Introduction
The Lancet Global Health Commission on Global Eye Health was published in 2021 [1]. Drawing on expertise from within and outside the eye health sector, the Commission set out to:
- inform governments and other stakeholders about the path forward for universal eye health beyond 2020
- further the achievement of the Sustainable Development Goals (SDGs)
- work towards a world without avoidable vision loss.
A team of 73 academics and eye health practitioners from 25 countries worked together to harness lessons learned over the previous two decades and bring together the growing evidence for the life-transforming impact of eye care.
The Commission was co-chaired by Matthew Burton, Director of the International Centre for Eye Health (ICEH) at the London School of Hygiene & Tropical Medicine (LSHTM), and Hannah Faal, Professor of International Eye Health at the University of Calabar, Nigeria.
The Commission builds on the foundations laid by VISION 2020 and the WHO World Report on Vision to provide an evidence base for the future of eye health [2].

Background
Over a billion people are currently living with vision loss that could be prevented or treated with existing cost-effective interventions. Latest estimates show that this is expected to grow to 1.8 billion people by 2050 unless there is significant urgent investment and a coordinated response. Nine in every 10 people living with vision impairment live in low- or middle-income countries (LMICs). There is also gender inequality, with 55% of people living with vision loss being women and girls.
Despite the reduction in age-standardised prevalence of vision impairment observed in the past 20 years, the number of people with vision impairment has risen due to the expanding and ageing global population.
Sustainable Development Goals
The Commission contends that eye health should be part of the mainstream agenda to achieve universal health coverage and sustainable development. With this in mind, it undertook a systematic scoping review of the relationship between improving eye health and advancing the SDGs [3]. It found evidence that the provision of eye health services is associated with improvement in workplace and economic productivity, household consumption and income, and employment. The resulting economic benefits contribute to advancing the SDGs relating to poverty reduction, food security and decent work. In addition, the Commission found evidence that providing spectacles to children improves educational performance, supporting the SDG relating to quality education.
The work of the Commission has successfully brought together and clarified the evidence for the benefits of addressing eye health as part of the mainstream development agenda.
Call to action
The Commission concluded that improving eye health and reducing vision impairment is an important enabler for advancing the delivery of the SDGs. Eye health needs to be reframed as a development issue and needs to be given greater prominence within the global development and health agendas. The Commission emphasised the need to eliminate cost barriers and improve access to quality eye care, particularly in remote areas and for historically underserved population groups. This requires the inclusion of eye health in national health plans, financing structures, workforce development and service delivery at every level of the health system.
An integrated approach to delivery of eye health services
The WHO World Report on Vision published in 2019 had emphasised the need for an integrated, people-centred approach to eye care delivery [2]. Often, eye care has been delivered via vertical programmes, which in many cases have worked well for specific diseases such as trachoma and onchocerciasis, but are inappropriate for treatment of chronic eye diseases such as glaucoma or diabetic retinopathy, which need to be integrated into health systems.
The Commission found that more systematic implementation research is needed to clarify how health systems can advance towards delivering high-quality, integrated, people-centred eye care within universal health coverage.
A first for the United Nations
In 2021 the United Nations (UN) General Assembly adopted its first ever resolution on vision. The resolution has incorporated eye health within the UN’s Sustainable Development Goals (SDGs). Known as Vision for Everyone; accelerating action to achieve the sustainable development goals, the resolution was unanimously passed by the 193 countries of the UN. The work of the Commission provided clear evidence for the role of eye health in achieving the SDGs. Before this, eye health did not feature in any of the 17 Sustainable Development Goals and their 169 targets – recognised by the global eye health community as a disappointing omission. The Commission’s findings of multiple links between eye health and several of the SDGs provided a compelling case for its inclusion.
The resolution sets targets for ‘vision for everyone’ by 2030, calling for countries to ensure full access to eye care services and to make eye health integral to the UN’s commitments to achieving the Sustainable Development Goals.
