This article follows the Correspondent News articles in the previous five print issues of Eye News [1-5] on the VISION 2020 LINKS Programme [6]. This article describes how African and UK eye care teams are working together to tackle childhood blindness in Africa.
Childhood blindness – causes and magnitude
Childhood blindness is a priority in ‘VISION 2020: The Right to Sight’, and childhood cataract is the leading cause of treatable childhood blindness in sub-Saharan Africa. In 2010 the World Health Organization (WHO) estimated that there were 1.5 million children blind worldwide [7]. It has been estimated that at least 30%, and in some situations up to 70%, of childhood blindness is avoidable [8]. The priority conditions identified for control are corneal scarring, cataract, retinopathy of prematurity, refractive error (mostly myopia) and low vision [8].
The control of blindness in children is a VISION 2020 priority because, although the number of blind children is relatively low, they have a lifetime of blindness ahead, with an estimated 75 million blind-years, which is second only to cataract globally [9]. If VISION 2020 targets for children can be met, the global prevalence of blindness will have fallen from 7.5 per 10,000 children in 1997 to four per 10,000 children by the year 2020. The number of children worldwide who are blind will reduce to approximately 800,000 [10].
Childhood blindness poses different challenges to adult blindness. Children’s visual systems develop during their early years and they need to see clear images in order for normal visual maturation to occur. Failure of this process (i.e. amblyopia) cannot be corrected in adults, so treatment of childhood visual loss and blindness has a defined timeframe beyond which interventions have a limited impact.
Assessing children’s vision and examining children’s eyes requires specialist skills and training. In Africa, there are very few training programmes for orthoptists and limited practical training in paediatric ophthalmology for ophthalmologists and other cadres. Assessing vision and examining the eyes of children requires time and experience on the part of the examiner. There can be a tendency to consider children as smaller versions of adults, and children’s eyes as smaller versions of adult eyes, when in fact they respond differently and require very specific approaches [11]. Other important issues are the need for training in safe anaesthesia for children and the need for appropriate equipment and consumables.
VISION 2020 LINKS are making major strides in addressing the need for whole-team training in paediatric eye care through regular, repeat visits to share specialist skills between counterparts (ophthalmologists, nurses and allied health professionals) in the UK and Africa.
Addressing the problem
The WHO recommends the establishment of one fully functioning Paediatric Eye Centre per 10 million population, with the appropriate skills and equipment to provide tertiary-level children’s eye care services. In some of the African countries with smaller populations, this would be one main centre for the whole country (e.g. Blantyre in Malawi, Harare in Zimbabwe). In theory, in Tanzania it would be five centres and in Nigeria it would be 17. In practice, while this sounds a logical approach, actually achieving it is very challenging, given the pressure on Ministry of Health and non-government organisation (NGO) funding across sub-Saharan Africa and the shortage of trained ophthalmologists and other cadres. Also, the picture is complicated by the distribution of the population, which is not evenly distributed across countries and is predominantly rural, and the distribution of ophthalmologists, which is invariably centred on the capital city and other urban centres.
When asked to choose the priority areas for training support, many of the VISION 2020 LINK partner institutions chose paediatric ophthalmology. To date, 17 LINKS in 13 countries across Africa have chosen paediatric ophthalmology as a priority for their institution and their VISION 2020 LINK. The VISION 2020 LINKS that have chosen paediatric ophthalmology as one of their priorities are shown in the table. Each has been matched with a UK partner eye department keen to work on developing children’s eye services and able to provide the necessary expertise from within their team. (See following table.)
