Firstly, my sincere thanks to those of you who responded to last edition’s survey. We had a record response.
Laser was never my most exciting clinical treatment, but in this environment how I wish for even that degree of patient contact.
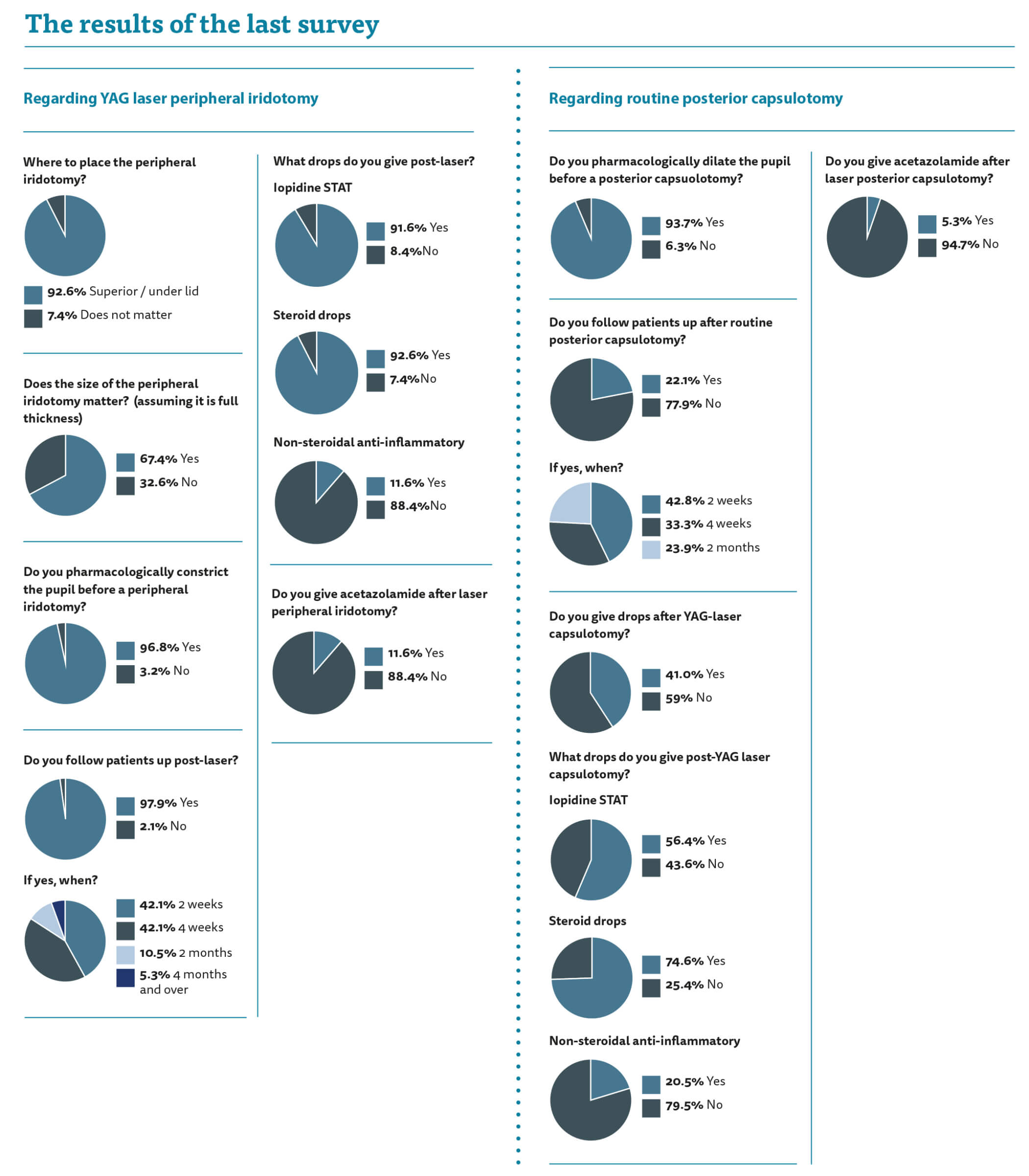
Again, we see variation but this time we seem to be more in agreement. We all tend to pharmacologically miose the pupil prior to peripheral iridotomy and dilate the pupil prior to posterior capsulotomy. Most of us agree that a peripheral iridotomy should go under the eyelid and two-thirds of us believe that size does matter. Consensus seems to be strong that such patients require a follow-up appointment between two and four weeks after their laser.
Regarding postoperative management we all seem to give topical Iopidine and steroids post laser peripheral iridotomy (PI). Only approximately one in 10 of us give acetazolamide post-treatment.
We are more divided when it comes to long-term follow-up. The split is almost 50:50 as to whether such patients require long-term follow-up and more than half of those who say they do would do so in the hospital setting. This means a lot of hospital appointments on a yearly basis forever. I do follow-up my narrow angle patients as I was trained that they have an approximately 15% chance of converting to chronic narrow angle glaucoma. I follow them up until they have their cataracts out and then I believe the risk of the pressure rise goes away as the drainage angle opens up widely. Challenging myself, I wonder why I need to see them in hospital and whether we could simply discharge them back to their own optometrist to measure their pressures? I think the value of guidance here is clear. If a professional body guided us as to whether such patients do or do not require hospital follow-up then we could avoid unnecessary appointments or conversely avoid the risk of avoidable harm.
I personally do not follow-up laser capsulotomy patients as I think the safety profile of this procedure does not require it. Equally, I do not give any post-procedure drops as I do not believe they get much inflammation or a significant pressure rise. I have never had problems with cystoid macular oedema (CMO) or inflammatory problems post capsulotomy.
I hope you find these results interesting and they will aid your practice reflection.
COMMENTS ARE WELCOME