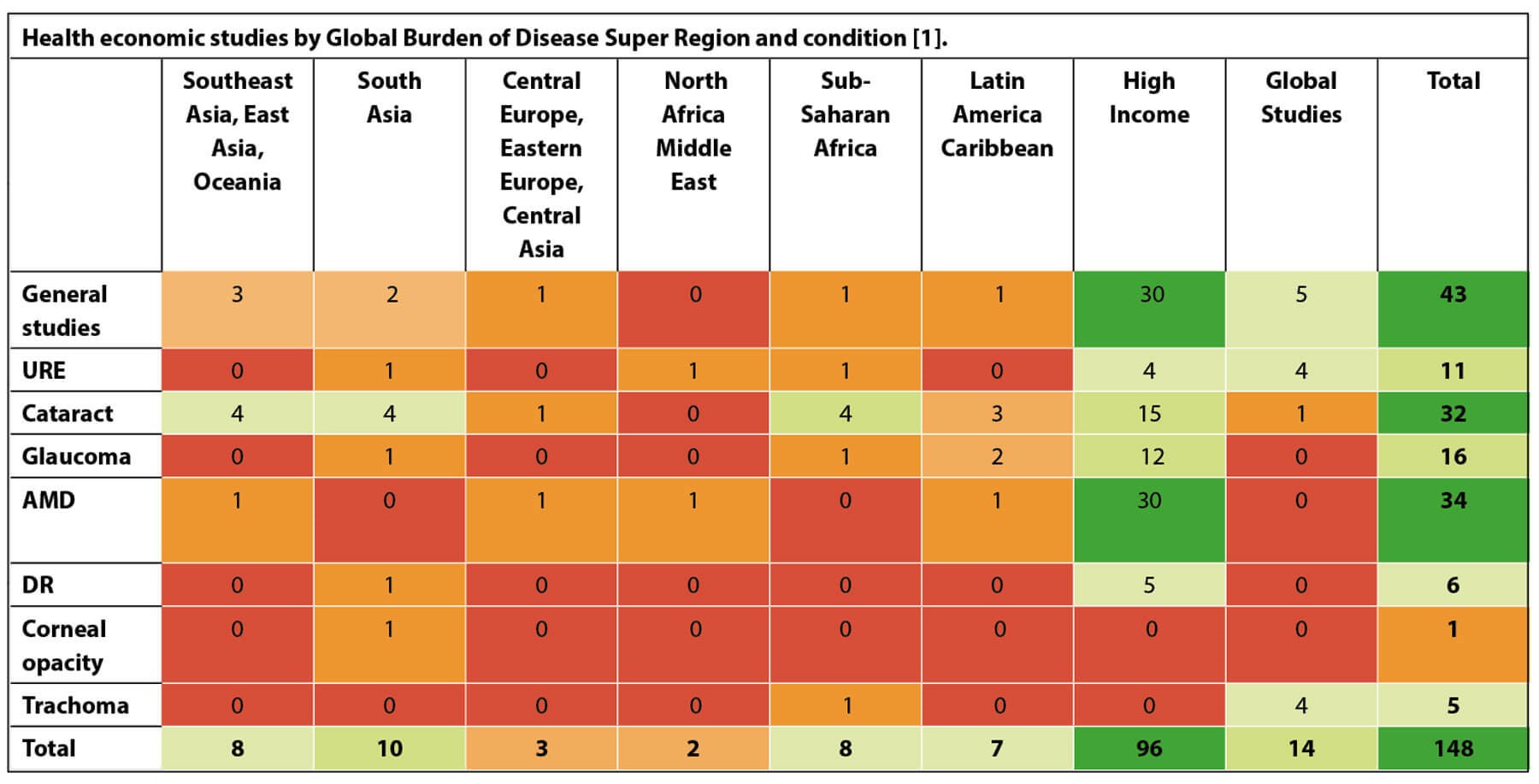
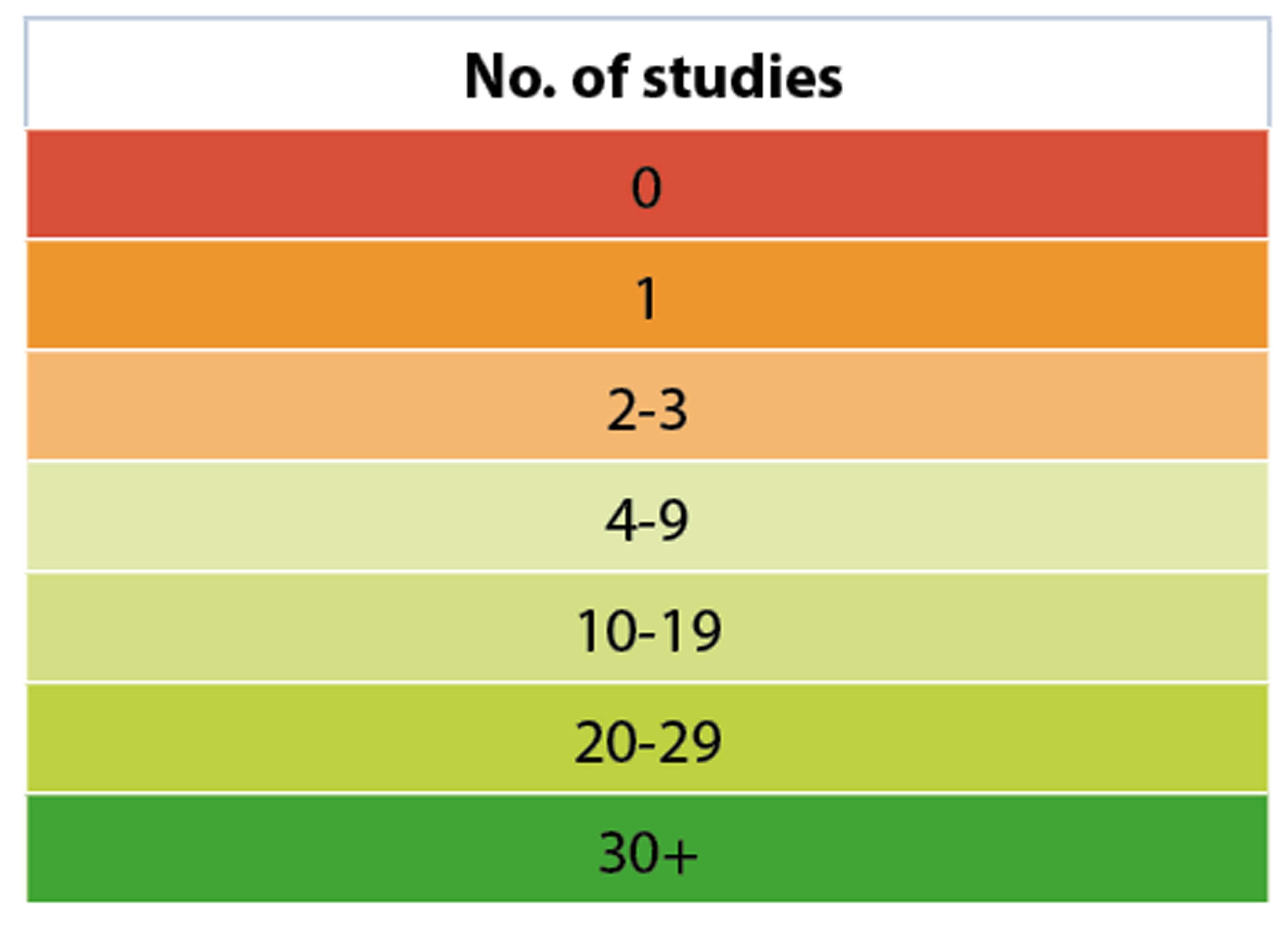
NOTE: Several studies report data from multiple regions. The Commission’s authors recorded the different regions separately, therefore the total of region-specific reports exceeds the total number of studies in the systematic review.
