The Royal College of Ophthalmology of Eastern, Central and Southern Africa (COECSA) and the Royal College of Ophthalmologists (the Royal College) have had a successful VISION 2020 LINK partnership for over 12 years. The partnership was established by the VISION 2020 LINKS Programme, which is part of the International Centre for Eye Health (ICEH), London School of Hygiene & Tropical Medicine (LSHTM).
Following a request to the VISION 2020 LINKS Programme from Dr Fredrick Korir, Chair of the Ophthalmological Society of Kenya, and from other COECSA African LINK partners, an online open-access webinar was convened on 9 April 2020. The aim was to discuss COVID-19 and ophthalmology, with a focus on eye care units in African countries, with shared learning from the UK situation.
Co-hosted by the Royal College, ICEH and COECSA, the session featured presentations by the Presidents of both Colleges: Mr Mike Burdon and Dr John Nkurikiye. They spoke of the high transmission risk posed by close contact specialties like ophthalmology, and the importance of tailoring responses to each country: bearing in mind the severity of the pandemic in each region, and the differently structured healthcare systems. Mr Victor Hu from the ICEH, who is also based in UK ophthalmology departments and a LINK partner, spoke about ways to modify ophthalmic practice, to protect patients and staff. Simple measures – such as hand washing, 2m distancing, and covering mouths when coughing – are to be encouraged across all contexts. Strategies discussed include postponing all face-to-face outpatient activity unless urgent, and which factors would push clinicians in favour of seeing a patient (e.g. only one seeing eye) versus against (vulnerable patients).
Triaging, hygiene measures and optimal personal protective equipment (PPE) were also covered, by Dr Elanor Watts. The stratified approach to PPE was discussed, in which low-risk settings employ surgical masks and disposable aprons, and high-risk settings (e.g. those where aerosol-generating procedures are undertaken) warrant more intensive PPE – filtering facepiece (FFP3) respirators and fluid-resistant gowns. Gloves and eye / face protection are recommended throughout.
However, an important topic in the webinar was that of adapting these guidelines to settings with different resources. Although PPE would ideally always be purchased from suppliers with guaranteed quality, this may not always be possible. Options in crisis include using homemade items, such as slit lamp guards, face visors and hand gel, or decontaminating and re-using some items, e.g. goggles. Mrs Archana Kulkarni from Warwick reviewed options for modifying paediatric ophthalmic practice.
The specific situations in Nigeria, Kenya and The Gambia and their successful response strategies were presented. Prof Adeola Onakoya described how, in Lagos, clinical services were significantly scaled down at the end of March following a surge in cases. PPE and hygiene measures were strictly enacted, and patients’ temperatures checked before entering the clinics, to reduce transmission from incoming patients. These had successfully prevented COVID-19 transmission in Lagos eye clinics.
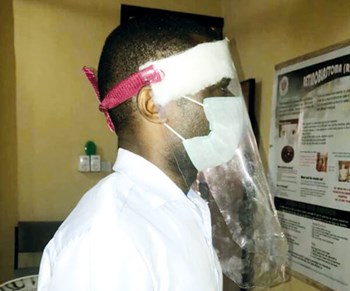
Homemade visor, UITH Ilorin Nigeria.
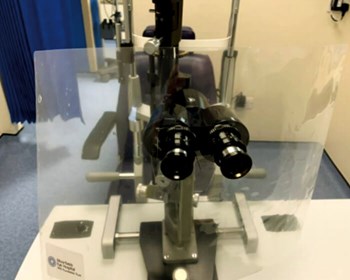
Slit lamp guard, RCOphth.
Kenya’s guidelines were reviewed by Dr Fredrick Korir, including the role of telemedicine. The economic impact of reduced services was raised. Meeting essential costs of private clinics, including staff wages and rent, is exceedingly difficult during this time. Finding solutions to enable clinics to fully re-open following the pandemic is a high priority for long-term vision service provision.
Dr Abba Hydara described how, in The Gambia, mandatory patient handwashing was instigated, slit lamp examinations avoided completely, and only urgent and emergency patients seen. Examples of urgent cases included patients with newly diagnosed diabetic retinopathy or advanced glaucoma, and children with congenital / developmental cataracts, while examples of emergency cases included sudden loss of vision, and paediatric leukocoria. Non-essential staff were sent home.
The disruption to training resulting from these changes was also discussed, specifically in the contexts of Rwanda (Dr Ciku Mathenge) and the UK (Miss Melanie Corbett). Rwandan trainees had to return from their electives and remain at home during lockdown, so instead received online didactic training and tests. In the UK, many ophthalmology trainees were re-deployed to medical wards, and so a similar tele-teaching approach has been used. COECSA leads and senior faculty were invited to remotely attend a Royal College advanced ‘Training the Trainers’ course at the end of April, focussing on tele-teaching. The potential for the UK and the COECSA regions to each learn from the other was highlighted.
The webinar concluded with a question and answer session, mediated by Mr Will Dean.
Over 270 participants attended the webinar, and feedback has been very positive. A recording is available online:
There are plans for another session in the near future to continue international knowledge sharing as the pandemic situation evolves.
COMMENTS ARE WELCOME