Country: Uganda
VISION 2020 LINK: Mulago-Royal Free
African partner institution: Mulago Hospital/Makerere University
UK partner institution: Royal Free Hospital
UK LINK Coordinator: Clare Davey
Country: Uganda
VISION 2020 LINK: Mbarara-Bristol
African partner institution: Mbarara Hospital/Ruharo
UK partner institution: University Hospitals Bristol
UK LINK Coordinator: Derek Tole
Country: Tanzania
VISION 2020 LINK: Muhimbili-STH
African partner institution: Muhimbili University of Health and Allied Sciences
UK partner institution: St Thomas’ Hospital
UK LINK Coordinator: Denise Mabey
Country: Tanzania
VISION 2020 LINK: KCMC-Birmingham
African partner institution: KCMC, Moshi
UK partner institution: University Hospitals Birmingham
UK LINK Coordinator: Victor Hu
Country: Tanzania
VISION 2020 LINK: Mbeya-N Cumbria-WHSCT
African partner institution: Mbeya Referral Hospital
UK partner institution: Western Health and Social Care Trust, N Ireland
UK LINK Coordinator: Rosie Brennan
Country: Ethiopia
VISION 2020 LINK: Addis-Bucks
African partner institution: Menelik II Hospital
UK partner institution: Bucks Healthcare
UK LINK Coordinator: Bandu Jayaratne
Country: Ethiopia
VISION 2020 LINK: Yirgalem-N Wales
African partner institution: Yirgalem and Hawassa Hospitals
UK partner institution: Betsi Cadwaladar, Abergele
UK LINK Coordinator: Claire Morton
Country: Malawi
VISION 2020 LINK: Blantyre-Glasgow
African partner institution: Queen Elizabeth Central Hospital, Blantyre
UK partner institution: Royal Hospital for Sick Children, Yorkhill
UK LINK Coordinator: Tim Lavy
Country: Madagsacar
VISION 2020 LINK: Madagascar-Leeds
African partner institution: MoH Hospitals and SALFA
UK partner institution: Leeds Teaching Hospitals
UK LINK Coordinator: Andy Cassels-Brown
Country: Zimbabwe
VISION 2020 LINK: Harare-Barts
African partner institution: University of Zimbabwe College of Health Sciences
UK partner institution: Barts Health
UK LINK Coordinator: Ashwin Reddy
Country: Swaziland
VISION 2020 LINK: Swaziland-SPROG
African partner institution: Good Shepherd Hospital, Siteki
UK partner institution: Scottish Paed Ophth Group
UK LINK Coordinator: SPROG/Tim Lavy
Country: Botswana
VISION 2020 LINK: Botswana-Addenbrooke’s
African partner institution: Ministry of Health Botswana
UK partner institution: Addenbrooke’s Hospital, Cambridge
UK LINK Coordinator: Malcolm Kerr-Muir
Country: Zambia
VISION 2020 LINK: Lusaka-Brighton
African partner institution: UTH, Lusaka
UK partner institution: Brighton and Sussex University Hospitals
UK LINK Coordinator: Joy White
Country: Zambia
VISION 2020 LINK: Kitwe-Frimley Park
African partner institution: Kitwe Central Hospital
UK partner institution: Frimley Park Hospital
UK LINK Coordinator: Andrew Elliott
Country: Nigeria
VISION 2020 LINK: Lagos-Bolton
African partner institution: Lagos University Teaching Hospital
UK partner institution: Royal Bolton Hospital
UK LINK Coordinator: Clare Inkster
Country: Ghana
VISION 2020 LINK: Moorfields-Korle Bu
African partner institution: Korle Bu Teaching Hospital
UK partner institution: Moorfields Eye Hospital
UK LINK Coordinator: Ian Murdoch
Country: The Gambia
VISION 2020 LINK: The Gambia-Swansea
African partner institution: Sheikh Zayed Regional Eye Care Centre (SZRECC)
UK partner institution: Singleton Hospital, Swansea
UK LINK Coordinator: David Laws, Stella Elliott
Examples of how VISION 2020 LINKS are helping to develop children’s services in Africa are shown in boxes 1-4 below. Skill transfer and training includes surgical and theatre nurse skills, visual acuity assessment in children by eye nurses and optometrists, safe anaesthesia for children, developing child-friendly waiting and play areas, and, in some cases, donating equipment, instruments and consumables.