The economic impact of vision loss
When the Commission undertook a systematic literature review of studies on the economic costs of vision impairment over the last 20 years, it found that there is very little data from LMICs. The literature that is available globally has multiple limitations and leaves huge gaps in knowledge. This exercise highlighted for the first time the scarcity of high-quality data for the economic impact of blindness and vision impairment in LMICs. It recognised that previous estimates for the economic impact of vision impairment may have been substantially over- or underestimated, potentially leading to flawed policy decisions.
The Commission carried out a new analysis of global annual productivity loss caused by vision impairment in people of working age. It found that the economic cost of blindness and moderate to severe vision loss was 411 billion USD per year. Treatment for cataract and refractive error would meet 90% of unmet needs and are highly cost-effective [4].
The findings highlight the importance of unlocking human potential by addressing avoidable vision impairment and providing rehabilitation services for people whose sight cannot be restored.
Grand Challenges in Global Eye Health
The Commission ran a ‘Grand Challenges in Global Eye Health’ prioritisation exercise to identify crucial issues still to be addressed and highlight key areas for concerted research and action. Over 300 people from 118 countries were involved. They contributed 3400 responses, which were thematically analysed and consolidated into 85 unique challenges [5].
Ranking was done across two further rounds to arrive at 16 priority challenges, which fell within four broad themes:
- improve detection and treatment (condition-specific)
- strengthen the health system
- increase access and equity
- build human resource capacity.
Within the challenges relating to improving treatment, the key conditions were refractive error, cataract, child eye health, glaucoma and diabetic retinopathy.
The results provide a clear direction of travel for eye health researchers and service providers. The aim is that different groups will galvanise around specific challenges; the work of ICEH is well aligned to develop and support many of them.
