department. It was great to be part of ‘history in the making’!
- Finally, most of our VR surgery was done under general anaesthesia. This can be very risky because patients with diabetes and systemic complications are at high risk. Visits to Dundee showed us that most VR procedures can be performed safely using sub-Tenon’s anaesthesia. Now, half of our procedures are done under sub-Tenon’s block.

(L to R) Drs Blaikie, Ellis and Pyott at the RB symposium in Makassar last December.
During my visit to Dundee in June-July 2014 with a fellow resident, Dr Hasyim Asyari, I saw a lot of things that could make a real difference in our practice. Some of these would be easy and quick to apply:
- In busy outpatient clinics, all staff interact with each other very well. They are polite and respectful to colleagues, consultants, nurses, optometrists and of course to patients. This kind of attitude drives the service and keeps the patient at the centre of their story. The clinicians don’t dictate things to solve the patient’s problems, they work together as a team with the patient and explain every detail and all the treatment possibilities. It’s like saying to the eye patient: “We are on the same side, let’s face this problem together.” This is the kind of relationship I want with my patients in Indonesia.
- In theatre, I saw a nurse whose only job was to hold the patient’s hand through the whole operation, giving comfort and helping the patient relax. This is exactly the model that I want in my district. It is the way I want to treat my patients – as human beings, caring for them not only physically but also psychologically.
- In one of the corridors at Ninewells Hospital, I saw a full length mirror. On top of the mirror, are these words: ‘This is the one that is responsible for your health in the world’. I am going to have one of those in my district very soon!
Other things we admired would be more difficult to introduce in Makassar:
- The learning structure in the UK seems to be like an apprenticeship: one resident to one clinical supervisor and one educational supervisor. In our department we have about 20 consultants but 50 residents, and many of the consultants have duties in other hospitals in Makassar. Indonesia has only about 2,000 ophthalmologists for the whole population and at least half of these live and work in Java.
- An appointment-based service is so nice to see, and the referral system seems to work very well in the UK. In our hospital, patients mostly come to the hospital without scheduling. There are days where we have few patients and others when we are overwhelmed.
- One thing shocked me. Single-use equipment for every single patient, which may be great for patient safety, seems very wasteful to us here in Indonesia. It seems a step too far! With 240 million people in our country, it would be a huge burden to our government to provide single-use equipment for our patients. High volume, high quality and low cost care is what we need.
As a registrar I appreciate the importance of community ophthalmology. It has been my passion to create better systems to ‘reach the unreached’ in my country. The Makassar-Dundee VISION 2020 LINK sponsored me to attend the Global Ophthalmology Day organised by the Royal College of Ophthalmologists on 27 June 2014 in London. It was a humbling and motivating day; truly one of the best meetings I have ever attended. The projects shared and the discussions one-to-one opened my mind and stirred my heart with a picture of what is possible and of what can be achieved by humble people who don’t give up! As Dr Pyott said: “If Africa can achieve so much, with so little resource, we in Indonesia should be able to achieve so much more.”
“We have a deep desire to adopt those parts of best practice we have learned from Dundee at home, to be better doctors who are compassionate with our patients.”
One week per year visiting Makassar by the Dundee team does not seem long enough to teach and improve everything, but by keeping it up for years, it is fair to say that improvements have been felt since this LINK was born. We are now seeing the fruit of a deep friendship. The ‘face’ of our department has changed. Conversely, it may not be enough to learn many things in only a few weeks in Dundee, but it is perfectly long enough to evaluate what we see, to open our minds and to see one of the finest health services in the world. We have a deep desire to adopt those parts of best practice we have learned from Dundee at home, to be better doctors who are compassionate with our patients. The devoted work and friendship of the VISION 2020 Makassar-Dundee LINK has changed us. Someday I will look back and be proud that I was a part of it.
A resident’s view from Dundee
My name is Lai Ling Tan, and I have been fortunate to be one of the registrars involved with the VISION 2020 LINK with Makassar. Dundee’s population is just over a tenth of Makassar’s, though we have responsibility for a population of almost half a million. I worked with a team that included two ophthalmology consultants and two optometrists. We spent a week in 2011 working in Makassar and I returned the following year.
The main objective of the visit in 2011 was to improve skills in refraction amongst the trainee ophthalmologists. The ability to refract is a core skill and essential in paediatric ophthalmology. One week was a short time for a team of five to teach all the trainees in Makassar (there were over 50). It was even more challenging to make sure that all the trainees were competent and comfortable refracting both adults and children. We tried to do so by holding multiple workshops during the day to teach the trainees in groups. However, as teaching times were not protected, a large number of trainees were called away from the teaching to attend to other duties. We therefore held workshops in the evenings to help overcome this.
We also realised that it was important for senior trainees to teach refractive skills to juniors. We identified five senior trainees for this purpose. We helped to develop plans for future workshops led by them. These senior trainees continued this training in Makassar long after we returned to Dundee.
One of the benefits of returning to Makassar a year later was the opportunity to see the positive changes that the LINK had brought to Makassar. It was delightful to see junior trainees refracting well when we returned. This transfer of skills from senior trainees to junior trainees represented a significant shift in the teaching culture at Makassar.

Refraction training workshop for Makassar trainees in 2011,
following the principle of ‘see one, do one, teach one’.
In addition, there was an obvious change in the teaching environment when I returned in 2012. The trainees were significantly less harassed by mobile phones ringing in the middle of a teaching session (phones were used rather than bleeps) and fewer trainees left the teaching sessions halfway through. This change happened only because of the emphasis senior trainees had put onto the junior trainees of the importance of skills development despite having a busy work schedule.
I also observed an improvement in the clinical teaching process in Makassar. Due to the relatively short ophthalmology specialist training there, the trainees who had visited Dundee as part of the LINK were now consultants working in Makassar. Their exposure to the teaching culture here in the UK resulted in them being more actively engaged in postgraduate teaching within a clinical setting. Such a hands-on clinical teaching culture did not seem to be commonplace before the establishment of the LINK.
I have benefited greatly as a trainee ophthalmologist through my involvement in the LINK. I have improved my ability to teach in various settings and had good exposure to diseases not commonly seen in the UK, such as retinoblastoma (new cases presented both weeks I was there, whereas I have never seen a new presentation in the UK). The most important and cherished benefit I have gained, however, is the great friendships with fellow trainees in Makassar. I am grateful to be part of the VISION 2020 LINKS Programme, which empowers ophthalmologists to bring about changes that benefit themselves and their patients.
COMMENTS ARE WELCOME