Box 1: Impact of VISION 2020 LINK between Blantyre and Glasgow
During 2010, 121 cataract surgeries and 89 other surgeries were performed at Lions SightFirst Eye Unit, Queen Elizabeth Central Hospital, Blantyre, Malawi. In 2012, 4,806 children were seen in the unit, 190 cataract surgeries were carried out and 262 other surgeries were carried out successfully at the unit. This represents a 157% increase in childhood cataract surgeries, and a nearly three-fold increase in other surgeries on children’s eyes over two years. This highlights the very real difference a VISION 2020 LINK makes.
Gerald Msukwa, Paediatric Ophthalmologist, Blantyre, Malawi.
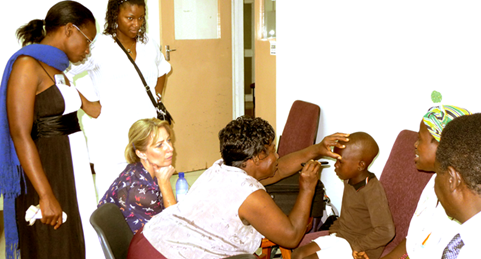
Training in children’s vision assessment through the VISION 2020 LINK between Blantyre and Glasgow.
Box 2: Development of paediatric cataract services in Swaziland through a LINK
A link was forged between Good Shepherd Hospital in Swaziland and Glasgow and in 2003 a team stepped onto Southern African soil, blinking in the fierce heat. Comprised of a paediatric ophthalmologist, an anaesthetist and anaesthetic assistant and two scrub nurses, they had one week to start to pass on their skills.
Twelve children had been booked for surgery but, on the day, only seven showed up. One of them was Sihle, a two-week-old boy, with bilateral micro-ophthalmia and congenital cataracts. His parents were very anxious, as was David the anaesthetist who would have to use the untested equipment on such a young child.
Tim Lavy did that first surgery, with me assisting. After operating on one eye, we rescrubbed and I did the other in line with the old adage ‘Watch one, do one’. Surgery went as well as it could and David was able to establish procedures for neonatal anaesthesia. He left behind a bag of laryngeal masks and a well-trained anaesthetic team. The other paediatric surgeries that week were squints and probing of canaliculi.
Following the second visit of Tim and David, we decided that the incidence of paediatric cataracts was inadequate for learning the procedure, and arranged a one-month mini-fellowship for me at CCBRT in Dar es Salaam, Tanzania. At that paediatric unit, the numbers were high and allowed for rapid assimilation of the techniques.
Fast-forward 10 years, and those same procedures are now routine at Good Shepherd, with at least 40 surgeries per year. Sihle is now 10 and, though he has glaucoma, he has useful vision and attends a normal school. The skills needed for paediatric ophthalmology have been successfully transferred!
Dr Jonathan Pons, Ophthalmologist at Good Shepherd Hospital in Siteki, Swaziland. In 2003 he was the only ophthalmologist in Swaziland, serving the population of a million people. There is now a second ophthalmologist.
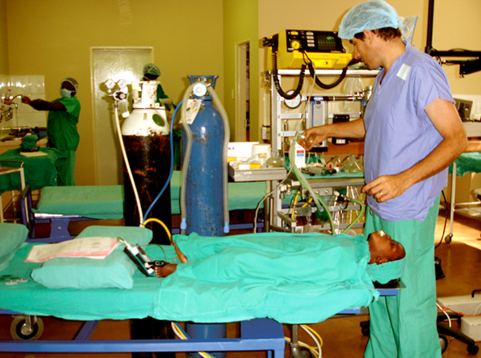
Dr Jonathan Pons, Ophthalmologist in Swaziland, with a child patient.
Box 3: Improving children’s eye care in Nigeria through a VISION 2020 LINK
“We benefited from our LINK with Altnagelvin Hospital, N. Ireland, led by Paediatric Ophthalmologist Rosie Brennan, as follows:
a) Dramatic improvement in our general anaesthetic procedures and standards for children. Conversion from endotracheal intubation to laryngeal mask has made anaesthesia for this group easier and almost risk free. We have not lost any child to anaesthesia since then.
b) Paediatric visual acuity assessment has improved greatly, alongside refraction for children. Glasses prescription for children and management of amblyopia improved through the LINK.
c) Intraocular lens calculation for both children and adults. This has improved the outcome of cataract surgery for both groups.
d) Theatre management – we had an upgrade in our aseptic procedures. Improved sterilisation and theatre procedures, backed up by donation of sterilisation equipment.
e) Biomedical engineering revived a number of items of equipment that were out of use before the LINK started. Our technician was taught how to maintain these machines.