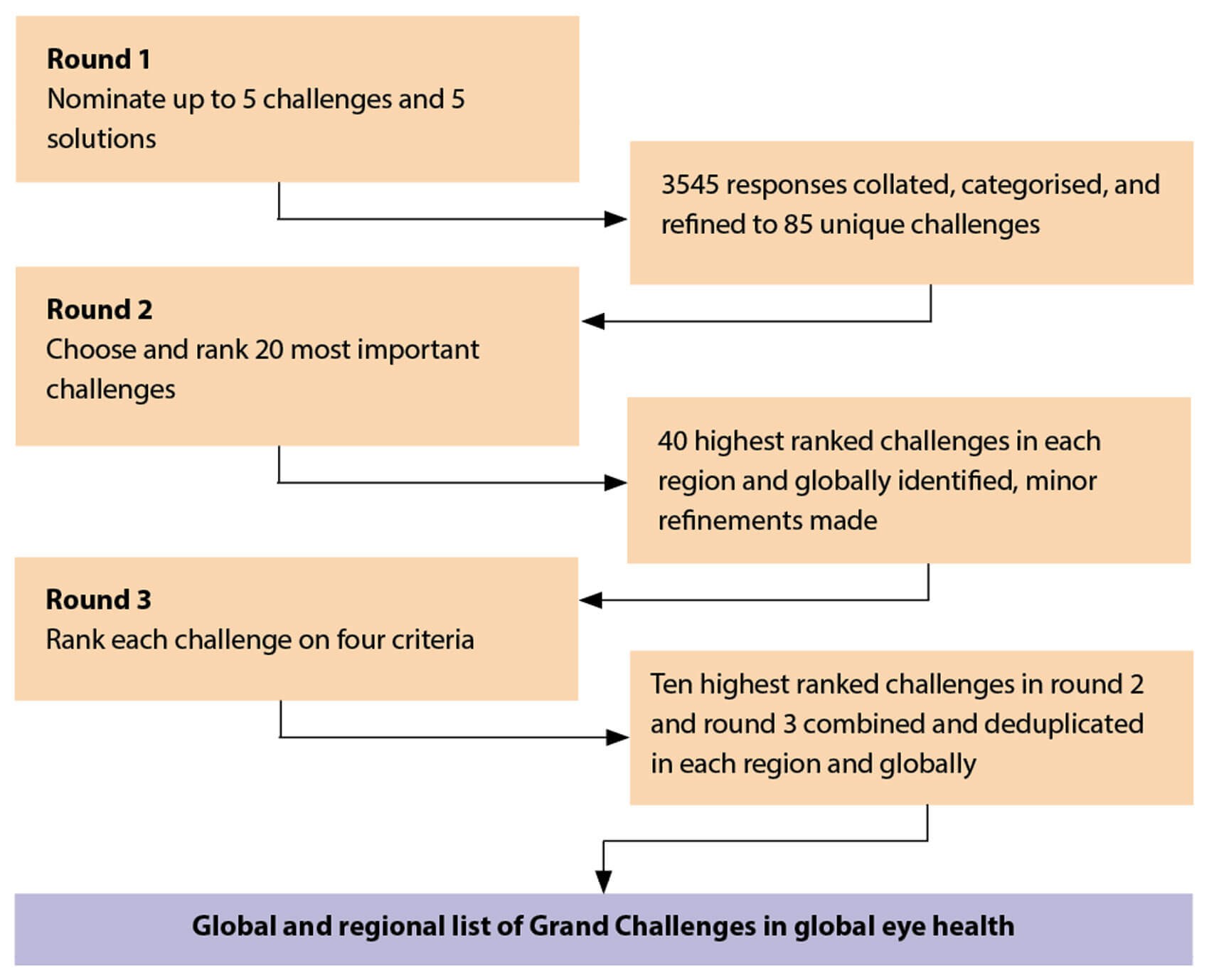
Diagram to show the process followed by the Grand Challenges [5].
Summary
The systematic analyses carried out by the Commission, and the novel research undertaken, shed new light on the shift from infectious eye diseases as a cause of vision impairment towards the greater contribution of chronic eye diseases, and the consequent need for a refocused public health and clinical response.
The need for greater integration of eye health care within primary health and prevention strategies is widely recognised. High-quality evidence, together with discovery research and implementation research, is needed to guide more effective implementation at scale. Expanding the eye health workforce, providing high-quality training and then distributing trained workers according to population need are all crucial.
The Lancet Global Health Commission on Global Eye Health is a clear call to action for the essential role of eye health in achieving universal health coverage and sustainable development.
References
1. Burton MJ, Ramke J, Marques AP, et al. The Lancet Global Health Commission on Global Eye Health: vision beyond 2020. Lancet Glob Health 2021;9(4):e489-e551.
2. World Report on Vision – World Health Organization.
https://www.who.int/docs/default-source/
documents/publications/
world-vision-report-accessible.pdf
Last accessed June 2022.
3. Zhang JH, Ramke J, Jan C, et al. Advancing the Sustainable Development Goals through improving eye health: a scoping review. Lancet Planet Health 2022;6(3):e270-e280.
4. Marques A, Ramke J, Cairns J, et al. Global economic productivity losses from vision impairment and blindess. EClinicalMedicine 2021;35:100852.
5. Ramke J, Evans JR, Habtamu E, et al. Grand Challenges in global eye health: a global prioritisation process using Delphi method. Lancet Healthy Longev. 2022;3(1):e31-e41.
Full copies of the Commission report are available on request from Hugh Bassett at the International Centre for Eye Health by emailing hugh.bassett@lshtm.ac.uk, or see https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30488-5/fulltext
COMMENTS ARE WELCOME