History
-
A 73-year-old female patient was referred for rapid growth of two new lesions on the face.
-
She had past medical history of systemic lymphoma.
-
On examination, there was a palpable mass over the left superior orbital region and the right-side of the nasal bridge.
-
Excisional biopsies of the lesions were sent for ophthalmic pathology assessment.
-
Macroscopic examination revealed: A) left orbital lesion – white fleshy tissue measuring 4mm in diameter; and B) a nasal bridge lesion – three pieces of white firm tissue, the largest measuring 6 x 5 x 4mm.
Questions
-
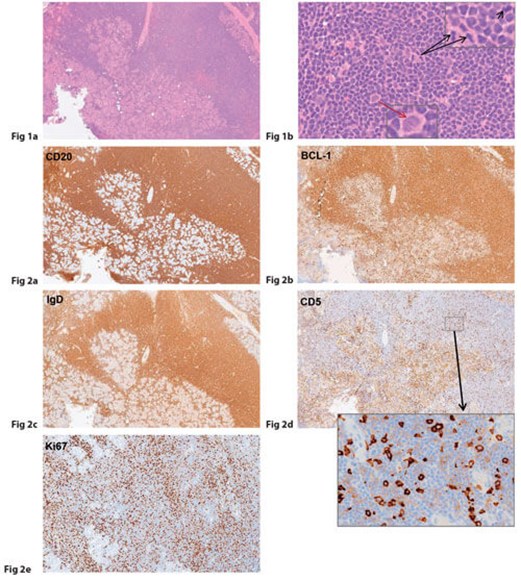
Figure 1 shows a representative H&E section of the lesion. How can this be described?
-
What immunohistochemical stains would help?
-
Figures 2a-e demonstrate positive immunostaining for select markers. What is the most likely diagnosis?
-
What genetic translocation can be associated with this condition?
Answers
1. Figures 1a and 1b show extensive infiltration of orbital tissue and the lacrimal gland with small-to-medium sized atypical lymphocytes, which are centrocyte-like with scant cytoplasm, cleaved and irregular nuclei with condensed chromatin. Mitoses are relatively frequent. The inset demonstrates the frequent mitotic figures (black arrows) along with a pale staining blast-like cell (characteristic of this lymphoma subtype; red arrow). The appearances are consistent with a non-Hodgkin lymphoma.
2. Immunohistochemistry to subtype the lymphoma would include: CD20 & CD79a (B-cell markers); CD3 & CD5 (T-cell markers, latter also subset of B-cells); CD23, BCL-1 (cyclin D1), BCL-2, surface IgM & IgD; and MNF116 (a pancytokeratin marker to exclude carcinoma).
3. Representative panels show the neoplastic B-lymphocytes staining positively for CD20, BCL-1, IgD, IgM, CD5 (aberrant weak membranous and also dot-like positivity in the neoplastic B-cells amongst the strongly staining T-cells) and Ki67 growth fraction of approximately 45%. The cells were negative for CD23, CD3 and MNF-116. The histomorphologic and immunhistochemical features are those of a MANTLE CELL LYMPHOMA. Orbital lymphomas are most commonly low-grade primary extranodal marginal zone B-cell lymphoma or so-called ‘mucosa-associated lymphoid tissue’ (MALT) lymphoma. In this case, however, the lesions were secondary and revealed an intermediate to high grade B-cell lymphoma, which is relatively rare in orbital adnexal structures and the skin.
4. Translocation t(11;14) is often reported in this NHL subtype, leading to over-expression of BCL-1.
Eye News would like to thank previous Section Editor Dr Luciane Dreher Irion for her excellent work on this section since 2016, and welcome new quizmasters Professor Sarah E Coupland and Dr Yamini Krishna to the Pathology Quiz.
COMMENTS ARE WELCOME




