Orthoptists see a wide range of conditions that can range from reduced binocular single vision (BSV) that may be solved with exercises, to more extreme neurogenic cases requiring further intervention. Because of this variety, it is important to be able to know when further investigation is needed.
Many orthoptic conditions can present similarly in clinic and can cause distress when a health professional feels unable to confidently diagnose a patient and as a result, cannot determine the aetiology. That fear of missing something important may cause the health professional to order a surplus of tests, many of which may be invasive, distressing and completely unnecessary. This article will discuss the differential diagnosis of two common orthoptic conditions, and contribute to the avoidance of unnecessary examinations and provide timely and accurate diagnosis.
While both a sixth nerve palsy (VI np) and a decompensating distance esophoria (DDE) may present similarly in clinic, there are some key features that will help differentiate between the two.
“The patient’s history can give you major clues as to what the diagnosis is likely to be”
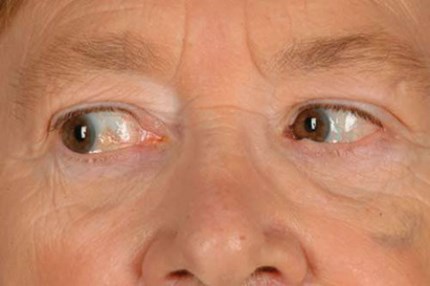
Figure 1: Left VI cranial nerve palsy, patient looking right.
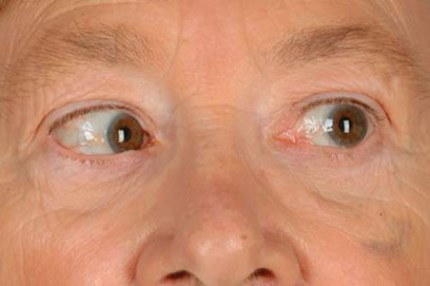
Figure 2: Left VI cranial nerve palsy, patient looking left (note subtle limitation of abduction).
Case history
The patient’s history can give you major clues as to what the diagnosis is likely to be. While both may present with horizontal double vision in the distance, a VI np is also likely to cause further separation of the two images on ipsilateral side gaze. A DDE may cause intermittent symptoms of diplopia, possibly more frequent when the patient is tired, while a VI np is more likely to report consistent, sudden onset diplopia.
Common risk factors for cranial nerve palsies are ischaemic issues [1], and asking about a patient’s general health and current medications can flag up any relevant risk factors.
Specific symptoms
Try to get the patient to be as clear about their symptoms as possible. Both a VI np and a DDE can present with horizontal diplopia, however, as a DDE is a patient losing control over their deviation, symptoms may include blur and headaches as they struggle to maintain control, and intermittent diplopia when they do lose control. On examination, if the decompensating patient is intermittently binocular at distance, they may demonstrate a reduced base-in fusion range.
A patient that is fully decompensated may have initially had asthenopic symptoms, but now appreciates constant diplopia in the distance. A VI np is more likely to give rise to clear, constant diplopia in the distance and an inability to fuse without the aid of a prism or head posture as the deviation will likely be too large to control.
Head postures
A VI np may cause the patient to turn their head towards the affected side (i.e. moving their eyes away from the problematic area). So a left VI np will cause worse diplopia on laevoversion, making the patient want to turn their head left and keep their eyes in dextroversion. They may even be able to regain BSV with their head in this position. A DDE is unlikely to elicit a head posture due to the absence of incomitance.
Ocular motility and measurements on side gaze
Ocular motility is likely to demonstrate asymmetrical / unilateral lateral rectus restriction in a VI np. While a DDE can also present with lateral rectus restrictions, they are likely to be minimal and symmetrical, and prism cover test measurements on side gaze would not demonstrate any significant lateral gaze incomitance.
To perform lateral gaze measurements, get the patient to remove their glasses and fix in primary position on a distance target. Ask the patient to turn their head to one side as far as they can without losing fixation in either eye. Perform a prism cover test in this position and repeat with the patient’s head turned the other way. A left VI np will result in a larger base-out measurement when the patient’s eyes are in laevoversion.


Figure 3: Top) Left VI nerve palsy with lateral gaze incomitance.