The LINK helped us to step up the standards of our services in all areas of practice for children and adults, including glaucoma and general ophthalmology.”
Dr Abuh Sunday Omogani, Paediatric Ophthalmologist, ECWA Eye Hospital.
“In the past, children who came to our hospital for eye care had their sight checked using adult vision checking materials. But through the VISION 2020 LINK with Altnagelvin, N. Ireland, I have been well trained and equipped with children’s vision testing materials. Now, specific visual problems commonly found in children like refractive errors, amblyopia, strabismus and retinoblastoma are identified early and well managed. Paediatric cataract patients now have proper calculation of their intraocular lens prior to surgery with the result being improvement of surgical outcome. There is an appreciable increase in our paediatric patients, because our new and improved way of caring has given rise to a nationwide referral to our hospital. The understanding gained and knowledge applied in my care given to patients now in comparison with the previous practice makes a sharp difference, like moving from night to daylight.”
Thomas Achi, Paediatric Orthoptic Nurse, ECWA Eye Hospital, Kano, Nigeria.
ECWA is linked with WHSCT, Altnagelvin, N. Ireland. Sadly, the difficult situation in northern Nigeria has meant that this LINK cannot progress for the time being, but the skills shared continue to be used.
Box 4: Example of retinoblastoma success
“I have just finished surgery and fitted a prosthesis in a five-month-old child with retinoblastoma – since the campaign when Ashwin Reddy and team from Barts were here the family has come forward and agreed to surgery. We were so pleased that the father of the child agreed to have this done! This child has every hope of living now.”
Mayuri Patel, Ophthalmologist at Parirenyatwa Hospital, Harare, Zimbabwe.
Two of the specialist areas where progress is being made through LINKS, paediatric cataract and retinoblastoma, are described below.
Paediatric cataract
Paediatric ophthalmologists remove cataracts and insert intraocular lenses (IOLs) into the eyes of babies and young children. This technique requires considerably more expertise than adult cataract. It also requires access to a vitrectomy machine, as the posterior capsule and anterior vitreous have to be removed [10]. However, few eye departments in Africa have a vitrector. Community health workers need to be aware of the signs and symptoms of cataract in babies and children. Referral pathways from the community to tertiary centres are challenging in developing countries, with poor infrastructure and communications, and the cost of travel may be prohibitive for families. Long-term follow-up is also crucial, to manage visual correction and offer low vision devices.
Tim Lavy, Paediatric Ophthalmologist, describes the development of the VISION 2020 LINK between Blantyre, Malawi and the Royal Hospital for Sick Children, Glasgow: “The link between the Royal Hospital for Sick Children in Glasgow and Lions SightFirst Eye Hospital in Blantyre, Malawi has been running for six years. In that time we have selected and trained Malawi’s first paediatric ophthalmologist, set up a national referral unit, and have gone on to provide specialist paediatric training to over 40 ophthalmic clinical officers (OCOs) and optometrists across the whole country.
In the early days, we took an anaesthetist with us, allowing us to carry out theatre lists without putting pressure on the Blantyre anaesthetic department, which was always very stretched. At that time we were trying to teach Dr Gerald Msukwa as much paediatric ophthalmology as we could in two weeks each year, as well as train the local OCOs in Blantyre in measuring and recording visual acuity in children.
However, after the first year, Dr Msukwa acquired sponsorship to go to Tanzania for specialist training in Dar es Salaam. This fellowship at CCBRT Hospital gives intensive training ‘on the job’ for African ophthalmologists in an African setting on African patients. The advantages of this over any sort of training that might be possible in the UK cannot be overemphasised. In our case it was particularly opportune as I independently managed to obtain a year’s leave from Glasgow to work at CCBRT, coinciding with Gerald’s fellowship. This gave us much time to develop a close working relationship and share our visions for paediatric ophthalmology in Malawi.
Having completed his fellowship in Tanzania, Gerald now runs his national referral unit (Child Eye Health Tertiary Facility) in Blantyre and the visiting team from Glasgow helps him to provide a training course annually to spread the word about paediatric ophthalmology and the referral process across Malawi. Direct involvement in delivery of clinical care by the Glasgow team has therefore moved on to a wider training role disseminating information across the country. We see this is as a crucial step towards maturity of the service in Malawi.
In the next three years we plan to complete our paediatric training of all the current OCOs in the country and get the course inserted into core training for all future OCOs, thus giving Glasgow an exit strategy. During the six years there have been visits to the UK for Gerald, some OCOs from his unit in Blantyre, theatre nursing staff and one anaesthetist. Additionally, Gerald and I have presented at the Royal College of Ophthalmologists Annual Congress, the World Ophthalmology Congress and international retinoblastoma meetings. This achievement has been made possible through five years of grant funding from the Scottish Government, with additional support from Christian Blind Mission (CBM), and the VISION 2020 LINKS Programme at London School of Hygiene and Tropical Medicine (LSHTM).
I have learnt that it is important for both sides to keep re-examining the activity of the LINK and not be afraid to alter things in the light of what works or doesn’t work. The UK partner particularly needs to keep a sense of proportion in order to avoid disappointment if unrealistic dreams have not been possible. Ultimately, personal relationships are extremely important and establishing these long-term might be just as valuable as anything else. The longer a link is going the more the partners understand about each other and the more you realise how little you knew (about anything) at the beginning. Overcoming unforeseen difficulties together without a script is what builds the team’s confidence and enthusiasm. I have thoroughly enjoyed being part of our LINK and look forward to the next three years (funders / sponsors willing)!”
Retinoblastoma
Retinoblastoma (Rb) causes much unnecessary suffering to children and their families in Africa. There are about 2,000 known new cases each year in Africa [12]. The tertiary eye units in Africa have a constant influx of children presenting with advanced Rb on their wards and the ophthalmologists are frustrated at being unable to do anything to save their lives.
Currently, lack of public awareness and health worker awareness means children are not diagnosed early enough to be cured. When they eventually reach tertiary centres, lack of accurate pathology leads to under- or over-treatment, poor application of limited resources and unnecessary family burdens. Chance of survival in Africa is little above zero [13], whereas in the UK, where the necessary systems are in place, more than 95% of children are cured [14].
Public awareness and accurate pathology are key to tackling Rb. Raising awareness of the early signs of Rb (white pupil and squint) amongst health workers and the public is essential so that babies and children are recognised and treated early, while it is still curable. A health worker and public awareness campaign highlighting white pupil and squint as early signs of Rb will also pick up cases of treatable childhood blindness such as cataract, which also presents with a white pupil. This will help to reduce unnecessary blindness in children due to cataract, decreasing the number of ‘blind-years’ for children, a priority in National Prevention of Blindness Plans.
Accurate pathology of removed eyes quickly identifies children who have been cured by surgery alone, and curable children who require postoperative chemotherapy to reduce risk of their cancer returning. Mortality from Rb correlates with stage of cancer at diagnosis, and spread beyond the eyeball increases risk of death substantially [15]. Honduras is one of the few countries to measure the impact of a Rb public awareness campaign in the developing world. The study compared children presenting to hospital before and after an annual public awareness campaign about Rb, linked to the national immunisation programme. During the two years after the campaign, 35% of children had disease that had spread outside the eye at diagnosis, compared with 73% in the previous eight years. The Honduran study highlights the importance of accurate pathology, not just in informing postoperative care for each child but also for assessing impact of an awareness campaign [16].