Bottom) Typical symmetrical restrictions of abduction, likely age-related with no lateral gaze incomitance.
Saccades
Saccades are often very useful when trying to prove a neurological weakness. The saccadic movement to the affected side will appear slow or incomplete (hypometric) in the direction of the affected muscle compared to the unaffected eye. So a left VI np will produce hypometric abducting saccades in the left eye only. As a DDE does not involve any nerve weakness, saccades will be swift, symmetrical and accurate in both eyes.
“The Hess Chart can give a good indication of whether a deviation is neurological or mechanical”
Primary deviation versus secondary deviation
An important observation that can be noted in a VI np is the secondary deviation being larger than the primary deviation. The primary deviation can be described as the angle that is measured when the patient is fixing with the unaffected eye, i.e. the prism bar is held over the deviating eye.
The secondary deviation is the angle that is measured when the patient is fixing with their affected eye, i.e. the prism bar is held over the unaffected eye.
According to Hering’s Law of equal innervation and vergence movement, when an impulse is sent to an extraocular muscle instructing it to contract, the same impulse is also sent to its contralateral synergist [2]. When the primary deviation is being measured in a left VI np, a certain amount of innervation is required to instruct the right eye to take up fixation. An equal amount of innervation is also then sent to the left medial rectus.
When the secondary deviation is measured, due to the disruption of the nerve supply in the left eye, more innervation is needed for the left eye to take up central fixation, so more innervation is also sent to the right medial rectus, causing a much larger eso deviation when fixing with the affected eye. This would not be seen in a DDE as there is no nerve weakness, so each extraocular muscle will receive the same innervation, and the primary and secondary deviations will be equal.


Figure 4: Top) Hess Chart of a decompensating esophoria. Bottom) Hess Chart of a left VI nerve palsy.
Hess Chart
The Hess Chart can give a good indication of whether a deviation is neurological or mechanical; however, it must not be taken in isolation and should be considered with the rest of the orthoptic report.
If the lateral rectus function line appears ‘squashed’, this can indicate a VI np. If the Hess Chart demonstrates an eso shift but does not appear ‘squashed’ in any way and both fields appear relatively symmetrical, this is more indicative of a DDE.
A useful tip for interpreting the Hess Chart; counting the squares between the inner and outer fields will help determine whether or not the field is ‘squashed’. A full field will have approximately three squares between the inner and outer field.
Conclusion
In the investigation of VI np and a DDE there are some clear differences, however, it is important to consider the investigation as a whole rather than looking at tests in isolation. Patients do not always fit into a ‘perfect box’ and there are rarer cases where asymmetrical lateral rectus restrictions and lateral gaze incomitance are found in a DDE. Some patients may need monitoring over two to three months so their eye movements can be observed over a period of time before the diagnosis is clear.
References
1. Jung JS, Kim DH. Risk factors and prognosis of isolated ischemic third, fourth, or sixth cranial nerve palsies in the Korean population. J Neuroophthalmol 2015;35(1):37‑40.
2. Bridgeman B, Stark L (eds). The Theory of Binocular Vision: Ewald Hering (1868). Springer US; 1977:17-22.
Case history
VI nerve palsy:
Clear diplopia, further separation of images looking to affected side
Decompensating esophoria:
Mixture of diplopia, blur, headaches
Head posture
VI nerve palsy:
Face turn to affected side
Decompensating esophoria:
No head posture
Ocular motility
VI nerve palsy:
Asymmetrical / unilateral restriction of lateral rectus with lateral gaze incomitance
Decompensating esophoria:
No / minimal and symmetrical restrictions of lateral recti with no lateral gaze incomitance
Saccades
VI nerve palsy:
Hypometric in affected eye to affected side
Decompensating esophoria:
Normal
Primary vs. secondary deviation
VI nerve palsy:
Secondary deviation larger than primary deviation
Decompensating esophoria:
Primary and secondary deviation are equal
Hess Chart
VI nerve palsy:
Squashed lateral rectus function line in affected eye
Decompensating esophoria:
Equal fields, with an eso shift
Field of BSV
VI nerve palsy:
Restricted to affected side but improves when looking in away from affected side
Decompensating esophoria:
Variable, not particularly effected in any one position of gaze
COMMENTS ARE WELCOME