The VISION 2020 LINKS Programme has built key alliances to tackle the problem of Rb in Africa. Some LINK leads have attended meetings of the Kenya National Retinoblastoma Strategy (KNRbS) group. This group, supported by Daisy’s Eye Cancer Fund (DECF), has led the way in establishing standardised pathology protocols and management guidelines for Kenya, based on experience in Canada (with specialist input from Brenda Gallie of Sick Kids, Toronto). The KNRbS group includes medical professionals, parents and survivors, health advocates and community and government leaders. The KNRbS Group is happy to share its expertise with other countries and the VISION 2020 LINKS Programme hopes to use its experience to help the paediatric LINKS to tackle Rb.
What is needed for retinoblastoma?
The VISION 2020 LINKS Programme is currently looking for substantial funding for the paediatric LINKS that are keen to develop national Rb strategies and awareness programmes. Raised awareness amongst health workers and in the community is essential. Standardised protocols and infrastructure (covering specialist pathology, artificial eyes and implants, record-keeping and patient database, patient and family support) are too. Together, these will result in more children coming forward earlier and hence curable through surgery, and the integration of pathology, oncology and ophthalmo logy services will result in better quality treatment. The VISION 2020 LINKS Programme is seeking funding partners who share our goal of saving sight, and lives, through early diagnosis and effective treatment of Rb in Africa.
References
1. Zondervan M, Walker C, Astbury N. VISION 2020 Links Programme: building capacity for eye care internationally. Eye News 2013;19(5):34-9.
2. Walker C, Zondervan M, Astbury N. VISION 2020 Links Programme: building capacity in Eastern Africa. Eye News 2013;19(6):48-50.
3. Astbury N, Zondervan M, Walker C. VISION 2020 LINKS Programme: raising standards in Eastern, Central and Southern Africa. Eye News 2013;20(1):46-8.
4. Walker C, Oyewole K, Zondervan M. Building capacity in West Africa: the Moorfields-Korle Bu VISION 2020 LINK. Eye News 2013;20(2):11-4.
5. Subramani S, Okoronkwo A, Robinson J, et al. Developing leadership for eye care in Nigeria: the Lagos-Bolton-North Western Deanery VISION 2020 LINK. Eye News 2013;20(3):28-33.
6. VISION 2020 LINKS Programme:
http://iceh.lshtm.ac.uk
7. Mariotti S. Global data on visual impairments 2010. World Health Organization; 2012:
http://www.who.int/
blindness/GLOBALDATAFINALforweb.pdf
8. Gilbert C, Rahi J, West K Jr, et al. Visual Impairment and Blindness in Children. In The Epidemiology of Eye Disease, 3rd Edition. Edited by Johnson GJ, et al. London: Imperial College Press; 2012.
9. Childhood Blindness, IAPB:
http://www.iapb.org/
vision-2020/what-is-avoidable-
blindness/childhood-blindness
10. Gilbert C, Muhit M. Twenty years of childhood blindness: what have we learnt? Comm Eye Health J 2008;21(67):46-7.
11. Gilbert C, Foster A. Childhood blindness in the context of VISION 2020: The Right to Sight. Bull World Health Organ 2001;79(3):227-32.
http://www.who.int/
bulletin/archives/79%283%29227.pdf
12. Daisy’s Eye Cancer Fund:
www.daisyfund.org/
programs/rati/today.html
13. Gallie BL, Zhao J, Vandezande K, et al. Global issues and opportunities for optimized retinoblastoma care. Pediatr Blood Cancer 2007;49(7):1083-90.
14. MacCarthy A, Birch JM, Draper GJ, et al. Retinoblastoma: treatment and survival in Great Britain 1963 to 2002. Br J Ophthalmol 2009;93(1):38-9.
15. Navo E, Teplisky D, Albero R, et al. Clinical presentation of retinoblastoma in a middle-income country. J Pediatr Hematol Oncol 2012;34(3):e97-101.
16. Leander C, Fu CL, Pena A, et al. Impact of an education program on late diagnosis of retinoblastoma in Honduras. Pediatr Blood Cancer 2007;49(6):817-9.
COMMENTS ARE WELCOME